Text neck and the curse of thoracic dysfunction

Thoracic spinal or mid back pain is a common complaint among a wide range of age groups within the general population, with adolescents and the elderly alike reporting pain. Shoulder biomechanics can be affected due to restrictions in movement in the thoracic spine leading to narrowing of the subacromial space(1). Therefore, when patients complain of shoulder pain, clinicians should also consider the possibility of thoracic spine dysfunction, and assessment of the thoracic spine is recommended.
Background
It is widely acknowledged within the literature that thoracic flexion or also referred to as kyphosis is a factor in reduced shoulder range of movement(1). However, researchers from the University of Limerick, Ireland, stated that increased kyphosis of the thoracic spine may not be a factor to reduced shoulder range of movement(2). The authors stated that further research of a higher quality is warranted.When discussing reduced thoracic range of movement, there are a multitude of factors to consider. This region of the spine is the support structure for the ribs and breastbone, as well as the many vital organs the thorax protects. The volume of research and level of understanding of the thoracic spine is relatively less well researched in comparison to the lumbar and cervical spines(2).
A position we frequently find ourselves into is that of cervical neck flexion leading to an increase in thoracic flexion. This is due to a recent and growing phenomenon dubbed ‘text neck’. It’s a common site now to see athletes and non athletes walking, sitting, standing looking downwards at a smartphone texting or reading, and it is essential to draw attention to this as health practitioners.
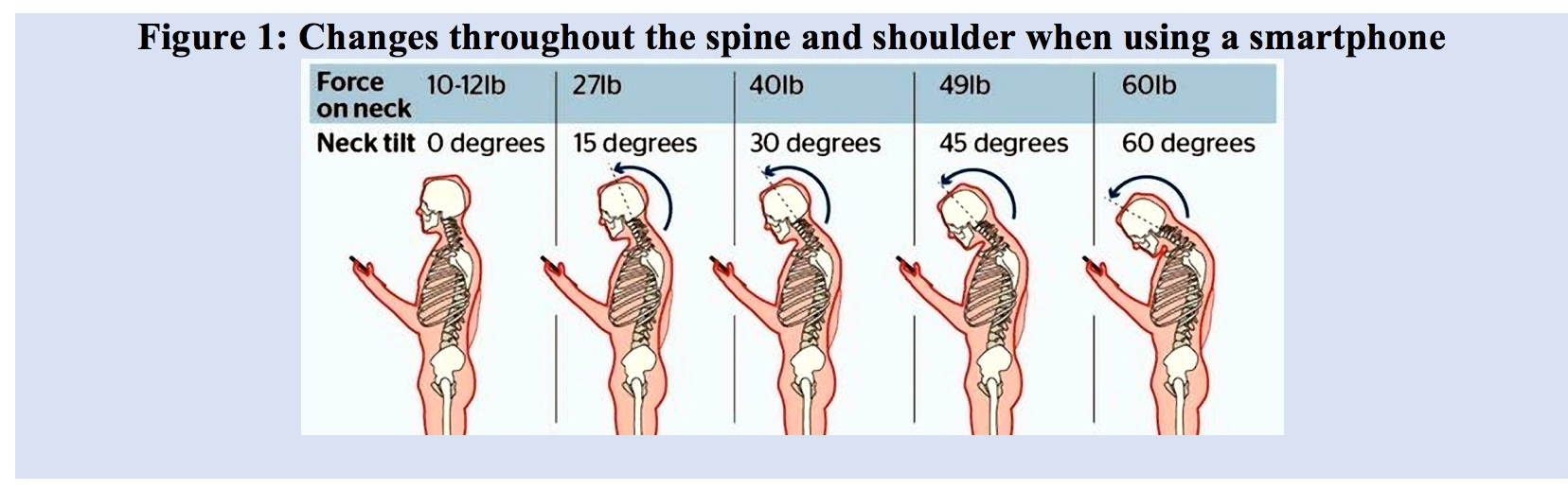
This posture leads to increased stress within the cervical spine, causing protraction at the shoulder girdle and increased flexion of the thoracic spine. Researchers from a Spine Surgery and Rehabilitation department in New York investigate biomechanical forces(3). They found that the head weighs approximately 10-12 pounds, and as the head leans forwards, the forces at the neck increases to 27 pounds at 15 degrees of neck flexion, 40 pounds at 30 degrees, 49 pounds at 45 degrees and 60 pounds at 60 degrees.
Figure 1 demonstrates not only changes in neck flexion angles but also the changes within the thoracic spine when using a smartphone. It can be suggested that the longer someone maintains neck flexion, the more the more muscles fatigue and the greater the increase in neck flexion that occurs. With the volume of phone usage in modern times it is plausible that the positions developed from phone use carry over into the work station and sporting arena, and therefore may become a major player in the onset of back dysfunction and associated injury onset.
Researchers from Daegu University, Korea, not only looked at the effect of smartphone usage on posture but also looked at the effect on respiratory function(4). Fifty participants were separated into two groups of 25 with one group using a smartphone for less than four hours per day and one group using a smartphone for greater than four hours per day. They measured peak expiratory flow, scapula positioning by looking at shoulder protraction and the craniovertebral angle also known as the forward head posture.
The results showed that significant differences existed in terms of posture at both the neck and the shoulder. They also showed a reduction in peak expiratory flow in those using a smartphone for longer than four hours per day. Slumping postures can inhibit the diaphragm and increase the activity of the scalenes promoting the forward head posture and trunk flexion(5).
Anatomy and biomechanics (see figure 2)
To achieve shoulder elevation at 180 degrees, a number of joints need to accommodate sufficient movement to occur. These include the acromioclavicular joint, sternoclavicular joint, glenohumeral joint and the thoracic spine(1). Scapular position is largely determined due to the orientation of the thoracic spine; therefore if a patient has an increased kyphosis, then shoulder elevation can be implicated.
During shoulder elevation, the scapula tilts posteriorly, with the activation of key stabilising muscles such as the serratus anterior and the lower trapezius. Therefore the thoracic spine must be able to extend to allow for the scapular tilting and rotation to be optimised(1). Thoracic extension predominately occurs in the lower portion of the thoracic spine as opposed to the upper region due to the orientation of the facet joints and ribs. During shoulder elevation, around 37 degrees of extension in the lower thoracic spine has been observed in comparison to seven degrees in the upper thoracic region(1).
Sporting actions requiring overhead arm function such as swimming, bowling in cricket and the tennis serve, require thoracic extension and rotation. A limitation of thoracic extension therefore demands the lumbar spine to excessively extend, or requires increased flexion and abduction of the glenohumeral joint to effectively execute these sporting actions.
The sporting actions described above all require an element of thoracic rotation, which is the primary action of the thoracic spine due to the orientation of the facet joints. This can only be achieved if thoracic extension is available; if the spine is positioned in flexion, rotation will likely be restricted. Therefore, if the athlete is unable to actively rotate, it is appropriate to improve extension to allow for rotation to occur.
Examination and assessment
To carry out a thoracic spine assessment, it is essential to carry out specific spine mobility tests, but also to incorporate movements of the extremities too. This will inform the practitioner whether it is related to a mobility restriction or a muscle activation-related issue(1). A key test to assess for thoracic extension is to measure the range of shoulder elevation within the scapular plane (see figure 3).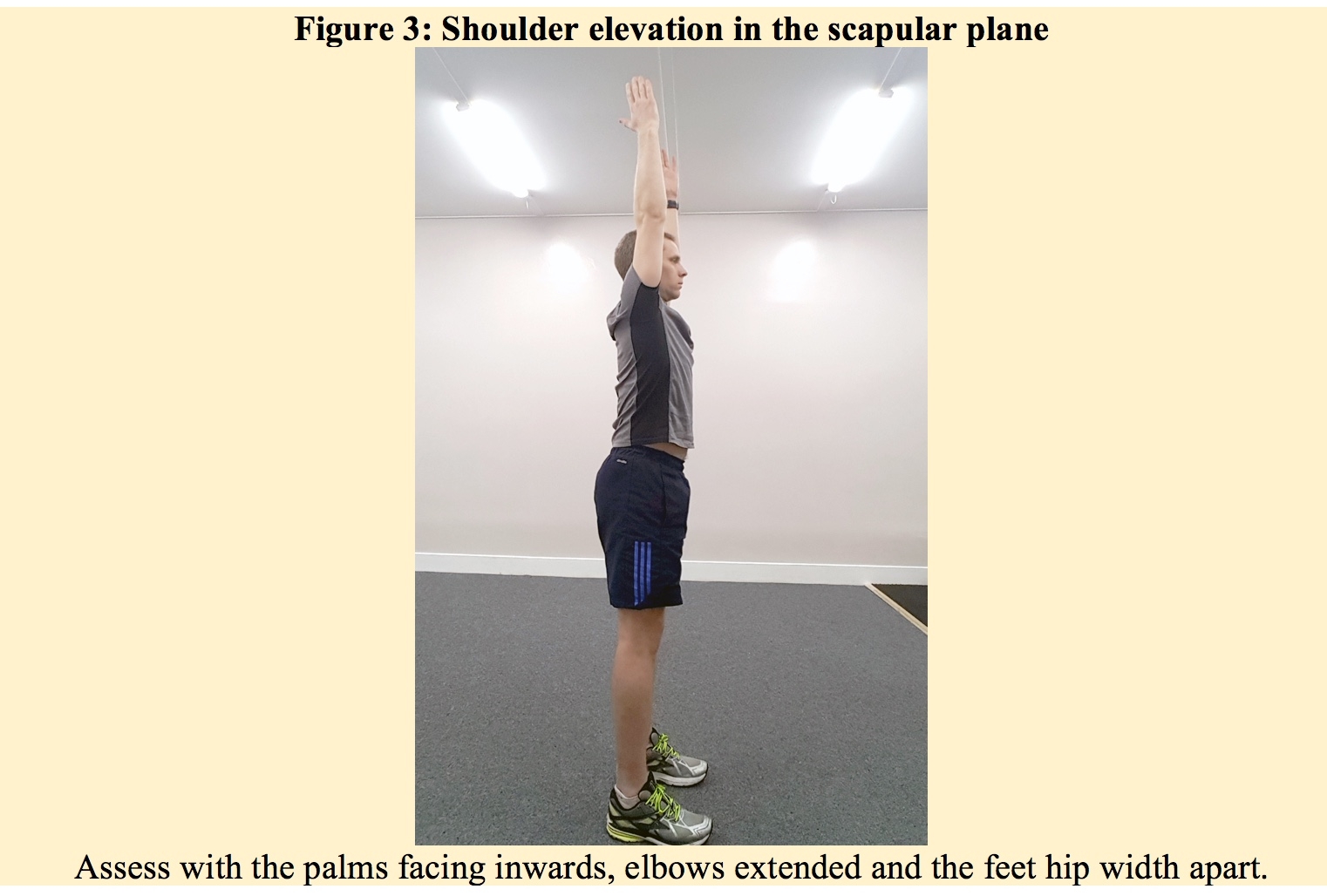
If a limitation into elevation exists then it is essential to explore whether thoracic mobility is restricted using the occiput-to-wall test (see figure 4). The occiput-to-wall test has good test/retest reliability, needs no equipment and is quick and easy to implement(2). There is also a very similar test called the tragus-to-wall test whereby the distance measured is from the tragus of the ear to the wall as opposed to the occiput to the wall. If the restriction is within the thoracic spine then this can be treated appropriately using the exercises shown later.

If there is full active range of motion of the shoulder into elevation, it’s important to measure shoulder elevation under load - ie with dumbbells in a shoulder press type position (see figure 5). It is important to assess both the angle of the shoulder into elevation (ie whether the individual can still attain 180 degrees if they could previously), but also the angle of the thoracic spine. It is possible that a muscle imbalance between the trunk flexors and extensors, with increased activity of the abdominals causing thoracic flexion, brings about a reduced range of movement of the shoulder into elevation when loaded with weight. This would indicate reduced activity of the extensor muscles of the back in relation to the trunk flexors - as opposed to joint stiffness in the thoracic spine.

One of the key movements of the thoracic spine is its ability to rotate based on the orientation of the facet joints. By assessing rotation in a seated position the pelvis is stabilised, which eliminates movements from the extremities (see figure 6). It may also useful to observe rotation in standing, as this can help identify potential restrictions throughout the kinetic chain.
Rotation in sitting may provide additional compensation of the lumbar spine; therefore it is ideal to use a box to ensure the hips and knees are flexed to 90 degrees, which also places the lumbar spine into slight flexion. The hips can be stabilised further by placing an item between the knees approximately 20cm apart(1). This test is easy to carry out and has shown to have a good level of reliability(6). Normal ranges of movement for the thoracic spine are in the region of 30 degrees of rotation.

Management of the thoracic spine
A common approach to managing thoracic joint stiffness is a high-velocity low-amplitude manipulation, which is often considered as a more attractive approach to physiotherapy or satisfactory to the patient. Thoracic manipulation using a crossed pisiform grip has been found to be effective in increasing shoulder movement into abduction, and a reducing pain in patients with rotator cuff tendinopathy(7).It is important to emphasise the requirement of self-mobilisation techniques to the patient in addition to joint manipulations. If not, it is very possible for the thoracic stiffness to recur as a result of postural habits. A research study in Sweden carried out an assessment of self-mobilising thoracic techniques in patients with ankylosing spondylitis. Physiotherapy sessions were for one hour, twice per week. The results yielded a significant increase in chest expansion at the xiphoid process, as well as positive changes in posture and spinal mobility(8).
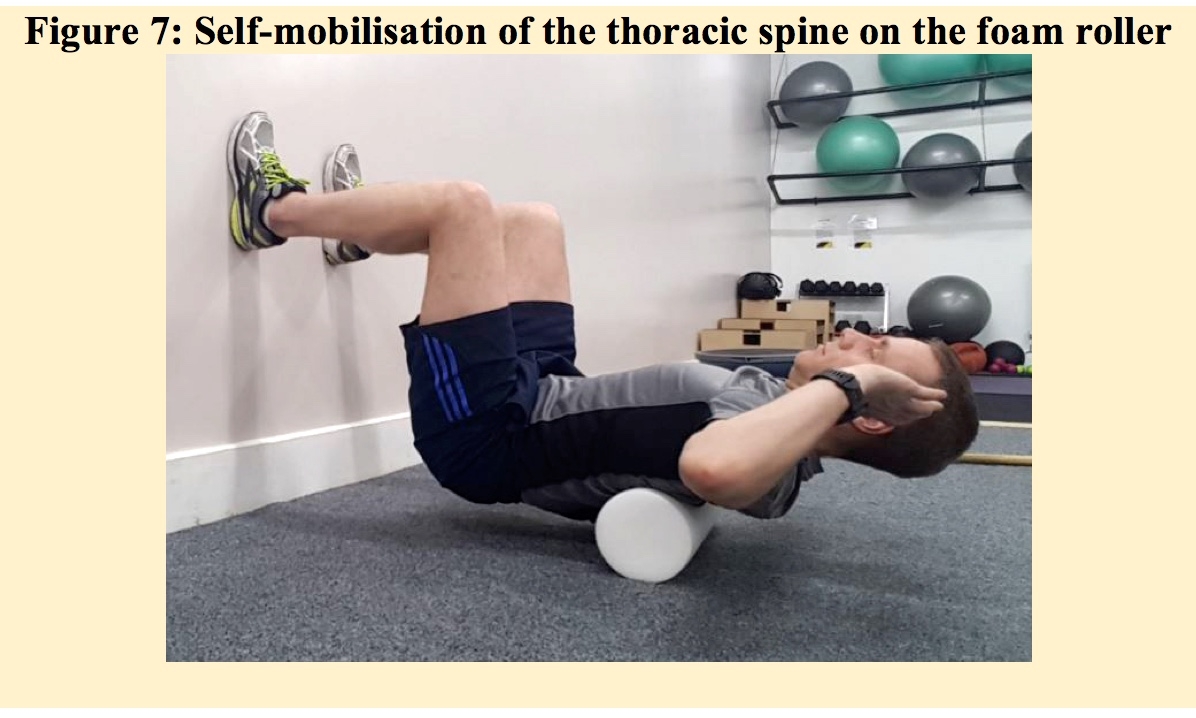
Thoracic mobilisation can be performed in a variety of positions, all of which should prevent unwanted compensatory movements through the lumbar spine(1). On the foam roller for example, the feet are placed on the wall to prevent lumbar extension, and to promote a small range of lumbar flexion (see figure 7). This position should be maintained for 30 seconds at a time and aim to work at different levels of the thoracic spine to optimise joint mobility. As part of the rehabilitation, and to study the effectiveness of the rehabilitation exercises, a test-retest process should be included. The rotation exercises should be performed into an extended position to allow for optimal rotation to occur without the trunk going into a flexed position (see figure 8).

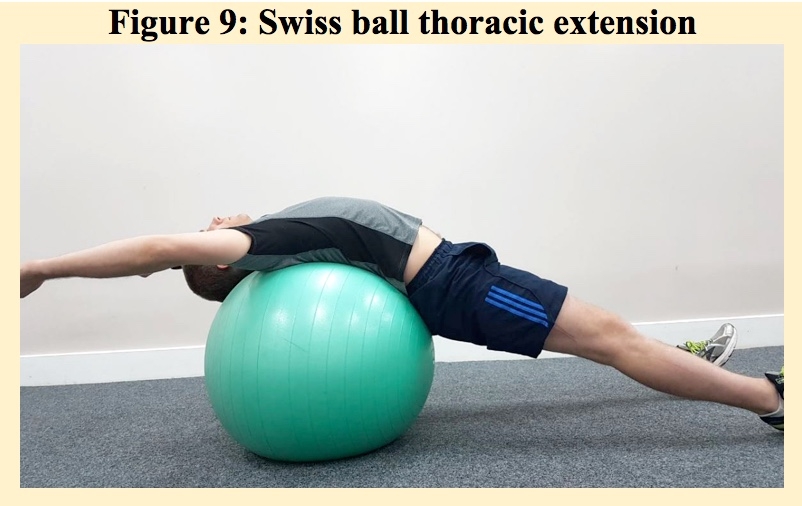
Thoracic extension can enhance chest expansion, and a good starting point is on a Swiss ball where by enhanced inhalation can occur by opening up the chest and shoulder muscles (see figure 9)(5). In this position however, it’s important to be aware that patients may experience dizziness so allow the patient to become used to this position.
 A more progressive exercise into extension can be executed in a squat position whereby the arms are placed on the wall and the mid thoracic spine T4-T8 can be opened up by pressing the arms into the wall (see figure 10). Ensure in each of the positions into extension that a rhythmic breathing pattern is maintained throughout to encourage joint mobilisation.
A more progressive exercise into extension can be executed in a squat position whereby the arms are placed on the wall and the mid thoracic spine T4-T8 can be opened up by pressing the arms into the wall (see figure 10). Ensure in each of the positions into extension that a rhythmic breathing pattern is maintained throughout to encourage joint mobilisation.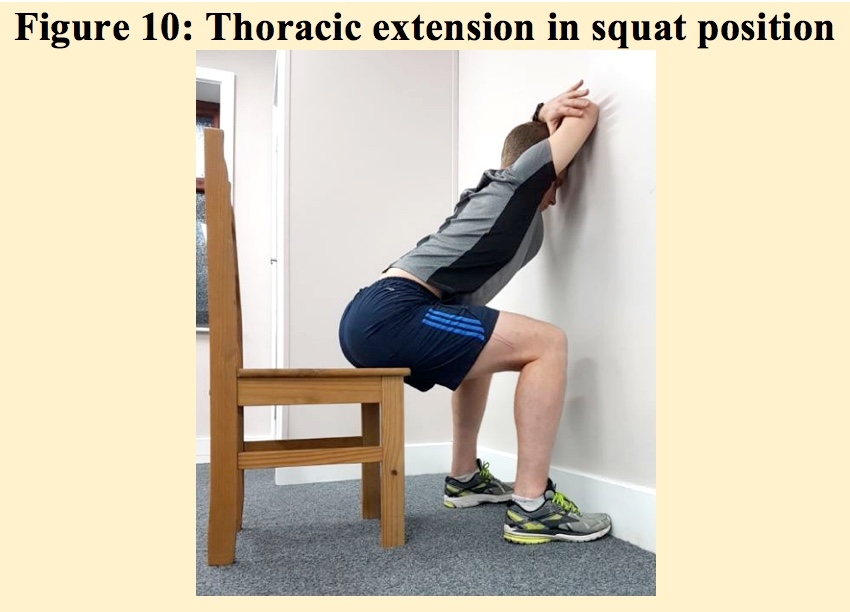
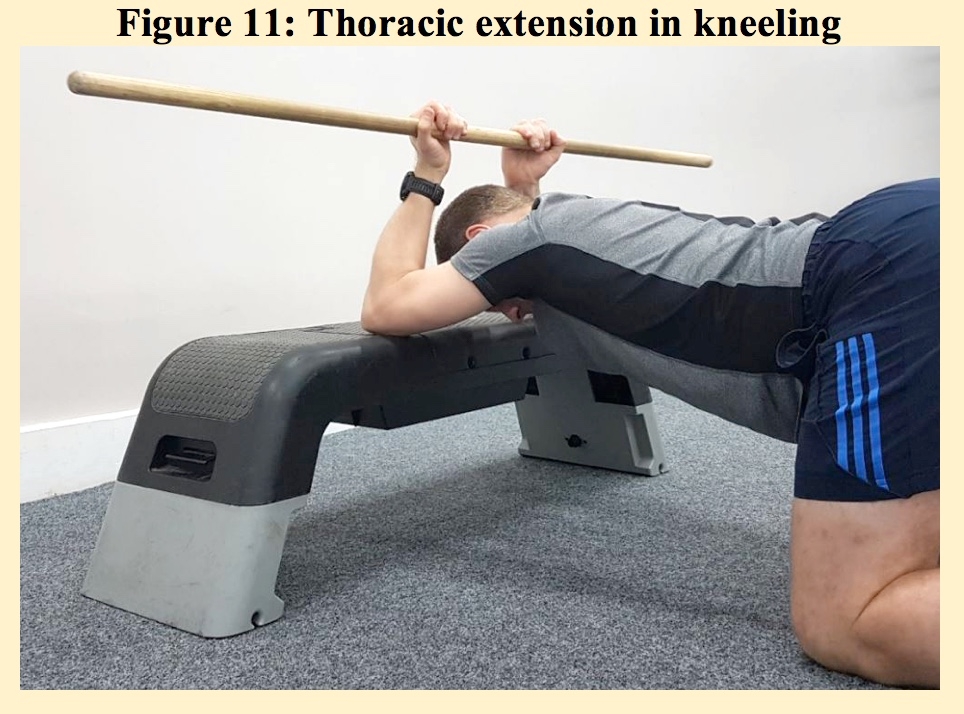
The more advanced exercise into extension is shown in figure 11, whereby the force is exerted downwards, encouraging both shoulder and mid thoracic spine mobility. Each of these positions should be maintained for up to 30 seconds and repeated three to five times.
Summary
Thoracic spine dysfunction can lead to biomechanical changes at the shoulder and lumbar regions, and therefore contribute to injuries elsewhere. When clinicians consider the thoracic spine, they should try think of it in isolation, but rather think of it more holistically, as part of the chest wall as a whole. It is important to ask whether thoracic dysfunction is related to poor technique in a given sport, or whether it is posture related – for example excessive smartphone use. When managing thoracic dysfunction, an assessment of mobility is important before a therapy programme begins – this allows clinicians to monitor progress and modify the management as appropriate.References
- Prof Strength and Cond, 2015, 39, 21–30
- J Rheumatol, Sept, 2004, 31, 9, 1779-1784
- Surg Technol Int,Nov, 2014, 25, 277-9
- Phys. Ther. Sci, 2016, 28, 186–189
- Dynamic Chiropractic, Sept, 2001, 19, 19
- J of Ath Train, 2012, 47, 1, 52 – 60
- MTP & Rehab Journal, 2016, 14, 383
- Clin Rehabil, July, 2009, 23,7, 599-608
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










