Bring pressure to bear on sports injury with blood flow restriction training
Is blood flow restriction training just one more fad? Alejandro Piris Nino takes an updated look at the history, uses, risks, and guidelines of this novel intervention.

Blood flow restriction (BFR) training, originally called Kaatsu (meaning training with added pressure), is the partial restriction of arterial and venous blood flow to exercising muscles to increase muscle mass. The approach started in Japan in the 1960’s after high school student Yoshiaki Sato noticed swelling and discomfort in his calf muscles following prolonged kneeling during a Buddhist ceremony. The sensation in his calves was similar to that produced by strenuous exercise, and he attributed it to decreased blood flow to his muscles. He started experimenting using different types of tubes and tourniquet pressures on his own body (see figure 1). However, it wasn’t until 1983 (and after a few mishaps) that now Professor Sato generalized Kaatsu training for public use(1). Active research continues to expand the body of knowledge concerning BFR and makes it easier to follow an evidence-based approach when
implementing BFR training(2).
Figure 1: Yoshiaki Sato, 1983(1)
Uses
When excessive loading of a muscle is not feasible or contraindicated, BFR is capable of achieving hypertrophy with a significantly decreased load. This approach results in substantial gains in muscle size, strength, and endurance without the strain. Results of its successful use include:
- Improved muscle tone and neck stability in a two-year-old child with West syndrome(3).
- Significantly increased muscle size and strength in elderly adults(4).
- Prevented muscle atrophy in bedridden patients(5).
- Avoided postoperative disuse atrophy in patients with anterior cruciate ligament reconstruction surgery(6).
- Strength gains achieved in patients with metabolic syndrome(7).
- Enhanced resistance training when used with electrical stimulation(8).
- Enriched functional training when used in water-based drills with swimmers(9).
- Employed to treat astronauts with orthostatic intolerance in space flight(10).
In the athletic population, one systematic review demonstrated improvements in performance indicators, such as sprint, agility, and VO2max following low-load BFR use(11). Although the practicality of incorporating BFR training in an elite athlete’s training program is questionable, trainers can utilize it in specific instances (see figure 2). Examples include low-load BFR training following high-load training, during the recovery phase of periodized training, or following an injury. Blood flow restriction training may also benefit athletes who do not tolerate exercise with or have a decreased capacity to recover from high loads, such as Masters athletes (see figure 3)(11).

Figure 2: A professional dancer utilizing BFR training to build strength during the offseason.
Figure 3: 104 Year old doing Kaatsu. Kaatsu Global.
Physiology and theory behind it’s usefulness and effects
The specific mechanisms by which low-load BFR training can facilitate greater muscular gains than training without BFR are not entirely understood. There are several neuromuscular, metabolic, endocrine, and cellular mechanisms involved in the process(12). A few of the coinciding factors reported include increased concentration levels of growth hormone, lactate, insulin-like growth factor-1, and norepinephrine in the blood plasma during BFR training(12). These physiological changes result in the muscle adaptations seen with BFR, such as increases in muscle size, strength, muscle glycogen concentration, and a decrease in muscle ATP concentration. (For more on the physiology of BFR training, see article here.)
Another important adaptation with BFR training is the early activation of fast-twitch muscle fibers. Since BFR training reduces the amount of oxygen supply to muscle fibers, type I fibers cannot sustain the stress applied to the body; therefore, fast-twitch type II fibers are activated much sooner and more intensely(13). For this reason, one could hypothesize that BFR training is especially beneficial for athletes in which fast-twitch fiber recruitment is essential.
Possible Risks
One legitimate concern regarding exercising with a partial tourniquet in the limbs is the formation of venous thromboembolism. However, a systematic review of studies using BFR did not show a significant increase in D-dimer or creatine kinase values, indicators of hypercoagulation(8). A safety study performed in Japan, with over 12,000 subjects, showed that the most common side effect was subcutaneous bleeding (13.1%)(5). The appearance of red or purple spots under the cuffs caused by micro-bleeding (collapsed capillary vessels) beneath the skin usually is harmless and disappears within a few days.
The second most frequent side effect was numbness (1.2%)(5). However, numbness disappeared in all subjects as soon as the cuffs were removed. Of the more severe side effects, seven subjects (0.055%) developed a venous thrombus, and one participant with a suspected pulmonary embolism recovered without intervention(5). In summary, numerous BFR reviewers agree that correct implementation presents no more significant risk of injury than traditional exercise modes(5, 6).
Although injury from BFR training is rare, an adverse event case report of a male ice hockey player was published in 2010(14). Two days after a single first-time bout of ischemic resistance training, the athlete developed extreme muscle soreness in his quadriceps muscle and sought emergency medical care. He was admitted to a hospital without signs of deep vein thrombosis; rather, his blood creatine kinase (CK) levels were elevated to 12,400 U/L. Doctors diagnosed the athlete with rhabdomyolysis. This case report suggests that some subjects produce higher CK levels than others with the same exercise. Therefore, studies examining CK values with different loading protocols of BFR training are needed. The hockey player was discharged from the hospital three days later. After three weeks, he resumed the low-load BFR training and returned to competition seven weeks after the incident(14).
Contraindications to BFR use:
- Cancer
- Acidosis
- Extremities with dialysis port
- Post-mastectomy
- Excessive swelling in the post-surgical limb.
- Infection within extremity
- Increased intracranial pressure
- Impaired circulation
- Lymphedema
- Open fracture or open wound
- Previous revascularization of limb
- Sickle cell anemia
- Severe crush injury
- Vascular graft
- History of deep vein thrombosis
- Venous thromboembolism
- Acute sickness or fever
- Blood pressure > 180/100 mmHg
- Early postoperative period
- Higher class arrhythmia or coronary ischemia
- Pregnancy
Precautions:
- Varicose veins
- Early postoperative period – confirm surgeon’s consent regarding the integrity of the incision
- Prolonged inactivity
- Blood pressure of 160-170/95-99 mmHg
- Age > 60
- BMI > 30 Kg/m2
BFR in the literature
Several systematic reviews suggest that significant muscle mass gains are possible following low-load resistance training with BFR(6,11). Nevertheless, the weekend warrior and the elite athlete should know that a 2018 systematic review on BFR training in clinical musculoskeletal rehabilitation suggested that higher-load exercise without BFR results in greater motor unit recruitment than low-load resistance exercise with BFR(6). Moreover, the same researchers noted that the collateral increase in the strength of connective tissue might not occur with BRF due to the decreased mechanical loading(8). Therefore, although BFR training can be an adequate substitute for high-load training while minimizing pain during the early phase of musculoskeletal rehabilitation, it is neither practical nor recommended for simply improving fitness in healthy individuals(6).
Basic Guidelines
It is imperative to perform a complete and thorough assessment before implementing BFR, including screening for precautions and contraindications. The next step is to determine the correct occlusion cuff size. Refer to the device’s worksheets for recommended sizes based on the circumference of the occluded limb. Measure the limb at the level of cuff placement. Place the cuffs as proximal as possible on the limbs. Position it between the deltoid and biceps muscles on the arms, and at the greater trochanter on the legs. Use the cuffs in either both upper extremities or lower extremities, but never in arms and legs at the same time.
Next, find the amount of pressure required to stop blood flow to a limb. This amount is called the limb occlusion pressure (LOP). Determine the LOP by using a handheld doppler ultrasound machine and a sphygmomanometer and inflate the cuff to the point where blood flow stops. Some BFR-dedicated devices have a pressure monitoring system that determines the LOP, inflates, and deflates the cuffs automatically.
Use a percentage of the LOP during exercise. Perform upper extremity BFR training with a pressure of 40-50% of the LOP, and lower extremity with 60-80% of the LOP(8). For example, if an individual’s lower extremity LOP is 220 mmHg, then 0.80 x 220 mmHg = 176 mmHg. So set the tourniquets to 176 mmHg pressure during the training exercise.
Use BFR with resistance training exercise, aerobic exercise, or passively without exercise (see figure 4). Each modality has extensive evidenced-based protocols for enhanced safety, muscle strength, and hypertrophy. Here is an example of a resistance training program protocol(8):
- Exercise load: Use low loads between 20-40% of an individual’s one-repetition maximum (1RM).
- Volume: A typical set and repetition strategy consists of 30-15-15-15 for a total of 75 repetitions of each exercise(8). It is also common to complete three to five sets to concentric failure. Maintain occlusion pressure throughout the repeated sets and rests. Despite the high number of repetitions, a complete BFR exercise set, and thus occlusion, should not last more than 20 minutes.
- Rest periods: Use rests between sets of 30 to 60 seconds with the BFR sustained throughout.
- Frequency: Two to four times per week for hypertrophy and strength adaptations.
- Duration of training programs: Hypertrophy and strength adaptions occur as early as one to three weeks of training. Most studies utilize time frames of three to eight weeks of duration(8).

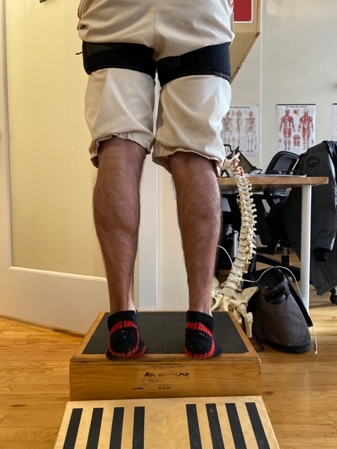
Figure 4: Low-load BFR training in a patient with calf atrophy secondary to Achilles rupture.
References
- Int J KAATSU Training Res. 2005;1:1-5.
- Sports Med. 2015;45(3):313-25.
- Int J KAATSU Training Res. 2015;11:7-12.
- J Geriatr Phys Ther. 2010;33(1):34-40.
- Int J KAATSU Training Res. 2006;2:5-13.
- Br J Sports Med. 2017;51(13):1003-11.
- Int J KAATSU Training Res. 2011;7:7-12.
- Front Physiol. 2019;10:533.
- J Strength Cond Res. 2018.
- Int J KAATSU Training Res. 2006;2:45-52.
- J Sci Med Sport. 2016;19(5):360-7.
- Sports Med. 2014;44(8):1037-54.
- Int J KAATSU Training Res. 2005;1:37-44.
- Clin J Sport Med. 2010;20(3):218-9.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









