Medial tibial stress syndrome: a novel approach?

Medial tibial stress syndrome (MTSS - commonly known as shin splints) is a frequent injury of the lower extremity and one of the most common causes of exertional leg pain in athletes and other active individuals. Studies suggest that the incidence of MTSS among physically active soldiers is 7.9%, while among athletes it varies between 4% and 35%(1,2). Although often not serious, it can be quite disabling, and progress to more serious complications if not treated properly. To further complicate matters, the rate of relapse in MTSS is high.
Causes of MTSS
The precipitating factors leading to MTSS are thought to be multi-factorial, involving training errors and various biomechanical abnormalities (these factors are discussed at length by Alicia Filley here). Many believe the main cause of MTSS involves underlying periostitis of the tibia due to tibial strain when under load. However, the associated lower leg anatomy makes this unlikely (see figure 1). Also, other evidence indicates it is likely that a whole spectrum of tibial stress injuries are involved in MTSS, including tendinopathy, periostitis, periosteal remodeling, and stress reaction of the tibia(3-6).Dysfunction of the tibialis posterior, tibialis anterior, and soleus muscles are also commonly implicated(5,6). These various tibial stress injuries appear to be caused by alterations in tibial loading, as chronic, repetitive loads cause abnormal strain, bending of and micro-damage to the tibia. In other words, while MTSS is sometimes composed of different etiologies, MTSS and tibial stress fractures may be considered on a continuum of bone–stress reactions. One thing that is unarguable is that over the last few decades, comparatively few advances have been made in the treatment of MTSS. Current treatment options are mostly based on expert opinion and clinical experience rather than peer-reviewed comparative studies(7).
Figure 1: Anatomy of the lower leg and MTSS
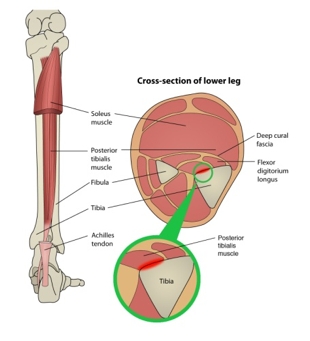
The anatomy of the lower leg makes it unlikely that the posterior leg muscles cause a traction-induced injury to the periosteum of the tibia. While the pain of a shin splint is felt along the anterior leg, the muscles that arise from this area are the posterior calf muscles. The tibialis posterior, flexor digitorum longus, and the soleus all arise from the posterior-medial aspect of the proximalhalf of the tibia. Therefore, the traction force from these muscles on the tibia is unlikely to be the cause of the pain typically felt on the distal portion of the leg. Cadaver studies, however, seem to support the theory that repeated or prolonged tension placed on the deep crural fascia by posterior compartment muscle contraction would provide sufficient strain to trigger periostitis and produce pain.
Risk factors and predicting MTSS
Given that an ounce of prevention is worth a pound of cure, and the fact that following an episode of MTSS, the rate of relapse is high, being able to predict the onset of MTSS and take proactive and pre-emptive action is a valuable asset for a clinician. The literature reports that a number of factors can elevate the risk of MTSS. Studies have variously reported the following factors as risk factors:- Hyperpronation of the foot, female gender, and a history of previous(8).
- Flattening of the longitudinal arch of the foot, increased plantar flexion in the upper ankle joint, and a restriction of internal hip rotation (see Alicia Filley’s article in issue 156)(9,10).
- Smoking and poor cardiovascular stamina(1).
- An increased body mass index, which has an adverse effect on the duration of MTSS(11).
The above risk factors are undoubtedly useful to be aware of but are there any tests that can accurate predict the likely onset of MTSS? Newman and colleagues attempted to identify the effectiveness of two clinical screening tests to identify individuals in a pre-symptomatic stage of MTSS(12). Three hundred and eight-four cadets at the Australian Defence Force Academy (96 female, 288 male) underwent a pre-participation musculoskeletal exam, which included two simple clinical tests for MTSS. These tests consisted of the shin palpation test (SPT) and shin oedema test (SOT), which together took only around 30 seconds to complete.
The SPT was performed by palpating the distal two thirds of the posteromedial lower leg and surrounding musculature. Pain with palpation was considered a positive test. Performing the SOT consisted of a sustained (5-second) hold of the distal two thirds of the medial surface of the tibia bilaterally. The test was considered positive if pitting edema was present. All tests were conducted by physiotherapists with a minimum of 2 years of experience.
For 16 months after the assessments, the authors monitored the healthcare centres available to the cadets for any diagnoses of MTSS and noted any subsequent diagnostic imaging or treatment. Overall, 76 (20%) reported pain during the SPT and 12 (3%) had pitting edema. Eleven (3%) had both reported pain and pitting edema on one or both legs. Of those who tested positive during screening, 26 of 76 with positive SPT (34%), 11 of 12 with positive SOT (92%) and 11 of 11 with positive SPT and SOT (100%) were later diagnosed with MTSS by a doctor or physiotherapist. In contrast, among those with tested negative during screening, 276 of 307 with negative SPT (90%), 325 of 372 with negative SOT (87%), and 326 or 373 with positive SPT and SOT (87%) were not diagnosed with MTSS. These results suggest that both the SPT and SOT tests are strongly predictive of future development of MTSS. For subjects who score positive on both tests, the result is extremely predictive.
While other physical examinations are still important, this study makes a strong case for inclusion of these quick tests into clinician’s preseason musculoskeletal screenings. They take minimal time to perform, and the finding(s), combined with the athlete’s sport, and gender could aid a clinician in determining which athletes are at an increased risk for developing MTSS. With this knowledge, clinicians can be aware of early signs of the condition, and treatment offered to keep the condition from worsening.
Assessment and diagnosis
MTSS typically presents with vague, diffuse pain of the lower extremity, along the middle-distal tibia, and which is associated with exertion(13). In the early stages, pain is worse on commencing exercise and gradually subsides during training or shortly after the cessation of exercise. However, as the injury progresses, less and less activity is required to produce pain, and eventually it can occur even at rest.When faced with an athlete presenting with these symptoms, clinicians should obtain a comprehensive exercise history including:
- The athlete’s weekly exercise routine and total training volumes (eg total running mileage)
- Exercise intensity/pace/loading
- Footwear used
- Training terrain
Particular attention needs to be given to any of these factors that have changed radically over the past three months. This is because research suggests that MTSS is most likely to occur in athletes who have attempted to do ‘too much, too fast’(14,15).
Common errors include a recent onset of rapidly increased activity, intensity, or duration(16). Running on hard or uneven surfaces is also a common risk factor and all risks are increased once weekly mileage exceeds around 20 miles per week(17). Clinicians should also be aware of the MTSS gender factor; studies indicate that the risk for progression to stress fractures is 1.5 to 3.5 times greater in females(17,18). This is especially relevant in females at risk of diminished bone density and osteoporosis – commonly observed is the ‘female athlete triad syndrome’ (osteoporosis, amenorrhea, and disordered eating – see figure 2)(19).
Figure 2: The ‘female triad’ spectrum
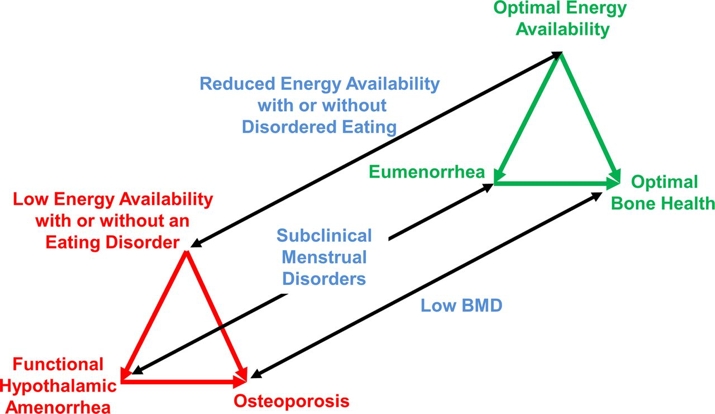
Rather than an ‘either/or’ condition, the female triad can be considered as spectrum from optimum eating, hormonal function and bone health (green) to poor eating/eating disorder, amenorrhea and osteoporosis at the other end (red). The further towards the red end of the spectrum, the greater the risk of MTSS progressing to a stress fracture.
Physical examination and differential diagnosis
Clinicians should complete a thorough musculoskeletal examination of the patient, focussing on the lower extremity. Typically, the medial ridge of the tibia (origin of the tibialis posterior and soleus muscles) will be tender to palpation, especially at the distal and middle tibial regions. The anterior tibia, however, is usually non-tender. Neurovascular symptoms are usually absent(13).However, because MTSS is often associated with biomechanical abnormalities of the lower extremity, clinicians should also evaluate their clients for possible knee abnormalities (especially genu varus or valgus), tibial torsion, femoral anteversion, foot arch abnormalities, or a leg-length discrepancy. Ankle movements and subtalar motion should also be evaluated. In addition, examining the athlete’s training shoes may reveal generally worn-out shoes or patterns consistent with a leg-length discrepancy or other biomechanical abnormalities. Abnormal gait patterns should be evaluated with the patient walking and running, either in the office hallway or on a treadmill.
A thorough history and physical examination are usually sufficient to make a diagnosis of MTSS. However, some patients may require further imaging or work-up to rule out stress fractures such of that of the tibia manifested by focal tenderness of the anterior tibia(17,20). Symptoms such as sensory or motor loss in association with exertional lower leg pain could indicate acute or chronic exertional compartment syndrome, which is one of the conditions most likely to be confused with MTSS. Peripheral vascular disease is another common cause of exertional leg pain in older and diabetic athletes. In this circumstances, further imaging, compartment pressure measurements, and vascular and nerve conduction studies may occasionally be required to reach the correct diagnosis(21).
Having said that, recent research suggests that MTSS can be diagnosed reliably using history and physical examination alone(22). In a study at multiple sports medicine sites in The Netherlands, athletes with non-traumatic lower leg pain were assessed for MTSS by two clinicians, who were each blinded to each others' diagnoses. Forty-nine athletes participated of whom 46 completed both assessments. The prevalence of MTSS was among the athletes was 74%. Importantly, the percentage of agreement was very high at 96% and the ‘inter-rater reliability’ was almost perfect. Of note was that out of the 34 athletes diagnosed with MTSS, eleven were also found to have a concurrent lower leg injury, bearing out the findings discussed above.
Treatment options for MTSS
There are a number of conservative treatment options for MTSS. As we will see shortly however, some have been shown to be more effective than others. An excellent and detailed description of these approaches is described by Galbraith and Laverlee(7). In their paper, a brief summary of the conventional treatment pathway is also described (see table 1).| Phase | Focus | Key Objectives |
|---|---|---|
| Stage 1 | Protection andhealing | Adequate healingRestore homeostasis |
| Stage 2 | Motion andstrength | Gross muscle mass and strength developmentROM restorationPropulsive and absorptive force development |
| Stage 3 | Return to function | Functional patterns of movementSkill development relevant to the chosen sportMultidirectional speed and agility |
| Stage 4 | Return toperformance | Technical skill competenceCompetitive confidenceResilienceTraining load tolerance |
Acute phase
In the acute phase of MTSS, rest is recommended, with a complete or partial cessation of activity for 2-6 weeks depending on symptom severity(23). NSAIDs and paracetamol are often used for pain relief while ice application to the affected area directly after exercise for approximately 15–20 min is also commonly used in the acute period.
Given the undesirability of weeks of complete inactivity in athletes, other treatment modalities to speed healing have also been advocated in the acute phase. These include ultrasound, whirlpool baths, phonophoresis, augmented soft tissue mobilisation, electrical stimulation, and unweighted ambulation. However, while these are popular approaches among some clinicians, there’s little evidence in the literature that they offer tangible benefits over and above rest and ice(3,6,13-15).
Post-acute phase
- Training modification - Once the initial symptoms have subsided, the goal is to enable the athlete to gradually return to training and competition without a relapse. Without doubt, the most important requirement is to modify the training regimen and address any biomechanical abnormalities. Research indicates that runners can continue to improve without cessation of activity so long as their weekly running distance, frequency, and intensity are reduced by at least 50%. In addition, they should eliminate running on hills and uneven or very firm surfaces, which increase loading on the tibia(3,13-15). A better option is train on a synthetic track or treadmill, both of which provide a uniform surface with more shock absorption. During the post-acute phase, athletes can benefit from cross training utilising other low-impact exercises such as pool running, swimming, elliptical trainers or stationary cycling. This is also the time for clinicians to work with athletes on proper technique and gait retraining, helping them to return to activity in a step-wise fashion. Over a period of weeks, training intensity and duration can be gradually increased and jumping exercises and hill running added as long as the athlete remains pain-free(3). However, athletes should scale back any exercises that exacerbate their symptoms or cause pain.
- Footwear - Many studies report that appropriate footwear can reduce the incidence of MTSS(3,15, 23,24); athletes should therefore switch to shoes with sufficient shock-absorbing soles and insoles, in order to reduce forces through the lower limbs. Runners should also change running shoes every 250–500 miles, a distance at which most shoes lose up to 40% of their shock-absorbing capabilities and overall support(14,25). In addition, athletes with foot-related biomechanical problems may benefit from orthotics (13,14,16). Over-the-counter insoles may be sufficient to help with excessive foot pronation and low foot arch but problems caused by forefoot or rearfoot abnormalities may benefit from custom orthotics(26).
- Other possible treatments –A number of other treatment options that may be relevant in the post-acute phase of MTSS have been described in the literature. Extracorporeal shock wave therapy (ESWT) has been used to treat various tendinopathies of the lower extremity with varying degrees of success. However, there are no randomised control trials (RCTs) examining this approach in MTSS. Various injection methods, including cortisone, have successfully been used for decades to treat others injuries of the lower extremity(27-29). There are also newer methods, such as dry-needling, autologous blood injection, platelet-rich plasma, and prolotherapy, which seek to stimulate a local healing response in injured tissues. Once again however, no RCTs have been performed with these different injection techniques for MTSS. The same is true for acupuncture. This is not to say that clinicians should rule out experimentation with these technique – only that the evidence they are of value is lacking.
Fascial distortion and MTSS
Manual therapy techniques such as osteopathic manipulation, stretching and massage have been commonly used to treat lower-extremity injuries with the benefit of improved pain and function(30-32). However, there is a paucity of properly controlled scientific trials into the role of manual therapy in treating specifically MTSS.Some researchers have postulated that the fascia plays an important role in pathophysiology of MTSS. Bouché and Johnson have hypothesised that with contraction of the deep leg flexors, tension would be imparted to the tibial fascial attachment at the medial tibial crest and that circumferential straps would dampen tension directed to the medial tibial crest(33). Meanwhile, Stickley et al. Have described the tibial attachments of the deep crural fascia and concluded that there is deep crural fascia involvement in the aetiology of MTSS(34).
The treatment of fascial distortions is also based on targeted manual therapy techniques, which has led some researchers to suggest that this approach could be effective in MTSS. Therapeutic success using this approach has already been described for shoulder pain, in particular for the management of frozen shoulder, where improvements in function and pain sensation were quickly achieved and superior to conventional physiotherapy(35,36).
New research
A recent study has suggested that a treatment therapy based on the fascial distortion model could be a useful adjunct for clinicians seeking to hasten the recovery of athletes suffering from MTSS. The 32 participants in the study were soldiers who had been diagnosed with MTSS, because they showed the typical symptoms of pain following exercise as well as tenderness of the anterior or posterior medial and lateral anterior surfaces of the tibia. In some cases, the symptoms were acute, while in some patients the symptoms had been present for several years.Before and after the intervention period, the patients performed running and jumping tests and a visual analogue scale (VAS) was used for the quantification of pain. Scores were also given to rate the maximum painless exercise tolerance of the patients. Following initial testing, treatment of the crural fascia was performed using (see box 1). The therapy was continued until full exercise tolerance or painlessness was reached. The main finding was that a significant reduction of the VAS pain score (from 5.2 to 1.1) was achieved in a relatively short time span (the duration of treatment was just 6.3 days on average). Also, the impairment of exercise tolerance following therapy was reduced from 7 to 2 points (see figure 3).
| Grading system for ACJ injury | |
|---|---|
| Type | Features |
| I | The AC ligaments are sprained, but the joint is intact. No palpabledisplacement of the joint itself. Minimal to moderate tenderness andswelling over the AC joint. Patients have only minimal pain with movementof the arm. Radiographically there may be mild soft tissue swelling, butthere is no widening, separation, or deformity at the AC joint. |
| II | AC ligaments are torn, but the CC ligaments are intact. Type II injuriesare characterised by moderate to severe pain at the AC joint. The distalend of the clavicle may be palpated to be slightly superior to theacromion and shoulder motion produces more pain at the AC joint. Thedistal clavicle is also found to be unstable in the horizontal plane ifgrasped and moved anterior to posterior. A bilateral Zanca view maydemonstrate that the distal clavicle is slightly elevated, but the CCinterspace is the same in both the injured and uninjured shoulders. |
| III | Patients with type III injuries present with the upper extremity in asupported, adducted and elevated position to help relieve pain. In typeIII injuries both the AC and CC ligaments are torn, but the deltoid andtrapezial fascia are intact. The distal clavicle may be prominent enoughto tent the skin and is unstable in both the vertical and horizontalplanes. These patients have a severe amount of pain with tenderness topalpation at the AC joint. Any movement of the arm, especiallyabduction, creates pain and discomfort, especially for the first 1“3weeks. Both plain and bilateral Zanca x-rays reveal that the distalclavicle is 100% displaced superiorly in relation to the acromion. Inactuality, the position of the clavicle is not altered by the injury. Theweight of the upper extremity causes the acromion to displace inferiorlyin relation to the horizontal plane of the lateral clavicle. In obviouscases of dislocation the clavicle is displaced superiorly from theacromion and the CC interspace will be greater in the injured shoulder. |
| IV | Type IV injuries are characterised by complete dislocation withposterior displacement of the distal clavicle into or through the fasciaof the trapezius. Physical examination of these patients reveals agreater amount of pain as compared with patients with type III injuries,and the pain is located more posteriorly. Examination of the seatedpatient from above will reveal that the distal clavicle is displacedposteriorly when compared with the uninjured shoulder. It is possiblefor the distal clavicle to become ˜button-holed in the trapezius andtent the skin posteriorly. With a type IV injury it is also important toexamine the SC joint for a concomitant anterior dislocation. Theposteriorly displaced clavicle is best appreciated on an axillary view ofthe shoulder. |
| V | Type V injuries represent a greater degree of soft tissue damage withthe deltotrapezial fascia being stripped off the acromion and theclavicle. These injuries present as a more severe type III injury withmore pain and a greater amount of displacement at the AC joint. Thedistal end of the clavicle appears to be grossly displaced superiorlytowards the neck. The scapula is translated anteriorly and inferiorly asit migrates around the thorax. On bilateral Zanca view there is 100“300% increase in the CC interspace. Patients with a type V injury mayhave pain in the neck or trapezius due to the disruption of thedeltotrapezial fascia. |
| VI | Type VI injuries are inferior AC joint dislocations into a subacromial orsubcoracoid position. Type VI injuries are usually seen in high energypolytrauma patients. The mechanism of injury is extremehyperabduction and external rotation of the arm combined withretraction of the scapula. Associated injuries include clavicle and upperrib fractures and upper root brachial plexus injuries. It is notuncommon for these patients to have transient paraesthesias thatsubside after reduction. |
Figure 3: Effects of fascial distortion model therapy on exercise impairment
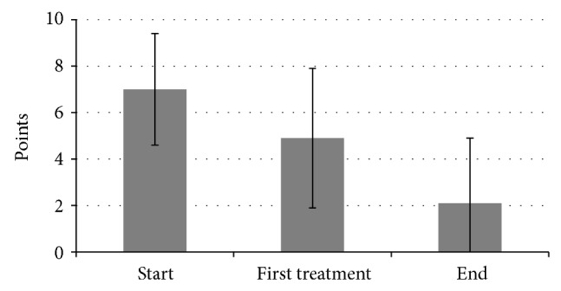
Pain scores fell from an average of 7 to 2.
The results of this clinical study suggest that the treatment method according to the fascial distortion model could be an effective option to relieve patients of pain and restore their exercise tolerance. The duration of this treatment was significantly shorter than the therapy periods indicated in the literature for shock wave therapy and physiotherapy(38,39). The drawback for the clinician however is that this method is time consuming. In severe cases, a complete initial treatment can take up to one hour for each lower leg (although the time expenditure will decrease in the subsequent treatment sessions). Moreover, the method is very painful for the patient, and the patient must be informed of this prior to treatment in order to improve the therapy tolerance.
Furthermore, this study only demonstrated that exercise tolerance in MTSS can be restored within a short time by targeted manual intervention; there was no long-term follow up. Moreover, there was no direct comparison with alternative treatment options – this would be desirable to prove that therapy based on fascial distortion is superior to other therapeutic approaches. Despite these caveats however, therapy according to the fascial distortion model has proved to be superior to other physiotherapy methods in the management of shoulder pain syndromes(35,36), which suggests that this approach could be another weapon in the clinician’s armoury when seeking a rapid resolution of MTSS in athletes.
References
- Gait & Posture. 2011;33(3):361–365
- Clinics in Sports Medicine. 2012;31(2):273–290
- Sports Med. 1998;26(4):265–279
- 1997;204:177–180
- Sports Med. 1986;3(6):436–446
- Am J Sports Med. 1995;23:427–481
- Curr Rev Musculoskelet Med. 2009 Sep; 2(3): 127–133
- MTSS Clin Sports Med. 2012 Apr;31(2):273-90
- Journal of Foot and Ankle Surgery. 2008;47(2):89–95
- Scandinavian Journal of Medicine and Science in Sports. 2012;22(1):34–39
- Journal of Orthopaedic and Sports Physical Therapy. 2007;37(2):40–47
- Br J Sports Med. 2012 Sep;46(12):861-4
- MedSci Sports Exerc. 2000;32(3 suppl):S27–S33
- Sports Med. 1996;21:49–72
- Clin Sports Med. 2004;23:55–81
- Phys Med Rehabil Clin N Am. 2006;17(3):537–552
- Phys Med Rehabil Clin N Am. 2007;18(3):401–416
- J Sports Med Phys Fitness. 1990;30(3):307–315
- Am J Sports Med. 2004;32(3):772–780
- Am J Sports Med. 1978;6(6):391–396
- Phys Sportsmed. 2001;29(6):35–50
- Br J Sports Med. 2017 Feb 8. pii: bjsports-2016-097037
- Phys Sportsmed. 2002;30(6):29–361
- Med Sci Sports Exerc. 2002;34(1):32–40
- Am J Sports Med. 1985;13:248–253
- Med Sci Sports Exerc. 1995;27:800–804
- Br J Sports Med. 2007;41(8):518–522
- Am J Sports Med. 2006;34(11):1738–1746
- Br J Sports Med. 2002;36(3):173–177
- J Am Osteopath Assoc. 2005;105(12):563–567
- J Am Osteopath Assoc. 2006;106(9):537–545
- J Am Chiropr Assoc. 2004;41(9):32–42
- Journal Am Podiatric Med Assoc. 2007;97(1):31–36
- Med Sci Sports Exercise. 2009;41(11):1991–1996
- Zeitschrift fur Orthopadie und Unfallchirurgie. 2012;150(4):420–427
- Stein C. Untersuchung der Wirksamkeit einer manuellen Behandlungstechnik nach dem Faszien-Distorsions-Modell bei schmerzhaft eingeschränkter Schulterbeweglichkeit - Eine explorativ-prospektive, randomisierte und kontrollierte klinische Studie. Medizinische Hochschule Hannover; 2008
- European Fascial Distortion Model Association . Das Fasziendistorsionsmodell (FDM) nach Stephan Typaldos D.O. Die Typaldos-Methode. 1st. Bramsche, Germany: Rasch Druckerei; 2012
- Clinics in Sports Medicine. 2012;31(2):273–290
- British Journal of Sports Medicine. 2012;46(4):253–257
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










