Painful truths: the physical impacts of emotional stress

Figure 1: Stress and homeostasis
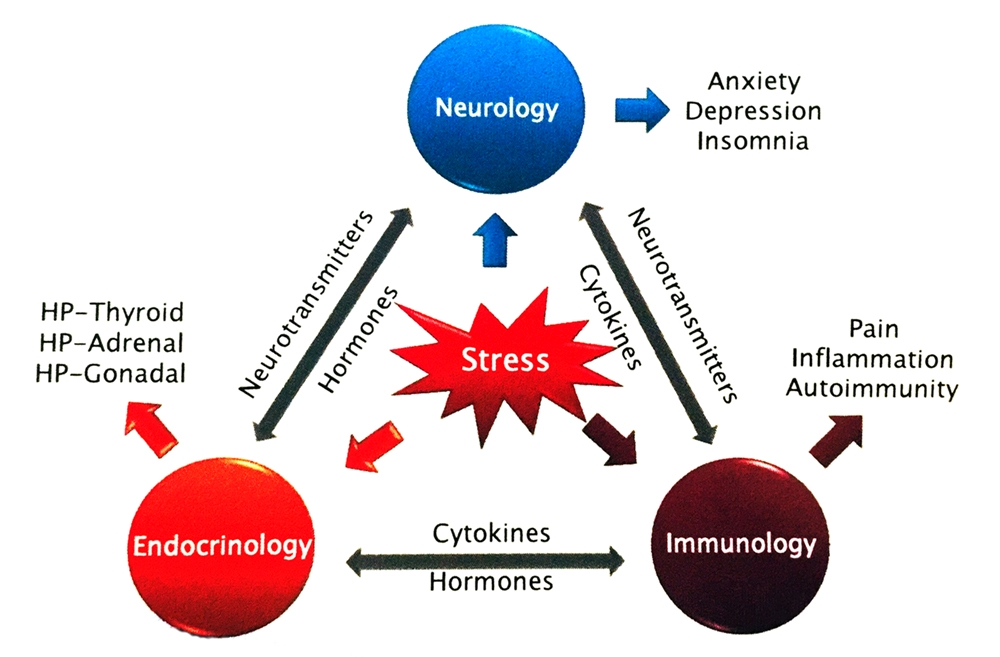
Through its impacts on the CNS, endocrine and immune systems, stress can alter the physiological homeostasis in the body.
Background
Athletes at all levels of sport are exposed to emotional and physical stresses, which may lead to the onset of pain or exacerbate the pain level percieved from an injury(2). When a stressful situation - whether pain or non-pain related - monopolizes someone’s thought processes it can overtake their life and affect their mental wellbeing. This in turn affects mood, the way a person carries their body, and their motivation to exercise. What physiotherapists sometimes miss is the emotional stress that a patient may be suffering, and which could be contributing to a patient’s pain. Although clinicians must be careful not to delve into areas beyond their expertise and take on the role of a counsellor, they must be aware of the psychological as well as physiological aspects of pain.Physiological response to stress
The physiological response to stress caused by fear (a perceived threat to safety, status or our well-being) can induce a chain of events both acute and chronic (see figure 2)(3). Fear of pain, failure, or the worst possible outcome, known as catastrophization, activates the amygdala in the brain, which triggers the HPA axis (hypothalamic–pituitary–adrenal axis – see figure 3) to release the sympathetic hormones norepinephrine and epinephrine(3). Once released into the bloodstream, these neurotransmitters cause an increase in heart rate, blood pressure, respiratory rate, sweat secretion, and narrowing of the arterioles(3).Figure 2: Acute and chronic physiological cycle of stress resulting in inflammation(3)
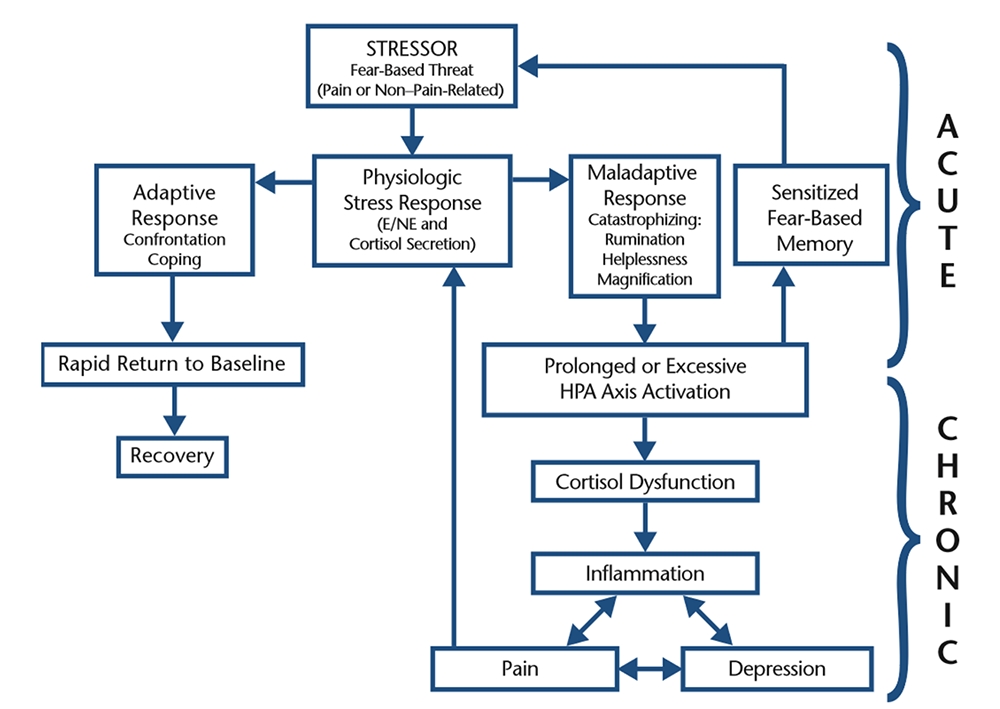
Figure 3: The HPA axis*
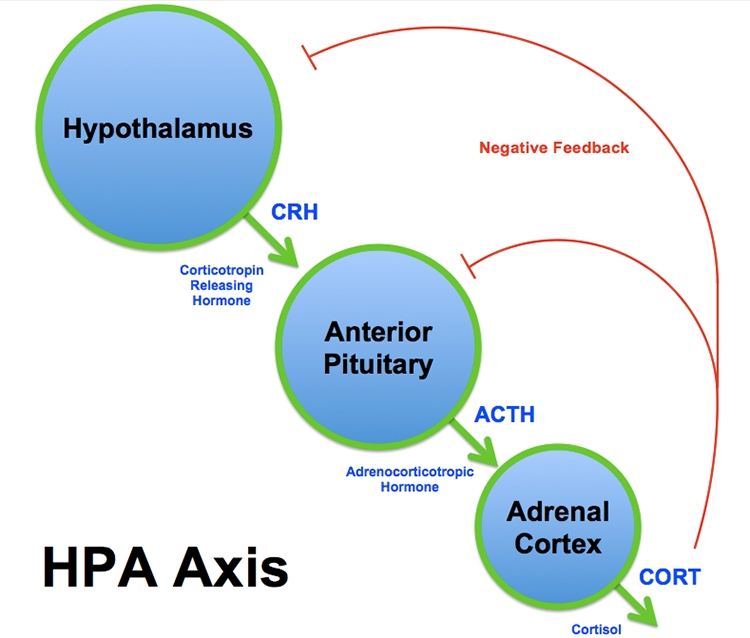
The HPA axis is a complex set of direct influences and feedback interactions between three glands: the hypothalamus, the pituitary and the adrenal glands.
*Image courtesy of Brian M Sweis, University of Minnesota
While the initial physiological responses to stress are regulated by the sympathetic neurotransmitters, there is also a neuroendocrine response to stress that is prolonged and delayed(3). During this secondary cascade, the anterior pituitary gland releases adrenocorticotrophic hormone (ACTH), which triggers the release of cortisol from the adrenal cortex. Within 15 minutes after the initial stress response, cortisol levels rise throughout the body and can remain elevated for a few hours.
Cortisol primarily functions as an anti-inflammatory; cortisol’s action is so effective that the synthetic version known as ‘corticosteroid’ is widely used to treat many inflammatory injuries(3). During a stress response, increased levels of cortisol mobilize glucose for fuel so that the body is ready to fight or flee, while the anti-inflammatory action inhibits pain, thus assisting the body in managing stress or perceived threat(3).
Prolonged stress
Prolonged stress, whether related to an injury or not, can deplete cortisol levels and result in cortisol dysfunction, which inhibits the body’s ability to deal with pain(3). Stress-induced inflammation due to hypocortisolism can be a factor in the occurrence of a number of conditions such as osteoporosis, chronic low-back pain, joint pain and chronic fatigue syndrome(3). Furthermore, many idiopathic inflammatory autoimmune diseases may be the result of widespread inflammation caused by chronic stress and impaired cortisol regulation(2). Signs and symptoms of stress induced cortisol dysfunction include:- Bone and Muscle breakdown
- Fatigue
- Depression
- Pain
- Memory impairments
- Orthostatic hypotension
- Impaired pupillary light reflex
Treatment and management techniques
Part of any physical therapy treatment process is to improve ergonomic positions and postural stress whilst improving muscle balance and reducing joint forces where needed (while bearing in mind that not every patient with postural stress and muscle imbalance will have a dysfunctional HPA axis and elevated cortisol levels)(3). Beyond the physical treatment, there exist a variety of techniques to improve physiological parameters and mood states to help patients to deal with pain, regulate cortisol levels and resolve a dysfunctional HPA axis.It is important to recognize that stress management protocols can be effective for healthy populations as well as those presenting with pain or a particular condition(1). Deep breathing exercises alone reduce stress, anxiety, depression. Researchers from Beijing University studied the effects of an 8-week program of diaphragmatic breathing exercises on healthy subjects(4). Participants inhaled as deeply and slowly as possible whilst expanding their abdomen and then exhaled as deeply and slowly as possible whilst contracting the abdomen. Subjects performed diaphragmatic breathing for 15 minutes in total in addition to 15 minutes of regular breathing. Salivary cortisol levels were taken prior to and immediately after the test. Compared to a control group that did not perform breathing exercises, the breathing intervention group had significantly lower levels of cortisol than the control group, suggesting lower stress levels.
Cortisol levels increase when muscle glycogen and blood sugar is diminished after exercise. During endurance training, drinks delivering 70 grams per litre of carbohydrate (as sugars) reduced post exercise cortisol levels. However, drinks containing only 15 grams per litre of carbohydrate had no effect(5). Therefore, endurance athletes should ensure glycogen stores are restored either during or immediately after exertion to maintain proper cortisol levels.
Sports scientists in the United States studied the effects of different types of music on salivary cortisol levels in 60 healthy females(6). The participants were randomly allocated to a rhythmic music group, sound of rippling water group, and a rest group (as a control) without acoustic stimulation. Saliva samples were taken at baseline measure and then immediately after one of the 10-minute auditory interventions.
Following the acoustic/control intervention, the subjects performed the ‘Trier Social Stress Test’ (TSST – which has been found to be a reliable stress test that activates the HPA axis and cortisol levels)(6). The test required participants to firstly talk for five minutes about why they are suitable for a particular job role and to list their qualities and personal attributes. The second task was arithmetic based; participants were required to count backwards for five minutes in values of 17 from the number of 2043 and if they stumbled, they had to return to 2043.
The results produced significant differences in the salivary cortisol levels between the groups, with the sounds of rippling water producing lower cortisol levels than the rhythmic music group. However, there wasn’t a significant difference when comparing the sounds of rippling water group to the control cohort before or after the stress test. The authors concluded that the music impacts the autonomic nervous system more than the endocrine system. It may therefore be beneficial for an athlete to listen to the sounds of rippling water in the lead up to a training event or rehabilitation session as a way to promote relaxation, and help alleviate the intensity of stress. In the same way, meditation lowers stress, helps manage pain, and can be employed before rehab sessions.
Summary
Emotionally-induced stress caused by a multitude of factors has the ability to trigger the HPA axis and increase cortisol levels. If the stress is persistent then cortisol levels can become dysfunctional resulting in excessive inflammation causing pain, fatigue and mental health issues. Pain after injury may itself become a primary stressor. To manage pain, athletes should learn relaxation techniques in conjunction with other physiotherapy interventions. Clinicians should be receptive to holistic approaches to treatment, which can help patients manage daily stresses by using familiar and motivating strategies.References
- Health Sci J.2011;5(2):74-89
- Psychoneuroendocrinology, 2005 Nov;30(10):1010-6
- Phys Ther. 2014 Dec;94(12):1816-25.
- Frontiers in Psych.2017 June;8:874
- Eur Food Res Technol.2016;242(12):2001-9
- Plos One.2013 Aug;8(8):e70156
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










