Is telehealth the answer for clinicians in a new post-COVID-19 era?

The global community is currently transitioning to a new way of living through social distancing, which presents both new opportunities and challenges. The use of telehealth consultations, used within physiotherapy settings in the last two decades, is now even more relevant as a result of the COVID-19 pandemic. Telehealth includes telephone or video conferencing to provide healthcare to patients, without direct contact(1).
With five billion people globally using a mobile phone every day, and four billion having access to the internet daily, the scope for remote healthcare is fast developing(2). Although some clinicians may question its efficacy, telehealth consultations can have a positive effect on chronic disease, quality of life, clinical indicators, and reduce the use of secondary healthcare services(3).
Future predictions estimate that by 2030, 75% of healthcare appointments will take place through digital media(2). Even as society re-opens, telehealth is here to stay. Therefore, adapting healthcare services to the new technology while maintaining quality is vital. Some healthcare providers have reported concerns about losing face-to-face contact with patients. However, these concerns may arise from a lack of information and awareness within healthcare settings as to the correct implementation of telehealth(4).
Staying in touch
During times of movement restrictions such as in the current COVID-19 pandemic, healthcare providers need to find effective means of staying in contact with their patients. It may well be that a patient has a particular connection with a clinician, but they’re isolated in a different location. Telehealth can provide the link that preserves the continuity of care between the provider and the patient. Telehealth also provides a solution to maintaining appropriate social distancing while saving travel time, costs, and reducing the environmental impact of travel(5). Moreover, patients seem willing to engage in this new medium, which can positively affect their health management.In one study, researchers from the University of Queensland, Australia, asked 85 patients who had chronic musculoskeletal conditions about their perceptions of telehealth(5). Fifty-three percent of patients said they were willing to use telehealth if it saved money and travel time. Sixty-five percent of patients who were in paid employment said they were more likely to use telehealth if it reduced time away from paid work. These results prove that telehealth consultations may be viewed positively by many, although, attitudes may vary across different cultures.
In another study, researchers compared pain and physical function in two groups of 25 patients with osteoarthritis of the knee joint(1). Groups were randomly divided into either a clinically-treated group or a telehealth-treated group, and all patients were treated three times a week for six weeks. In the telehealth group, patients were guided through an exercise rehabilitation program via mobile phone after being assessed initially in the clinic setting. The results indicated significant reductions in pain in both groups after six weeks of rehabilitation and no significant differences in pain between the groups. Although this was a small sample size, it nevertheless shows that telehealth physiotherapy appointments carried out remotely can be useful for patients.
Remote examination and assessment
During a regular examination, clinicians gather information by listening to the patient’s description of the problem and conducting a physical exam, which often involves putting their hands on the patient. This physical touch can provide reassurance to some patients, or be off-putting to others. Often the same information can be conveyed through close observation of the quality of movement.During a video call, the therapist still interviews the patient to obtain their subjective history. However, there isn’t the added advantage of assessing a patient when they’re unguarded as they walk from the waiting room to the treatment room. A therapist also doesn’t have the opportunity to shake their hand with a warm welcome and potentially meet a family member. So when you log on to the meeting room in a video conference capacity, greet the client with a friendly smile to create that bond early on and help them feel at ease.
To enable an effective appointment via a video call, establish that the patient is in the right setting for an appointment (see panel 1). Secondly, use clear and simple communication with everyday words rather than industry-speak. This clarity avoids confusion and gives the patient confidence that you know what you’re doing. In the clinic setting, a therapist may use scientific words while demonstrating an action. The patient ignores the language and focuses on imitating the motion. Or, the clinician may manually move the body part and position it themselves. Without that opportunity, language becomes essential for getting good information from the evaluation.
For instance, “Could you turn and face your fireplace, please?” is much easier for the patient to interpret than, “Could you turn 90° to your right?” It is important to remember that the patient may be stepping out of their comfort zone by embracing video technology. Using too much technical language could increase their anxiety and frustration with the service, reducing its effectiveness. When asking the patient to assume a particular position, speak slowly, precisely, and with a sense of calm.
Panel 1: Some simple telehealth appointment guidelines for physiotherapists
- Ensure there are clear lines of communication between the patient and the healthcare provider -ie no delay in sound or white noise in the background (as this could make gathering information difficult).
- Ensure there’s no glare from windows that makes the patient appear as a silhouette. A clear view of their fascial expressions and mouth help therapists understand their speech and understanding.
- Ensure there is no background noise – eg from other family members, dogs, mobile phones etc.
- Ensure the camera is adjusted to an angle so that the therapist can obtain the most effective view. Ask for adjustments to the camera angle as needed to allow for a change in perspective, for example, as the patient moves from a standing posture to a supine lying position.
- Ask the patient to wear appropriate clothing.
- Ensure there are no trip hazards or something that is of danger to the patient as they move about the room.
The therapist may need different camera angle views of the patient while performing a clinical test (see figure 1-3). Ideally, the patient will be in full view, allowing visualization of the entire body and the limb involved. Using mobile technology, rather than a desktop, gives the patient the flexibility to adjust camera angles easily. Thus, ask patients to change the views as needed, such as when needing a transition from a frontal to a sagittal view to evaluate joint angles.
Optimizing viewing angles
Figure 1
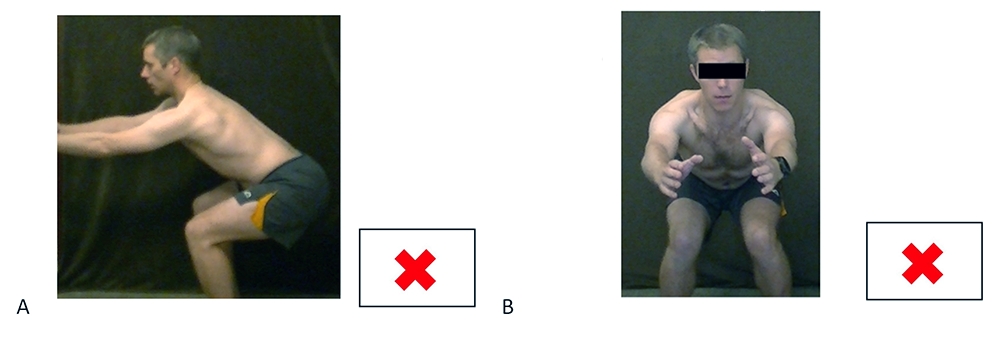
- A) View of a squat from the side view seems appropriate but is of poor quality as the whole body isn’t in view.
- B) View of a squat from the frontal plane reveals a different quality of technique (observe the collapse of the left knee), but it is also a poor image as the feet aren’t in view.
Figure 2
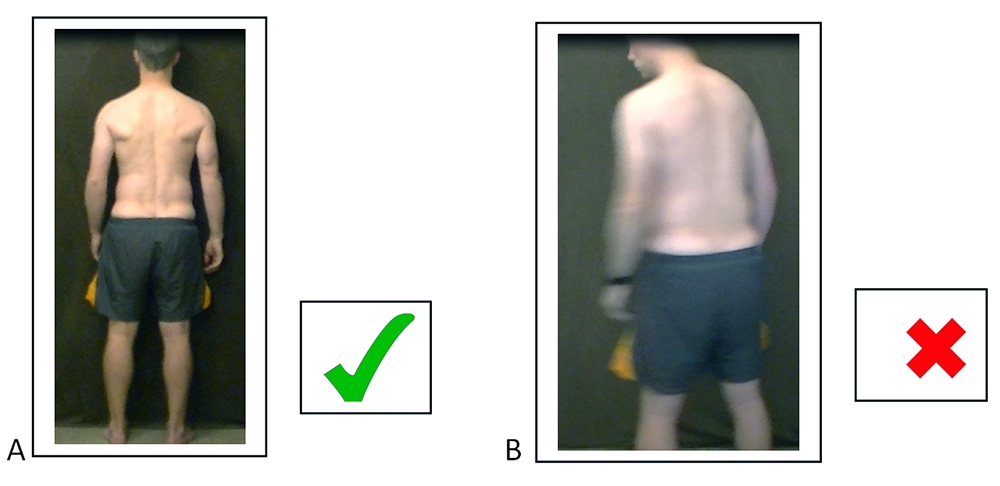
- A) Correct angle for viewing posture with an enhanced image quality;
- B) Incorrect angle and poor picture quality to view posture. In situations like this, clarify communication with the patient until they assume the right position. Note: Sometimes, poor internet connection may not allow for a high-quality picture.
Figure 3
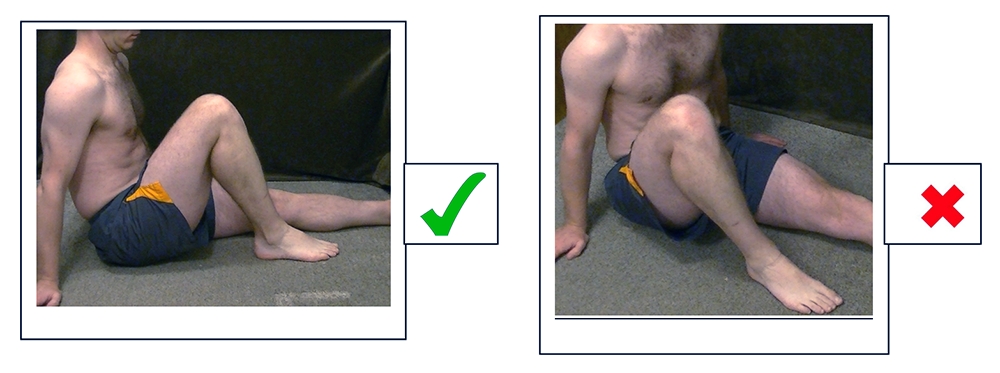
- A) Correct angle for measuring active knee flexion.
- B) Incorrect angle for measuring active knee flexion.
It is useful to view the patient’s face when possible, as facial expressions are a non-verbal expression of pain or discomfort. At the same time, the clinician must be versatile and work with the space available to the patient, remembering that some home living spaces aren’t adaptable in terms of camera angles and space. Ask the patient if they have wall space, stationary or swivel chairs, or steps that may function as pieces of equipment to aid a home exercise program. Of course, the patient may already have typical workout items such as a Swiss ball, foam roller, dumbbells or resistance bands, but other household items can also be used to great effect.
Conclusion
Telehealth can positively influence people’s lives during a time of social distancing, reaching those unable to attend healthcare appointments due to distance or travel restrictions. It is essential for clinicians to adapt their treatment approach but to maintain their patient-centered approach. A telehealth appointment shouldn’t be considered as a substandard service compared to face to face appointments; indeed, many patients will likely prefer this approach. Once life returns to what will be a new way of living following COVID-19, telehealth will likely remain and evolve in frontline healthcare.References
- Int J of Telerehab, 2013, 5, 1, 11-20.
- www.csp.org.uk/frontline/article/digital-healthcare-realities-today-possibilities-tomorrow
- BMJ, 2012, 344, e3874.
- J of Pharmacy, Mar, 2017, 25, 3, 203 – 209.
- J Telemed Telecare.2018, Aug, 24, 7, 445 – 452.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.






