Medial Collateral Ligament Strain: Where, How and Why
In the first of a 2-part article, Chris Mallac describes the anatomy and biomechanics of the medial knee ligaments, the implications of injury, and how these injuries are identified and graded.
The superficial medial collateral ligament (s-MCL) is one of the most commonly injured structures at the knee, in both contact sports and sports that involve sharp cutting and direction changes. It may also be associated with more severe injuries to the medial knee such as deep medial collateral ligaments (d-MCL) and posterior oblique ligament(1-6).
The majority of MCL tears are isolated. These injuries occur predominantly in young individuals participating in sports activities, with the mechanism of injury involving valgus knee loading, external rotation, or a combination of these. These are common in sports like skiing, ice hockey, rugby, and soccer, all of which involve movements requiring knee flexion and valgus loading and potential of direct contact to the outside of the knee(7-9).
The treatment of medial-sided knee injuries has moved away from aggressive surgical treatments towards non-operative management. Surgery is generally reserved for chronic MCL deficiency that has failed non-operative treatment, or more severe and complex injuries. The majority of athletes who sustain an MCL injury will achieve their pre-injury activity level with non-operative treatment.
Anatomy
The iconic anatomy reference point for understanding the medial knee joint stabilizers comes from Stan James at Iowa State University, who performed a very thorough dissection study on the medial knee joint in the 1970s(10). The medial knee was divided into the static and dynamic stabilizers:
- The static stabilizers of the medial knee include the superficial MCL (s-MCL), the deep MCL (d-MCL) or medial capsular ligament, and the posterior oblique ligament(5, 10).
- Dynamic stabilizers include the musculotendinous units of the semimembranosus, quadriceps, and the combined tendon of the semitendinosus, gracilis, and sartorius (pes anserinus)(10). The semimembranosus plays a significant role in the dynamic stability of the medial side of the knee. It achieves this by tightening the normally lax posterior oblique ligament, while posteriorly displacing the posterior horn of the medial meniscus to prevent impingement during knee flexion(11). Furthermore, the quadriceps and pes anserinus complex may potentially increase the effective stiffness of the MCL complex of the knee by 164 percent and 108 percent respectively(12).
The anatomy is described as having three layers: superficial (I), intermediate (II), and deep (III)(13, 14):
- The superficial layer (I) consists of the deep crural fascia, which invests the sartorius and quadriceps and continues into the deep fascia of the lower extremity to cover the gastrocnemius and popliteal fossa.
- The intermediate layer (II) comprises the s-MCL and medial patellofemoral ligament (MPFL).
- The deep layer (III) includes the joint capsule and d-MCL. A bursa separates the d-MCL and s-MCL and is biomechanically important by allowing anteroposterior excursion of the s-MCL during flexion and extension(15).
Superficial medial collateral ligament
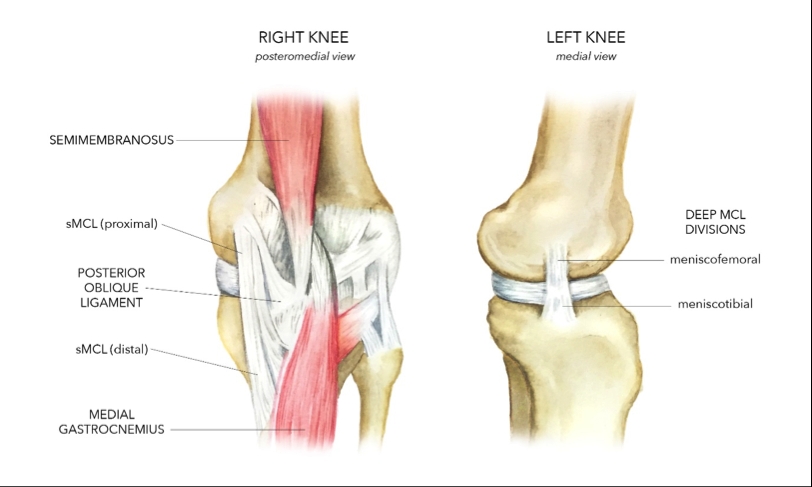
LaPrade et al 2007 have made the most detailed examination to date on the s-MCL(18). They claim the s-MCL is the largest structure of the medial aspect of the knee (see Figure 1). It has one femoral attachment and two tibial attachments(18). The femoral attachment is oval in shape and, on the average, 3.2mm proximal and 4.8mm posterior to the medial epicondyle.
As the s-MCL courses distally, it has two tibial attachments. The proximal tibial attachment is primarily a soft tissue attachment onto and over the termination of the anterior arm of the semimembranosus tendon, and is located an average of 12.2mm distal to the tibial joint line(18). The distal tibial attachment of the s-MCL is broad and is directly attached to bone at an average of 61.2mm distal to the tibial joint line; it is located just anterior to the posteromedial crest of the tibia(18). The two distinct tibial attachments have been reported to result in two distinct functioning divisions of the s-MCL(19).
A more recent study by Liu et al found that the s-MCL was triangular in shape and the proximal and distal parts were composed of parallel fibers. In contrast, the middle part of the s-MCL was composed of parallel and oblique fibers, and the middle portion was 1.7 times wider than the proximal/distal components(20). It is would be interesting to note whether the ‘oblique’ fibers in this study refer to the posterior oblique ligament, which is discussed further below, and numerous authors have made this same point(13, 14, 21, 22).
Deep medial collateral ligament
Deep to the s-MCL is the d-MCL, which is comprised of the thickened medial aspect of the joint capsule. It is divided into meniscofemoral (MFL) and meniscotibial (MTL) components (Figure 1) and is firmly attached to the medial meniscus at the joint line(20).
The larger, but thinner MFL has a slightly curved convex attachment 12.6 mm distal and deep to the femoral attachment of the s-MCL. The MFL is about three times longer than the MTL(20). The MTL attaches just distal to the edge of the articular cartilage of the medial tibial plateau, 3.2 mm distal to the medial joint line, and 9.0 mm proximal to the proximal tibial attachment of the s-MCL(18), and is 1.7 times wider than the MFL(20). It has also been reported that that the MFL attaches deep to the s-MCL, and the MTL attaches just distal to the tibial articular surface(25, 27). The d-MCL might play an important role to anchor the peripheral parts of the medial meniscus in the medial side of the knee(20).
Posterior oblique ligament: not a variation of s-MCL
The posterior oblique ligament assists the semimembranosus to dynamically stabilize the medial knee(21). Previous anatomical studies had described the s-MCL as having oblique posterior portions(23-25). It is now believed that these studies were, in fact, identifying the posterior oblique ligament and not variations of the s-MCL(18). More recent authors have noted that the s-MCL and the posterior oblique ligament are separate structures, although its femoral attachment has been varyingly described(21, 26).
The posterior oblique ligament is a fibrous extension off the distal aspect of the semimembranosus, which blends with and reinforces the posteromedial aspect of the joint capsule (See Figure 1). It consists of three fascial attachments at the knee joint(18, 21):
- Central - A prominent tibial arm on the edge of the posterior surface of the tibia.
- Capsular - A capsular arm, which is continuous with the posterior capsule and the proximal part of the oblique popliteal ligament.
- Superficial - An inferior arm, which blends with the sheath covering the semimembranosus, and which continues on to the tibia distal and to the semimembranosus insertion.
These three attachments course off the distal aspect of the semimembranosus tendon, but also off the medial meniscus, posteromedial tibia, and medial head of the gastrocnemius.
Relevant biomechanics
The s-MCL is the primary restraint to valgus laxity of the knee and at 25 degrees flexion it provides 78% of the valgus restraining force(1, 2, 28-30). At this angle of flexion, the posterior oblique ligament becomes lax and does not provide valgus support. In full extension, the ACL, posteromedial corner and semimembranosus contribute to valgus restraint and the s-MCL only provides 57% of the restraining force(1, 2). In general, an isolated s-MCL tear leads to valgus laxity in flexion, while additional injury to the secondary valgus restraints (posterior oblique ligament or ACL) leads to increased laxity in extension.
It has always been assumed that the two distinct tibial portions of the s-MCL had similar functions. However, less than a decade ago it was determined via biomechanical studies that there are differences between the two divisions of the distal s-MCL in terms of their responses to applied loads(19). The two divisions of the ligament actually function as conjoined but distinct structures. Therefore, any operative repair of the s-MCL should restore the distinct functions of both divisions by reattaching the two tibial attachments, in an attempt to reproduce the overall function of the s-MCL.
The posterior oblique ligament functions as a stabilizer of both internal rotation and valgus movement at between 0 and 30 degrees of knee flexion(1-4, 19, 31-35). With the tibia internally rotated at 0 degrees flexion, the loads on the posterior oblique ligament are significantly higher than those on either division of the s-MCL, which is tauter in external rotation(19). Furthermore, the load response between the posterior oblique ligament and s-MCL is reciprocal as the knee approaches 90 degrees flexion.
Also of interest is the fact that if the d-MCL and s-MCL are surgically cut, significant increases in force are experienced by the posterior oblique ligament under valgus loads at 0, 20 and 30 degrees of knee flexion(36). Therefore, the posterior oblique ligament in intact knees experiences tensile load with valgus forces, especially close to knee extension(19, 36), and it also has a secondary role in providing valgus stability of the knee(13, 14, 31, 36).
The function of the d-MCL (the MTL and MFL) is poorly understood in comparison to the s-MCL. Its specific role is to act as a secondary stabilizer of the knee to valgus load(35, 36). Valgus stabilization is provided by the MFL portion at all tested flexion angles. The MTL portion stabilizes primarily at 60 degrees of knee flexion. The d-MCL provides restraint against external rotation torque in knees flexed between 30 and 90 degrees(36).
In studies, it has been found that the maximum load to failure for the three structures were as follows(36):
- s-MCL - 534 Newtons
- d-MCL - 194 Newtons
- Posterior oblique ligament - 425 Newtons
Controversy also exists as to where the weakest part of the complex is and how this correlates with an actual injury in athletes. To summarise, however:
- The location of maximum strain of the entire medial collateral complex from cadaver studies was found to be near the femoral insertion when the knee was in full extension(36).
- Other clinical and laboratory studies suggest that the femoral insertion is the most common location for MCL injury(37-39)
- However, intraoperative findings have found that the tibial attachment is the most common injury site for the s-MCL, and the femoral attachment as the most common injury site for the d-MCL and the posterior oblique ligament(11,40).
- Finally, Hughston et al demonstrated that the tibial insertion was the most common site of injury for all the components of the MCL complex(3).
Injury classification
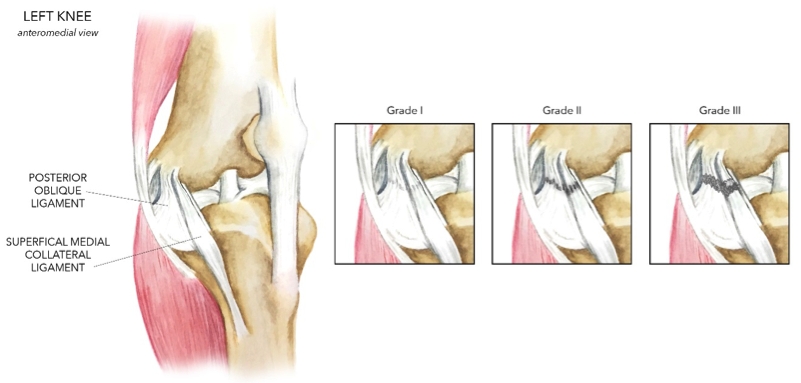
The time-honored classification of grading ligament injuries is derived from the American Medical Association Standard Nomenclature of Athletic Injuries (see Figure 2)(41). Within this naming system:
- Isolated grade-I first-degree tear presents with localized tenderness and no laxity.
- Isolated grade-II, second-degree tear presents with localized tenderness and partially torn medial collateral and posterior oblique fibres. The fibres are still opposed, and there may or may not be pathologic laxity.
- Isolated grade-III, third-degree tears present with complete disruption and laxity with an applied valgus stress.
Isolated medial knee injuries have also been classified in accordance with the amount of laxity observed at 30 degrees of knee flexion with a valgus applied moment compared to the uninjured limb(5, 42, 43):
- Grade 1 (3-5mm)
- Grade 2 (6-10mm
- Grade 3 (more than 10 mm)
Fetto and Marshall have a different classification system(44):
- Grade I injuries as those without valgus laxity in both 0 and 30 degrees of flexion.
- Grade II injuries as those with valgus laxity in 30 degrees of flexion but stable in 0 degrees of flexion.
- Grade III as those with valgus laxity in both 0 and 30 degrees of flexion.
It is important to perform valgus stress testing in 0 degrees of flexion, which is different from in full extension. In full extension (almost hyperextension), there is recruitment of ACL function that can mask the laxity of the complete medial-sided injury. There is a high incidence of associated ligamentous injuries with ACL injuries in grade III cases using this classification system.
Clinical assessment
History
The classic mechanism of injury reported is a sudden contact or non-contact valgus force to the knee with pain and swelling along the medial aspect of the knee. They may feel a tearing sensation with acute pain or in severe cases of rupture may hear a pop. Those with low-grade medial knee injuries involving either the s-MCL, posterior oblique ligament or d-MCL may attempt to continue competing. However, they often described a side-to-side feeling of instability, especially when performing cutting and pivoting maneuvers.
Clinical evaluation
The key features that may be found clinically are(18):
- Swelling over the medial side of the knee.
- Tenderness on palpation at the tibial or femoral insertions of the s-MCL.
- Tenderness on palpation along the medial joint line with the d-MCL.
- Valgus laxity and end point feel at 0 degrees full extension and 30 degrees knee flexion. If there is increased laxity at 30 degrees but not at 0 degrees, then the posterior oblique ligament is most likely still intact. However, the ACL may still mask an instability at full extension.
- Laxity at 0 degrees flexion (not quite full hyperextension) would indicate that this would be a Fetto and Marshall grade-3 injury indicating damage to the posterior oblique ligament and posteromedial capsule(44).
- A complete injury to the medial structures will cause increased external rotation at both 30 degrees and 90 degrees of knee flexion, resulting in a positive dial test(1, 2, 19). Therefore, careful correlation with the results of valgus stress testing and assessment of the location of tibial subluxation during the dial test are necessary to exclude the possibility of a posterolateral, rather than a medial knee injury.
Stress testing
With the patient lying supine, the assessor grasps the ankle with one hand and places the other hand on the outside of the thigh above the knee. A gentle outward force is applied to the ankle. This can be done at full extension, 0 degrees flexion and 30 degrees flexion:
- At full extension, this assesses the s-MCL and d-MCL, the posteromedial capsule, the posterior oblique ligament, and the ACL and PCL.
- At 0degrees flexion, the posteromedial capsule and ACL and PCL are taken off slight stretch.
- At 30 degrees flexion, the s-MCL is the primary restraint to valgus stress.
Imaging
Plain film X-rays are usually unnecessary unless the clinician wants to assess the degree of gapping of the medial joint line under imaging. In one study, a load applied by a clinician to a knee with a simulated isolated grade III s-MCL injury increased medial joint gapping, compared with that in the intact knee, by 1.7 and 3.2mm at 0 and 20 degrees of flexion, respectively(45). A complete medial knee injury, with sectioning of the s-MCL and d-MCL and the posterior oblique ligament, increased gapping by 6.5 and 9.8mm at 0 and 20 degrees of flexion respectively, under the clinician-applied load (45).
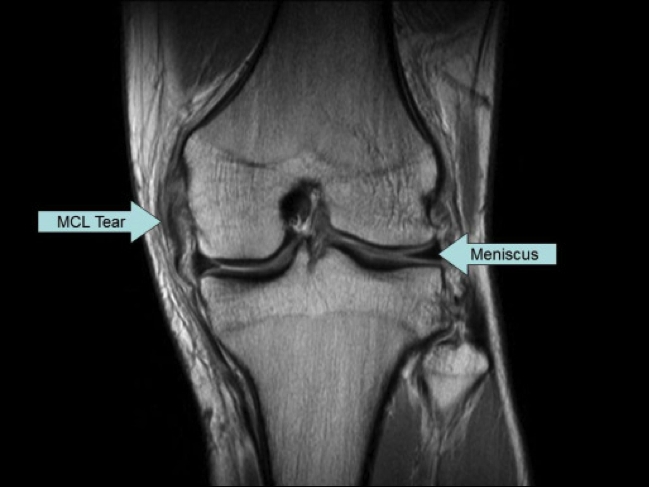
Magnetic resonance imaging (MRI) is more commonly used to assess the involved structures in patients with injuries to the medial side of the knee (see Figure 3). T2-weighted MRI is the gold standard for diagnosing both partial and full tears of the s-MCL. MRI has an accuracy of 87% for the assessment of MCL injuries(46).
Aspects of healing
Studies of the variables involved in the healing of the s-MCL in animals have shown that the healing is location dependent and immobilization dependant:
- Injuries to the attachment sites take longer to heal than mid-substance injury(47).
- In a rabbit model, a reduction of collagen mass and increased collagen degradation were observed after twelve weeks of immobilization(48).
- Immobilization leads to disorganization of collagen fibrils, a decrease in the structural properties of the bone-ligament-bone complex, and resorption of bone at ligament insertion sites(49).
- These negative effects of immobilization were believed to be caused by collagen matrix reorganization and tissue catabolism within the MCL after injury(50,51).
- In another study performed on dogs that had undergone surgical transection of the s-MCL(49)it was found that in the three groups: early motion, immobilization for three weeks, and immobilization for six weeks, the early motion protocols led to enhanced healing and improved biomechanical properties of the s-MCL.
Conclusion
MCL injuries are a common occurrence in sports that require sharp cutting and changing directions, and in contact sports. The anatomy of the medial side of the knee is reasonably complex and composed of the static stabilizers such as the s-MCL, d-MCL, posterior oblique ligament, and the posteromedial capsule. It is supported by the active stabilizers, the muscles. Injuries to the inside of the knee predominately involve the s-MCL. This is ideally tested with a 30-degree valgus stress test and can be confirmed on MRI. Management of grade 1-2 and most grade 3 injuries involve brace immobilization and conservative management. Surgery is reserved for severe and complex ligament disruptions or in the case of chronic valgus instability. Part two of this article will discuss in detail the conservative progression following an injury to the s-MCL.
References
- J Bone Joint Surg Am. 1981;63:1257-69
- J Bone Joint Surg Am. 1988;70:88-97
- J Bone Joint Surg Am 1976;58(2): 159-72
- J Bone Joint Surg Am. 1994;76:1328-44
- Iowa Orthop J. 2006;26:77-90
- Rheumatology (Oxford). 2006;45:595-9
- Am J Sports Med. 1995;23: 597-600
- Am J Sports Med. 1988;16:392-6
- Am J Sports Med. 2000;28(5 Suppl):S51-7
- Fortschr Med 1978;96(4):141-6,166
- Am J Sports Med 2004;32(2):337-45
- J Bone Joint Surg Am 1979;61(3):398-402
- J Bone Joint Surg Am Vol 1979;61(1):56–62
- J Bone Joint Surg Am. 1974;56:665-74
- Orthop Rev. 1989;18:947-52
- J Bone Joint Surg Am. 1983;65:323-9
- Clin Orthop Relat Res. 1990;256:174-7
- J Bone Joint Surg Am. 2007;89: 2000-10
- Am J Sports Med. 2009;37:140-8
- Journal of Orthopaedic Surgery and Research 2010, 5:6
- J Bone Joint Surg Am 1973;55(5):923-40
- J Bone Joint Surg Br.1948; 30:683-8
- J Bone Joint Surg Am. 1943; 25:121-31
- J Bone Joint Surg Am. 1941;23:44-66
- J Bone Joint Surg Am. 1968;50: 211-25
- AmJ Sports Med. 1985;13:390-7
- 2000;20 Spec No:S83-9
- J Bone Joint Surg Am. 1944;26:503-21
- Acta Orthop Scand. 1965;36:179-91
- Clin Orthop Relat Res. 1995;321:3-9
- Am J Sports Med. 1994;22:402-9
- Am J Sports Med. 1977;5:144-53
- Acta Orthop Scand. 1984;55:30-4
- Arch Orthop Trauma Surg. 1984;103:165-9
- Am J Sports Med. 2009;37:1771-6
- Am J Sports Med. 2006;34:1815-23
- J Orthop Res 2003;21(6): 1098-106
- Med Eng Phys 1999;21(5):279-91
- Am J Sports Med 2003;31(2):261-7
- Clin Orthop 1991;(271):3-8
- American Medical Association; 1966. p 99-100
- Sports Med Arthrosc. 2006; 14:12-9
- Prim Care. 2004;31:957-75, ix
- Clin Orthop 1978;132:206-18
- Am J Sports Med. 2010;38:330-8
- Skeletal Radiol. 1994;23:521-4
- Acta Orthop Scand. 1995;66:455-62
- Clin Orthop Relat Res. 1983;172: 265-70
- J Orthop Res. 1983;1:22-9
- J Orthop Res. 1992;10:895-900
- Clin Orthop Relat Res. 1992;277:277-88
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.