Taking a crack at groin pain

Groin pain accounts for up to 30% of all sports injuries(1). Treating this ailment requires careful sleuthing from the sports injury clinician. The list of differential diagnoses to consider for groin pain is lengthy, including:
- Hip, pelvic, or knee joint pathology
- Bone pathology
- Tendon or ligament strain
- Muscle belly strain or tear
- Sports hernia
- Abdominal or gastrointestinal disorders
- Nerve entrapment
- Genitourinary causes
- Vascular disorders
Treatment of groin pain in athletes is often prolonged and unsatisfactory (see figure 1). Confounding the issue, groin pain often radiates to the hip as well. One disorder that usually gets overlooked when exploring the cause of groin and hip pain is impairment at the thoracolumbar junction (TLJ). Why would trouble here manifest as groin or hip pain?
Figure 1: Decision tree for the differential diagnosis of groin pain(2)
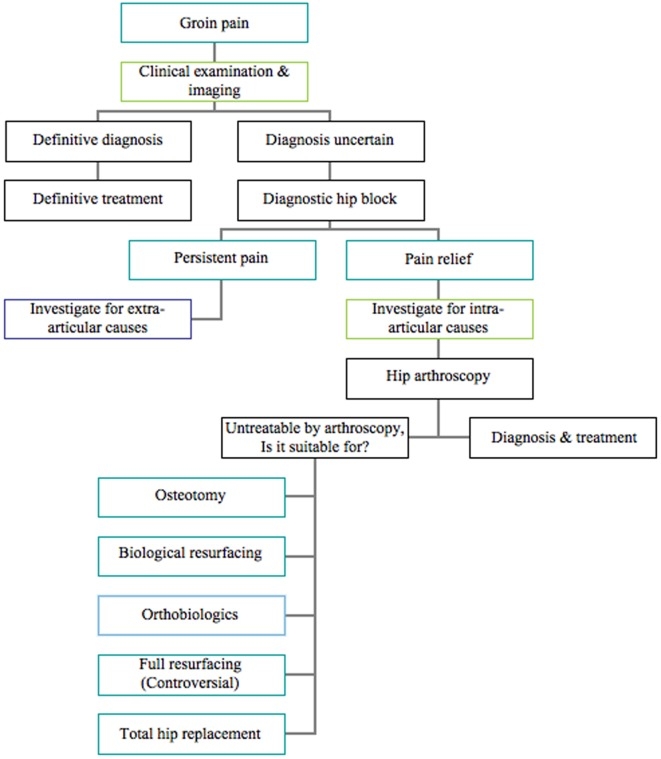
Athletes often complain of prolonged groin pain. Once clinicians eliminate life and limb-threatening possibilities, athletes are left with vague approaches to address musculoskeletal causes.
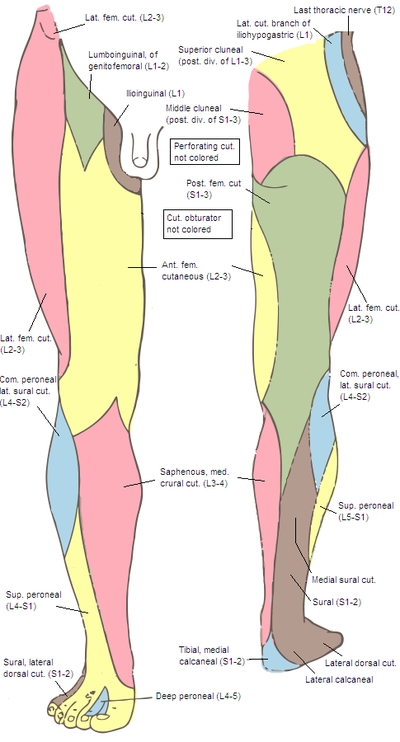
Also called dorsal ramus-mediated pain or Maigne syndrome, TLJ syndrome often presents without low back pain (LBP). Rather, pain radiates from the TLJ facets along the dorsal ramus of T11 to L1 vertebrae, or the cutaneous branches of these nerves (see figure 2). Along this distribution, pain can extend to the groin, lower abdomen or pelvis, lateral hip, and inner thigh.
Figure 2: Dermatomes for thoraco-lumbar and sacral nerves
Focusing on active adults with complaints of chronic groin pain, a multicenter case series in the United States highlights three cases of referred pain from TLJ syndrome(3). Each patient underwent previous sessions of typical treatment approaches, including physical therapy, with little relief. All experienced functional decline and desired to return to their active lifestyle. One subject sited the onset of pain after a ‘bad golf swing’ where he hit the ground forcefully with his club. Another noticed the pain after participating in an exercise class.
Eliminating other causes of pain, the treating therapists employed a manual therapy and exercise approach to treat the pain and loss of function in the presumed TLJ syndrome. The patients received both rotational and posterior to anterior mobilization and manipulation techniques to the lower thoracic and upper lumbar spine. The subjects also performed home exercises to increase the mobility and stability in the area. Exercises included:
- Open book trunk rotation
- Thoracic extension / flexion over a foam roller
- Cat / Cow
- Lion stretch
- Seated thoracic rotation
At baseline, the subjects reported six, seven, and five out of 10 on a visual pain score respectively. At discharge, all patients reported zero pain. All patients demonstrated a meaningful improvement in their function after six, eight, and four physiotherapy visits, and all met their initial goals.
Oh Snap
This study was a retrospective look at select cases from different centers and different therapists. The subjects were aged 65-76, however, they were active adults who’s pain was brought on by exercise. A soccer player who kicks a player instead of the ball may experience the same type of jolting TLJ force as one of the subjects did by hitting the ground with a golf club.When athletes complain of groin pain, the most serious and threatening causes must first be ruled out. Often times when they’ve been cleared, the origin is assumed to be a musculoskeletal issue in the hip and pelvis. Despite therapy, groin pain can continue to sideline athletes. Therefore, consider TLJ syndrome when treating unresolved groin pain.
References
- 2015;15(1):3-8
- SICOT J. 2015; 1: 16.
- 2019 Aug;49(8):611-19
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.






