Cool it! Why cryotherapy may not get desired results in women.

A recent newsletter explored the effect of post-exercise cryotherapy on the uptake of protein in muscles. While the immediate use of cooling after resistance exercise might diminish muscle building, it is a common strategy used to decrease delayed onset muscle soreness (DOMS) after endurance exercise. Muscle cooling post-exercise comes in many forms:
- Cold water immersion (CWI) of either individual limbs or the whole body by standing in the cooled water;
- Partial-body cryotherapy (PBC) which takes place in a chamber that covers the neck to the feet;
- Whole-body cryotherapy (WBC) within a cooling room;
- Localized cooling with direct application of ice or cold packs.
The body of literature concerning cryotherapy continues to grow; however, most of it is conducted on men. Swiss researchers wondered whether PBC or CWI had a greater effect on specific physiological and performance measures of recovery in women(1). They conducted a randomized controlled, parallel-group study of 28 recreationally active women to see how they responded to PBC and CWI after exercise-induced muscle damage (EIMD) (see figure 1).
The researchers randomly sorted the women into a PBC, CWI, or control group. The subjects first underwent a baseline screening and familiarization with the protocol before performing 100 drop jumps from a .6m box. The PBC group then entered a walk-in cryo-cabinet with head and hands protruding. The exposure was dosed as -60ºC for 30 seconds, then -135ºC for two minutes. The CWI group stood in chest-deep water, cooled to10ºC for 10 minutes. The control group rested for 10 minutes, lying down in a temperature-controlled room.
Figure 1: The experimental protocol
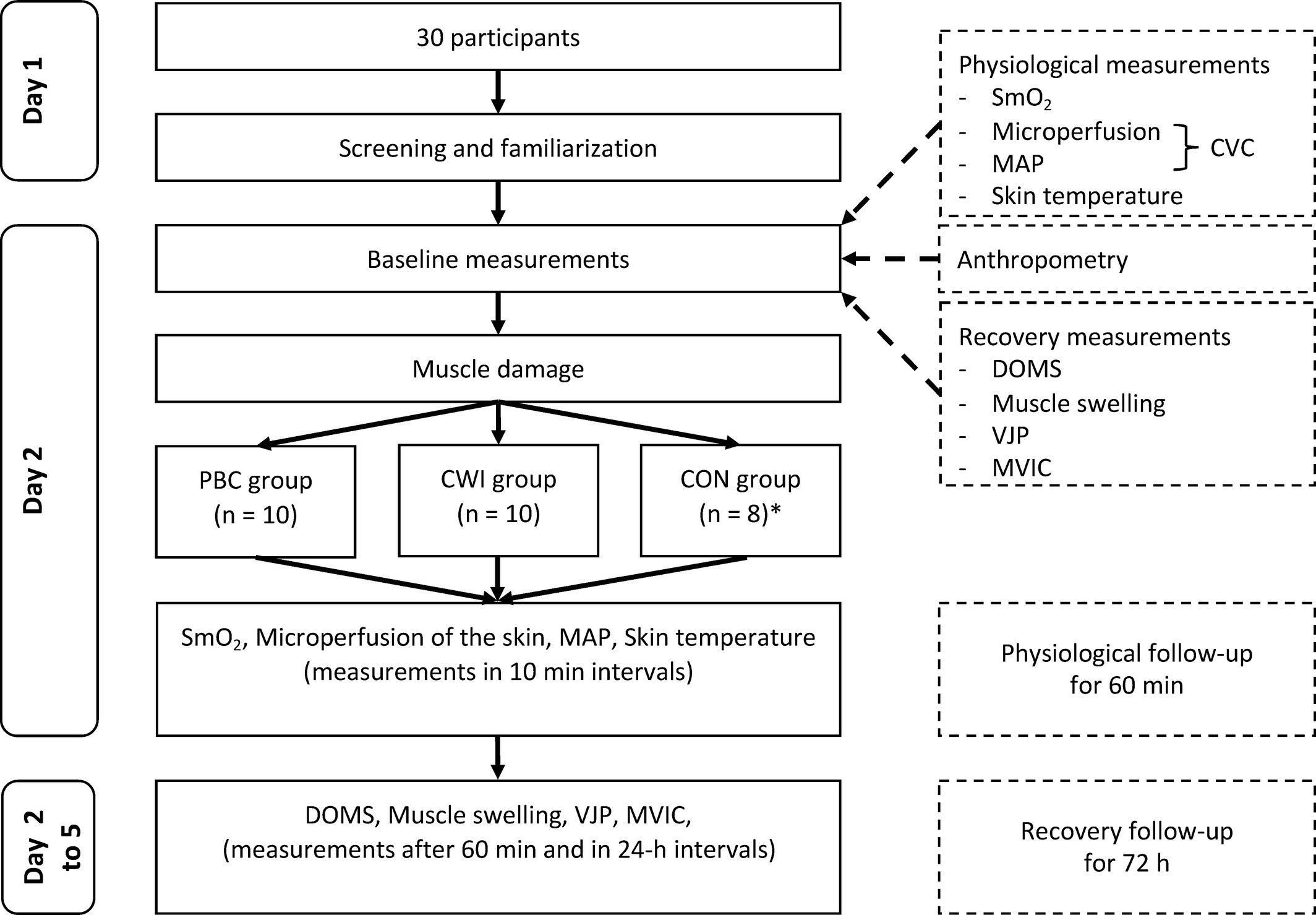
"Schematic representation of the experimental protocol in function of time. CON, control; CVC, cutaneous vascular conductance; CWI, cold‐water immersion; DOMS, delayed onset of muscle soreness; MAP, mean arterial pressure; MVIC, maximum voluntary isometric contraction; PBC, partial‐body cryotherapy; SmO2, muscle oxygen saturation; VJP, vertical jump performance. *n = 2 drop‐outs due to illness"(1)
Immediately after the cooling intervention, the researchers gathered physiological measurements from each group and continued with the measurements every 10 minutes for a total of 60 minutes. Muscle oxygen saturation was measured from the vastus lateralis using near-infrared spectroscopy. Using the mean arterial pressure and a Laser-Speckle Contrast Imaging device, they also calculated cutaneous vascular conductance. Lastly, they computed mean skin temperature from the readings of skin sensors placed in multiple locations on the body.
Recovery and performance measurements were taken at one, 24, 48, and 72 hours after the intervention. Subjects reported their delayed onset muscle soreness (DOMS) using a visual analog scale (VAS) after isometrically holding a squat for three seconds. To determine the amount of muscle swelling present, each participant underwent an ultrasound evaluation of the right anterior thigh. The researchers then measured vertical jump performance (VJP) while the subjects performed counter-movement jumps on a force plate. Each woman also executed a maximum voluntary isometric contraction of their right quadriceps muscle while seated.
Results
The muscle oxygen saturation was significantly less in the PBC and CWI than in the control group for the entire 60 minute evaluation period. As expected, the cutaneous vascular conductance was also lower in the cooling groups, but not significantly so. While the mean arterial pressure was consistent in all groups, the CWI intervention significantly lowered mean skin temperature compared to the PBC and control group.While lower in the PBC and CWI groups compared to the control, the difference in measurements of DOMS did not reach significance. Neither was there a difference in the DOMS measurements between the two interventions. Though all three groups showed evidence of muscle swelling, the cooling didn’t appear to have any effect on this parameter either. The vertical jump measurements of the subjects who received PBC were significantly higher than the control group after 24 hours. However, these values didn’t differ much from those who underwent the CWI intervention.
Practical implications
The authors concluded from this study that PBC and CWI resulted in comparable physiological changes. They also found that despite the small amount of difference in the performance and recovery measurements between the cooling interventions and the control group, the cryotherapy did resolve the DOMS more quickly than no intervention at all. Since the other measures resulted in similar outcomes among the groups, the placebo effect cannot be ruled out since DOMS is a subjective, self-reported measurement.In what might be the most thought-provoking aspect of this study, the same researchers previously conducted a study with a similar protocol on male subjects(2). Comparing the results of the two studies suggests that the greater amount of adipose tissue in females might insulate women from the effects of cooling. Therefore they propose that women may need a more prolonged exposure to cooling in order to obtain the same physiological effects as men.
The other noteworthy finding in this study is that the vertical jump values significantly improved in the PBC group 24 hours after the intervention. For athletes in a multiday competition, PBC may prove a valuable asset to performance recovery.
The authors are to be commended for conducting this study with the awareness of the,
“significantly under-represented female participants in the wider sport and exercise medicine literature.”
They cite limitations to the study, such as lack of control for the stage of the menstrual cycle of the participants, and recognize the protective effect of estrogen on muscles. They also acknowledge that the physical differences between men and women may impact the results of the intervention. The sports medicine literature needs more well-conducted studies like this testing the efficacy of popular interventions while acknowledging the uniqueness of the female athlete.
References
- Scand J Med Sci Sports. 2019,00:1-11
- Scand J Med Sci Sports. 2018;28(3):1252-62
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.






