Breaking protocol: using the four pillars of exercise prescription to enhance rehab

Diagnosis-based protocols focus on the specific injury. For example, hamstring injuries are treated with Nordic exercises, adductor strains with the Copenhagen protocol, Achilles tendinopathy with the Alfredson protocol, etc. Clinicians and trainers then turn to strength and conditioning strategies, focusing on outcomes such as strength, power, and hypertrophy, to prepare the athlete for return to sport. Though evidence-based, these exercise prescriptions and methodologies may not create the same adaptations in every person. Every athlete moves differently, and their goal within their sport varies from player to player. Therefore, exercise prescription should consider how to influence each athlete’s mechanics, technique, and tissue adaptation in addition to rehabbing a specific injury.
Muscle Structure
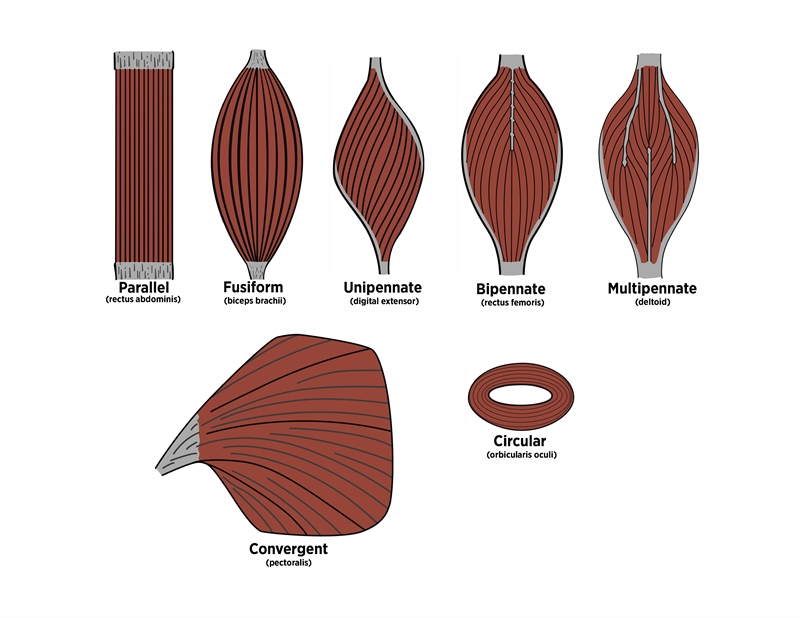
Muscle architectureA muscle’s architecture defines its role. Therefore, rehabilitation should optimize it’s function relative to the muscle’s anatomy. A muscle is made of fibers arranged in either a parallel, convergent, circular, or pennate pattern (see figure 1). Parallel fibers run the length of the muscle and gather at each end to join their tendons in a fusiform shape or attach to a wide flat aponeurosis. A combination of a wide attachment at one end of the muscle and a gathering at the other end forms a convergent shape. Sphincters and openings in the body are made of circular muscle fibers.
Most of the skeletal muscles in the limbs are pennate. Pennate muscles resemble a feather, with fibers attaching to a tendon that runs through the muscle. The pennation angle is the angle of the muscle fiber to the tendon(1). If the muscle fibers attach to only one side of the tendon, they are unipennate. Bipennate fibers attach to both sides of the tendon and multipennate muscles have several tendonous attachments within the muscle.
Pennate muscles with oblique pennation angles, such as the rectus femoris, typically contain more muscle fibers than other types of muscle. Thus, they generate stronger contractile forces. While the force a muscle exerts is related to its physiological cross-sectional area (CSA), the degree of pennation also affects the muscle’s strength and velocity generating potential(1). A higher pennation angle increases the force-generating capacity of the muscle. Whereas muscles in parallel, while perhaps having the same CSA, can’t generate as much force because their fibers attach in series with one another. However, having a greater number of sarcomeres in a row means fewer but longer muscle fibers which are well suited to high velocity through large ranges of motion.
Figure 1: Muscle fiber arrangements and examples.
Most clinicians understand that training increases CSA, but can it affect the pennation angle as well? Researchers in Denmark subjected 11 healthy male volunteers to 14 weeks of heavy resistance training of their lower limbs to answer this question(2). Before and after the training protocol, they measured the volume and CSA of the rectus femoris muscle and the pennation angle and CSA of the muscle fibers of the vastus lateralis.
The training protocol consisted of the following exercises: hack squats, incline leg press, knee extension, hamstring curl, and calf raises. The program began with 10 to 12 rep max (RM) loads for the first four sessions and progressed to a four to six RM for the last four weeks of the 14-week program. After the exercise period, the mean pennation angle in the vastus lateralis changed from roughly 8% to 10%, signifying a change of 35%(2). Average muscle CSA increased by about 15%, with the largest growth in the number of Type II fibers(2). Maximal quadriceps isometric strength also increased significantly after the training program. Based on previous research, the authors suggest that the heavy progressive loads were responsible for the increase in pennation angle and CSA. While smaller loads can result in increased CSA, pennation angle changes seem to occur with near-maximal loading. Thus, knowing the muscle’s structure allows the clinician to select exercises to train the muscle such that it increases in both the number of muscle fibers and their pennation angle.
Muscle fiber type
Skeletal muscle is composed of different muscle fiber types which have marked differences in their characteristics, function, and role. Identifying the muscle fiber type within the injured muscle can provide awareness to rehabilitation needs and expectations. Muscle fibers are classified as slow-twitch (Type I) or fast-twitch (Type II).
Slow-twitch fibers develop force and relax slowly; therefore, they are more energy-efficient and fatigue-resistant. Fast-twitch fibers create force and relax rapidly, meaning they have high anaerobic power but fatigue quickly and are inefficient. For example, the soleus is composed of Type I fibers and will take longer to build force, whereas the quadriceps contain a mixture of both fibers types. Thus, plan rehabilitation exercises to stimulate growth of the muscle’s predominant fiber type(1).
Muscle Function
Planes of movementThe anatomical planes of movement describe how the body moves through space. Knowing the movement patterns required for an athlete’s sport improves the specificity of exercise planning. While this specificity is important, most movements require vertical forces, followed by horizontal and rotational. Therefore, movement typically occurs in the sagittal plane, followed by the coronal and transverse planes. Athletic injuries, such as ACL tears, usually occur due to a loss of rotational control in transverse plane movements. Since movement occurs predominately in the sagittal plane, lack of strength and stability in the other planes may contribute to this injury pattern(3).
This injury theory suggests rehabilitation should focus on developing vertical and horizontal force production within sagittal and transverse planes to enhance rotational stability. For example, the gluteus medius is the primary mover of femoral external rotation. However, rehabilitating this muscle using only rotational exercises like clamshells will not produce enough of a stimulus load to obtain the desired training response. Therefore, training the muscle in other planes of movement recruits all the fibers and maximizes training benefits. Consider activities such as single-leg high step-up (the movement pattern is flexion to extension in the sagittal plane) and load with a heavy weight in the opposite hand for a transverse plane stress. This approach increases gluteal load by up to 200%, far more than could be achieved through an isolated rotational exercise(4).
The majority of sports involve multi-joint coordinated movements through multiple planes rather than single-joint movement in a single plane. Once strength returns in single-plane exercises, begin neuromuscular training to facilitate coordinated movement patterns and improve fiber recruitment rate. This kind of training fosters coordinated movement and joint control in all planes of motion. Neuromuscular deficits in the timing of muscle activation may be responsible for some sports injuries. Therefore, an athlete’s rehabilitation program must also include rate of force production training adequate for a return to sport beyond that needed for daily living activities.
Muscle as levers
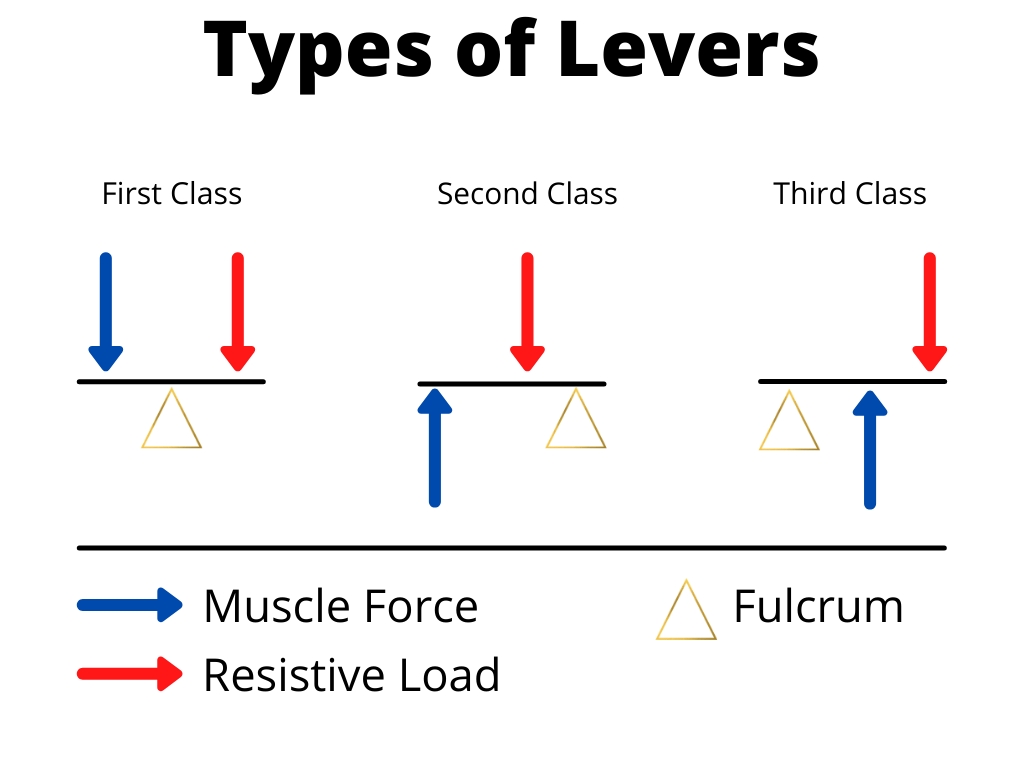
Most extremity muscles work via a lever system. A lever consists of three parts: the effort required by the muscle force, the resistive load, and the fulcrum, which is the joint (see figure 2). Understanding how these work can help identify mechanical disadvantages and direct rehabilitation prescriptions (see table 1).
Figure 2: First, second, and third-class levers
| Class of lever | Definition | Aim | Example |
|---|---|---|---|
| First | A lever where the muscle and the load act on opposite sides of the fulcrum. | Speed of movement when the fulcrum is close to the load. Strength when the fulcrum is close to the muscle force. | Elbow extension - the fulcrum is the elbow joint, the muscle force is the upper arm and the load is at the hand. |
| Second | A lever where the muscle and load act on the same side of the fulcrum. The load is closer to the fulcrum than the muscle force. The required muscle force is smaller than the load. | Force output. | Plantarflexion - the fulcrum is the ball of the foot, the muscle force is up the lower limb, and the load is the downward force of the fibula. |
| Third | A lever where the muscle force and load act on the same side of the fulcrum. The muscle force is closer to the fulcrum and has to be greater than the load. | Speed and movement, but a mechanical disadvantage are present. | Knee flexion - the fulcrum is the knee joint, the muscle force is the hamstrings insertion on the tibia, and the load is the weight of the lower leg. |
Tissue loading
Three different types of muscle contractions generate force within the muscle: isometric, concentric, and eccentric. Isometric contractions occur when the muscle length does not change; therefore, no mechanical work occurs. Even though there’s no external load, isometric contractions produce large muscle forces. Thus, they require a high amount of energy to produce (see figure 3). Contractions in which the muscle shortens are called concentric contractions. They produce the least amount of force but require the greatest amount of energy to produce. Those contractions in which the muscle lengthens are eccentric contractions. This type of contraction generates the highest amount of force yet needs much less energy. Because of this, eccentric contractions are sometimes better tolerated in injured athletes.
Athletes with joint injuries often tolerate isometric contractions better because the joint doesn’t move, and the athlete has more control over the amount of force they produce. In those with fear-avoidance behaviors, consider facilitating isometric contractions while holding the joint in static positions throughout its range of movement. The proprioceptive neuromuscular facilitation (PNF) contract-relax technique eases the patient into more joint range of movement, helps with pain, introduces isometric loading, inhibits the opposing muscles, and improves muscle lengthening. Starting with isometric contractions elicits adequate loading stress to produce muscle adaptations and improved strength while keeping the patient more comfortable.
Figure 3: Relationship between muscle contractions and the energy to produce them
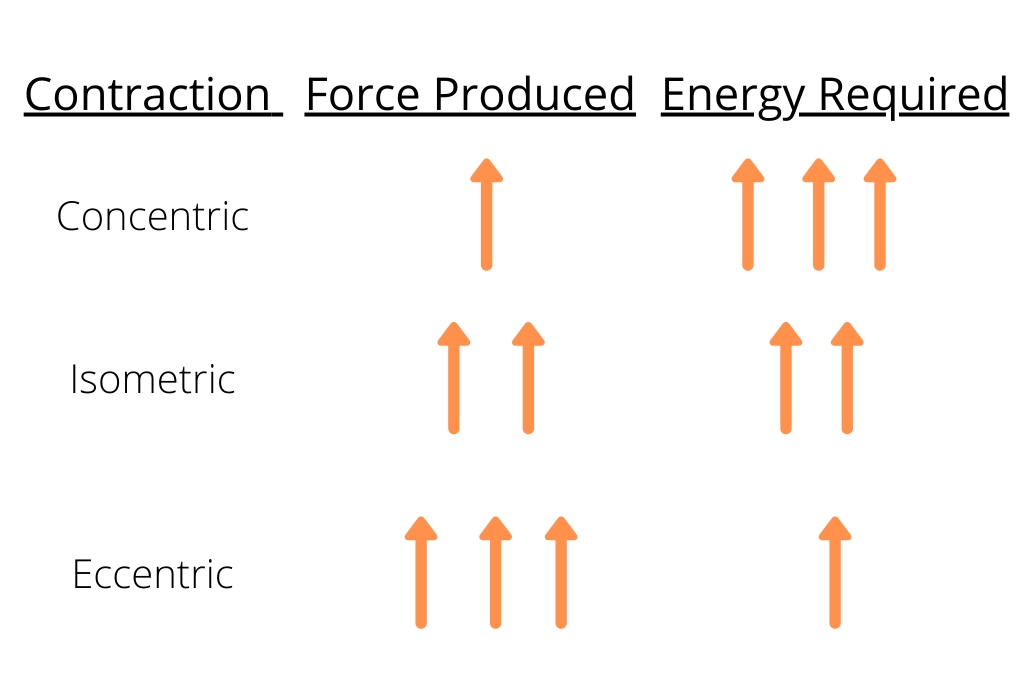
Also, consider the entire muscle-tendon unit as muscles and tendons respond differently to loading due to their active and passive characteristics and relative elastic energy (see figure 3). Tendons have a linear progression to failure, meaning they often do not fail instantly. In contrast, muscles have a steeper failure curve and fatigue quickly upon excessive load.
Tendons help withstand eccentric movement and amplify muscle power due to their elasticity. They also act as a mechanical force transmitter by preventing a muscle from reaching its peak muscle force or breaking point and avoiding injury(5). Therefore, training tendons is an important part of the rehabilitation of a muscle. While elastic, they also provide stiffness and stability to the muscle. They can increase their stiffness by up to 69% just by prescribing the correct dosage of loading. Increased stiffness also helps protect the whole musculotendinous unit against additional injury risk(6).
Figure 4: A schematic representation of adaptations in tendon and muscle in response to loading*(7).
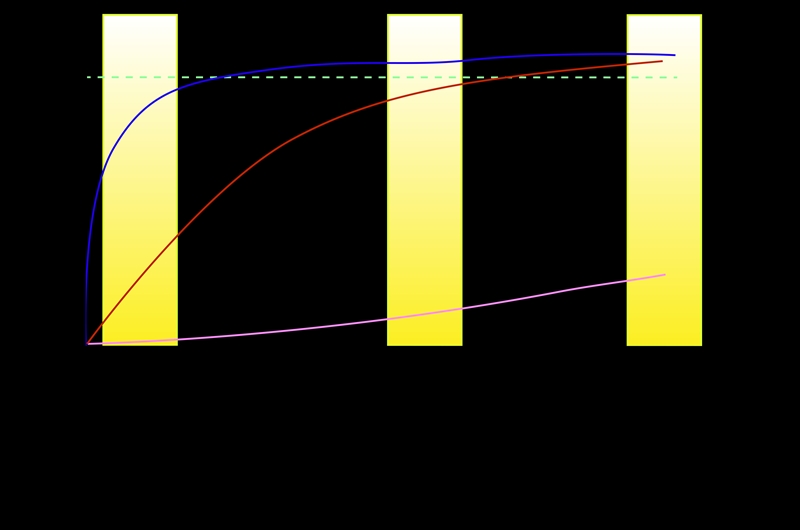
*Adapted from Br J Sports Med. 2018; 52(10): 622-623
Movement
Muscle spindleForce production occurs via the recruitment of muscle fibers within the muscular motor unit. A stretch on the muscle spindle wrapped around the muscle fibers stimulates a contraction. If a single stretch occurs, the resulting muscle contraction produces minimal force. Exercise can increase the force output in one of two ways. Spatial summation recruits more motor units by increasing the stretch to the muscle through additional load and the recruitment of more motor units. Temporal or wave summation increases the rate of neural firing, building force output by stimulating the muscle fiber before it fully relaxes from a previous contraction. More than half of the muscle fibers are stimulated in the final 10% of a maximal muscle contraction(8). Therefore, sub-maximal efforts don’t recruit the entire muscle(8). Muscles only enlist what is needed to overcome the resistance at hand. Thus, muscles require maximum load to recruit all the motor units within the muscle.
Golgi-tendon organ
This heavy loading of the muscle causes an increase in muscle tension and tendon stretch, which triggers the Golgi-tendon organ (a sensor in the muscle-tendon junction that regulates tendon stretch to prevent excessive tension). The Golgi-tendon organ then activates an inhibitory motor-neuron in the spinal cord, which inhibits muscle activation and causes the muscle to relax. An adaptation to regular heavy resistance training may be the over-riding of this inhibition and the key to greater force production(1).
Understanding the regulation of force production is key to facilitating greater muscle responses to enhance performance, but also to overcome or prevent injury. Athletes who get injured often can’t generate maximal force production as quickly as required. Maximizing neural recruitment is another way to increase force production and prepare the athlete to return to sport (see table 2).
| Task: | Category of influence: |
|---|---|
| Increase muscle cross-sectional area | Structure & architecture |
| Perform multi-joint, multi-muscle exercises to optimize fast-twitch recruitment | Fiber type & force production |
| Identify a mechanical advantage | Movement planes & muscle levers |
| Train heavy loads to maximize neural recruitment | Summation and Golgi-tendon organ over-riding |
Metabolism
Injury versus repairMechanotransduction is the physiological process where the body converts mechanical load stimulus to cellular responses that promote structural change. The resulting protein synthesis fosters the growth and hypertrophy of muscle tissue(9). Muscles, ligaments, tendons, and bone all respond to this, but the rate at which they adapt varies between the tissues(9).
Phase of healing
The rate at which the tissues adapt to the stimulus depends on the phase of healing. Once loaded, tissue needs time to adapt to the increased load before increasing it again. If trainers progress the load too rapidly, there is the risk of further injury, inhibited healing, or increased pain which may prevent further progress. The resulting protein synthesis requires approximately 48-72 hours after loading to complete.
Systemic versus local healing
The cardiovascular system adapts the fastest to training, so athletes often seem ready to return to sport ahead of developing the required mechanical strength. While their injury may appear resolved, the injured tissue may not be prepared to withstand the strenuous demand of sport. Therefore, ensure the athlete demonstrates complete tissue adaptation, not just a return to fitness, before resuming competitive play.
What if loading causes pain?
Pain on loading the injured tissue likely inhibits further progress. Therefore, consider using lateral force transmission when athletes resist or have continued difficulty loading a muscle. Resistive loads applied to a nearby healthy muscle influence the injured muscle’s ability to tolerate load. This approach creates a perpendicular force through the tendon, provides fluid transport, and increases hydrostatic pressure, thus optimizing tissue healing(10). For example, stop loading the hamstring muscle longitudinally if it aggravates a sensitive high hamstring injury. Instead, perform isometric loading exercises throughout the muscle range, then perpendicularly load the tendon with abduction and adduction work. This method allows indirect loading without pain and gives the damaged hamstring time to repair while still providing stimulus to and adaptation in the tendon.Ready to run?
Upper legWhile focused on injury recovery, don’t forget that most athletes need to run or sprint when they return to sport. Be mindful of rehabilitating the whole athlete, especially if they’ve been laid up with a long recovery. To help them return to efficient running, strengthen the leg muscles that assist with vertical forces and extension torque. The main muscles involved in developing this vertical force are the soleus, quadriceps, and gluteus medius muscles.
Most lower limb strength programs that address these muscles involve squats. Clinicians can tailor a squatting program to foster an individualized outcome. A multi-center study recorded the net moments at varying joint angles in 10 resistance-trained women performing a back squat at 50% and 90% repetition max (RM)(11). They found that the adductor magnus played a greater role in producing hip extension force in deeper squats and those with lighter loads(11). Interestingly, the gluteus maximus contributed more during shallow squats, and this contribution was the same at lighter and heavier loads.
The study found that with greater loads, the hamstring contribution increases to assist the adductor magnus. As the hamstrings are a two-joint muscle, they also exert a knee flexion moment while contracting to produce hip extension. Thus, the quadriceps are recruited to counter the knee flexion force. Identifying where the athlete requires increased strength allows for individualized and targeted exercise prescriptions, rather than just assigning everyone the same squat program.
Lower leg
Efficient training is important to make the most of the time in rehabilitation. Since the foot and ankle complex absorbs up to 12.5 times bodyweight in sprinting, it pays to focus on this region(12). Almost all lower leg muscles contribute to plantarflexion. Therefore, training in plantarflexion develops these muscles, improves running mechanics, and strengthens the ankle, which reduces the risk of further injury (see table 3).
| Exercise | Prescription |
|---|---|
| Squat-position lean back heel raises while holding on to a frame | 3 sets of 30 reps |
| Seated heel raises with weight behind the knees | 3 sets of 30 reps |
| Seated heel raises with weight more toward the knees | 3 sets of 30 reps |
| Plie calf raises, performed with legs externally rotated | 4 sets of 25 reps |
| Seated plantarflexion on a leg press with fast footwork | 4 sets of 50 reps |
| Quick foot changes, performed as seated plantarflexion on a leg press with single-leg plantarflexion alternating feet | 15-25 reps on each foot |
Summary
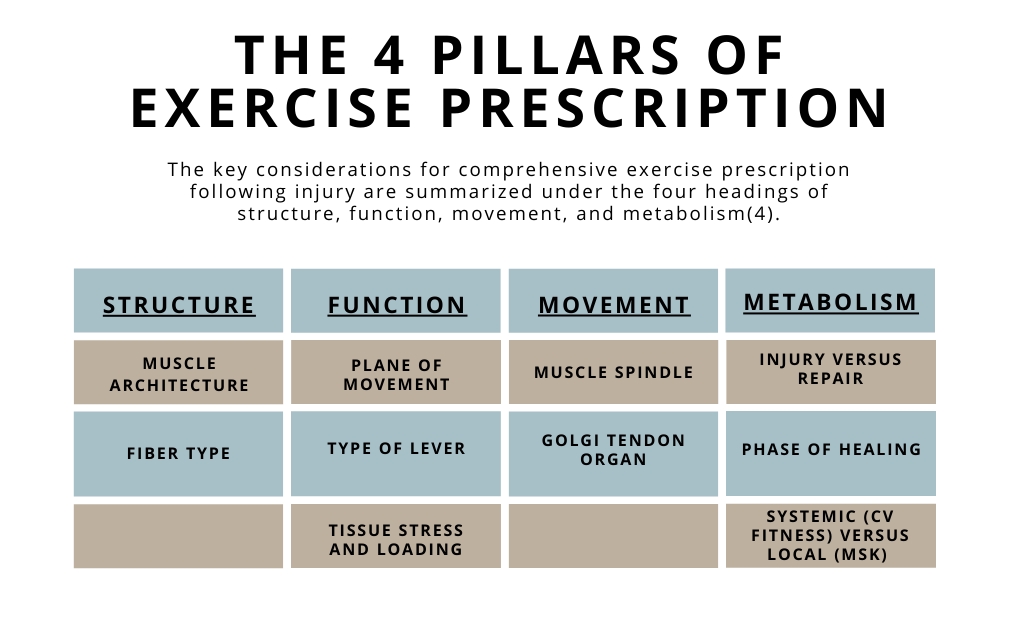
Clinical protocols are diagnosis-specific guidelines for rehabilitation. While they are based on accepted standards of practice, they don’t consider the individual athlete’s needs for returning to their sport and previous level of play. Developing an exercise prescription based on the four pillars ensures that the athlete receives a customized program that prepares them for the best post-injury outcomes (see figure 5).Figure 5: The four pillars of exercise prescription
References
- Essentials of Strength Training and Conditioning. 2016. 4th Ed. Human Kinetics.
- J Physiol.2001 Jul 15; 534(Pt 2): 613–623.
- www.hd-pn.com. Creating athletic movement, James Moore.
- Int J Sports Phys Ther. 2019; 14(1): 14-31.
- J Appl Physiol. 2010; 109(2): 396-404.
- J Musculoskelet Neuronal Interact 2006; 6(2):174-180.
- Br J Sports Med. 2018; 52(10): 622-623.
- Trans. R. Soc. B (2011) 366, 1466–1476
- Br J Sports Med 2009;43:247–251.
- Ex Sport Science Review 2003; 31(2): 73-78.
- 40 Annual Meeting of the American Society of Biomechanics; August 2 – 5 , 2016.
- Europ J of Appl Physiol and Occ Physiol 1980; 44:279-289.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










