Exercise-induced bronchoconstriction: testing, testing
Exercise-induced bronchoconstriction (EIB) is a very common condition among sportsmen and women, regardless of age or athletic ability(1-3). The symptoms typically begin shortly after exercise commences, and the athlete also reports occasional wheezing after the end of an exercise session. In all other respects however, the athlete feels well and has no other medical conditions.
Although EIB and exercise-induced asthma (EIA) are often regarded as one and the same thing, this is not strictly true. The term EIB is more accurate because while exercise triggers bronchoconstriction, it does not directly induce the clinical syndrome that defines asthma. Also, the condition of EIB can occur in sportsmen and women without the typical features of asthma. For these reasons, the term EIB is preferred and used here.
The precise physiological and biochemical mechanisms that are responsible for EIB are complex and poorly understood. However, what is fairly well agreed among scientists is that during exercise, the increased flow of air in the airways can act to ‘dry out’ the surface layer of cells in the airway tissues. This in turn can cause physiological changes in the cells below, which may cause them to shrink, stimulating the movement ions and the release of mediators that ultimately lead to the contraction of the smooth muscle in the airways(4).
Symptomatic assessment of EIB
Although rare, the presence of cardiac problems can manifest in symptoms similar to EIB; for this reason, clinicians should be aware of this possibility when faced with an athlete presenting with breathing difficulties and keep this in mind. Also, be aware that as described above, self reporting of symptoms without follow-up testing is not a reliable method of diagnosing EIB. That said however, an initial enquiry should evaluate the following:- Does the athlete complain of shortness of breath, an increased breathing effort, chest tightness, wheeze and/or cough after exercise?
- Are these symptoms also accompanied by reduced performance or increased fatigue?
- Do the symptoms typically appear 5-10 minutes after the start of vigorous exercise (ie heart rate at or above 85% of maximum)?
- Do the symptoms usually subside within 30 minutes or so? If so, can the athlete perform a repeated bout of exercise shortly afterwards, with no repetition of the symptoms?
- Are the symptoms more common/more severe when the athlete swims in chlorinated pool water or exercises outdoors in cold conditions (the volatile chlorinated compounds released from pool water and the lower humidity levels that typify cold weather can both result in increased irritation to the airways(8,9))?
If the answer to all of these questions is ‘yes’ EIB can be suspected and a follow-up test can be performed (see later). If the symptoms are more prominent during inspiration, are maximal at peak intensity and fade when exercise is stopped, this may indicate a transient upper airway obstruction, otherwise known as ‘exercise-induced laryngeal obstruction’. However, the only way to determine this for sure is to use direct visualisation of the upper airway during exercise.
It’s also important to note that where the symptoms persist (see question 4) after 30 minutes, EIB can still be suspected since some symptoms associated with EIB (eg coughing) may actually arise from resulting stimulation of sensory nerves within the airway tree. For the same reason, the presence of coughing alone after exercise may also suggest that EIB is not present.
Clinical assessment of EIB
In cases where EIB is suspected, a true diagnosis of the condition can only be made with the help of functional tests. Essentially, these will involve measurements of airflow using a spirometry device (see box 1). It’s important to point out that peak-flow measurements (sometimes used in fitness testing protocols) are of little use when it comes to evaluating the physiology of the airway in athletes and should not therefore be used. Also, while it might seem intuitive to challenge athletes with an exercise test and monitor responses, this approach is not recommended in the initial stages of investigation because not only are they difficult to perform reliably, their sensitivity for diagnosis is rather poor(10).Box 1: Spirometry devices
A spirometer is a device for measuring timed expired and inspired volumes of air, and hence indicates how quickly and effectively the lungs can be emptied and filled. More mature readers may remember the large volume-displacement devices with bellows or a water-sealed bell, which were standard issue in many physiology labs. These days however, most modern-day spirometers used in the clinical setting are electronic, flow-sensing devices. These include:- Small, hand-held devices that provide digital readings- These are the cheapest options (typically costing around £500) and will fit into a medical bag. However, they do not provide a graphical display (spirogram) and therefore it may be difficult to judge when an expiration is complete. They also need to be used in combination with predicted charts and a calculator to interpret results.
- Portable meters with integrated printers - Typically more expensive than the devices above but will provide calculations, spirograms to monitor exhalations, and a printout including a flow volume loop.
- Systems designed to work with a computer- These will display a graph, make calculations of predicted values and reversibility and provide a printout for records. They also enable tests to be emailed for a second opinion and for electronic storage.
Whatever equipment is used, any device should be regularly calibrated, maintained, cleaned and disinfected according to the manufacturer's instructions. Disposable 'one-way' valved mouthpieces reduce the risk of cross infection (but prevent inspiratory flow-volume loops). A good practice is to keep a calibration and maintenance log and list of patients tested with the spirometer. This enables contact tracing if need be – for example, in case of unwitting testing of a tuberculosis patient.
Testing protocol
In the clinical setting, resting spirometry measurements are the norm, which of course is unlikely to be useful alone when trying to diagnose EIB (see figure 1). A bronchial provocation challenge is necessary therefore to establish evidence of variable airflow obstruction and demonstrate airway narrowing in response to a provocative substance – for example, a cold dry gas. Typically, an athlete will perform two spirometry tests – one before and one after a bronchial challenge. A positive result is signified by a 10% or more fall in FEV1 in the second test. If resting spirometry does demonstrate significant airflow obstruction, a bronchodilator challenge can be performed in order to look for evidence of reversibility of this obstruction. This is confirmed when the administration of a bronchodilator produces an increase in FEV1 of more than 12% or 200mls of air expired(11,12).Figure 1: Diagnostic algorithm for EIB

NB: It may be necessary for athletes to repeat a bronchoprovocation test if negative initially. Note too that other investigations such as marked peak flow variability may be used to support a diagnosis of asthma.
The broncoprovocation challenge
As we have seen, spirometry and exercise alone is unlikely to be sufficient to diagnose EIB. What is required is a reliable bronchoprovocation challenge. But what form should this challenge take? In recent years, the ‘eucapnic voluntary hyperpnea’ (EVH) test, has gained prominence in the diagnosis of EIB –primarily because research shows that hyperpnea of dry air provides a provocative stimulus to the airway(13).The EVH test requires an athlete to complete a period of voluntary hyperpnea with a dry gas inhalant, which desiccates the airways, mimicking the osmotic priming stimulus to EIB. This EVH methodology was first established in 1984 to test army recruits for EIB and is now routinely employed for the diagnosis of EIB in athletes. Indeed, it is now often considered or cited as the ‘optimal’ means for establishing the diagnosis of EIB in athletes(14-16). Moreover, it is now frequently employed to ‘screen’ athletes for airway dysfunction, as an inclusion criterion for studies, and to establish the efficacy of treatment interventions(17,18).
Two types of EVH challenge methodology have been described: the single-stage and the stepped protocol (see figure 2). The single-stage protocol is most commonly employed for athletes and requires subjects to maintain minute ventilation (VE) close to 85 % of their maximal voluntary ventilation (MVV) for six minutes. The target ventilation is typically predicted by multiplying baseline FEV1 by 30 or 35, although it is important to note that this approach is likely to be imprecise in elite athletes(19). Alternatively therefore, target ventilation can be calculated from ventilation data obtained in a prior maximal aerobic exercise test(20).
Figure 2: Broncoprovocation protocol

The single-stepped protocol should be used for athletes. Subjects should be tested only when clinically well (i.e., free from a respiratory tract infection 6 weeks prior to the test), should be advised not to ingest caffeine, and should not exercise on the day of the challenge, as this may exert a refractory protective effect against EIB(21-23).
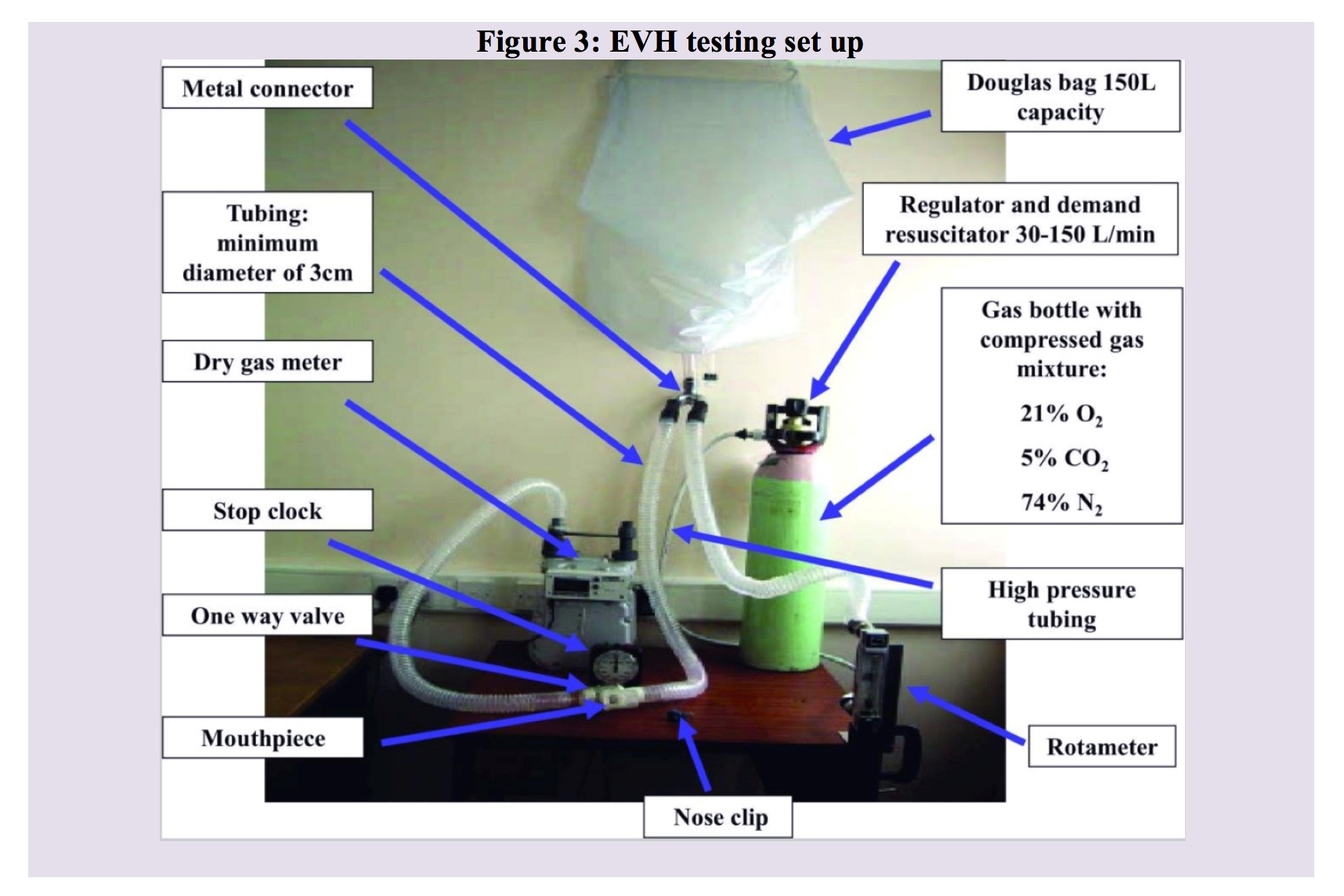
For a subject to achieve this target ventilation and simultaneously maintain eucapnia (ie - perform hyperpnea), the compressed gas source should contain 21 % O2, 5 % CO2, with a balance of N2 (in the UK supplied as BOC code 280890 AK-PC). This inspirate can be administered from a gas cylinder via a direct demand valve or a Douglas bag/balloon (see figure 3) or via a commercial system, which can be used to mix O2 and CO2 gases (eg EucapSys SMTEC, Switzerland). For clinicians unfamiliar with this procedure, see video below.
Video: How to perform an EVH challenge
[video width="640" height="360" mp4="https://www.sportsinjurybulletin.com/wp-content/uploads/2018/07/video-lungs.mp4"][/video]Interpreting the results from an EVH challenge
An EVH test is typically considered positive if the FEV1 falls ≥10 % from the baseline measurement within 20 min of challenge cessation(24). Indeed, some researchers have suggested that the ≥10 % FEV1 fall from baseline should be seen at consecutive time points post EVH and that the highest value out of two reproducible measurements (ie values within 150 ml or 5 % of each other) should be selected(25). While this does support the physiological nature of a response, there is no yet any published data indicating that this criterion improves the sensitivity and/or specificity of the test.The fall in FEV1 during a bronchoprovocation challenge is dependent on the level of ventilation maintained during the test(26). In light of this, it is important to report the VE achieved during the test (see figure 4). It has been proposed that the severity of bronchoconstriction following an EVH test can be classified as mild (≥10 to ≤20 %), moderate (≥20 to ≤30 %), or severe (>30 %), depending on the magnitude of the largest drop in FEV1 and ventilation achieved(27).
The gold-standard test?
The EVH test has been cited as optimal or the ‘gold standard’ and employed in clinical practice to provide a definitive diagnosis of EIB in athletes presenting with respiratory symptoms. As such, it has been endorsed by the International Olympic Committee as the airway challenge of choice in the diagnosis of EIB in athletes(27).However, while the EVH test appears to have good test–retest reproducibility when a subject develops airway narrowing of at least moderate severity (ie >20 %) [48, 49] -it appears to demonstrate poor repeatability at levels approximating a mild fall in FEV1 (10–15 %). Indeed, in a study by Price et al, the poor diagnostic repeatability of EVH indicated that, in a cohort of recreational athletes with a mild reduction in FEV1 post EVH, clinicians should not depend on a single positive test to support or refute a diagnosis(28).
A recent review by Hull et al, also concluded that despite the long history and widespread use of EVH, data to support its position as the ‘gold standard’ for diagnosing EIB are sparse(29). The team carrying out this review concluded:
"the data are highly heterogeneous with regards to athletes’ age, sex, sporting discipline, and level of physical activity. In addition, there are significant methodological differences concerning the clinical (EIB with or without asthma) and functional (FEV1 % fall) adopted diagnostic criteria, the length of the challenge, and the ventilation rate, to permit a definitive conclusion."
Moreover, in terms of methodology, the EVH test has important limitations, including the cost of the compressed gas mixture and a requirement for specialist equipment and skilled technicians to conduct the challenge. In this respect, trained specialists should perform EVH, with precautions taken to minimise the risk of an adverse event (ie severe bronchoconstriction).
There’s also the question of whether EVH represents an appropriate diagnostic test in recreational and non-competitive exercisers, who might not easily maintain high ventilation rates for a prolonged time. One of the major strengths of EVH testing in elite athletes is the ability to achieve a VE rate that mimics the demands of high-intensity exercise. For recreational athletes however, the increased ventilation associated with EVH may not reflect real life – ie EVH may desiccate the airway to a greater extent than typical exercise does in these subjects.
This observation may also be relevant when considering the evaluation of airway symptoms in elite swimmers. In this specific population of athletes, there exists a high prevalence of respiratory symptoms(30), and EVH has been utilised to assess the risk of EIB. However, there are obvious differences between the dry, cold stimuli of EVH and the humid, moist, warm environment encountered in the pool. These are reflected by comparator studies, which have demonstrated a significantly lower prevalence of EIB when testing is performed at the poolside(31).
Making sense
EIB is prevalent in athletes of all abilities and can seriously impact health and performance. The observation of symptoms associated with EIB as a result of exercise is however insufficient to properly diagnose the condition – functional testing is the only reliable way of determining whether EIB is present.With the above in mind, how useful is EVH testing to diagnose EIB? Despite its limitations, the evidence suggests there is still merit in its use. While it might not be a perfect as a ‘gold standard’, the research suggests that EVH remains a valuable indirect bronchoprovocation test in the context of testing athletes for EIB(29). In particular, the key utility of the EVH test lies with the finding of a negative result – ie in terms of the ability to rule out a diagnosis of EIB (because EVH testing is more desiccating to the airways than many comparable exercise scenarios, and a negative results therefore provides strong evidence that EIB is not present).
However, it is also important that prevalence estimates are accurate and not over-estimated by the application of overly sensitive diagnostic test methodologies - ie resulting in a false-positive diagnosis and potential for mistreatment. Also, it is unclear whether EVH provides the same reliability, in terms of sensitivity and specificity, for diagnosing and distinguishing between EIB with and without underlying clinical asthma, which according to the most recent international guidelines should be considered two distinct phenotypes in view of the different pathophysiologic mechanisms and inflammatory patterns(32).
To conclude therefore, the wide sensitivity and specificity indices and poor repeatability in mild to moderate cases preclude EVH being termed a ‘gold standard’ test for EIB. Nevertheless, it is essential that clinicians continue to utilise and undertake some form of objective testing to establish a secure diagnosis of EIB, and not to rely on symptomatic assessment alone. In this respect, the EVH test has a key role in the diagnostic algorithm for EIB testing in athletes. It undoubtedly detects moderate to severe airway hyper-responsiveness (AHR) in susceptible athletes, and its greatest value appears to lie in its negative predictive value.
References
- J Asthma 2003;40(4):349-55
- Thorax 2005;60(8):629-32
- Med Sci Sports Exerc 2007;39(12):2117-24
- J Allergy Clin Immunol 2000;106(3):453-9.
- Med Sci Sports Exerc. 2001 Feb;33(2):208-13
- Br J Sports Med 2010;45(14):1126-31
- Allergy 2012;67(3):390-5
- J Allergy Clin Immunol 1998;101(5):646-52
- Br J Sports Med 2012;46(6):402-06
- J Allergy Clin Immunol 2002;110(3):374-80
- ATS/ERS criteria (www.thoracic.org/statements)
- International Olympic Committee (β2-adrenoceptor agonists and the 2008 Olympic Games in Beijing;www.olympic.org)
- N Engl J Med. 1977;297(14):743–747
- Eur Respir Mon. 2005;33:48–66
- Asthma and the elite athlete: summary of the International Olympic Committee’s consensus conference, Lausanne, Switzerland, January 22–24, 2008
- J Allergy Clin Immunol. 2008;122(2):254–260
- Br J Sports Med. 2006;40(2):179–182
- Clin Respir J. 2007;1(1):3–15
- Med Sci Sports Exerc. 2011;43(3):375–381
- J Asthma. 2004;41(7):745–749
- Chest. 1985;87(1 Suppl):44S–48S
- Chest. 1991;99:1374–1377
- Immunol Allergy Clin North Am. 2013;33(3):329–345
- Respir Med. 2000;94:750–755
- Ann Allergy Asthma Immunol. 2009;103(5):363–369
- Respir Med. 2000;94(8):750–755
- Br J Sports Med. 2001;35(5):344–347
- J Allergy Clin Immunol Pract. 2015;3(2):243–249
- Sports Med. 2016; 46: 1083–1093
- Sports Med. 2009;39(4):295–312
- Br J Sports Med. 2010;44(10):736–740
- Am J Respir Crit Care Med. 2013;187(9):1016–1027
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.







