Mindset and Return to Sport - Ready, Steady, Go!
Tracy Ward explores the basics of psychological readiness to return to sport, and identify some useful tools for clinicians with athletes in their care.
Following injury, athletes will experience different emotions, and their psychological responses will change as they progress through their rehabilitation. But when is an athlete psychologically ready to return to sport? This is often a commonly overlooked question – often because the physical outcomes of rehabilitation are much easier to measure and tend to take precedence.
Returning to sport following severe injury requires extensive rehabilitation, planning and preparations. The athlete must overcome the acute injury by initially allowing the physical damage to heal, and then by preparing prepare for their specific sport at the skill level required. They must also have the confidence, positivity and overall emotional strength to return to competitive play.
Although this preparation sounds simple, implementing such a plan and getting the timing correct is very complex. The rate of injury recurrence following return to sport is well documented across many injuries and sports. For example, the rate of recurrence following hamstring injuries is reported as 12% and 34% in British and Australian football respectively and is one of the highest rates of injury recurrence of all sports injuries(1, 2).
Evidence has also demonstrated a clear link between psychological readiness to return to sport and the ability of an athlete to return to their pre-injury level. Researchers have ascertained that athletes with positive psychological responses are much more likely to successfully return to sport at their previous level of participation, and also at a quicker rate than those with negative psychological responses(3, 4).
For example, following anterior cruciate ligament (ACL) injuries, just 50% of athletes will return to their pre-injury standards(5). Since an athlete’s pre-injury fitness, gender, and age apparently do not influence return to sport timings or success, it’s therefore logical to assume that there needs to be a greater emphasis placed on the quality of the rehabilitation measures and discharge to sport criteria.
Rehab expectations and injury
An athlete’s expectation and/or opinions also impacts injury recurrence rates. Athletes often severely underestimate the time to return to pre-injury level and sports performance is often reduced during the initial return to sport phase. Research shows that this can be because the athlete is not physically or mentally prepared.
For example, when a group of runners and dancers were asked to estimate when they would be back at their individual sports post-injury, the runners answered an average of four weeks and the dancers one week. The actual average return was 16 weeks for the runners and 50 weeks for the dancers(6). This greatly highlights the risk of premature return on their behalf. These figures demonstrate a greater need to ensure return to sport is correctly timed from ensuring the athlete is psychologically prepared, as well having realistic expectations and goals to aim for.
What is sports injury psychology?
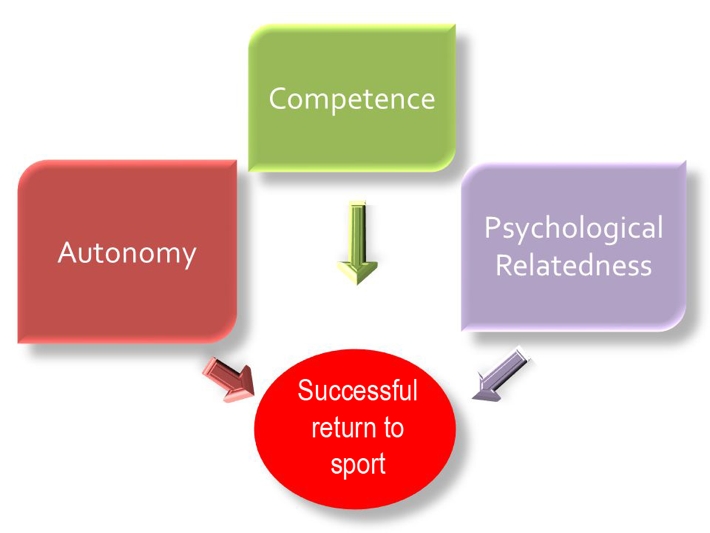
There are three key elements that are involved in addressing an athlete’s psychology in returning to sport (see Figure 1):
- Autonomy - the psychological factors that promote personal involvement. E.g. their motivation and drive to do it for themselves.
- Competence - the cognitive response to control the outcome. E.g. to overcome fear and build confidence.
- Relatedness - the athlete’s perception of interacting and belonging.
When all three of these elements are embraced, it is suggested the athlete has the best chance of successful return to sport(3). To fulfill autonomy, the athlete must recognise their own desires to return to sport. Reminding them of their position in the team or achievements and motivating them to get better through goal setting are useful tactics. Competence requires a reduction in fear and confidence building through progressive rehab drills, which gradually encourage more effort on the injured limb and a step closer to sports-specific scenarios. Providing a good support network from the whole multi-disciplinary team and continued inclusion despite not being able to train will address relatedness.
Fear and return to sport
When the athlete’s fear of returning to sport becomes disproportional to the actual event, or hinders the progression of rehabilitation, this can have substantial consequences on their performance and the timeframes. Evidence suggests that as rehabilitation progresses towards full recovery, an athlete’s emotions will shift from a negative outlook to a positive one - but the feeling of fear will remain until they perceive that they have made a successful return to sport(7).
Those who return to pre-injury levels of performance reportedly have the lowest level of fear of re-injuring themselves. It is therefore crucial to fully support the athlete during the transition from rehabilitation to sports-specific play. This will allow him/her to attain pre-injury performance levels, which results in a positive perception of themselves returning to their sport.
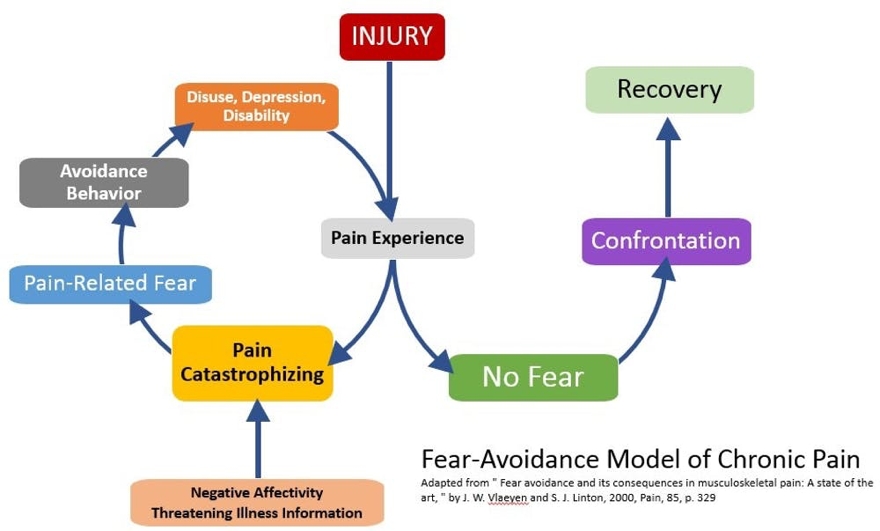
There are two ways that an athlete can choose to cope with this fear to overcome it and move forwards: confrontation or avoidance (see Figure 2). Those who experience fear avoidance are more likely to develop chronic pain from their injury, with a greater risk of not returning to their sport(8). This is in contrast to those who confront this fear of pain and deal with it appropriately. To assist with confrontation, rehabilitating the injured limb to match the capability of the non-injured limb - and demonstrating this clearly to the athlete - will help with forming positive psychological responses and confidence about using the injured limb in return to sport(9).
Figure 2 above shows how a negative pain experience can initiate the catastrophe of fear and anxiety, whereas low fear will more likely result in confrontation and success(10). To further help with identifying those more at risk of maladaptive psychological responses to injury various assessment tools have been designed. These range from injury specific, to general identification of fear avoidance and anxiety on returning to play.
Assessment tools
Numerous questionnaires now exist to try and identify fear avoidance, anxiety, and general psychological readiness to return to sport following injury. Depending on the athlete’s situation, clinicians are advised to pick the best assessment tool for that athlete or use a combination and then use these results to diagnose early onset of negative psychological factors. This provides a greater chance of converting these to positive psychological factors early in the rehabilitation stage. This in turn can help to ensure a smooth transition to sport when rehabilitation and sporting demands get more challenging.
| Eccentric loading guidelines used for tendiopathies (1) |
|---|
| One REP MAX to determine load should be avoided to prevent further damage. Load should be determined by number of repetitions rather than weight. 3-4 sets of 6-12 repetitions to start initially. 4 sessions per week as opposed to daily. Lift with two legs and lower with involved leg. |
Physical tests for psychological guidance
Some physical tests can also demonstrate the psychological readiness of an athlete, because certain movements not only rely on the physical factors of skill, mobility, strength etc., but the athlete must also be confident performing the task without hesitation and be able to commit fully to the action. Here are some examples that can provide good indications of confidence prior to returning to play.
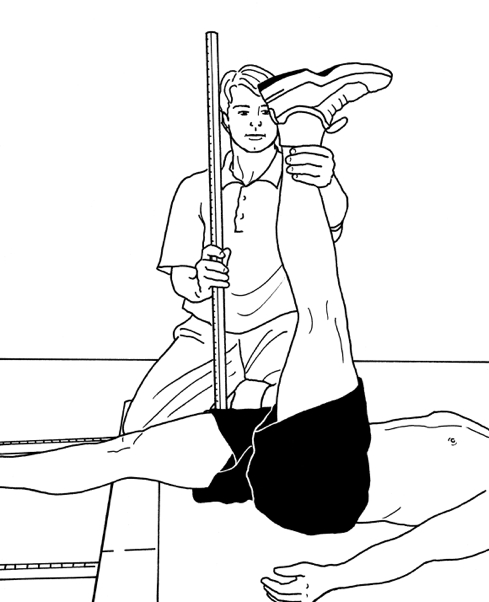
The H-Test (Figure 3)
The H-test assesses the physical readiness of the hamstring muscles but also accounts for athlete confidence in performing a rapid test on the injured leg. The test is performed lying flat on the back. The athlete raises their injured leg straight upwards from the hip as high as possible. This is to be performed once for practice and then three consecutive times at speed. The degree of flexibility should be recorded and the athlete then rates their level of insecurity performing this task using a scale of 0-100, with 100 being the most insecure(14). If an injury is still present, the test may reveal a reduced level of flexibility (height) or a higher degree of insecurity on the injured leg compared to the uninjured side.
Throw and catch test (Figure 4)
This can be completed with varying weights/sizes of balls, which can also be thrown at different speeds until the action replicates the intensity of the sport. The number of successful attempts is recorded. Athletes with low levels of confidence/high levels of fear may often score poorly due to avoidance, even though less dynamic tests indicate good shoulder rehabilitation(15).
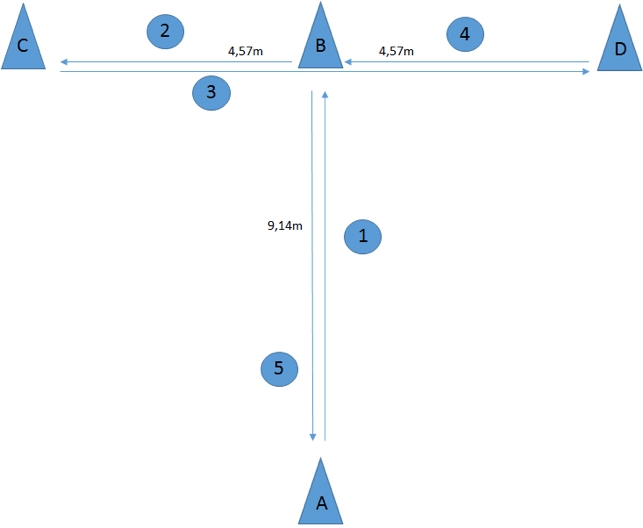
The T-test (Figure 5) (16)
A tightly woven T-shape is run following the numbers 1-5, and the time taken recorded. This can be compared to future trials as the athlete progresses, as well as observing their path and the effort it takes to turn the tight corners.
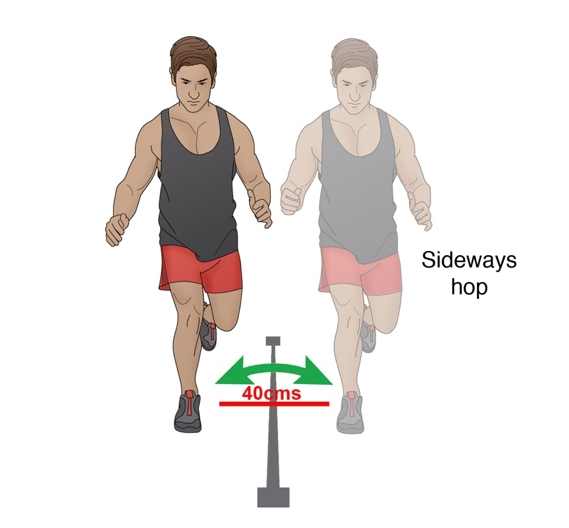
Side hop test (Figure 6)
The side hop test consists of jumping on one foot laterally from side-to-side over two lines that are placed 40cm apart. The number of hops achieved within 30 seconds is recorded. This can be compared to the uninjured leg. The side hop test has a greater ability to determine side-to-side deficits compared to other hop tests(16).
Additional psychological tools
To further assist with return to sport readiness, there are several tools and techniques the physiotherapist and team coaches can implement to support the athlete further and promote a smooth transition back to competition:
- Muscle relaxation and breathing control - Having good, steady breathing control can reduce the heart rate, stress levels, and anxiety. This involves taking a deep inhalation and a slow exhalation, and repeating several times. As the athlete follows these breaths they should focus on the abdominal muscles and the movement of their diaphragm. This can provide relaxation and focus the athlete’s attention on just the breathing cycle. As they continue to focus on their breath, they should then try to focus on their skills required or a critical aspect, giving a more directed thought process without distractions or anxieties. This technique can be good to bring the athlete under control when negative thoughts or increased anxiety are escalating.
- Mental imagery and routine preparation - Visualising training sessions and game activity can be a useful skill for mental preparation. This allows the athlete to focus on each key stage, and rehearse the technical skills, positioning, behaviours etc. they wish to execute. If there is a particular skill they struggle with, or a challenging situation, it can be useful to imagine this situation and focus on executing it correctly step by step. Visualising the athlete’s pre-competition routine and having a set routine is also an important strategy. This provokes consistency and ensures the athlete is always prepared prior to the event ahead. Adhering to this strict routine can help alleviate fears or insecurities because the athletes has been trained to go through things systematically, one task at a time, until event time. This regime promotes calmness and minimises extra stress.
Summary
Sustaining a sports injury can escalate psychological responses. The athlete requires multi-disciplinary support, motivation, goal setting, and encouragement to ensure a positive emotional response, and to minimise any fear avoidance and anxiety that may delay returning to sport. Fear is inevitable following an injury and therefore fearful thoughts must be dealt with appropriately to ensure progression through rehabilitation.
Avoiding dealing with fear of pain can lead to chronic pain and puts an athlete at risk of a delayed return to sport. Several assessment tools exist that can measure fear avoidance, anxiety, psychological readiness, as well as injury specific questionnaires. These should be used, along with physical tests, to identify negative psychological responses to injury and minimise their further development.
References
- Sports Med. 2004; 34(10):681-695
- Clin Exp Phar Phys. 2004; 31:546-550
- Br J Sports Med. 2013; 47: 1120-1126
- Br J Sports Med. 2014; 48: 1613-1619
- Br JSports Med 2015. 49: 1295-1304
- Br JSports Med. 2006 June;40:40-44
- Knee Surg Sports Traumatol Arthrosc. 2005; 13(5): 393-397
- Behav Res Ther. 1983; 21(4): 401-408
- J Sports Rehabil. 1998; 7:206-220
- J Behav Med. 2007; 30(1): 77-94
- J Athlet Training. 2014; 49(3): 000-000doi: 10.4085/1062-6050-49.3.75
- J AthletTraining. 2009; 44(2): 185-189
- PhyTher In Sport. 2010; 11: 23-29
- Knee Surg Sports Traumatol Arthrosc.2010 Dec; 18(12):1798-803
- Clinical Sports Medicine. 2006, Revised Third Edition; Australia: McGraw-Hill
- Knee Surg Sports Traumatol Arthrosc. 2006 14:778-788
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.