Patellofemoral pain: soleus to the rescue?

It is well understood that patellofemoral pain (PFP) has a high incidence rate among runners(1). There are many intrinsic factors which are believed to influence PFP in runners, including abnormal anatomical alignment and foot posture, as well as faulty foot landing patterns(2).
Multiple interventions have been developed in an attempt to mitigate these factors, including exercise programs to improve strength, neuromuscular control, and flexibility, with positive effects(3,4). In particular, a multimodal intervention program is recommended for the management of runners with PFP - specifically including gluteal and quadricep strengthening, and running retraining(5,6).
Interestingly however, there is limited research investigating the role of soleus in runners with PFP. We know that soleus length can influence PFP(7), and that greater duration of soleus activation distinguishes PFP from asymptomatic runners(6). Therefore, it is logical to conclude that there must be some justification for improving soleus capabilities for runners with PFP. This article will explore that notion.
The role of soleus in running
Soleus consists of 80-96% slow twitch muscle fibres(8), and is therefore thought of as a more ‘endurance’ muscle, but one whose role is largely eccentric in nature(9). During the running gait, the soleus muscle produces up to 50% of total vertical support force, which is made possible by the fact that it makes up to 52% of the volume of the posterior calf (see figures 1a and 1b)(10,11).Figure 1: Soleus muscle basic anatomy
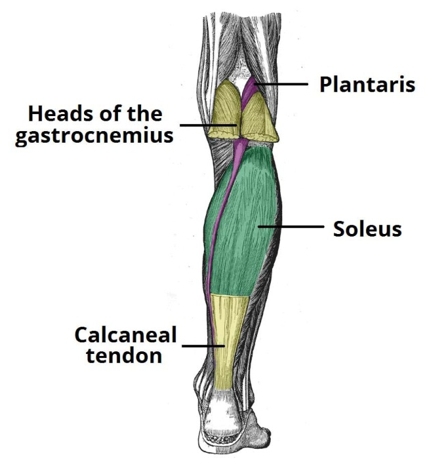
a) Showing soleus (gastrocnemius cut away for clarity).
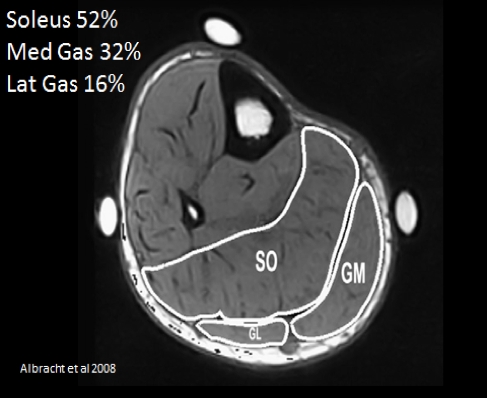
b) CT scanning shows that soleus muscle volume can account for up to 52% of the volume of the posterior calf(10,11).
During ground contact, soleus regulates knee flexion by controlling tibial movements in relation to the foot - and therefore the floor. In later stance, soleus decelerates the leg through its action at the ankle, and propels the trunk forwards through its plantarflexor function, producing vertical forces approaching eight times body weight(10).
These forces are thought to be as a result of the ‘bipennate’ structure of the soleus muscle. The fascicle attachments of the medial and lateral aponeurosis onto the central tendon has a larger oblique or pennation angle, which allows for a greater net force production, much like a pulley system (see figure 2 below)(12, 13). The degree of pennation angle of soleus is greater than that of any other of the tricep surae structures, and is found to be on average 15 degrees larger in men compared to women(12).
Figure 2: Pennation angle
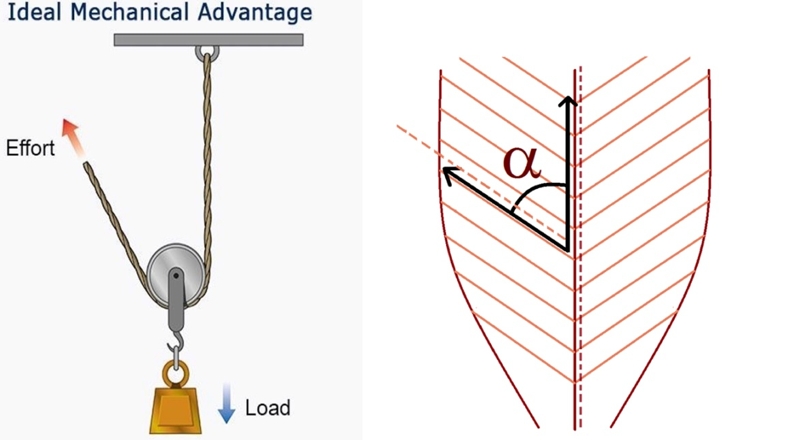
As the pennation angle (α) increases, more mechanical advantage is created, which allows for greater force production.
PFP and running
PFP is described as retropatellar pain or pain along the lateral and medial borders of the patella, and is the most common running injury with 17% of diagnoses(6). It has been suggested that runners with PFP show higher vertical loading rates of ground reaction forces during early stance, which have been linked with increased patellofemoral joint forces(6). Additionally, there is a link between PFP and runners with greater hip adduction, hip internal rotation, and tibial internal rotation, as well as a reduced contralateral trunk lean, and a reduced ankle dorsiflexion angle(7,14). Similarly, an increased peak knee flexion angle on landing, as well as over-striding; heavy landing patterns, and an upright running posture have all been suggested as risk factors for PFP in runners(2).As well as improving gluteal and quadricep strengthening(4,5), the benefits of practically applying running retraining to counter the above risk factors has been highlighted as a treatment for PFP(2). More specifically, addressing the presence of excessive hip adduction using visual (mirror) and verbal feedback, as well as increasing forward lean have been supported.
Of more interest to this article however, is the strong recommendation for increasing step rate or cadence to limit over-striding and reduce impact loading(2). This is performed using a metronome, music or verbal cues, and working towards reaching 180 steps per minute(2). The significance of this figure is supposedly related to more efficient power absorption of the hip, knee and ankle joints on impact, which is proposed to be linked with injury prevention (see figure 3 below)(15).
Figure 3: Effects of step rate on impact energy absorption(15)
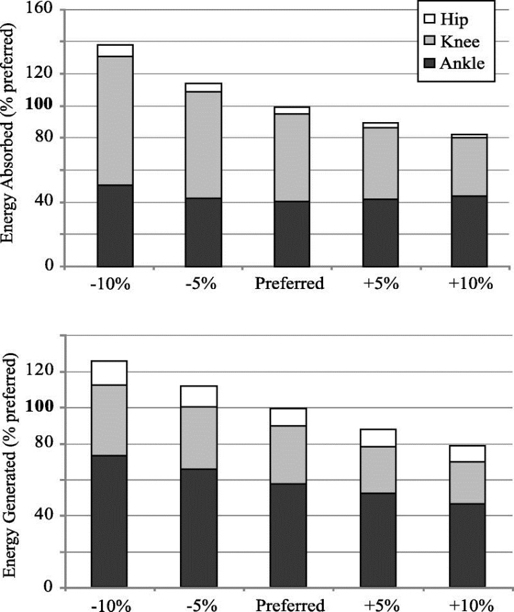
Research shows that at higher stride rates, less energy is generated (bottom) on impact and less energy therefore needs to be absorbed (top), particularly at the knee joint (shown in grey).
Assessing soleus length and strength
Measuring length- There are two reliable ways of assessing a runner’s ankle dorsiflexion range of movement, and therefore soleus length (see figures 4 and 5). Both have a good reliability and low measurement error(16), and can be easily applied in a clinical setting.The half-kneel, knee-to-wall test is measured in centimetres from the toe to the wall. It is measured at the point that the knee touches the wall, but the recipient must be able to keep their heel on the floor. The benefit of kneeling is to avoid any trunk/hip/ pelvic rotation compensation of the athlete, which produces a more accurate reading.
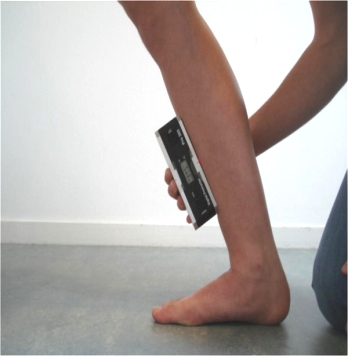
The tibial inclination angle is measured using an inclinometer or tilt meter. This is achieved by the athlete bending their knees over their toes without their heel elevating off the floor. By performing this bilaterally at the same time, again you will prevent any rotational compensation from the trunk or hips, which results in a more accurate measurement. Most commonly, an inclinometer application can be downloaded on smart phones, which makes it even easier to use in a clinical setting.
Figure 4: Half-kneel knee-to-wall test
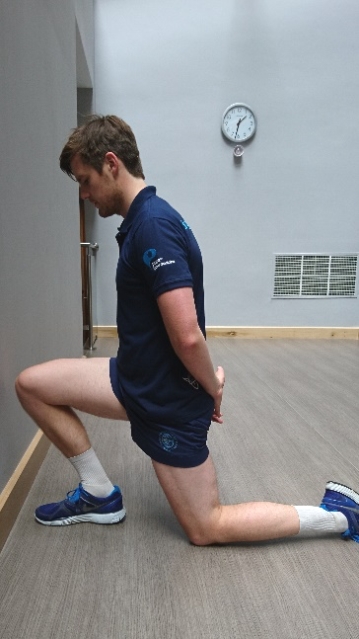
Figure 5: Tibial inclination angle using inclinometer
Measuring strength- Single leg soleus capacity testing can be assessed on the flat, or off a step in order to indicate the runners concentric and eccentric ability(17). This can be completed in standing, but must be performed with a knee flexion angle of 30-60˚to maximise soleus activation(18). This position can be aggravating for PFP however, so a seated weighted single heel raise (see rehabilitation section) might be more beneficial, and a comparison between each limb achieved.
Rehabilitating soleus for runners
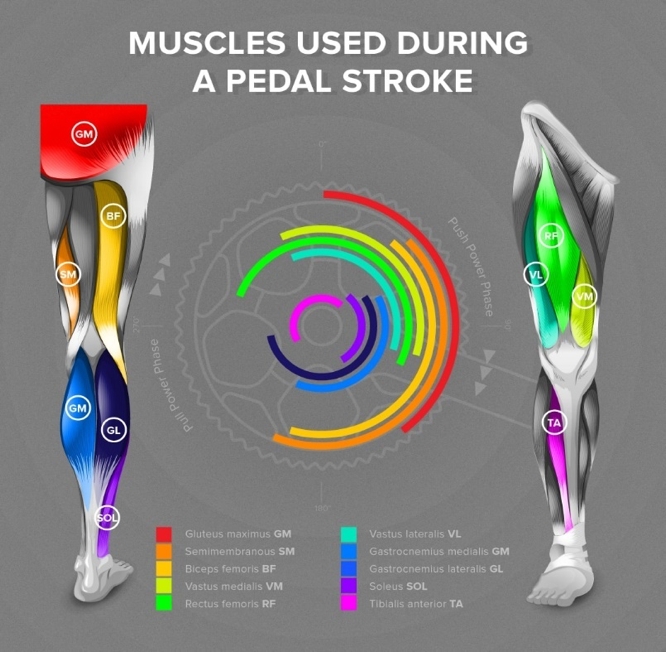
Considering the power output and endurance characteristics of soleus as well as the significance of step-rate retraining in runners with PFP, the inclusion of soleus rehabilitation for treatment is rationalised. The main aims of rehabilitation should be to improve the slow-twitch muscle fibre properties(8), and eccentric capabilities of soleus(9). This can be achieved in ways that are supported by evidence, but that can be applied in a clinical setting and avoid aggravating PFP levels.Use cycling to promote soleus activity- The greatest activation of soleus is achieved in the downstroke phase (ie 0-180 degrees) of cycling; from 45-135 degrees (see figure 6)(19). Likewise, achieving a pedal rate of 90+ repetitions per minute (rpm) will also generate improved EMG activity for soleus(19). More specifically however, research shows that around 32% of soleus’ maximum voluntary contraction (MVC) will be achieved when resisting a workload of 120W whilst cycling(19, 20).
Having the pedal positioned in the middle of the foot is also important for increasing soleus activity(21), as well as avoiding using toe-clip pedals which appears to reduce soleus activation(19). These variables can all be applied practically within a clinical setting to promote the activity of soleus in a runner who needs to maintain aerobic capacity, but may be restricted in their running capabilities due to PFP.
Figure 6: Bicycle crank position and soleus activity
Use balance training to promote soleus activity- We know that unstable surfaces can produce increased soleus EMG activity by 30-40%, particularly while squatting(22, 23). There can be many ways to apply balance training in a clinical setting. A good example is shown below (figure 7), which additionally works on retraining of knee-hip-ankle alignment control as previously mentioned(3,4).
It’s important that centre of gravity is placed over the standing foot and a knee flexion angle of 30-60˚ is maintained during the activity in order to gain maximum soleus activation(18). Anterior pelvic tilt should be promoted however, to avoid overload of the patellofemoral joint, which may aggravated PFP. Weight can also be added using dumbbells or kettle bells. Holding this position until fatigue is ideal.
Figure 7: Balance training to promote soleus activity

Use weight training (to promote slow-twitch muscle fibre and eccentric development)- A position of 80-90 degrees of knee flexion is recommended to isolate soleus activation(24), which is best to replicate when seated. As previously stated, this seated position will avoid aggravation of PFP because patellofemoral joint load is limited.
The best way to do this is by using the leg extension machine (see figure 8); ideally using a resistance equivalent to body weight and more, if manageable. A step can be added to promote eccentric contraction, and high repetition count of 30 reps should be targeted over four sets.
Figure 8: Weight training to promote soleus slow-twitch muscle fibre and eccentric development

Increasing soleus length- According to some research, runners with PFP present with reduced soleus length, which results in a decreased ankle dorsiflexion angle(7). A theory is that if athletes with PFP do not have sufficient dorsiflexion range of motion, they may use compensatory mechanisms such as excessive subtalar joint pronation. Consequently, they may experience increased lower extremity internal rotation, or perhaps external rotation of the lower leg, to gain additional motion during the terminal stance phase of gait(7). It has been suggested that tight plantar flexors and increased subtalar joint pronation will change how the lower extremity distributes joint reaction forces during gait, and might be a source of various running injuries(14).
Increasing soleus length can be achieved using a medicine ball for direct trigger point release to the muscle belly, or by stretching soleus through ankle dorsiflexion with knee flexion; holding for a prolonged period of 30-60 seconds (see figure 9).
Figure 9: Soleus trigger point release

Summary
PFP is a very common problem in runners. There has been much research debating the most appropriate management for this musculoskeletal injury. Surprisingly however, a very limited quantity has investigated the role of soleus.Given the significant force that soleus generates in the stance phase when running, and the recorded impact on PFP when its length is reduced, inclusion during rehabilitation must be taken into consideration. This rationale is further strengthened by the fact that increasing step rate or cadence in runners is now a recommended form of rehabilitation for PFP.
References
- Br J Sports Med, 2007; 41: 469-480
- Br J Sports Med, 2016; 0: 1-16
- Cochrane Database Syst Rev, 2011; 7: CD001256
- Br J Sports Med, 2014; 48: 871-7
- Br J Sports Med, 2014; 0: 1-13
- Gait & Posture, 2015; 41: 813-819
- J Orthop Sports Phys Ther, 2005; 35: 793-801
- J of Biomec, 2005; 0: 2-9
- Eur J Appl Physiol, 2006; 97: 298–306
- J of Exper Biology, 2012; 215: 1944-1956
- J of Biomech, 2008; 41: 2211-2218
- Muscle Nerve, 2000: 23: 1647-1666
- J of Applied Biomec, 2006; 22: 255-263
- Clin Biomech, 2012; 27(4): 366-371
- Med Sci in Sports Exerc, 2011; 43(2): 296-302
- Int J Sports Phys Th, 2012; 7(3): 279-287
- Brukner, P. in: Khan K. 2007 (3rd ed). Clinical Sports Medicine. Sydney. PA: McGraw-Hill Companies.
- J Jpn Phys Ther Ass, 2006; 9: 21-26
- J of Electr Kines, 2009; 19: 182-192
- J of Electr Kines, 2003; 13: 181-190
- Motor Control, 2001; 1: 36-49
- Can J Appl Physiol, 2005; 30(1): 33-45
- J Strength Condi Res, 2011; 25(9): 2605-15
- Physiol Rep, 2014; 2(6): 1-10
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









