Proximal tib-fib joint: an uncommon site for lateral knee pain

Pain about the lateral aspect of the knee is usually attributed to conditions such as iliotibial band compression/friction syndrome, lateral meniscus lesions and patellofemoral pain, and the supporting patella lateral retinaculum. In the absence of these conditions, other less common presentations could be lateral plica, fabella syndrome, biceps tendinosis, or popliteus tendinosis.
One of the more unusual forms of lateral knee pain in the athlete may be the proximal tibiofibular joint (PTFJ) - either as hypomobility or instability(1-4). This injury occurs in various sports involving twisting forces around the knee and ankle such as football, rugby, wrestling, gymnastics, long jumping, dancing, judo, and skiing. The range of symptoms it can cause, include outer knee pain (especially on weight bearing), locking and ‘popping’ in the knee and transient nerve symptoms. This makes this injury an important one to recognize and address, especially in high demand athletes.
Anatomy of the proximal tibiofibular joint (PTFJ)
The PTFJ is an inherently stable ‘plane like’ joint on the posterolateral part the knee, and is stabilized by a host of primary and secondary stabilizers (see figure 1)(5,6). The primary stabilizers include(7):- Biceps femoris tendon
- Lateral collateral ligament
- The primary capsule and ligament associated with the joint.
The secondary stabilizers include:
- Arcuate ligament
- Popliteofibular ligament
- Popliteus muscle and tendon
These soft tissues work together to stabilize the PTFJ. The biceps femoris supports the joint anteriorly, the popliteus posteriorly, the lateral collateral ligament superiorly, and the interosseous membrane inferiorly. Kinematic studies have indicated that the lateral collateral ligament serves as the major stabilizer of the PTFJ in extension(1,2). Because of the resistance provided by the lateral collateral ligament, most of the joint injuries are thought to occur while the knee is in flexion. This may explain the association between multi-ligamentous knee injuries that occur in flexion and PTFJ disruptions.
The joint is surrounded by a fibrous capsule, which is further strengthened by prominent accessory ligaments that blend into the capsule. Posteriorly, it has a thick single band, which runs in an oblique direction from the head of the fibula to the back of the lateral tibial plateau. This is covered by the popliteus tendon. Furthermore, a single weak band runs from the fibular head to the posterior aspect of the popliteus tendon. Anteriorly two or three bands run obliquely from the front of the fibular head to the lateral condyle of the tibia(7).
Figure 1: Anatomy of the PTFJ
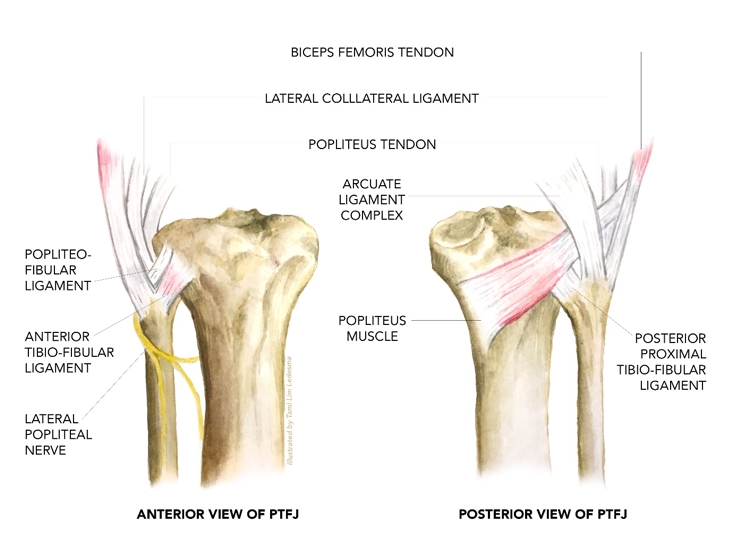
A synovial membrane- similar to that found inside the knee joint - lines the inner surface of the capsule of the PTFJ. In 10% of the population, this synovial space is continuous with that of the knee joint. The joint is intimately associated with the common peroneal nerve, moving forward from the popliteal fossa around the fibular head, and here it is vulnerable to injury. Such an injury to this nerve with an injury to the PTFJ may lead to foot drop and loss of sensation in parts of the leg and feet.
There are different anatomic variants of the PTFJ which can be classified into three types:
- Type I includes PTFJs with a nearly horizontal articular surface (less than 30° of inclination) and a surface area of less than 20mm(1,2).
- Type II includes PTFJs with a large, elliptical surface, concave on the fibula, and frequently having a joint communication to the knee.
- Type III includes PTFJs with a small articular surface (less than 15 mm) and a steep inclination (more than 30°)(8).
These anatomic variations must be considered when treating patients with an injury to the PTFJ.
Biomechanics of the PTFJ
The anatomy of the PTFJ directly relates to its functional stability. It can withstand stresses applied in either a longitudinal or axial fashion. Approximately one-sixth of the static load applied at the ankle is transmitted along the fibula to the PTFJ(9,10). Thus, the primary functions of the PTFJ are as follows:- Dissipation of torsional stresses applied at the ankle
- Dissipation of lateral tibial bending moments
- Tensile, rather than compressive, weight bearing(1,2).
As the ankle dorsiflexes, the PTFJ receives a torsional stress via external rotation and anterior glide of the fibula(4,8). Therefore, decreased mobility of the PTFJ may subsequently limit ankle dorsiflexion range of motion.
In 1974, Ogden evaluated anteroposterior motion of the proximal fibula with positional changes of the knee(1,2). When the knee flexes, the fibula moves anteriorly, and with knee extension, the fibula head moves posteriorly. It was found that with the knee flexed, the mobility of the proximal fibula increased and the fibular head could be moved approximately 1 cm in both anterior and posterior directions. With the knee extended, the excursion of the fibular head was minimal due to the stabilizing nature of the supporting soft tissues(1,2). There is also a slight upward movement of the fibula because of forced expansion of the malleolar mortise during maximal dorsiflexion of the ankle(11).
The shape and orientation of the PTFJ may also influence the way the PTFJ works. In a horizontal PTFJ, the two articulating surfaces are circular and planar, and their location provides some stability against displacement. In the oblique type of joint, the articulating surfaces are much more variable in the area, configuration, and inclination. The more oblique joints have the least area of contact between bones. Because this type of joint is less able to rotate and accommodate torsional stresses than a horizontal joint, it is thought to be more likely to dislocate.
The incidence of PTFJ injury
Injuries to the PTFJ are an uncommon consequence to the athlete. First reported in 1874(12), these injuries account for less than 1% of all knee injuries and have been reported to occur in isolation and in combination with other bony and ligamentous injuries such as tibial shaft fractures(9, 13, 14, 15). Injury severity can range from pain to subluxation to dislocation, with both acute and chronic presentations(1,2). Furthermore, it is also possible for PTFJ to be hypermobile and create movement issues at the knee and the distal ankle joint, particularly the inferior tibiofibular joint.PTFJ dislocation
PTFJ dislocations have been classified as follows(1,2):- Type 1 (subluxation only)
- Type 2 (anterolateral).
- Type 3 (posterosuperior)
- Type 4 (superior)
Associated peroneal nerve injuries are more likely to be associated with types 2 and 3. The mechanism of injury has been described as a sudden inversion and plantar flexion of the foot and ankle, with a simultaneous knee flexion and external rotation of the leg. For this reason, it is commonly associated with lateral ankle injuries, and therefore usually associated with a traumatic event in the sporting context. Typical mechanisms of injury would be twisting injuries, hard landings or slipping with the knee bent under the body.
Dislocation may occur in isolation or it may be seen alongside a fracture of fibula or the ankle, or with dislocation of the hip(1,2). Sports physicians should also be alert to subluxation of the joint (excessive forward to backward movement of the tibial head, causing symptoms), which is often associated with ligamentous laxity.
The nature of the traumatic event dictates the way in which the PTFJ will dislocate. Although there are four types of dislocation, the usual one in sporting contexts is anterolateral (type 2). In a flexed knee, the biceps femoris tendon and lateral collateral ligaments are relaxed(1,2). This, along with the external rotational torque of the tibia on the foot during twisting of the body, springs the head of the fibula out laterally. At this point, a violent contraction of the peroneal muscles, the extensor digitorum longus and the extensor hallucis longus (caused by sudden inversion and plantar flexion of the foot), pulls the fibula forward.
Signs and symptoms
Diagnosis of this injury is usually based on clinical history and clinical suspicion. Because of the nature of the presentation, it is commonly mistaken for a meniscal injury. Common signs and symptoms that may alert a sports medicine practitioner to a PTFJ injury are as follows:- Outer-knee pain, which is aggravated by pressure over the fibular head.
- Anterolateral prominence of the fibula head in type 2 injuries.
- Usually minimal effusion.
- Limited knee extension.
- Crepitus (grinding) on knee movement
- Pain on weight bearing.
- Visible deformity.
- Locking or popping.
- Ankle movements provoking lateral knee pain.
- Temporary peroneal nerve palsy (pins and needles on the outside of the leg). However, this is less likely in the athlete who suffers a type-2 anterolateral dislocation as the nerve courses close to the front of the fibula head.
Plain X-ray imaging is usually not helpful but may show the subtle signs of increased interosseous space and displacement of the fibula from its normal position. However, a CT scan may be needed to confirm the diagnosis(16, 17). The principal abnormality is lateral displacement on the anteroposterior view, and either slight anterior or posterior displacement on the lateral view(18). It has been suggested that computed tomography of the knee may be appropriate in patients where this diagnosis is suspected, because of the poor diagnostic value of plain radiology(16). MRI has the advantage of revealing ligament injuries as well as the dislocation.
Injury management
Currently, there is no definitive option for surgical treatment of acute dislocations of the PTFJ. The options are:- Closed reduction and immobilization in a plaster cast.
- Closed reduction without immobilizing.
- Temporary operative stabilization of the joint and repair of the joint capsule.
- Immediate joint fusion (arthrodesis).
- Resection of the fibular head.
The treatment options also vary with the pattern of dislocation. The management of type 1 and 2 injuries is reduction by anteroposterior pressure over the fibula head, with the knee slightly flexed and the ankle everted. There is often an audible and/or palpable relocation with rapid improvement in symptoms.
There is insufficient evidence to support or refute the use of immobilization after a reduction of type 1 or 2 injuries, although several previous case reports have recommended immobilization for varying periods with the knee in extension or slight flexion for 2-3 weeks(1,2,19,20). It is controversial whether weight bearing should be performed after the procedure(21). It is more difficult to reduce type 3 and 4 injuries, and these may require open reduction and fixation. However, attempting a closed reduction initially is an option. Several techniques have been described involving fixation and stabilizing with a portion of the biceps femoris tendon(22, 23).
A PTFJ injury is commonly missed, and a number of patients present with chronic lateral knee pain or joint instability. Unrecognized dislocations often present with peroneal nerve symptoms such as pins and needles in the leg or feet, or weakness of foot movements. There is no role for an attempted closed reduction in this situation.
Surgical stabilization is required in up to 57% of late or recurrent cases because of persistent pain and chronic instability(1,2,24). Patients with chronic pain secondary to this condition have been successfully treated with excision of the fibula head, reduction and temporary internal fixation, arthrodesis, and tendon reconstruction(25,26). Typical ligament reconstructions include iliotibial band or the biceps femoris tendon(25, 27-29). Resection of the fibular head is believed to affect knee stability and gait. The decision to remove hardware after arthrodesis remains controversial. It has been found that PTFJ arthrodesis with early screw removal at three to six months has obtained good results in athletes(30).
PTFJ Hypomobility
It is also possible for the PTFJ to develop hypomobility and positional faults. A possible explanation is that PTFJ dysfunction may be indirectly related a history of a previous ankle sprain(3). In particular, it has been documented that following an ankle sprain, positional changes in the talus, tibia, and fibula may result (31-33).Two positional faults have been described to occur at either the talocrural joint or the distal tibiofibular joint(34):
- At the talocrural joint, the talus is thought to migrate anteriorly following lateral ankle sprains due to the disruption of the ligaments restraining anterior talus translation(34).
- At the distal tibiofibular joint, a slight anterior displacement of the fibula relative to the tibia is thought to occur(31-33). Anterior translation of the distal fibula is associated with a concomitant posterior translation (external rotation) of the proximal fibula(1,2).
Clinically, the positional faults are recognized as decreased posterior glide of the talus or distal fibula, or decreased anterior glide of the proximal fibula, all of which manifest as decreased ankle dorsiflexion ROM(31-33). By addressing hypomobility of the PTFJ, lower extremity mobility may be restored, ultimately altering stresses placed at the local joint.
A simple and effective mobilization technique is to have the client lie supine and grasp the proximal fibula using the heel of the hand at the anterior aspect of the fibula, with the fingers curled around the posterior aspect of the fibula. As the fibula head has more inherent mobility at 90 degrees knee flexion, a mobilization of the joint in this position will improve the mobility of the PTFJ (see figure 2).
Figure 2: PTFJ mobilizations
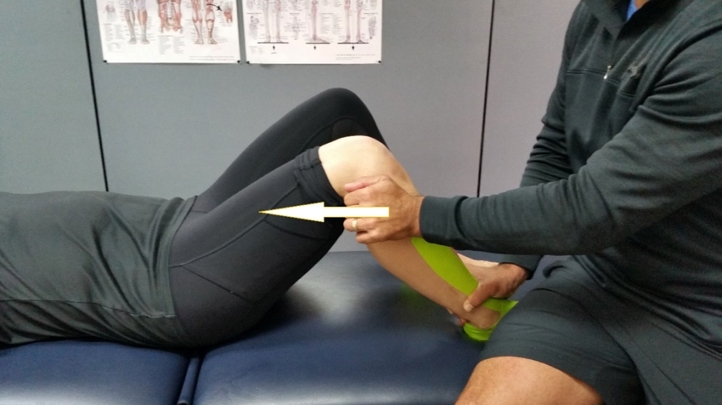
Conclusion
Injuries to the PTFJ are uncommon in the sporting knee. This injury type may manifest as frank instability and dislocation, or as a hypomobile joint following ankle sprains. Early diagnosis and treatment are essential to enable prompt rehabilitation. Treatment options vary according to the time of presentation, nature of the injury and associated morbidity. A return to sport is possible after successful treatment.References
- J Bone Joint Surg 1974;56-A:145–54.
- Clin Orthop; 1974. 101:192-197.
- J Orthop Sports Phys Ther. 1982; 3:129-132.
- J Orthop Sports Phys Ther. 1995;21:248-257.
- Emerg Med J. 2003;20(6):563.
- Knee Surg Sports Traumatol Arthrosc. 2006;14(3):241
- Arthroplasty Today; 2016. 2(3): 93–96.
- J Anat. 1952;86(1):1.
- J Bone Joint Surg Am. 1971;53:507–513.
- Gegenbaurs Morphol Jahrb. 1971;117(2):211.
- Moore K.L., Dalley A.F., Agur A.M., Limb L. 6th ed. Lippincott and Williams and Wilkins, Wolters Kluwer India Pvt; New Delhi: 2010. Clinically oriented anatomy; p. 508.
- Nelaton A. Elemens de Pathologie Chirugicale.Paris, France: Balliere; 1874. p. 292
- Am J Knee Surg. 1991;4:151–154.
- J Orthop Trauma. 1992;6:116–119.
- J Bone Joint Surg Am. 1973;55:177–180.
- Orthopaedics 1999;22: 255–8
- Br J Radiol; 1993. 66;108-11.
- Postgrad Med; 1989;85:153–63.
- Ann Emerg Med 1992;21:757–9.
- Am J Sports Med 1985;13:209–15.
- Cases J. 2009;2:7261.
- Arch Orthop Trauma Surg 1999;119: 358–9.
- Int J Clin Practice 2002;56:556–7.
- J Am Acad Orthop Surg. 2003;11(2):120
- 2001;17(6):668.
- Clin J Sport Med; 2007. 17(1), 75-77.
- Knee Surg Sports Traumatol Arthrosc. 1997;5(1):36.
- J Bone Joint Surg Am. 1986;68(1):126.
- J Bone Joint Surg Br. 2001;83(8):1176.
- Knee Surg Sports Traumatol Arthrosc. 2011;19(8):1406.
- J Orthop Sports Phys Ther. 2006; 36:3-9.
- Foot Ankle Int. 2000;21:657-664. 23.
- Foot Ankle Int. 2004; 25:318-321
- J Orthop Sports Phys Ther. 2002; 32:166-173.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










