Muscle strain injury: time to consider the fascia?

Muscle strain injuries frequently occur in athletes. In ball-sports (soccer, rugby, basketball, football etc), they are among the most common of all injuries reported by athletes(1-3). The consensus is that they occur during excessive loading, particularly during eccentric muscle contractions, which reflects the muscle’s inability to withstand elongating forces(4). Therefore, eccentric muscle strengthening and conditioning should build resilience against muscle strain injury.
There may be a flaw in this simplistic thinking about injury prevention. It turns out that in many muscles, less than 20% of the fibers span the entire distance between the muscle origin and its insertion. The bulk of the fibers terminate in the muscle belly, connected only via their endomysium (see figure 1)(5). This anatomy suggests that the intramuscular connective tissue also plays an influential role in transmitting or absorbing muscular forces. In short, this implies that fascial tissue assists the muscle in handling loads and that excessive loads can damage the fascia as well as the muscle.
Figure 1: The relation of the endomysium in the overall muscle architecture
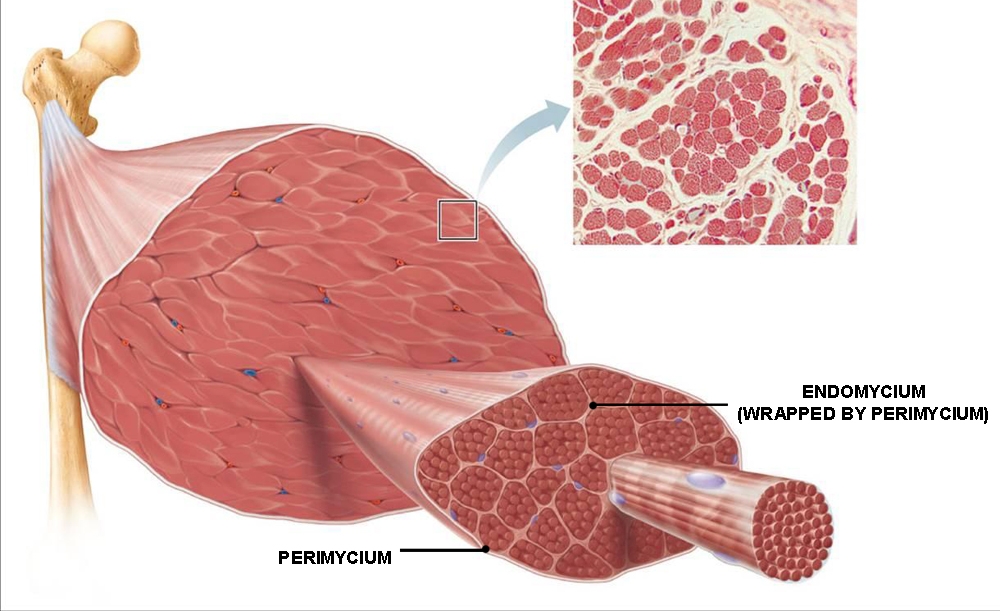
Evidence of fascial involvement in muscle strain injury
The participation of fascial tissue in the pathology of a muscle strain injury is quite a new concept. Until recently, the data on this subject has been limited and circumstantial. Rat muscle studies demonstrate force differences of up to 25% between the proximal and the distal tendon. This difference was eliminated with the removal of the extensor digitorum’s fascia which connects to the surrounding muscles(6). The implication is that the fascia played a role in the development of the muscle tension. In addition, fascia and tendons have similar mechanical properties relating to maximum stress tolerance(7). Therefore, if fascial tissue plays an integral role in distributing muscle forces (generated or absorbed), could it not also share in muscle strain injuries?A review published by German researchers examined the data collected from imaging studies that described the frequency, location, and extent of soft tissue lesions in athletes who suffered lower-limb muscle strain injuries(8). In total, 16 studies collectively evaluated a total of 1503 muscle injuries in athletes. These athletes included track and field athletes, Olympians, semi-professional and amateur athletes, professional soccer players, and American football players. All but one of the studies used MRI as an imaging modality. Two studies used MRI and ultrasonography while one study used ultrasonography only. The main findings were as follows:
- The most frequently examined muscles were the hamstrings followed by the soleus.
- Statistical analysis revealed myofascial lesions in 32.1%, myotendinous or tendinous lesions in 68.4%, and isolated muscular lesions in 12.7% of cases.
- Researchers observed myofascial tissue lesions most often in the soleus muscle (36.4%), followed by the hamstring muscles (27.9%).
- One in eight cases were isolated muscular injuries with the damage frequently located within or at the junction with the connective tissue.
Diagnosis
The diagnosis of the degree of fascial tissue involvement in a muscle strain is determined by MRI imaging. However, this is time-consuming, costly, and unlikely to be practical for all but the most elite athletes. Given that an isolated muscle tissue injury is present in just one in eight cases, clinicians should assume that some degree of fascial tissue damage is quite likely in such injuries. The presence of concurrent myofascial damage seems to be particularly the case for injuries to the soleus muscle. A soleus muscle injury should merit a focused investigation of the deep fascia by the clinician.Treatment implications
The presence of larger fascial lesions (over 20mm) on MRI suggests a more prolonged and gradual rehab protocol(9). Include dynamic stretches and eccentric exercises to promote connective tissue healing(8). Keep in mind that fascial tissue exhibits a higher pain sensitivity than muscle tissue(10). Athletes who suffer a soft-tissue injury with significant fascial tissue damage (confirmed by MRI) will experience significantly more pain and discomfort than those where the damage is restricted to muscle only. Rehabilitation may progress more gradually in these cases. Manage an athlete’s expectations of their return-to-play timeline accordingly.Finally, in the presence of fascial tissue damage, athletes may benefit from consuming vitamin C–enriched gelatin to promote collagen synthesis(11). Collagen forms an essential component of connective tissue. It is synthesized in the body from proline (present in gelatin) in the presence of vitamin C. Athletes who have a sub-optimum vitamin C status may experience reduced levels of collagen synthesis. Although it’s possible to purchase proline-rich peptides, gelatin (found in Jell-O, fruit chews, and gummy candies ) is an excellent source of proline, making it a cheaper option for athletes with a sweet tooth!
Fascial lesions and return to sport
Predicted return to sport times after a fascial injury may differ from other types of muscular injury. For example, a University of Virginia study compared the size of a diagnosed fascial lesion and the average downtime from the injury. The results showed that in athletes injured for two weeks or more, the average magnitude of the lesions was three times greater (27mm) than in those who returned to sport in under two weeks (8mm)(9).A Barcelona study observed that athletes with higher fascial injury scores reported a longer return-to-play time compared to those with injury at the myotendinous junction(12). However, the difference (35 days versus 27 days) was not significant. Researchers at the French National Institutes of Sports also compared return-to-play times between muscle and connective tissue (fascia and intramuscular connective tissue, including tendons) lesions. They concluded that athlete downtime was significantly longer for connective tissue injury (7.6 weeks) than for muscle-only injury (3.9 weeks)(13). It appears then that damage to the fascia takes longer to heal and thus results in a lengthier return-to-play time.
References
- Am J Sports Med. 2017;36(12):2328-2335
- Int J Sports Med. 2016;37(11):898-908
- Br J Sports Med. 2002;36(1):39-44
- Nuclear Medicine and Radiologic Imaging in Sports Injuries. Berlin, Heidelberg, Germany: Springer; 2015:939-948
- Acta Anat. 1997;159(2-3):99-107
- Acta Physiol Scand. 2001;173(3):297-311
- J Biomech. 1984;17(8): 579-596
- Orthop J Sports Med. 2019 Dec; 7(12): 2325967119888500
- Orthop J Sports Med. 2017;5(1):2325967116680344
- Eur J Appl Physiol. 2015 May; 115(5):959-68.
- Am J Clin Nutr. 2017 Jan; 105(1): 136–143
- Orthop J Sports Med. 2015;3(7):2325967115595802
- J Sci Med Sport. 2019;22(6):641–646
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









