NSAIDs: the good, the bad and the ugly

Non-steroidal anti-inflammatory drugs (NSAIDs) are cornerstones of pain management in homes, clinics and hospitals worldwide. These agents are consumed or prescribed for diverse conditions ranging from mild intermittent to chronic musculoskeletal pain, as well as for pain associated with cancer, surgery and rehabilitation after placement of prosthetic devices.
However, while NSAIDs have their place in these settings, they are not innocuous and can contribute to peptic ulcers, upper gastro-intestinal bleeding, renal disease and adverse cardiovascular events(1). Of more concern to otherwise healthy athletes however is that NSAID use has also been linked to poor wound healing and to increased risk of complications following surgery.
The process of inflammation
Inflammation is the body's basic response to injury. When an injury occurs, the body immediately recognises the damaged tissue as ‘foreign’, and a sequence of complicated and interrelated events are set in motion to defend the body and eradicate the damaged tissue by a process of destruction, followed by renewal. The general sequence of events following an injury is shown in the box below (see figure 1 also):| Box 1: Inflammation — what happens at the tissue level? |
|---|
| 1. Damage to tissue (e.g. torn ligament, strain or blow to muscle tissue) allows blood to leak into surrounding tissues. This causes a cascade of biochemical events signalling to the body that injury has occurred, and the acute phase of inflammation begins (see figure 1). |
| 2. One of the first reactions is a widening of the small blood vessels supplying the injured area (vasodilation) resulting in increased blood flow. As well as dilating, these blood vessels also start to become ‘leaky’ to proteins, allowing proteins in the blood to leak through the vessel wall into the surrounding tissue. |
| 3. The leakage of proteins into surrounding tissue then causes the filtration of fluid into the tissue, which leads to swelling. This swelling often impinges on sensitive nerve endings, causing pain. |
| 4. At this point, neutrophils (a type of white blood cell) exit from the blood vessels into the tissues, followed by monocytes (another type of white blood cell). Their job is to clean out any bacteria and prevent infection at the injury site. Many of the chemicals released during this phase are broken down into hormones whose role is to tell cells to become active or inactive during this phase of inflammation. Some of these chemicals are called prostaglandins, which can cause pain at the injury site. |
| 5. The arrival of the macrophages (yet another type of immune cell) at the injury site signals the beginning of the next phase in the healing process. Macrophages begin to clean up the area through a combination of digesting the broken-down cell parts and secreting enzymes, which break down damaged cells. With all this activity occurring, inflammation (and pain) often peaks at this stage. |
| 6. Once the wound has been successfully cleared of unwanted material it gives way to a process known as granulation, where new tissue is laid down with the help of special cells called fibroblastsand other cells associated with inflammation. Fibroblasts first appear in significant numbers in the wound on the third day post-injury and achieve peak numbers around the seventh day. Fibroblasts are the primary synthetic element in the repair process and are responsible for production of the majority of structural proteins, such as collagen, used during tissue reconstruction. This initial healing phase marks the end of the inflammation phase, although it may take many days or weeks for inflammation to subside completely. |
| 7. The final phase is called ‘maturation’, whereby the structural proteins in reconstructed tissue are gradually remodelled and strengthened to gain full functionality. This phase can last from a week to a year. |
Figure 1: Muscle injury-induced inflammation(2)
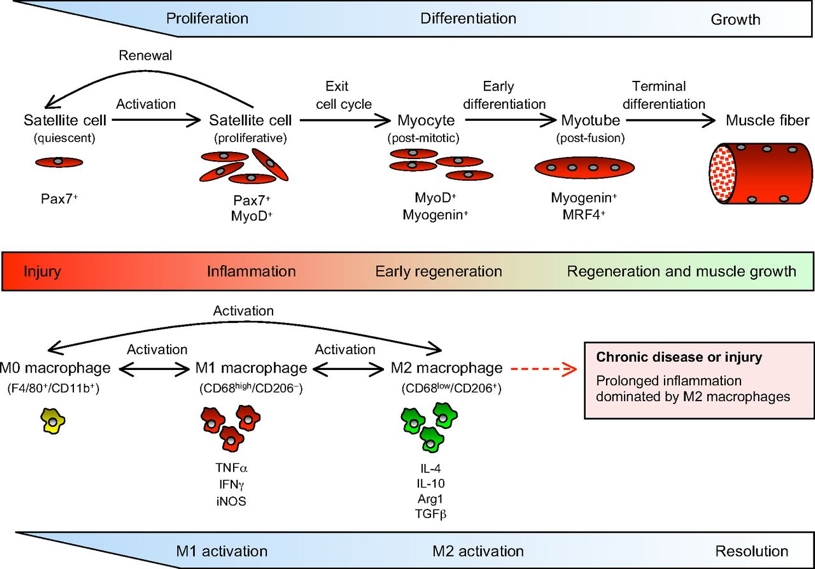
Diagram represents a schematic outline of the cascade of inflammation-related changes occurring following a muscle injury. The top shows the changes occurring to muscle cell architecture while the bottom shows some of the immune factors/cells involved at various stages of inflammation and regeneration.
The progress of muscle cells into early regenerative stages coincides with a shift of macrophages to an M2 phenotype that expresses IL-10, IL-4, arginase 1 (Arg1) and TGFβ. As muscle regeneration and growth proceed to restore normal homeostasis, the inflammatory response is slowly resolved. However, in the case of chronic injury or repeated acute injuries, prolonged activity of M2 macrophages can exacerbate muscle dysfunction by driving the excessive accumulation of connective tissue, which is attributable to prolonged production of the pro-fibrotic cytokine TGFβ and to increased metabolism of arginine by Arg1.
Although inflammation is an integral part of the healing process, however, it invariably causes pain and discomfort. Sometimes this can actually be advantageous. Sensations of pain help to limit movement in the affected area, which can help healing; damaged unrepaired tissue is weak tissue and further movement may worsen the injury. However, when it becomes chronic, inflammation can also be detrimental. For example, chronic joint inflammation can severely limit motion in a joint, yet recent research shows that maintaining mobility is crucial for the long-term health of those joints(3). Although painkillers like codeine and paracetamol can offer pain relief in these conditions, tackling the inflammation itself is a more targeted strategy, which is where anti-inflammatory medication comes in.
Risks of NSAID medication
Anti-inflammatory medications are by far the most commonly prescribed medication for pain involving inflammation. Anti-inflammatory medication falls into two main categories: steroidaland non-steroidal. Steroidal anti-inflammatories, such as hydrocortisone, are very effective, but carry a number of health risks, especially when used for extended periods of time.By contrast - and as their name suggests -non-steroidal anti-inflammatory drugs (NSAIDs), including aspirin, Ibuprofen and Diclofenac, among others, don’t carry the risks of steroid use and are therefore much preferred by medical practitioners. This also explains why the less potent types of NSAIDS, such as aspirin and ibuprofen, can be freely purchased over the counter and are widely used by athletes participating at levels of sport.
Unfortunately, the popularity of NSAIDs among athletes (and some clinicians) is often not matched by an awareness of the risks of regular and/or chronic NSAID use. One of the potential problems for sportsmen and women who use NSAIDs is the fact that many of these drugs can play havoc with the delicate lining of the stomach, with the potential to cause such serious gastric problems as ulcers gastric bleeding.
The reason why NSAIDs can be harmful to the stomach lining results as a consequence of the way they block the conversion of AA to PG2s (as illustrated in figure 2). Some of these protective PG2s are involved in maintaining the integrity of the stomach lining and protecting the stomach wall against the extremely strong acid secreted in the stomach to digest food. Blocking these protective PG2s increases the risk of this acid attacking the stomach wall, leading to such potentially severe gastrointestinal problems as ulcers and stomach bleeding.
Figure 2: NSAIDs and PG2s
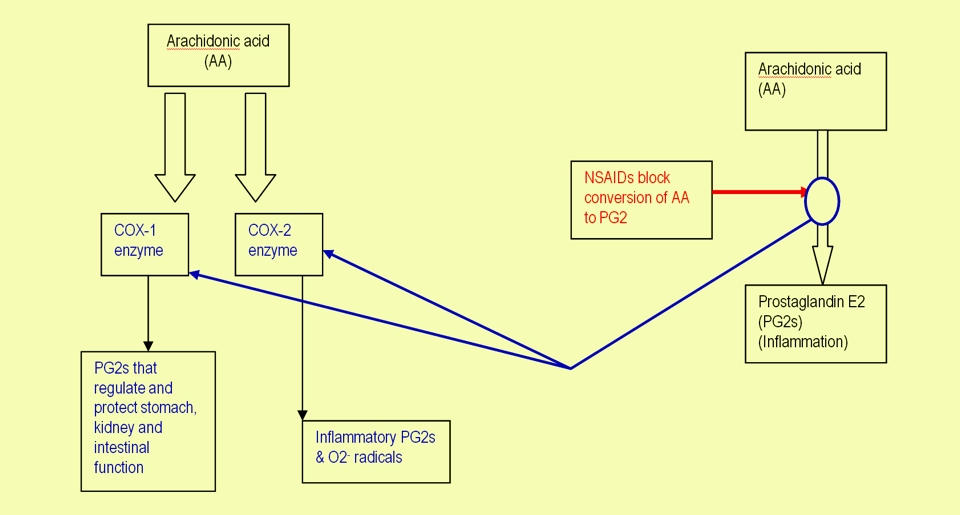
In normal metabolism (right), COX-1 and 2 enzymes convert arachidonic acid (AA) into both inflammation-produsing PG2s and protective PG2s. However, NSAIDs block both COX-1 and COX-2 enzymes, which while helping reduce inflammation, also reduces the production of protective PG2s – for example those involved in maintaining the integrity of the stomach lining.
The potential risks of chronic and/or regular NSAID use involved are considerable. One research study showed that in the USA, NSAIDs caused more deaths than bone marrow cancers, asthma, cervical cancer or Hodgkin's disease (cancer of the lymphatic tissues)(4). Another study published a year later indicated that on average, one in every 1,200 patients taking NSAIDs for at least two months was likely to die from gastro-intestinal complications – people who would not have died if they had not taken NSAIDs(5). A large UK study also showed that the risk of NSAID-induced gastric bleeding (a very serious condition) increases rapidly with age, as does death from complications (see table 1)(6).
| Age range (years) | Chance of GI bleed in any one year due to NSAID use | Chance of dying from GI bleed in any one year due to NSAID use |
|---|---|---|
| 16-45 | 2,100 | 12,353 |
| 45-64 | 646 | 3,800 |
| 65-74 | 570 | 3,353 |
| ‰¥ 75 | 110 | 647 |
NSAIDs and soft tissue healing
In sport, NSAID use is widely advocated to manage the inflammation, pain and swelling associated with acute muscle strain injuries. Within the first 24 to 48 hours following injury, a constellation of symptoms develops, which includes pain with muscle use, stiffness and swelling. These symptoms normally peak between 24 and 72 hours following the injury, typically resolving after five to seven days(7). It is during this period that NSAID use is frequently recommended by doctors and clinicians.However, recent evidence suggests that the inflammatory response to injury is a necessary phase of soft tissue healing, and its inhibition with NSAIDs can significantly delay muscle regeneration and decrease muscle strength after repair(8). These undesirable effects of NSAID use on muscle repair have been attributed to their ability to block COX-2-derived prostaglandins which are known to stimulate muscle progenitor cell (satellite cell) responses to exercise (see figures 1 and 2)(9-11).
These studies have compared satellite cell activity in human volunteers and animal subjects when NSAIDs were administered prior to resistance training or to exercise-induced injury (for example, strenuous downhill running with large amounts of eccentric contraction. In human studies, administration of non-selective NSAIDs (eg Ibuprofen) blocked the normally-observed exercise-induced increase in satellite cell number and mixed muscle protein synthesis(12). Likewise, animal studies have demonstrated a negative effect of NSAIDs on satellite cell responses to exercise and on regeneration after injury(13).
Some researchers have questioned the relevance of these findings, arguing that NSAID use prior to exercise/injury is not typical practice in the general population. However, the prophylactic use of NSAIDs among professional and elite athletes (for example to allow training to continue in the presence of a niggling injury, or to enable athletes to train again sooner after a very hard workout) is a practice that is becoming increasingly common and one with negative connotations for satellite cell activity (see box 2) .
| Analgesics are used widely in sport to treat pain and inflammation following associated with injury. However, there is growing evidence that some athletes might be taking these substances prophylactically, in an attempt to enhance performance(14). In recent review study, researchers looked at the evidence regarding analgesic use prior to exercise — ie are they capable of enhancing exercise performance and, if so, to what extent(14)? They concluded that ‘the ergogenic benefits of analgesics may warrant further consideration by regulatory bodies’. |
| Meanwhile, a 2016 study assessed the effects of Ibuprofen intake on an exhaustive protocol test after six weeks of swimming training in rats(15). Three repeated swimming bouts were performed by the groups and Ibuprofen (15‰mg/kg) was administered once a day. What emerged was that Ibuprofen intake decreased the acetylcholinesterase activity in the cerebral cortex (a measure of fatigue) after an exhaustive exercise test in both trained and sedentary rats. The researchers concluded that the additive anti-inflammatory effects of exercise and Ibuprofen may be a useful means to prevent exercise-induced fatigue. |
| Another 2016 study suggests that the long-term prophylactic use of Ibuprofen could impair the normal training adaptations that occur following exercise(16). Sprague-Dawley rats were divided into exercise or cage activity (sedentary) groups. Half of the rats were administered Ibuprofen to investigate the effects of this drug over time when combined with different activity levels (exercise and sedentary). Supraspinatus tendons were used for mechanical testing and histologic assessment (organisation, cell shape, cellularity), and supraspinatus muscles were used for morphologic (fibre cross-sectional area, centrally nucleated fibers) and fibre type analysis.The results showed that chronic intake of Ibuprofen did not impair supraspinatus tendon organisation or mechanical adaptations to exercise. In addition, the tendon mechanical properties were not diminished. In contrast however, the total supraspinatus muscle fibre cross-sectional area decreased with chronic Ibuprofen administration, and some fibre type-specific changes were detected. The researchers concluded: ‘Our findings suggest that Ibuprofen does not detrimentally affect regulation of supraspinatus tendon adaptations to exercise but doesdecrease muscle growth. Individuals should be advised on the risk of decreased muscle hypertrophy when consuming ibuprofen’. |
Post-exercise NSAID use
Even when used in the conventional manner (post injury), there’s good evidence that NSAIDs may have undesirable effects – particularly in cases of fracture. In one study, researchers looked at patients who had undergone spinal fusion treatment, where two or more vertebrae are fused together. They found that patients who had taken the NSAID Toradol had five times the rate of failed union of the vertebrae than those who had taken no NSAID medication(17).In a recent study, rats were treated Diclofenac, Prednisolone or a placebo following a closed transverse fracture to the femur. After 21 days, the biomechanical properties and histology of the injured bone were examined and a micro-CT performed. The key finding was that the Diclofenac-treated group showed significantly impaired fracture healing compared with the control group. His was evident in terms of reduced stiffness and trabecular thickness. Biomechanics of the Prednisolone group showed obviously lower absolute values than the control group. These alterations were also confirmed in conjunction with μCT and histology (see figure 3)(18).
Figure 3: Representative histological images of fracture sites(18)

Diclofenac (A and B), Prednisolone (C) and control (D) groups. Each section is oriented with the cortical bone on the bottom, periosteal fracture callus on the top and fracture site in the middle.
- A shows a gap without any signs of a union.
- B shows a fibrous bone union.
- In the prednisolone group (C), osteocondral bone union and active new bone formations were detected indicating that endochondral ossification had occurred, although the periosteal OC did not bridge the gap.
- D shows a sample with OC only, and a complete union with trabecular structure (right diagram).
COX-2 inhibitors: a superior alternative?
Around 15 years ago, a new generation of NSAIDS called ‘COX-2 inhibitors’ appeared on the market. These include such products as celecoxib and etoricoxib. As the name suggests, these NSAIDs inhibit the COX-2 pathway, but notthe COX-1 enzyme (see figure 2). In other words, they are able to reduce inflammation while minimising the harmful gastric effects of conventional NSAIDs.When it comes to injury however, the research on COX-2 inhibitors makes for disturbing reading. A group of American scientists examined the effects of COX-2 inhibitors on mice with bone fractures and found that, by comparison with untreated mice, COX-2-treated mice suffered from profoundly compromised bone healing(19).In particular, the bone nodules that formed (small bony growths that form the first stage of healing) were smaller and did not respond to growth factors that would stimulate bone healing in untreated mice. Moreover, when the COX-2 treated mice were then given a dose of the inflammatory PG2s (which had been blocked by the COX-2 drug), the bone healing process was restored, indicating that these inflammatory PG2s may play an essential role in bone healing.
In addition, several studies have shown that the COX-2 inhibitors including celecoxib and rofecoxib either delay or inhibit fracture healing in rats(20,21),while another study found that COX-2 inhibitors decreased the strength of fracture healing at 21 days(22). There is alsoevidence that these drugsimpair the return of mechanical strength following acute injury to ligaments and tendons, as well as bone(23). To make matters worse, the available evidence suggests that the extent of healing impairment is more severe with COX-2 inhibitors than traditional NSAIDs. In the COX-2/rat study above(20), 253 young rats with broken legs were given either one of two types of COX-2 NSAIDS (Vioxx, Celebrex), or indomethacin, which is a traditional NSAID. The indomethacin-treated rats took a week longer to heal than untreated rats, but the new bone was just as strong. However, rats given Vioxx or Celebrex had not fully healed after two months, and the researchers likened the new bone to a ‘weakened shell’.
Recommendations for clinicians
There is no doubt that NSAIDs can help athletes return to training and competition more rapidly, and provide effective pain relief in the process. It is also true that the new generation COX-2 inhibiting NSAIDs are less risky in terms of gastric health. However, clinicians should be aware of the (potentially considerable) downsides of NSAIDs when making recommendations to athletes.Athletes with a previous history of stomach ulcer or other gastric disorders should be steered away from NSAID use whenever possible. For such athletes, the use of a COX-2 inhibitor may be preferred – IF the injury is to soft tissue. In the case of fracture and ligament/tendon injury, the evidence suggests that COX-2 inhibitors should be completely avoided.
For athletes without a history of gastric disorders, the judicious short-term use of NSAIDs is unlikely to pose a problem. In these cases, conventional NSAID use is unlikely to adversely affect tendon/ligament healing. The evidence for NSAID impact on fracture healing is a little more mixed; on balance, long-term NSAID in the case of fracture is best avoided if possible.
In the case of muscle injury, the evidence suggests that NSAID use can significantly delay muscle regeneration and decrease muscle strength and size after repair. This seems to be an inevitable consequence of the fact that the inflammatory response to injury is a necessary phase of soft tissue healing. This has negative implications for athletes that are tempted to use NSAIDs such as Ibuprofen either prophylactically or as an performance-enhancing aid. Athletes should be educated about the risks, and dissuaded from using NSAIDs in this manner. The take-home message is that all NSAIDs pose risks, and should be used as a last resort, not a first!
References
- US Food and Drug Administration (2015) ‘Safety Announcement: FDA strengthens warning that non-aspirin non-steroidal anti-inflammatory drugs (NSAIDs) can cause heart attaches or strokes’.
- Development 2014. 141: 1184-1196
- Autoimmun Rev. 2018 Jan;17(1):53-72
- J Rheumatology 1999. 26 Supp 56: 18-24, 1999
- Pain 2000. 85: 169-182
- Aliment Pharmacol Ther 1997. 11: 283-91
- J Am Acad Orthop Surg 2002. 10: 67-73
- Scand J Med Sci Sports 2012. 22: e8-14
- Am J Physiol Cell Physiol 2004. 287: C475-C483
- Muscle Nerve 2004. 30: 497-500
- J Appl Physiol 2009. (1985) 107: 1600-1611
- 12 Am J Physiol Endocrinol Metab 2002. 282: E551-E556
- J Bone Joint Surg Am 1995. 77: 1510-1519
- PM R. 2018 Jan;10(1):72-82
- Scand J Med Sci Sports. 2016 Oct;26(10):1160-70
- Am J Sports Med. 2016 Sep;44(9):2237-45
- Spine 1998. 23(7): 834-838
- BMC Musculoskeletal Disorders (2016) 17:383
- Journal of Clinical Investigation, 109(11) – 1405-1415, 2002
- J Bone Mineral Research 2002. 17(6): 963-976
- J Bone Joint Surg Am 2004. 86-A(1): 116-23
- J Orthopaedic Research 2003, 21: 670-675
- Sports Med 2005. 35(4): 271-83
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










