Osteitis pubis: a likely cause of groin pain

Groin pain often plagues athletes who kick, cut, and twist as part of their sport. Studies suggest the incidence in male soccer players to be 18% of all injuries each year(1). One cause of groin pain - accounting for 3% to 5% of injuries- is osteitis pubis (OP)(1). With OP, athletes typically complain of pain near or on the pubic bone at the base of the groin when walking, stretching, or strengthening the adductor muscles or abdominal muscles.
The narrow inferior pubic ramus and symphysis is the site of attachment for two adductor muscles ( longus, and bravis) and the gracilis muscle (see figure 1). The repetitive pull of these muscles on this bit of bone inflicts microtrauma to the area. Inflammation and irritation in the bone, and often in the muscle tendons themselves, results. Adding to the problem, abdominal muscles also attach at the pubic bone. Therefore, both muscle groups may be pulling on the area at the same time and in opposite directions, especially when kicking. Another contributing factor may be decreased hip internal rotation(1). Without adequate hip range of motion, turning and cutting maneuvers generate a greater pull on the pelvis.
Figure 1: Pelvic Anatomy
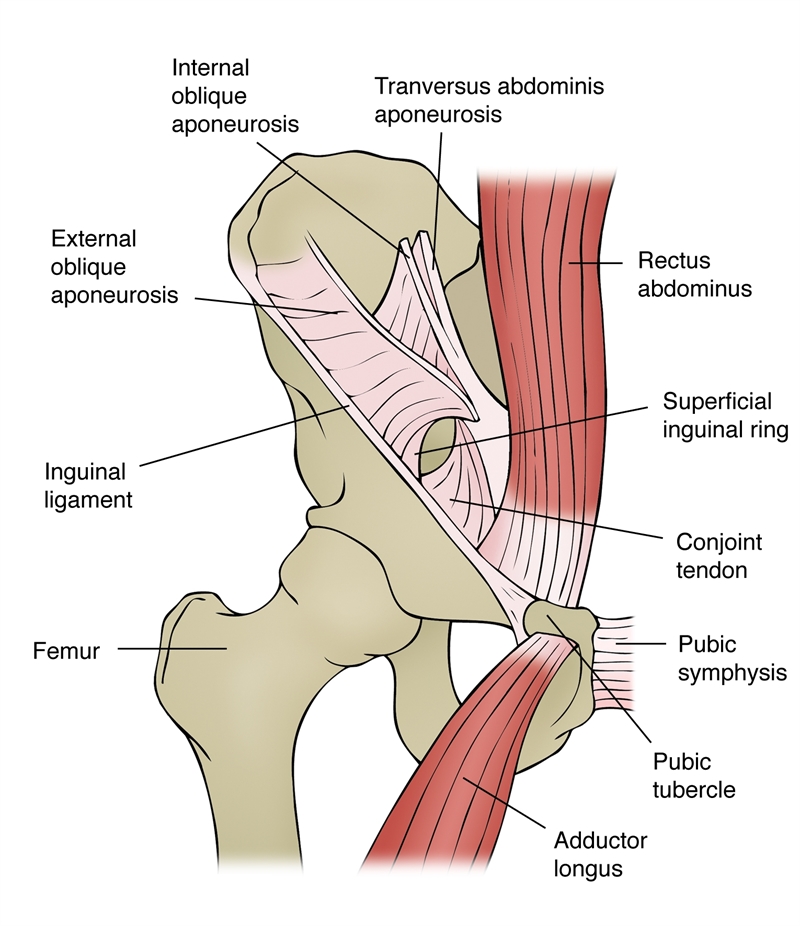
Diagnosis is made based on both clinical tests and the results of magnetic resonance imaging (MRI). Tests enable other causes of groin pain, such as pubic ostemyelitis, sports hernia and referring back or hip problems, to be ruled out. Once diagnosed, OP can be categorized into stages to help guide treatment and rehabilitation expectations (see table 1). The MRI results also help predict recovery outcomes. Italian researchers discovered that among professional athletes with OP, those that showed edema in the soft tissue and muscles at the pubic symphysis and greater signal intensity within the bone marrow of the pubic bone at the onset of symptoms, were more likely to experience only a partial recovery(2).
| Stage | Symptoms |
|---|---|
| I | Pain on one side feels better after warm up. Athlete able to participate in sport but symptoms become worse after training. |
| II | Pain felt on both sides, radiating into the adductor muscles at the groin, and worse after training. |
| III | Pain felt bilaterally in the adductor and abdominal muscles. Pain during activities such as kicking and sprinting prevent further participation in sport. |
| IV | Significantly worse pain felt in the adductor and abdominal muscles may also refer to the hips or low back. Pain interferes with normal daily activities such as walking. |
Most cases of OP are self limiting and respond well to conservative treatment(1). However, it isn’t uncommon to symptoms to last up to a year or more. Physical therapy treatment seeks to correct muscle and range of motion imbalances around the pelvis, manage symptoms through physical agents and modalities, and amend training errors through therapeutic exercise and guided return to sport. It’s important to note that the most effective part of this approach may be the therapeutic exercise. Athletes diagnosed with OP who received an active training program showed significantly better return to sport outcomes when compared to a group receiving only physical agents (79% to 14% respectively)(1). Specifically, strength training should focus on balancing the forces acting around the hip joints and pelvis. This includes the abdominal and back extensor muscles, as well as the hip flexor and extensor muscle groups.
Some suggest managing OP with injection therapy, specifically prolotherapy and corticosteroid injections. The evidence as to the efficacy of these treatments remains inconclusive. Some studies report relief, but not with a significant portion of the population studied(1). Therefore, these treatment approaches may best be reserved for the most unresponsive cases. Surgical intervention is indicated only in the most resistant 5% to 10% of cases.
Identifying the cause
Since groin injuries are the second most common type of muscle injury in soccer players, German researchers wondered if kicking was truly the biomechanical cause(3). They observed that soccer players passed more often than kicked and investigated whether or not the inside pass, more heavily utilized in today’s game, might play a greater role in the incidence of OP. To test the impact of the inside pass, they analyzed passing by 10 male competitive amateur club players using video movement analysis while players passed balls in the Footbonaut pass trainer.One interesting finding was the presence of internal rotation just before ball contact. While to the eye it appears that the leg externally rotates due to the foot position, the internal rotation actually serves to elevate the foot (see figure 2)(3). As some hypothesize that limited hip internal rotation contributes to OP (see above), athletes may strain the pelvis trying to compensate for what they lack in range of motion.
The researchers also calculated forces acting within the adductor and gracilis muscles. The load on the gracilis proved to be substantial, even in sub maximal effort passing. Furthermore, the gracilis elongates towards the end of the swing cycle, placing it at even greater risk for strain as it generates force while contracting eccentrically.
While the force produced by a muscle remains the same throughout the length of the muscle, the stress endured depends upon the cross sectional area. Therefore, as the gracilis and adductor longus muscles narrow towards their insertion, the stress upon the portion of the muscle near the insertion becomes greater. In addition, the pubic symphysis endures the forces of both muscles acting together during passing.
Repeated passing drills and increased training load likely contributes to the development of OP. Therefore, decrease the passing and kicking volume in the early stages of OP and strengthen the adductors and hip muscles through exercises such as bridging with a small ball between the knees, skating slider lunges, side lunges, and sumo squats.
Figure 2: Internal hip rotation with inside passing

Prevention
Norwegian sports scientists recently wondered if the addition of one exercise alone could decrease the incidence of groin injuries in soccer players. They assigned 18 semiprofessional male soccer teams to an intervention group, and 17 teams in the same league to a control group. The intervention group performed theFor more on hip and groin injuries, take advantage of our current special on the Hip and Groin Injuries: Prevention and Treatment book.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









