Piriformis: a contentious syndrome?
The piriformis muscle (PM) is well-known in the fraternity of sports medicine as a significant muscle in the posterior hip. It is a muscle that has a role in controlling hip joint rotation and abduction, and it is also a muscle made famous due to its ‘inversion of action’ in rotation. Furthermore, the PM also grabs attention due to its role in the contentious ‘piriformis syndrome’, a condition implicated as a potential source of pain and dysfunction, not only in the general population but in athletes as well.
Relevant Anatomy
The name piriformis was first coined by Belgian Anatomist Adrian Spigelius in the early 17th century. Its name is derived from the Latin word ‘pirum’ meaning ‘pear’ and ‘forma’ meaning ‘shape’ – ie a pear shaped muscle (see Figure 1)Contemp Orthop 6:92-96, 1983..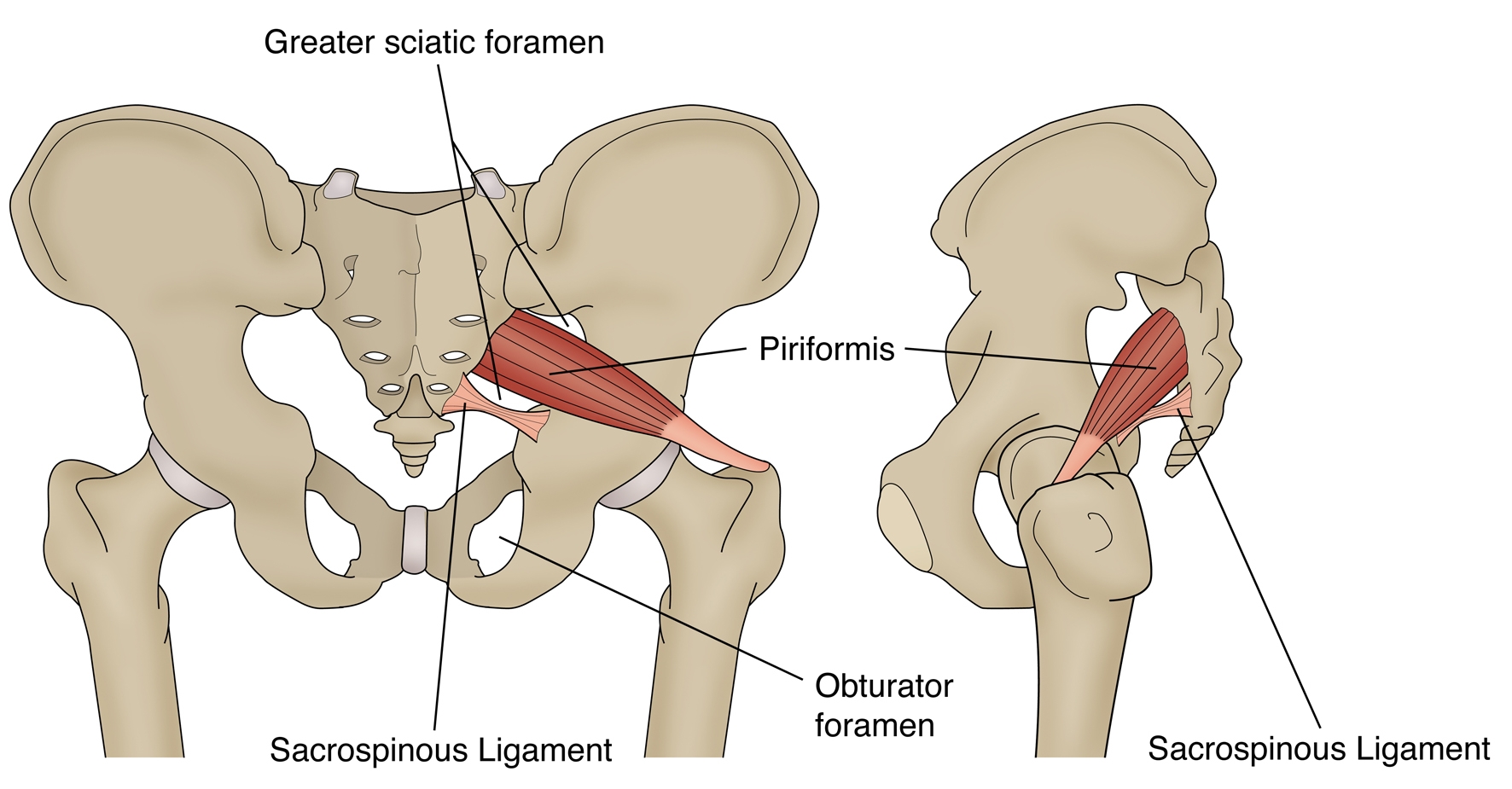
The PM originates on the anterior surface of the sacrum and is anchored to it by three fleshy attachments between the first, second, third and fourth anterior sacral foraminaSimons et al (1999) Travell and Simons’ Myofascial Pain and Dysfunction. Volume 1 Upper Half of the Body (2nd edition). Williams and Wilkins. Baltimore.. Occasionally its origin may be so broad that it joins the capsule of the sacroiliac joint above and with the sacrotuberous and/or sacrospinous ligament belowAnesthesiology; 98: 1442-8, 2003. Joumal of Athletic Training 27(2); 102-110, 1996..
PM is a thick and bulky muscle, and as it passes out of the pelvis through the greater sciatic foramen, it divides the foramen into the suprapiriform and infra-piriform foraminaJournal of Clinical and Diagnostic Research. Mar, Vol-8(3): 96-97, 2014.. As it courses antero-laterally through the greater sciatic foramen, it tapers out to form a tendon that is attached to the superior-medial surface of the greater trochanter, commonly blending with the common tendon of the obturator internus and gemelli musclesClemente CD: Gray’s Anatomy of the Human Body, American Ed. 30. Lea & Febiger, Philadelphia, 1985 (pp. 568-571)..
The nerves and blood vessels in the suprapiriform foramen are the superior gluteal nerve and vessels, and in the infrapiriforma fossa are the inferior gluteal nerves and vessels and the sciatic nerve (SN)Journal of Clinical and Diagnostic Research. Mar, Vol-8(3): 96-97, 2014.. Due to its large volume in the greater sciatic foramen, it has the potential to compress the numerous vessels and nerves that exit the pelvis.
PM is closely associated with the other short hip rotators that lie inferior such as the superior gemellus, obturator internus, inferior gemellus and obturator externusSimons et al (1999) Travell and Simons’ Myofascial Pain and Dysfunction. Volume 1 Upper Half of the Body (2nd edition). Williams and Wilkins. Baltimore.. The primary difference between the PM and other short rotators is the relationship to the SN. The PM passes posterior to the nerve whereas the other otators pass anterior (see figure 2).
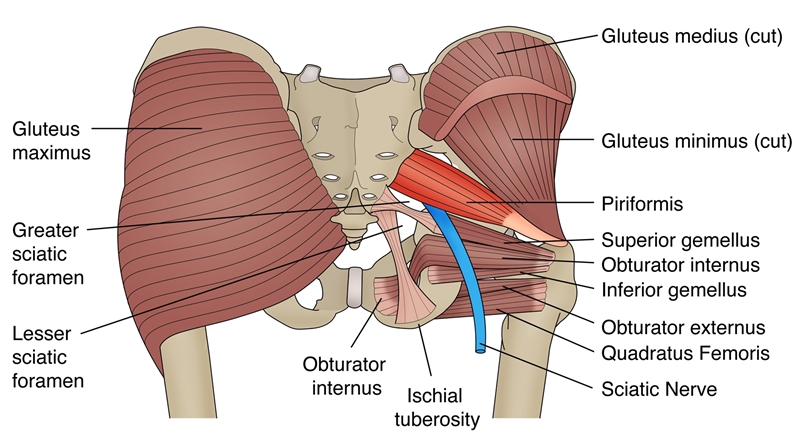
Variants
A few anatomical variants have been found with the PM:- Additional medial attachments to the first and fifth sacral vertebrae and to the coccyxMed J Malaysia 36:227-229, 1981..
- The tendon may fuse with the gluteus medius or minimus above, or superior gemellus belowMed J Malaysia 36:227-229, 1981..
- In less than 20% of cases it is divided into two distinct portions through which part or all of the sciatic nerve may passMed J Malaysia 36:227-229, 1981..
- It may blend with the posterior hip joint capsule as a conjoined tendon with the obturator internusJ Bone Joint Surg;92-B(9):1317-1324, 2010..
- The distal attachment of the PM has shown to vary in dimensions and position on the supero-medial surface of the greater trochanter. It can span a distance of between 25-64% of the anterior-posterior length on the greater trochanter, with 57% attaching more anterior and 43% more posteriorJ Ortho Sports Phys Ther. 2011;41(1):A84, 2011..
- Pine et al (2011) studied the insertion point extensively and found that four types of insertion existed and these were classified based on the relationship to the obturator internusClin Anat;24:70-76, 2011.. The variability in position and breadth of the distal attachment of the PM muscle may influence the validity of the concept known as ‘inversion of action’ (see below).
The other hotly debated issue is the relationship between the PM and the SN. The conclusion is that there are several anatomical variations of the PM and its SN relationship. The sub-types of this variation includeMed Sci Monit, 2015; 21: 3760-3768, 2015. J Bone Joint Surg Am 1938, 20:686-688, 1938. Journal of Clinical and Diagnostic Research. 2014 Aug, Vol-8(8): 7-9, 2014.:
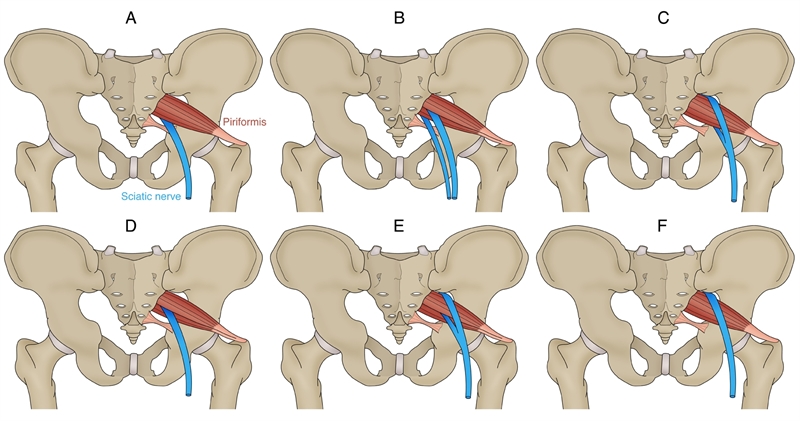
- Type 1 (A below). Typical pear shape muscle with the nerve running anteriorly and inferiorly to this (in 70%-85% of cases).
- Type 2 (B below). The PM is divided into two parts with the common peroneal nerve running between the two parts and the tibial nerve running anterior and below (found in 10-20% of cases).
- Type 3 (C below). The peroneal portion loops over the top of the muscle and the tibial portion is below (found in 2-3% of cases).
- Type 4 (D below). Undivided nerve passing through the PM (occurs in about 1% of cases).
It is also believed that two other very uncommon variations occur (see E and F below).
Type A is the most common variation, showing the SN passing below the PM
Functional considerations
The primary functional roles of the PM are;- Hip external rotationKapandji IA. The Physiology of Joints. 2nd ed. London: Churchill Livingstone; 1970: 68..
- Abductor at 90 degrees of hip flexionKapandji IA. The Physiology of Joints. 2nd ed. London: Churchill Livingstone; 1970: 68..
- In weight-bearing, the PM restrains the femoral internal rotation during stance phase of walking and runningSimons et al (1999) Travell and Simons’ Myofascial Pain and Dysfunction. Volume 1 Upper Half of the Body (2nd edition). Williams and Wilkins. Baltimore..
- Assists the short hip rotators in compressing the hip joint and stabilising the jointClemente CD: Gray’s Anatomy of the Human Body, American Ed. 30. Lea & Febiger, Philadelphia, 1985 (pp. 568-571)..
- As it can exert an oblique force on the sacrum, it may produce a strong rotary shearing force on the sacroiliac joint (SIJ). This would displace the ipsilateral base of the sacrum anteriorly (forward) and the apex of the sacrum posteriorlyJ Am Osteopath Assoc 73:799-80 7,1974..
As the PM is the most posterior of the hip external rotators due to its attachment on the anterior surface of the sacrum, it has the greatest leverage to exert a rotation effect on the hip joint. It is often seen clinically that the PM appears to be tight and hypertonic, while the other short hip rotators that are closer to the axis of rotation become inhibited and hypotonic.
Inversion of action
The most contentious issue related to the function of the PM is its ‘reversal-offunction role’ or ‘inversion of action’ role. Many authors have suggested that as the hip approaches angles of 60-90 degrees and greater, the tendon of the PM shifts superiorly on the greater trochanter. As a result, its line of pull renders it ineffective as a hip external rotator; however it does contribute to internal hip rotation. Therefore it reverses its rotation role at high hip flexion anglesKapandji IA. The Physiology of Joints. 2nd ed. London: Churchill Livingstone; 1970: 68. J Biomechanics. 1999;32:493-50, 1999. Phys Therap. 66(3):351-361, 1986..The function of the PM at varying joint angles is an important consideration for the clinician who is evaluating and treating ‘piriformis syndrome’. Often it has been advocated to stretch the hip into flexion, adduction and external rotation to stretch the PM over the glutes by utilising the ‘reversal of function’ concept.
However, more recent anatomical dissection studies have shown that the attachment of the PM onto the greater trochanter can be variable and in some instances it may insert in a position whereby it is unable to reverse its function, for example in a more posteriorly placed attachmentJournal of Student Physical Therapy Research. 8(4), Article 2 110-122, 2015.. Therefore, stretching the PM into external rotation when the hip is flexed beyond 90 degrees – based upon reversal of function – would be ineffective as a treatment or misleading as an examination techniqueJournal of Student Physical Therapy Research. 8(4), Article 2 110-122, 2015..
MSK dysfunction and PM syndrome
Many decades ago, the role that the PM played in creating sciatic-like symptoms was first suggested by Yeoman (1928) when it was considered that some cases of sciatica may originate outside the spineLancet. 212: 1119-23, 1928.. This was supported soon after when Freiberg and Vinkle (1934) successfully cured sciatica by surgically dividing the PMJ Bone Joint Surg Am 16:126–136, 1934.. Based on cadaver dissections Beaton and Anson (1938) gave the hypothesis that the spasm of the PM could be responsible for the irritation of the SNJ Bone Joint Surg Am 1938, 20:686-688, 1938..The term ‘piriformis syndrome’ was first coined by Robinson in 1947Am J Surg 1947, 73:356-358, 1947. and was applied to sciatica thought to be caused by an abnormality in the PM (usually traumatic in origin) with emphasis on ruling out more common causes of sciatica such as nerve root impingement from a disc protrusion. It soon became an accepted clinical entity – but with no consensus about the exact clinical signs and diagnostic tests to differentiate it from other sources of sciaticaJ Neurol Sci; 39: 577–83, 2012. Orthop Clin North Am; 35: 65-71, 2004.
Piriformis syndrome can be defined as a clinical entity whereby the interaction between the PM and SN may irritate the SN and produce posterior hip pain with distal referral down the posterior thigh, imitating ‘true sciatica’. Isolating the dysfunction to this region usually follows exclusion of the more common causes of buttock pain and sciatica.
More specifically, complaints of buttock pain with distal referral of symptoms are not unique to the PM. Similar symptoms are prevalent with the more clinically evident lower back pain syndromes and pelvic dysfunctions. Thus, a thorough evaluation of these regions must be performed to exclude underlying pathologyJoumal of Athletic Training 27(2); 102-110, 1996.. It has been suggested that piriformis syndrome’ is responsible for 5-6% of cases of sciaticaArch Phys Med Rehabil; 83: 295-301,2002. Arch Neurol. 63: 1469–72, 2006.. In the majority of cases, it occurs in middle-aged patients (mean age 38 yr)J Bone Joint Surg Am; 81: 941-9,1999. and is more prevalent in womenPostgrad Med 58:107-113, 1975..
Pathogenesis of piriformis syndrome (PS)
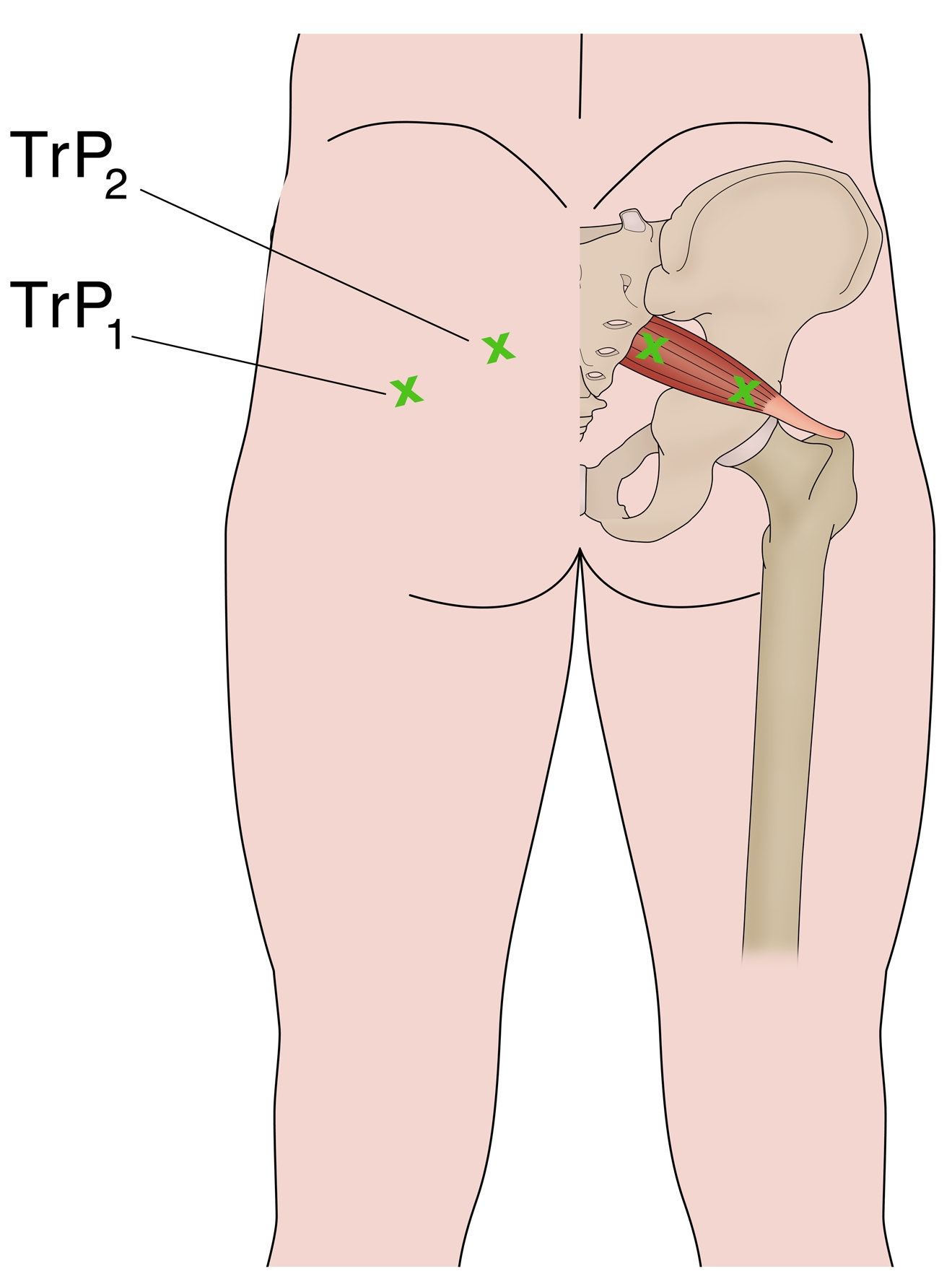
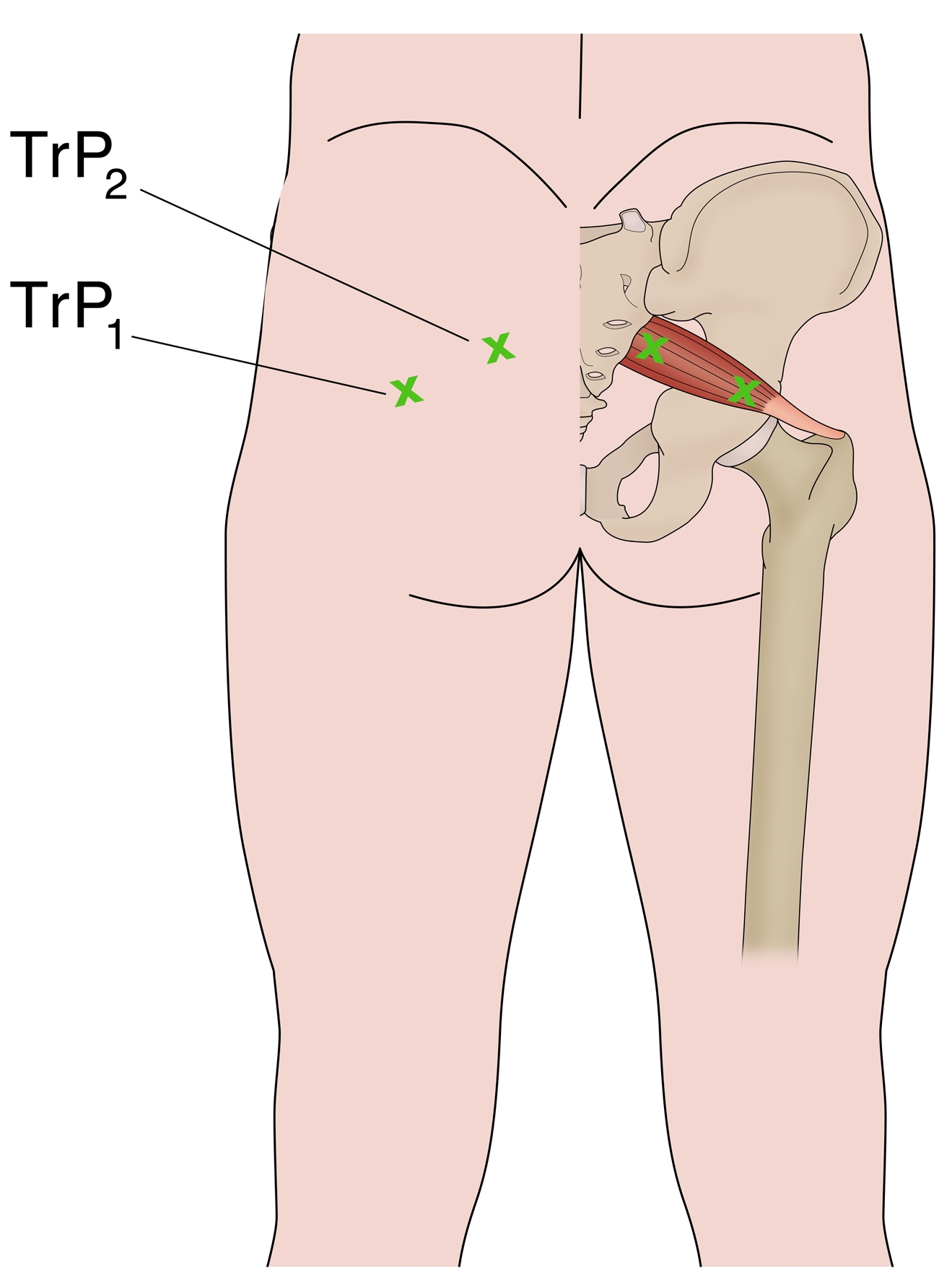
PS may be caused by or relate to three primary causative factors;- Referred pain due to myofascial trigger points (see Figure 4)Simons et al (1999) Travell and Simons’ Myofascial Pain and Dysfunction. Volume 1 Upper Half of the Body (2nd edition). Williams and Wilkins. Baltimore. Postgrad Med 58:107-113, 1975. Can J Anesth/J Can Anesth;60:1003–1012, 2013. Arch Phys Med Rehabil 69:784, 1988.. Examples include tight and shortened muscle fibres precipitated by muscle overuse such as squat and lunge movements in external rotation, or direct traumaJ Am Osteopath Assoc 73:799-80 7,1974.. This increases the girth of the PM during contraction, and this may the source of the compression/entrapment.
- Entrapment of the nerve against the greater sciatic foramen as it passes through the infrapiriform fossa, or within a variant PMCan J Anesth/J Can Anesth;60:1003–1012, 2013. Muscle Nerve; 40: 10-8, 2009..
- SIJ dysfunction causing PM spasmCan J Anesth/J Can Anesth;60:1003–1012, 2013. J Orthop Sports Phys Ther;40(2):103-111, 2010..
Janvokic (2013) has presented a number of causative factors in PSCan J Anesth/J Can Anesth;60:1003–1012, 2013.;
- Gluteal trauma in the sacroiliac or gluteal areas.
- Anatomical variations.
- Myofascial trigger points.
- Hypertrophy of the PM or spasm of the PM.
- Secondary to spinal surgery such as laminectomy.
- Space occupying lesions such as neoplasm, bursitis, abscess, myositis.
- Intragluteal injections.
- Femoral nailing.
Symptoms
Typical symptoms reported in piriformis syndrome include:- A tight or cramping sensation in the buttock and/or hamstringBr J Sports Med;35:209–211, 2001..
- Gluteal pain (in 98% of cases)Man Ther 2006; 10: 159-69, 2006..
- Calf pain (in 59% of cases)Man Ther 2006; 10: 159-69, 2006..
- Aggravation through sitting and squattingEur Spine J. 19:2095–2109, 2010., especially if the trunk is inclined forward or the leg is crossed over the unaffected legJournal of Orthopaedic Surgery and Research, 5:3, 2010..
- Possible peripheral nerve signs such as pain and paraesthesia in the back, groin, buttocks, perineum, back of the thigh (in 82% of cases)Man Ther 2006; 10: 159-69, 2006..
Physical findings and examinations
- Palpable spasm in and around the PM and obturator internus and external tenderness over the greater sciatic notch (in 59-92% of cases)Man Ther 2006; 10: 159-69, 2006. Eur Spine J. 19:2095–2109, 2010.. The patient is placed in the Sims position. The piriformis line overlies the superior border of the PM and extends from immediately above the greater trochanter to the cephalic border of the greater sciatic foramen at the sacrum. The line is divided into equal thirds. The fully rendered thumb presses on the point of maximum trigger-point tenderness, which is usually found just lateral to the junction of the middle and last thirds of the line.
- Hip flexion with active external rotation or passive internal rotation may exacerbate the symptomsJournal of Orthopaedic Surgery and Research, 5:3, 2010..
- Positive SLR that is less than 15 degrees the normal sideMuscle & Nerve. November. 646-649, 2003..
- Positive Freiberg’s sign (in 32-63% of cases)Man Ther 2006; 10: 159-69, 2006. Eur Spine J. 19:2095–2109, 2010.. This test involves reproducing pain on passive forced internal rotation of the hip in the supine position – thought to result from passive stretching of the PM and pressure on the sciatic nerve at the sacrospinous ligament.
- Pacers sign (in 30-74% of cases)Man Ther 2006; 10: 159-69, 2006. Eur Spine J. 19:2095–2109, 2010.. This test involves reproducing pain and weakness on resisted abduction and external rotation of the thigh in a sitting position.
- Pain in a FAIR positionMan Ther 2006; 10: 159-69, 2006.. This involves the reproduction of pain when the leg is held in flexion, adduction and internal rotation.
- An accentuated lumbar lordosis and hip flexor tightness predisposes one to increased compression of the sciatic nerve against the sciatic notch by a shortened piriformisKopell H, Thomnpson W. Peripheral Entrapment Neuropathies. Huntington, NY: Krieger, 1975:66..
- Electro-diagnostic tests may prove useful (see below).
Investigations
Conventional imaging such as X-ray, CT scan and MRI tend to be ineffective in diagnosing piriformis syndrome.However, some value may exist in electrodiagnostic testing.
It is beyond the scope of this paper to discuss in detail the process of electrodiagnostic testing; the reader is directed to references for more a more detailed description of how these tests are administeredEur Spine J. 19:2095–2109, 2010. Journal of Orthopaedic Surgery and Research, 5:3, 2010. Arch Phys Med Rehabil;73:359–64, 1992.. However the purpose of these tests is to find conduction faults in the SN. Findings such as long-latency potentials (for example the H reflex of the tibial nerve and/or peroneal nerve) may be normal at rest but become delayed in positions where the hip external rotators are tightenedJ Bone Joint Surg Am; 81: 941-9,1999. Journal of Orthopaedic Surgery and Research, 5:3, 2010. Arch Phys Med Rehabil;73:359–64, 1992..
It is accepted that the tibial division of the SN is usually spared, the inferior gluteal nerve that supplies the gluteus maximus may be affected and the muscle becomes atrophiedJ Bone and Joint Surg, 74-A:1553-1559, 1992.. However testing of the peroneal nerve may provide more conclusive results as is more likely to be the impinged portion of the SN. The H-wave may become extinct during the painful position of forced adduction-internal rotation of the affected legJournal of Orthopaedic Surgery and Research, 5:3, 2010..
The ‘myth’ of piriformis syndrome
Stewart 2003 argues that piriformis syndrome is an often over-used term to describe any non-specific gluteal tenderness with radiating leg painMuscle & Nerve. November. 644-646, 2003.. He argues that only in rare cases is the PM implicated in nerve compression of the SN to truly qualify as a piriformis syndrome. He cites only limited evidence and cases where the diagnosis of piriformis syndrome can be made.- Compressive damage to the SN by the PM. Stewart cites studies whereby in few isolated studies, the SN was seen to be compressed by the PM in instances such as hypertrophy of the muscle, usual anatomical anomalies such as a bifid PM, and due to compression by fibrous bands.
- Trauma and scarring to the PM leading to SN involvement; it is possible that rare cases of true Piriformis Syndrome have been caused by direct heavy trauma to the PM due to a blunt trauma to the muscle. This is termed ‘posttraumatic PS’.
McCory (2001) supports this argument by stating that it is more likely that (given the anatomical relationship of the PM to the various nerves in the deep gluteal region) the buttock pain represents entrapment of the gluteal nerves, and the hamstring pain entrapment of the posterior cutaneous nerve of the thigh, rather than the SN aloneBr J Sports Med;35:209–211, 2001. This would explain the clinically observed phenomenon in the absence of distal sciatic neurological signs. Whether the PM is the cause of the compression has not been clearly established. It is possible that the obturator internus/gemelli complex is an alternative cause of neural compression. He suggests using the term ‘deep gluteal syndrome’ rather than piriformis syndrome.



Treatment
When it is believed that a piriformis syndrome exists and the clinician feels that a diagnosis has been made, the treatment will usually depend on the suspected cause. If the PM is tight and in spasm then initially conservative treatment will focus on stretching and massaging the tight muscle to remove the PM as being the source of the pain. If this fails, then the following have been suggested and may be attemptedJ Neurol Sci; 39: 577–83, 2012. Journal of Orthopaedic Surgery and Research, 5:3, 2010.:- Local anaesthetic block – usually performed by anaesthesiologists who have expertise in pain management and in performing nerve blocks.
- Steroid injections into the PM.
- Botulinum toxin injections into the PM.
- Surgical neurolysis.
Here, we will focus on therapist-directed interventions such as stretching of the PM and direct trigger point massage. It has always been advocated that PM stretches are done in positions of hip flexion greater than 90 degrees, adduction and external rotation to utilise the ‘inversion of action’ effect of the PM to isolate the stretch to this muscle independent of the other hip external rotators.
However, recent evidence from Waldner (2015) using ultrasound investigation discovered that there was no interaction between hip flexion angle and the thickness of the PM tendon in both internal and lateral hip rotation stretching – suggesting that the PM does not invert its actionJournal of Student Physical Therapy Research. 8(4), Article 2 110-122, 2015.. Furthermore, Pine et al (2011)J Ortho Sports Phys Ther. 2011;41(1):A84, 2011. and Fabrizio et al (2011)Clin Anat;24:70-76, 2011. in their cadaveric studies found that the PM insertion is a lot more complex and varied than first thought. It is possible that the PM may invert its action only in some subjects but not others.
Therefore, due to the disagreements and confusions over the ‘inversion of action’ concept, it is recommended that the clinician ‘covers all bases’ and performs two variations of a PM stretch – stretches in flexion, adduction and external rotation and stretches in flexion, adduction and internal rotation. Examples of these stretches are given in figures 5-7 above.
Trigger points and massage (see Figure 8)
The best approach to palpate the PM trigger points is in the position suggested by Travel and SimonsSimons et al (1999) Travell and Simons’ Myofascial Pain and Dysfunction. Volume 1 Upper Half of the Body (2nd edition). Williams and Wilkins. Baltimore. and this is shown below. In this position, the clinician can feel for the deep PM trigger points and apply a sustained pressure to alleviate the trigger points – and also apply a flush massage to the muscle in this position. In this position the large gluteus maximus is relaxed and it is easier to feel the deeper PM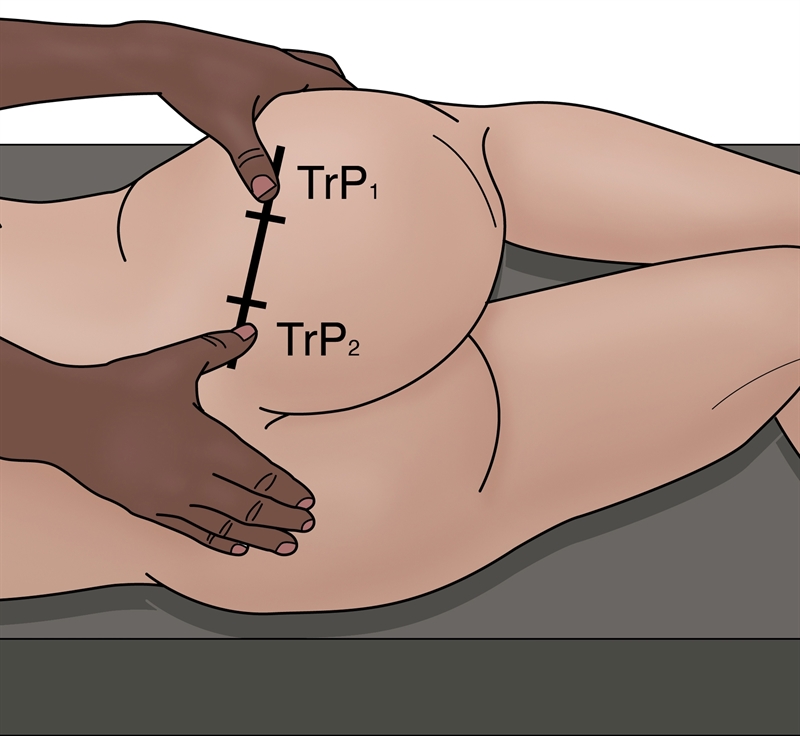
Summary
The PM is a deep posterior hip muscle that is closely related anatomically to both the sacroiliac joint and the sciatic nerve. It is a hip external rotator at hip flexion angles of neutral to 60 degrees of hip flexion, an abductor when in flexion and also contributes to hip extension.It has been previously accepted that the PM will ‘invert its action’ or ‘reverse its function’ after 60 degrees of flexion to become a hip internal rotator. However, recent ultrasound and cadaveric studies has found conflicting evidence that this ‘inversion of action’ may in fact not exist.
PM is a muscle that is a dominant hip rotator and stabiliser, and thus has a tendency to shorten and become hypertonic. Therefore, stretching and massage techniques are best utilised to reduce the tone through the muscle. Furthermore, it has also been implicated in compression and irritation of the sciatic nerve – often referred to as piriformis syndrome’.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









