Suprascapular nerve injury: a common entrapment for overhead athletes

Injury to the suprascapular nerve (SSN) is a common cause of shoulder pain and weakness in the overhead athlete, and its aetiology is still poorly understood. First described in a case study by German neurologist E.Schilf in 1952⁽¹⁾, Kopell and Thompson (1959) expanded upon compression observed at the suprascapular notch⁽²⁾. Another entrapment site was described by Ganzhorn et al (1981)⁽³⁾who described the first case of spinoglenoid notch entrapment.
SSN is currently of interest as a potential site of injury in the overhead athlete due to its unique anatomical relationship with osseo-ligamentous tunnels, which makes it vulnerable to compression and traction in overhead movements. Research suggests that up to 34% of beach volleyball players⁽⁴⁾and 52% of elite female tennis players⁽⁵⁾may suffer from this problem.
Anatomy and biomechanics (see figure 1)
The SSN originates from the upper trunk of the brachial plexus by the ventral rami of primarily C5 and C6 (76% of cases), C4,C5 and C6 (18%) and C5 alone (6%)⁽⁶⁾. The nerve courses laterally through the posterior cervical triangle, obliquely posterior to the clavicle, and enters across the superior border of the scapula into the suprascapular notch.⁽⁷⁾It passes underneath the transverse scapular ligament, with the suprascapular artery and vein passing over the top of the transverse ligament⁽⁸⁾. Two branches originate at this level: a thick branch (motor) for the supraspinatus muscle, and a longer one (sensory), which disappears into the acromiocoracoid dome within the subacromial bursa.Figure 1: Anatomy of the SSN
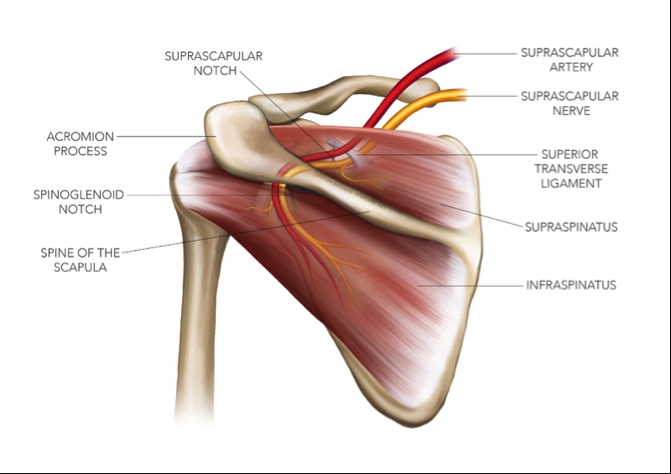
The SSN continues to course laterally and passes under the spinoglenoid ligament at the spinoglenoid notch and at this point supplies the infraspinatus with a motor branch⁽⁸'⁹⁾. The presence of the spinoglenoid ligament is variable with reported ranges from 50 to 72%⁽¹⁰⁾. It is more common in men then women (87% and 50% respectively)⁽¹¹⁾.
The SSN is recognized principally as a motor nerve, however it does also have sensory innervations to the coracohumeral and coracoclavicular ligaments, the acromioclavicular joint and the shoulder capsule and bursa⁽¹²'¹³⁾. However, this nerve has no skin sensory fibres.
Injury to the SSN
The SSN may be compressed or injured in a numerous number of ways. These include:
- Stenosis and compression of the nerve. Six different types of anatomic variations of suprascapular notch anatomy have been described⁽¹⁴⁾. Depending on the shape and depth of the notch, shoulder motion may cause an angulation of the nerve, pressing it against the suprascapular ligament or a bony edge, resulting in irritation of the nerve.
- Dorsally located ganglion compressing the nerve distal to the suprascapular notch. Males seems to suffer from this the most⁽¹⁵⁾.
- Labral tears and glenohumeral instability may lead to supraglenoid or spinoglenoid cysts, which may impinge the nerve⁽¹⁶'¹⁷'¹⁸⁾.
- Calcification in the suprascapular ligament⁽¹⁹⁾.
- Fractures of the suprascapular/spinoglenoid notch⁽²⁰⁾.
- Scar formation as a result of a clavicle fracture if located proximal to the suprascapular notch⁽²¹⁾.
- Thickened supraspinatus fascia, which may contribute to entrapment of the suprascapular nerve in the supraspinatus fossa⁽²²⁾.
- Anatomical abnormalities such as a hypertrophied inferior transverse scapular ligament⁽²³⁾and enlarged spinoglenoid notch veins⁽²⁴⁾.
- Particular viruses that lead to neuritis (such as Turner-Parsonage syndrome)⁽²⁵⁾.
- Rotator cuff tears which lead to medial retraction of the supraspinatus tendon. The retracted tendon creates tension by altering the angle between the nerve and its first motor branch⁽⁹'²⁶⁾.
The unique causative features that relate to an athlete include;
- Particular sporting actions (particularly overhead sports) may make injury to the SSN more common⁽²⁷⁾. Tennis players may be affected at the suprascapular notch, while volleyball players are more prone to entrapment at the spinoglenoid notch due to ‘float pass’ serves⁽²⁸⁾.
- The unique kinematics of the scapula during volleyball, which requires extreme upward rotation, posterior tilt and horizontal adduction⁽²⁹⁾.
- Throwers with an increased range of motion at the shoulder may be subject to damage to the SSN in the follow-through phase of throwing⁽³⁰⁾. The supraspinatus and infraspinatus impinge upon the scapular spine with excessive abduction/external rotation movements. The result is the motor branch of the SSN is squashed into the infraspinatus⁽²⁸'³¹⁾. This may be further compromised by particular anatomical variations in the suprascapular-scapular angle, which place greater compressive and tensile forces on the lateral branch of the SSN⁽³²⁾.
- The termination of the SSN under the infraspinatus may also predispose the nerve to traction⁽²⁸⁾.
- The SSN may elongate as much as 25% with extreme motions of the shoulder⁽³³⁾. This may be a factor in athletes who need large amplitudes of repetitive movement with throwing actions.
- Witvrouw et al (2000)⁽³⁰⁾and Ferreti et al (1997)⁽²⁸⁾found that although the condition is common in volleyball players, they did not show progressive shoulder dysfunction or any increased incidence of painful overuse syndromes.
Signs and symptoms
Clinical examination and history alone are usually insufficient to make a diagnosis of SSN pathology. Many conditions around the shoulder can present with the same symptoms, and therefore need to be excluded. The possible signs and symptoms an athlete may present with include⁽¹⁵⁾:- Deep and poorly localized posterolateral shoulder pain.
- An insidious onset of pain with no shoulder trauma (common).
- A history of blunt trauma to the back of the shoulder, previous shoulder surgery and repetitive overhead activity (less common).
- Athletes may describe shoulder weakness or refer to arm, anterior chest and neck pain.
- Thumb pressure over the spinoglenoid notch may elicit the pain⁽³⁴⁾.
- Possible wasting and weakness in supraspinatus and infraspinatus if the injury is at or above the suprascapular notch. Weakness/atrophy in the infraspinatus alone if it is below the suprascapular notch⁽¹⁸⁾.
Testing
Injury at the spinoglenoid notch observed in athletes such as volleyball players usually results in a painless atrophy of the infraspinatus muscle⁽³⁵⁾. An orthopaedic test has been described by Lafosse (2011) and is referred to as the ‘suprascapular nerve stretch test’⁽³⁶⁾.The purpose of this test is to provoke pain at the back of the shoulder by compressing the suprascapular notch against the SSN. The clinician holds the head of the patient in rotation away from the affected shoulder. The scapular is then retracted with the other hand. If posterior pain is reproduced then this is considered a positive test.
Alternatively, the ‘cross-body adduction test’can be useful as a diagnostic tool for suprascapular nerve entrapment in either the scapular or spinoglenoid notch. This is test is performed by adduction of the forward flexed arm across the body (this tenses the nerve and may increase the pain). The test can be enhanced by simultaneous external rotation of the humerus. This activates the infraspinatus and supraspinatus and places the SSN under greater tension and accentuates the impingement of the SSN on the medial border of the scapula at the spinoglenoid notch⁽³⁷⁾. Injection of local anaesthetic as a diagnostic block into the suprascapular or spinoglenoid notch can be useful to investigate the source of pain⁽³⁸⁾. The relief of pain is immediate and of short duration.
Imaging
MRI of the shoulder can visualise the degree of supraspinatus and infraspinatus atrophy; look for soft tissue masses around the shoulder; assess for labral and rotator cuff pathology; find cysts compressing the nerve; and examine the course of the nerve itself through the bony prominences. However it is not so helpful if the transverse ligament is compressing the SSN⁽¹⁵⁾. Electromyography (EMG) combined with nerve conduction velocity (NCV) studies are the gold standard diagnostic techniques. Indications for the use of EMG and NCV are⁽³⁹⁾:- Unexplained supraspinatus and infraspinatus muscle atrophy suggesting SSN pathology.
- Undiagnosed and recalcitrant posterosuperior shoulder pain.
- MRI that showing muscle oedema (suggesting a nerve injury).
- Large rotator-cuff tendon rupture with retraction.
- Weakness in external rotation. The accuracy of diagnosing SSN pathology in the presence of external rotation weakness was 91% in a study⁽⁴⁰⁾.
Treatment
As a rule of thumb, those patients who present with an overuse type of SSN injury tend to fail with surgery whereas patients who have a definitive compression due to structure tend to show positive results following decompression surgery⁽⁴¹⁾. Therefore, non-surgical treatment is suggested as the preferred course of action in those with an overuse-type etiology⁽³³⁾.The primary features of a conservative rehabilitation protocol include:
- Relative rest from provoking activities.
- Soft tissue work on tight and constricted scalene, supraspinatus and infraspinatus muscles.
- Cervical spine mobilisations at the C4-C6 level.
- Strengthening of the residual fibres of the external rotators (teres minor and infraspinatus) in a variety of positions to train the muscle in different planes and angles. This helps re-establish a satisfactory muscle balance and function, minimising the risk of progressive shoulder dysfunction.
- Injection of a corticosteroid into an entrapment at the suprascapular or spinoglenoid notch.
Surgical decompression of the SSN would be indicated if conservative treatment fails or if a structural and reversible cause of nerve entrapment is suspected in the suprascapular and spinoglenoid notch. Poor outcomes with conservative management are found in those with⁽⁴¹⁾;
- A long duration of symptoms.
- Marked muscle atrophy.
- Entrapment by a mass lesion
- Associated with a massive rotator cuff tear.
- If a paralabral ganglion cyst is present, then early decompression is recommended to prevent further long-term nerve damage⁽³⁴⁾.
Summary
Due to anatomical factors, the SSN is vulnerable to traction and/or compression type injuries; especially in overhead sports athletes such as volleyball, tennis and throwing sports. SSN pathology can often only be diagnosed by excluding other pathologies. Conservative treatment is usually preferred. In recalcitrant cases, surgical decompression and/or repairing damaged labral tissue, and removing paralabral cysts may be necessary.References
- Nervenarzt 1952; 23(8): 306-7.
- Surg Gynecol Obstet 1959; 109(1): 92-6.
- J Bone Joint Surg [Am] 1981;63:492–4.
- Am J Sports Med. 2012. 40(10):2303–2308.
- Am J Sports Med. 2015. 43(8):1989– 1993
- Surg Radiol Anat 2010; 32(3): 235-8.
- AnatomiaClinica 1981;3: 67–71.
- Arthroscopy 1990; 6(4): 301-5.
- J Bone Joint Surg Am 1992; 74(1): 36-45.
- J Bone Joint Surg [Am] 1991;73:1061–3.
- Int Orthop. 1 2 : 273–275, 1988
- Clin Orthop Relat Res 1996; (330): 202-7.
- J Shoulder Elbow Surg 2008; 17(3): 500-2.
- Neurosurgery 1979; 5(4): 447-51.
- International Orthopaedics (SICOT) (2002) 26:339–343
- Ann Acad Med Singapore 2007; 36(12): 1032-5.
- Neurology 2008; 70(11): 890.
- Arthroscopy 1995; 11(6): 727-34.
- Knee Surg Sports Traumatol Arthrosc 2003; 11(6): 393-8.
- Acta Orthop Scand 1978; 49(4): 338-40.
- J Orthop Trauma 2005; 19(5): 343-5.
- Surg Radiol Anat 2010;32:277–84
- Ann Neurol 1982; 12(3): 314-6.
- Skeletal Radiol 2003; 32(2): 72-7.
- Radiology 2006; 240(2): 501-7.
- J Shoulder Elbow Surg 2003; 12(5): 497-500.
- Br J Sports Med 1994; 28(3): 177-9.
- J Bone Jt Surg - Ser A 1987; 69(2): 260-3.
- Br J Sports Med 2013;47:239–244
- Br J Sports Med 2000; 34(3): 174-80.
- J Shoulder Elbow Surg 1998; 7(5): 516-21.
- Surgical and Radiologic Anatomy 2018’ 40:333–341.
- J Bone Joint Surg Am 1997; 79(8): 1159-65.
- Clin Orthop Relat Res 1999; (386): 92-100.
- Arch Phys Med Rehab. 1988. 69. 641–643.
- J Shoulder Elbow Surg 2011; 20(2)(Suppl.): S9-S13
- Narakas A: Compression syndromes about the shoulder including brachial plexus, in Szabo RM (ed): N e r v e C o m p r e s s i o n S y n d r o m e s : D i a g n o s i s a n d T r e a t m e n t . Thorofare, NJ, Slack, 1989, pp 236–239
- C l i n O r t h o p 1 2 3. 1977. : 73–75.
- Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 516985, 6 pages doi:10.1155/2012/516985
- Muscle Nerve 2002; 26(2): 201-5.
- Clin Orthop Relat Res 2001; 386: 131-8.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Further reading
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










