Osteochondral lesions of the talus: the sinister aftermath of a benign ankle sprain?

Talar dome injuries such as osteochondral lesions of the talus (OLT) can occur following an ankle injury, resulting in ongoing residual ankle pain and functional disability. Initially, OLT was described and classified as ‘transchondral fractures of the talus’ by Berndt and Harty in 1959(1). Since then, however, OLTs are more commonly referred to by other names such as osteochondritis dissecans, talar dome fracture, and flake fracture.
Anatomy and biomechanics
The talar dome is a trapezoid-shaped protuberance of the talus, 2.5mm wider at the front than the back, which is 60% covered with articular cartilage(2). The articulation of the talar dome and the trochlear surface (tibia and fibula) supports the weight of the body. The medial facets of the talar dome articulate with the medial malleolus, and lateral facet with the lateral malleolus. The talar dome has no direct muscle attachments(2); during normal ankle motion of ankle dorsiflexion and plantarflexion, the talar dome (trochlear) rotates and slides against the undersurface of the tibia.Injury mechanisms
An ankle sprain due to rotational forces likely causes OLT injuries. Typically, there is a compressive component to the movement that causes the ankle injury (such as inverting when landing from a jump) in association with a shear-type force, as the talus moves across the tibial plafond or the fibula. An OLT may not be caused or exist at the time of an acute ankle sprain. However, it may develop as a secondary problem due to the laxity of the lateral ankle ligaments following injury. An incongruent talar position due to an unstable ankle means that the lateral talus may experience excessive forces causing damage to the cartilage in that area(3).The cartilage on the talus has less inherent stiffness than the corresponding sites on the tibia (18-37% stiffer on the tibia); therefore it is more vulnerable to harm from shear and compression than the tibia(4). In rare cases involving younger and skeletally inmature individuals, avascular necrosis of the talus may result without trauma(5).
Injury locations
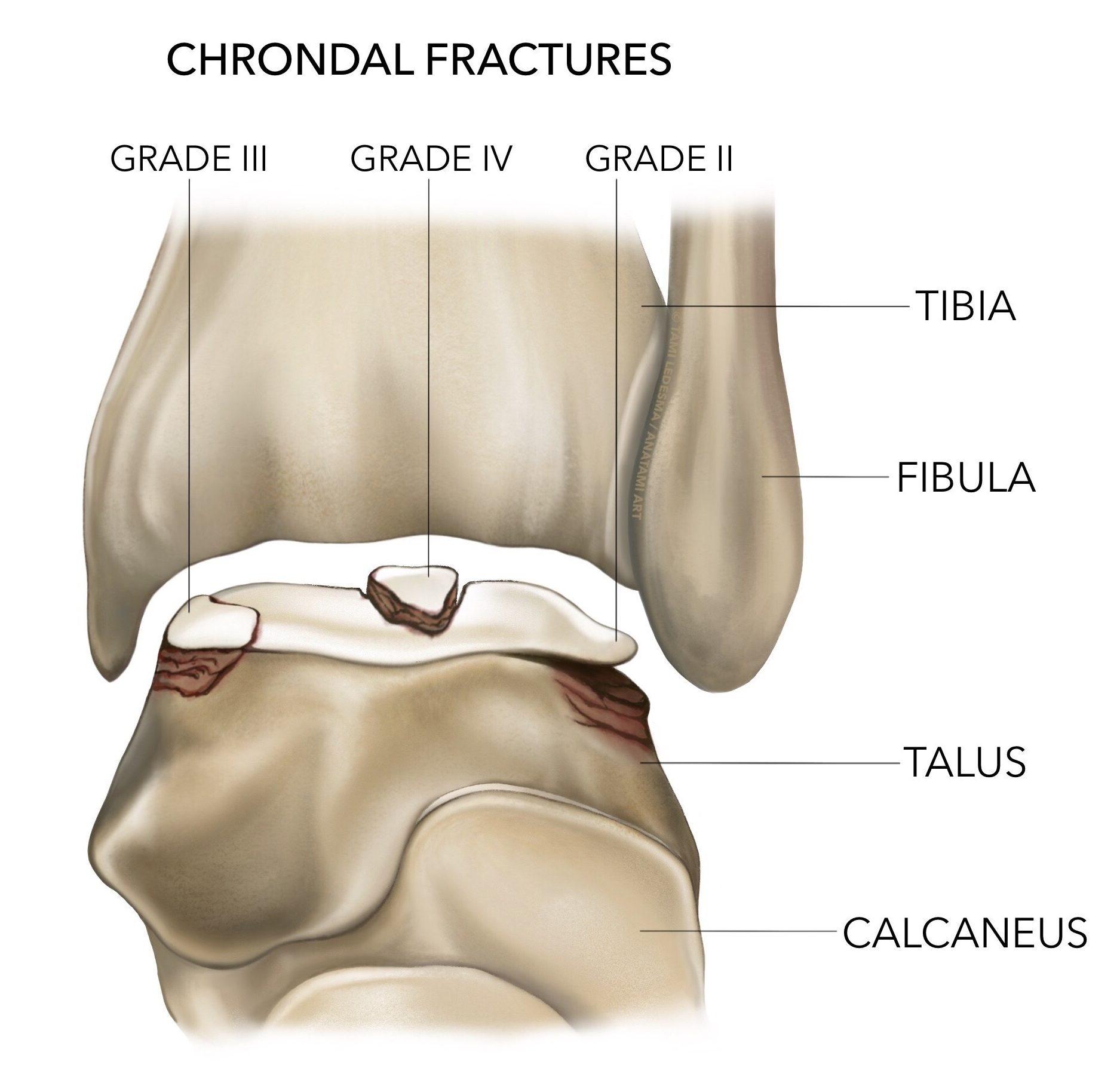
Medial OLT (superomedial) is more common than lateral OLT(3,6), however lateral OLT is more often associated with trauma compared with medial OLT (100% versus 64%)(7), and more likely in patients with chronic ankle instability(3). Most OLTs occur in either the central middle or lateral middle part of the talus (80%)(8). Lateral lesions caused by the shear force created with inversion sprains are often more shallow and wafer shaped compared with medial lesions(6). Medial lesions associated with trauma usually involve inversion with plantarflexion and external rotation which cause deeper cup-shaped lesions (see figure 1)(6).Figure 1: Anatomy of OLT injuries
How common is OLT?
Some studies have looked at the incidence of OLT in post-traumatic ankle injuries. These findings can be summarized as follows:- X-ray evidence showed a 4% rate (in a sample of 121 patients) with persistently symptomatic ankles(9).
- The incidence of bilateral OLT has shown to be around 10%(10).
- In long-term ankle pain patients, OLT shows up in 81% of patients - as a previously undiagnosed pathology(11).
- OLT represents only 4% of all osteochondral lesions in the body. These are more common in knees and elbows(12).
Diagnosing OLT
*Signs and symptoms- Typically, an OLT is not detected in the initial post-injury period unless there has been a large displaced osteochondral fragment. They usually present later after the soft tissue injury to the ligaments has healed. Patients will often progress well and quickly following an ankle sprain. However, once they start to increase the impact loading on the ankle, the signs and symptoms become more prevalent. Typical signs and symptoms of OLT are(13):- Pain, swelling, and feelings of stiffness in the ankle.
- Ankle pain described as dull and achy.
- Mechanical symptoms such as catching and locking.
- Tenderness to palpation over the talus.
- Decreased range of motion (this often is a crucial diagnostic feature).
- Ankle effusion.
- Pain with either or both dorsiflexion and inversion.
However, based on imaging studies compared with the above complaints, an OLT can be present without the physical signs mentioned above(14).
*Imaging studies– X-rays are usually done as anteroposterior, oblique views, mortise views in full plantar flexion. However, X-rays generally have a low sensitivity for picking up OLT unless a definitive displacement is present(14); therefore MRI is preferred. The main benefit of MRI is the soft tissue detail that it can show, and it has a sensitivity of 96% and a specificity of 96% for OLT(14). It can reveal an area of low-intensity on T1 imaging (suggestive of sclerosis in the talar bed)(15), while T2 images may show a signal rim of varying intensity between the talar bed and the osteochondral fragment (suggestive of an instability of the osteochondral piece). The majority of classification studies have compared MRI with arthroscopic findings to allow the clinician to classify the severity of the OLT based on MRI findings (see classification below). CT scanning is another modality, showing the bony architecture of the talus better than MRI. However, a CT scan is unable to see early lesions present only in the cartilage(16). CT can be coupled with single-photon emission computerized tomography (SPECT) to view activity in and around the OLT, such as deep bone edema (17).
Injury classification
The classification of OLT depends on the investigation of choice. Different terminology is used depending on whether consists of an X-ray (4 levels), CT (5 levels), MRI (6 levels), or arthroscopy (6 levels). Mintz et al. developed a combined classification system of both MRI and arthroscopy (see table 1)(18)a.| Stage | Features/definition |
|---|---|
| 0 | Normal cartilage |
| I | Abnormal cartilage signal but intact |
| II | Fibrillation or fissures in cartilage, not extending to the underlying bone |
| III | Cartilage flap present or bone exposed |
| IV | A loose non-displaced osteochondral fragment |
| V | Displaced osteochondral fragment |
Conservative treatment
Non operative treatment is commonly the primary choice of intervention in non-displaced OLT such as type I and II lesions above. Displaced intra-articular osteochondral fragments are usually immediate candidates for surgery. Some factors do lead to more favorable outcomes in conservative treatment. These are as follows(16):- Lesions smaller than 15mm
- Contained lesions
- Anterolateral lesions
Factors that lead to poor prognosis are:
- Age over 40
- Deep lesions (>7mm)
- Large lesions (>15mm)
- Cystic lesions
- Medial talar lesions
- Higher BMI
- History of trauma to the ankle
- Long duration of symptoms
- Presence of osteophytes
The typical framework for conservative treatment is as follows(16):
- An initial period of non-weight bearing or partial weight-bearing from three weeks to a month. This allows unloading of the injured cartilage so that bone marrow edema can resolve. (Some clinicians advocate early weight bearing in milder type-I and II lesions).
- Protected full weight-bearing period of 6-10 weeks in a restricted motion boot (CAM boot).
- Regaining passive range of motion into dorsiflexion and plantarflexion.
- Strengthening of muscles that perform ankle plantarflexion, dorsiflexion, eversion, and inversion.
- Functional lower limb retraining.
- Return to running and sport function.
To bear weight or not?
Logically speaking, a patient with an acute ankle sprain that may have an OLT of significance will most likely be in a degree of pain and discomfort. Therefore, they are more than likely to be initially non-weight bearing, and thus unloading a potentially damaged talar dome cartilage. It is likely that type I and II lesions, which are the more benign and can tolerate early protected weight-bearing, will progress through the weight-bearing stages much faster than more severe ankle sprains which may result in a Type III+ injury.Early access to MRI after the injury (24-48 hours) usually reveals any potential OLT. In elite sports, the sports medicine team consults and determines the exact length of time to be either non-weight-bearing or protected weight-bearing based on the degree of soft tissue injury and the presence of an OLT.
Operative treatment
The potential surgical options for OLT are quite exhaustive and beyond the scope of this article. Each surgery type has its own defined rehabilitation protocol. In summary however, the types of surgery performed include(17):- Excision of loose fragment.
- Excision and curettage of the cartilage rim.
- Excision and curettage of the cartilage rim, with microfracture/drilling to stimulate fibrocartilage repair.
- Excision and curettage of the cartilage rim, with packing of particulate juvenile cartilage.
- Excision and curettage of the cartilage rim, with autogenous bone grafting.
- Retrograde drilling.
- Fixation of the osteochondral fragment (usually anterolateral fragments).
- Autologous chondrocyte implantation - implant of a cultured periosteal patch.
- Osteochondral autograft transplantation.
- Osteochondral allograft transplantation.
- Metal inlay implant.
In summary
Osteochondral lesions of the talus are a reasonably infrequent cause of long-standing ankle pain and stiffness and are often the result of a severe ankle sprain type injury. The presence of an osteochondral lesion may initially go undetected and may manifest many months after the initial ankle injury. The severity of the injury is best assessed using MRI. Low-grade lesions are managed with initial weight bearing modifications and therapeutic interventions. Those that fail to respond may be candidates for various surgical options.References
- J Bone and Joint Surgery Am. 1959. 41-A; 988-1020.
- BMJ Open Sport and Exercise Medicine. 2018. 4. E000318.
- Foot and Ankle International. 2015. Vol 36(9); 1050-1057.
- Ann Biomechanical Eng. 1995. 23(5); 697-704.
- 2014. 2; 115-123.
- Foot Ankle Int. 2009; 30(8): 723-7.
- Orthop Trans. 1990;14: 172-8.
- J Bone and Joint Surgery. 1980; 62A: 646-652.
- J Bone Joint Surg Am. 1955; 37-A(6): 1237-43.
- Foot Ankle Clinics North America. 2003, 8, 73-90.
- J Bone Joint Surg Am. 1980; 62(1): 97-102.
- Foot Ankle Int. 2007; 28(2): 154-61.
- Foot Ankle Int. 2010; 31(1): 90-101.
- J Bone Joint Surg Br. 2005; 87(1): 41-6.
- 1997. 165; 775-780.
- The Orthopaedics Journal. 2017, 119supp-4, M15), pp 743-761.
- Foot Ankle Int. 2011; 32(3): 233-8.
- 2003; 19(4): 353-9.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









