What lies beneath: relieving fear of the retrocalcaneal bursa

Pain at the posterior heel is common in many athletes such as runners, tennis players and crossfit athletes. Although it is more commonly found in older athletes, young athletes may also experience posterior heel pain. Pain in this area may originate in the insertional Achilles enthesis (the attachment to the posterior calcaneus), the retrocalcaneal bursa (RCB) and the subcutaneous calcaneal bursa. Often all three of these co-exist and some consider these to be inter-related pathologies.
Anatomy and biomechanics
The retrocalcaneal bursa (RCB) and its primary anatomical features were first described by Rossler in 1896(1). It was described as a disc-like cavity moulded over the posterior-superior, and filled with a viscous fluid. Its anterior wall is composed of fibrocartilage, which is connected to the calcaneus. The posterior wall meanwhile is blended into the Achilles tendon epitenon, from which it is hard to distinguish bursa from epitenon (see figure 1). Adipose tissue makes up the superior margin. The bursa itself is fluid filled and is rich in hyaluronate(2,3). The primary purpose of the retrocalcaneal bursa is to protect the Achilles tendon from friction and shear forces against the calcaneus(4).More recently, Rufani et al determined that the RCB was lined by a periosteal cartilage on the calcaneus side, and the tendon side was a sesamoid fibrocartilage(5). An analogy would be that the RCB is ‘sandwiched’ between two cartilage plates. As both the periosteal cartilage and the sesamoid fibrocartilage are paired and opposite each other, they may function in unison to protect the bone from rubbing directly against the tendon, creating a compression zone (which is characteristic of other tendinopathies)(6,7).
Figure 1: Anatomy of the RCB
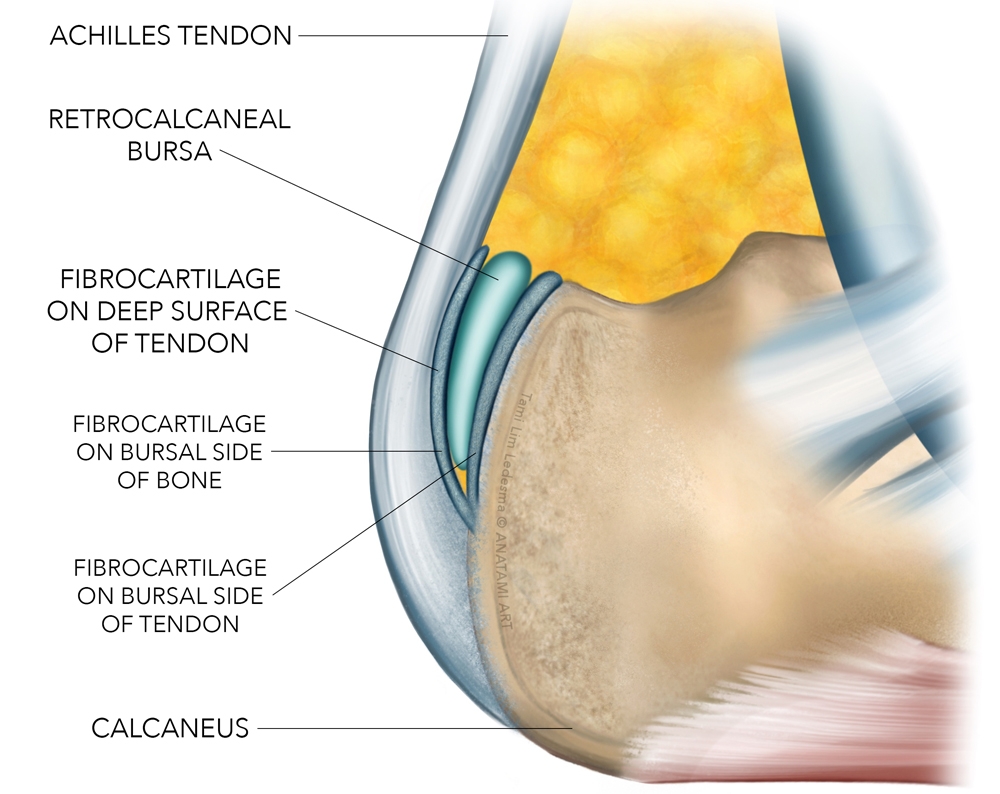
Histological analysis shows that degeneration in one cartilage is accompanied by corresponding degeneration in the other. This is explained as the fibrocartilages being compressed against each other in dorsiflexion. As these cartilages line the bursa, the degeneration in these cartilages may be considered to co-exist and be part of the same clinical entity as bursa pathology(5,8). The tendon, bursa and the Achilles attachment are therefore all interrelated components, which protect the tendon from undue compression against the posterior calcaneus(9). Some suggest that the more vertical the posterior wall of the calcaneus, the greater the likelihood of the tendon being pressed against the bone(5). Furthermore, injection studies reveal a direct connection between anteroinferior portion of the Achilles tendon and the RCB. This may represent a weak zone, which allows overlapping pathologies of tendon injury and RCB pathology(10).
Pathogenesis
Injuries to the RCB are related to the attachment of the Achilles tendon to the calcaneus. These represent an assemblage of assorted overlapping pathologies(11). Therefore, it is difficult to pry apart RCB injury from Achilles tendon injury as they very often co-exist. As mentioned above, in positions of full dorsiflexion, both the RCB and the Achilles tendon are both compressed against the calcaneus (see figure 2). This loading is greater with high-tensile loads. In summary, these injuries represent a chronic load-dependant pathology, which is caused by dorsiflexion compressive forces and high tensile forces from running, jumping and landing.In acute settings, an inflammation of the RCB may be caused by deposits of calcium pyrophosphate dehydrate (CPPD). This is a crystal deposition disease, which originates in the Achilles tendon and involves the fibrocartilage in the anterior wall of the bursa (because it connects to the calcaneus). The presence of CPPD is also typical in other inflammatory arthropathies.
Figure 2: Compressed retrocalcaneal bursa
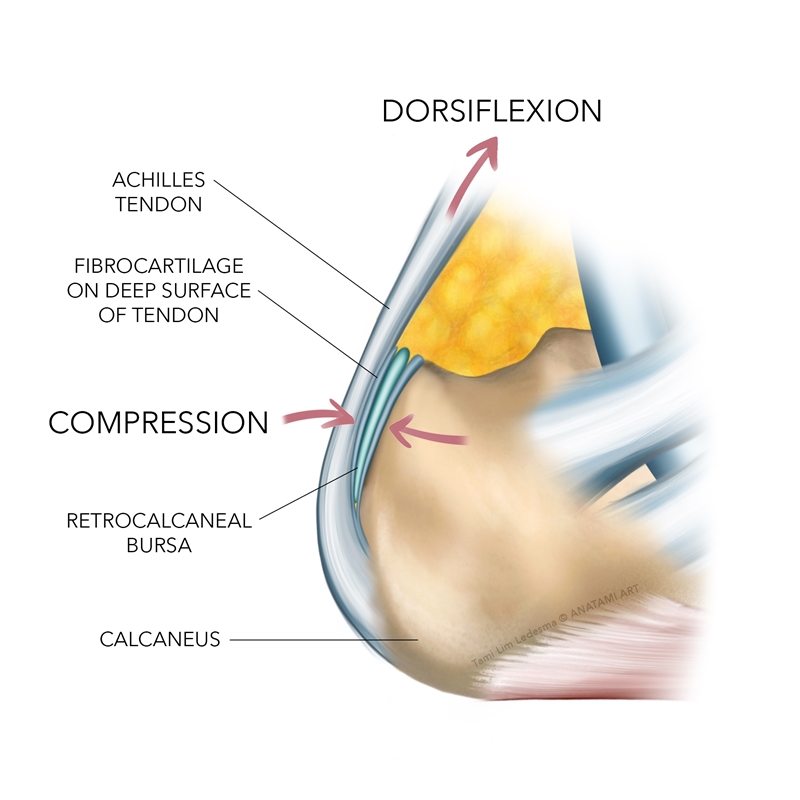
Signs and symptoms
The most common/typical signs of RCB are as follows(12):- Localized posterior heel pain on low load activities such as heel raises and full dorsiflexion.
- Tenderness on palpation, usually medial and lateral to the Achilles tendon at the posterior-superior calcaneus.
- Localized swelling and a prominence of the Achilles tendon proximal to its insertion(2,3).
- Pain on dorsiflexion (this leads to compression of the tendon against the bursa and the calcaneus).
As mentioned earlier, Achilles tendinopathy and RCB often co-exist, and some researchers have postulated that the conditions are one and the same(8). Therefore, it is very difficult to ascertain whether the insertional Achilles enthesis or the RCB is the source of pain, and the clinician may need imaging to determine exactly the contribution of RCB versus Achilles tendon in recalcitrant cases.
Using imaging modalities, MRI may show fluid and thickening. On X-ray, a retrocalcaneal recess is usually absent in the presence of a RCB and may be diagnostic of the RCB(2,3). The explanation for the loss of the retrocalcaneal bursa recess was investigated by Canosa et al(2). When X-ray and MRI images of patients with and without RCB were investigated, it was discovered that in non symptomatic patients, the retromalleolar fat pad migrates distally into the bursa relative to the calcaneus during plantarflexion and fills the angle between the Achilles tendon and the bone. This shows up as a retrocalcaneal radiolucency. In the presence of bursal fluid, the excessive bursa size would prevent the migration of the fat pad and would eventually push it forward and upwards.
Management
*ConservativeThe conservative management of a RCB is identical to an insertional Achilles tendinopathy and follows a similar format and timeframe(8):
- Pain relief stage – isometrics
In the initial stages of a painful RCB and/or Achilles insertion, isometrics are used to relieve pain. The use of isometrics has been studied extensively by Rio et al in the management of patella tendinopathy(13). The primary features of an isometric program to relieve pain are as follows.
- Long holds of 45 seconds. These are repeated five times with long rest periods (1-2 minutes).
- Compressive positions to be discovered (avoid dorsiflexion and remain in mid plantarflexion).
- No greater than a 3/10 pain score while performing the isometric.
- Progress or regress the load based on pain. Very painful RCB/Achilles insertions may only tolerate seated calf raise holds with no load. Low irritability problems may tolerate single leg loaded calf raise isometrics.
- Exercises are repeated every 4-6 hours daily.
- Isometrics can be used to relieve pain before an exercise session – eg may be used prior to running
- Isotonic strength-endurance stage
As the athlete/patient improves, the pain in the Achilles insertion reduces and he/she becomes more functional (they may now be able to walk and run with less than 3/10 pain). The next stage in the spectrum of management is to get the tendon and enthesis stronger by adapting to load. This can be performed in traditional ways used in strength programs. The athlete may choose one or a number of different exercises to include in a strength program, such as weighted standing calf raises (traditional calf raise machine or Smith machine), seated calf raise machine or stair walking. The important points to outline are:
- Load should be set as high as can be tolerated, but without greater than 3/10 pain score and without compromising form and technique.
- Exercises to be performed 3 times per week.
- Exercises best performed AFTER running or training sessions.
- Start with endurance type sets and reps (3 x 15-20 reps) and every 2-3 weeks drop the repetitions to increase load (eg moving to 3 x 12, 3 x 8, 3 x 6 etc.).
- Avoid full dorsiflexion (full heel drop) in the early stages. Only include deep dorsiflexion in the athlete who will be exposed to high loads in dorsiflexion.
- Energy storage stage
High-demand athletes will need to progress to energy storage type exercises to build the energy storage capacity of the tendon. Recreational athletes who participate in group fitness sessions 2-3 times per week may not have a need for this stage! Energy storage exercises are defined as an exercise that requires a fast concentric phase with only a slow or non-existent eccentric stage. Examples of exercises are fast stair walks/running, box step up, triple extension movements or simply faster calf raises. These are only needed once or twice per week depending on other training demands.
- Energy storage and release stage
These are only appropriate for training high-demand athletes. Often these may be difficult to perform within a competitive season due to the risk of overloading the RCB and tendon, negatively impacting training and competition. Often, the act of training and competing may be sufficient in itself at this stage. Direct interventions for this stage are best left to out-of-season programs. Examples of exercises are:
- Sled/prowler pushes
- Plyometrics
- Box jumps and jump downs
- Skipping
- Change of direction training
Other treatment options that have been studied and which may be effective (but will not be discussed in this article) are shockwave therapy, polidoconol injections, corticosteroid injections, heel raises in the shoe to reduce dorsiflexion compression and finally surgical excision of the bursa.
Summary
RCB is a commonly co-existing pathology with insertional Achilles tendinopathy. The primary causative factors are excessive compressive load during dorsiflexion coupled with high tensile forces due to calf muscle contraction. Load variables such as volume and intensity of running and jumping loads are a key factor and often spikes in loading precipitate the onset of RCB inflammation and insertional Achilles tendinopathy. Management follows a similar format to management of Achilles tendinopathy.References
- Dtsch Z Chir 1896; 42: 274-91
- Ann Rheum Dis 1988;47:910-912
- Ann Rheum Dis 1983; 42: 171-5
- Knee Surg Sports Traumatol Arthrosc 2010;18:638-643
- Journal of Orthopaedic Research 1995; 585-593
- J Anat. 1998; 193 (Pt 4): 481 – 94
- Br J Sports Med.2012 Mar;46(3):163-8
- Brukner P and Kahn K (2017) Clinical Sports Medicine, 5th Edition. Volume 1: Injuries. McGraw-Hill Education Australia
- Radiology 1977; 125: 355-66.
- Bone Joint Res 2015;6:446–451.
- Knee Surg Sports Traumatol Arthrosc 2011;19:835-841.
- Clin Podiatr Med Surg2005;22:19-43.
- Br J Sports Med 2015. Oct;49(19):1277-83
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









