You are viewing 1 of your 1 free articles
The Athlete’s Pelvic Floor
Tracy Ward discusses pelvic floor dysfunction in athletes, outlines the implications for rehabilitation, and raises awareness with a view toward prevention.
The impact of female pelvic floor dysfunction (PFD) is a hot topic in women’s health but rarely discussed within the context of sport. This oft-ignored problem affects both men and women and impacts an athlete’s quality of life and sporting performance. Data suggests that around 75% of mothers will experience PFD later in life(1). Of these postnatal women, 4-35% may experience stress urinary incontinence (SUI)(2). However, PFD also occurs in those who’ve never given birth. In fact, 12.5-80% of nulliparous athletes (those who’ve never experienced childbirth) suffer from SUI, putting the athletic population at higher risk for PFD(3).
Stress urinary incontinence (SUI) is the involuntary leakage of urine as a result of increased intra-abdominal pressure (IAP)(4). A rise in pressure within the abdominal cavity occurs with activities such as coughing, holding deep breaths, heavy lifting, and high impact exercise. The more frequently these activities occur, the greater the strain they exert, and the greater the risk of PFD. Just like normal skeletal muscles, pelvic floor muscles fatigue when exposed to long periods of IAP. This leads to compromised function.
PFD Risk Factors
Pelvic floor dysfunction (PFD) refers to a wide variety of disorders that can occur when the pelvic floor muscles and ligaments become impaired. This may include urinary or fecal incontinence, incomplete emptying of bladder, painful sex, and organ protrusion of the vagina, rectum or uterus. Symptoms vary but usually involve some form of discomfort, leaking, dragging sensations, and ‘bulging/bearing down’. PFD has also been related to lower back pain(5). Risk factors for developing PFD include(6):
• Complications with vaginal delivery.
• High birth weight of baby greater than 4kg.
• Three deliveries or more.
• Birth of twins or more.
• Chronic constipation.
• Increased maternal age.
• Exposure to increases in IAP.
• Excessive weight.
• Repeated impact exercise.
Pelvic Floor Basics
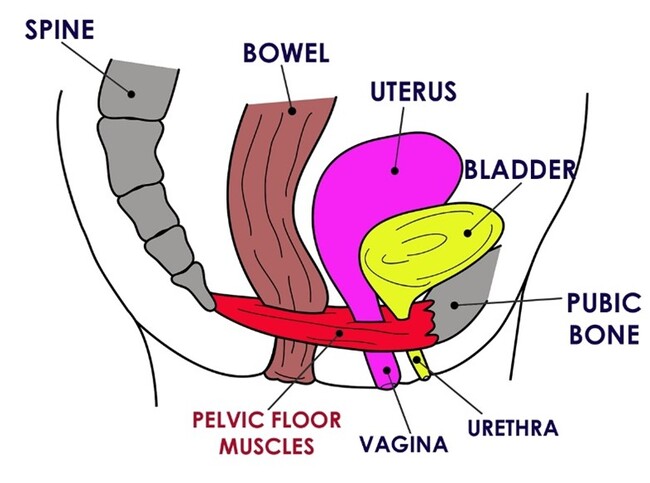
The pelvic floor musculature supports the base of the pelvis and all the internal organs inside it (see figure 1). The pelvic floor extends from the pubic bone at the front to the sacrum/coccyx region at the back, and from the inner side from the obturator internus to the outer aspect of the greater trochanter. These muscles are responsible for supporting the bladder, rectum, and uterus. They ensure the correct functioning of the organs by assisting the closing force of the bladder and bowel passages to prevent leakage and allowing relaxation for effective emptying.
Different Sports, Different Effects?
Athletes are at greater risk of SUI due to their continued exposure to increases in IAP throughout training. Most sports involve one of two exercise forms: jumping and landing (e.g., running, athletics) or the Valsalva maneuver (e.g., weight lifting). These two activities exert different deformations upon the pelvic floor due to their distinct direction and type of pressure loads (see table 1). The maximal IAPs experienced in jumping and landing produce greater pressure upon the pelvic floor than the Valsalva maneuver(4).
| Jumping and landing | Valsalva maneuver | |
|---|---|---|
| Number of IAP peaks | Two IAP Peaks | One IAP peak |
| Peak formation | Sudden but transient | Slow and steady |
| Direction of force on pelvic floor | Anterior and posterior | Infero-posterior |
Different physiology for athletes
Norwegian researchers compared the levator hiatus – the area of openings between the muscles in the bottom of the pelvis – of women newly pregnant with their first child who exercise regularly (more than three times per week) and those who didn’t(7). They expected to find that the exercisers had a more narrow levator hiatus and thus a more ‘fit’ and toned pelvic floor. On the contrary, the exercising group had a wider levator hiatus than non-exercisers.
This contradicts the misconception that those who exercise will automatically have better pelvic floor muscle control. This widening may also suggest why, when placed under stress, athletes may experience incontinence or organ prolapse. This study also found that in exercising subjects, the levator hiatus was stiffer. This stiffness may compensate for lack of strength during daily activities; however, during episodes of exercise when the pelvic floor endures IAP, symptoms of PFD may be more evident.
While athletes exercise regularly, many ignore including pelvic floor exercises in their routine. Studies show that 25-40% of women have poor awareness of how to exercise the pelvic floor muscles and contract them properly(1). However, training the pelvic floor muscles with exercise reduces the risk of urinary incontinence by 50% when performed prenatally and 35% when performed postnatally(6). It also results in a 4.6% reduction in cases of established pelvic organ prolapse(7). This suggests that regular muscle training also works as a PFD prevention measure.
Pelvic Floor Health
While an athlete may come to the clinic for a typical sports injury, including questions about urinary and bowel health in a routine history may reveal PFD. This may be an embarrassing topic for many athletes to discuss with their trainers, coaches, or peers. The first step is to reassure the athlete that while common, PFD isn’t normal and that there are effective treatment strategies. These exercise techniques are simple to integrate into a rehabilitation program. A comprehensive rehab program trains an athlete to properly engage their pelvic muscles during endurance or resistance activities in order to maintain pelvic health. Males can also suffer from PFD, so include them in your screening as well.
*How to perform a pelvic floor muscle contraction
Focusing on the pelvic floor muscles, from the back passage to the front passage, gently draw them inwards and upwards. Instruct athletes to imagine they are closing the anal and vaginal passages to prevent any bowel or urinary movements. If there were 10 different levels, imagine drawing the muscles upwards to level three. This ensures the contraction is effective but not overpowering. Over contracting can lead to discomfort and over recruitment of other muscles. Remind patients to never actually stop from going to the toilet. These instructions are used as a visual tool only.
There are two different ways to complete these contractions because the pelvic floor is made up of two different types of muscle fibers:
1. FAST contractions
This method works on the activation and efficiency of the pelvic floor muscles.
• Contract the muscles and then let go fully. Do not hold the contraction.
• Repeat for 10 consecutive repetitions.
2) SLOW contractions
This method builds muscle endurance and strength.
• Contract the muscles and hold this contraction for 10 seconds, then relax fully.
• Repeat for 10 consecutive repetitions.
• Once able to perform this 10 x 10 seconds, try to hold the contraction for longer and eventually build up to one minute.
Instruct athletes to complete both types of exercises three times per day. Ensure clients relax completely between each repetition. It can take 3-5 months for full benefits to accrue, so do not be put off if they do not notice changes initially.
*Pelvic floor endurance tests
You should be able to complete these tests with ease (and without discomfort) prior to undertaking any impact exercise, including running.
• 10 x fast contractions
• 12 x 6-8 seconds maximal contractions
• 1 x 60 seconds at 30-50% contraction
Pelvic floor and Core
As the pelvic floor contracts, the core muscles also contract as the two work in sync. If the pelvic floor is damaged, the erector spinae, obliques, and posterior pelvic floor muscles take over, and the transversus abdominis remains weak. This highlights the need to train both. Core training should first focus on retraining the sequence and timing of these muscle contractions. This creates neural networks automatically and efficiently. Once the mind can make these connections, athletes can commence further core strengthening.
*How to do this:
Lift the pelvic floor upwards from the back to the front passages, and then activate the core muscles in the lower stomach area by gently drawing them inwards from just below the hip bones at the front. Hold for 10 seconds, then release.
Assessment
These tests should be completed with the coordinated activation of the pelvic floor and core. If an athlete can achieve this without other compensations or fatigue, it suggests they are suitable to proceed with sports-specific drills.
1. Load and impact management tests (on each side)
• Walking 30 minutes
• Single-leg balance 10 seconds
• Single-leg squat x 10
• Jog on the spot for 1 minute
• Forward bounds x 10
• Hop on the spot x 10
2. Strength tests (aim for 20 on each side)
• Single-leg calf raise
• Single-leg bridge (see figure 2)
• Single-leg sit-to-stand
• Side-lying abduction (raise top leg up and down)

Modifying core exercises to reduce the load on the pelvic floor
- Avoid any sit-up exercises or where you raise your head up off the ground; these increase IAP and place pressure on the pelvic floor.
- Avoid full plank positions. Try doing these on the knees (see figure 3).
- Avoid holding plank positions for long durations as the muscles may not have sufficient endurance to hold the position comfortably. Instead, try the exercise shown below, and hold for a shorter duration but with a few repetitions.
- Avoid exercises that involve raising both legs up in the air at the same time, or lowering both legs from a raised position.

Monitoring pelvic floor training
When performing pelvic training, advise athletes to watch out for the following:
- Heaviness/dragging/discomfort in the vaginal region.
- Bulging/doming/straining/discomfort in the abdominal region.
- Leaking of any sorts.
- Bleeding not related to the menstrual cycle.
- Pelvic pain (pubic region, sides, or posteriorly) or lower back pain
Experiencing any of these symptoms is not normal and should be checked out by a women’s health professional before exercise is continued. This does not mean the athlete will have to stop training, but they should seek advice first.
Additional tips for pelvic health:
- Stay well hydrated to reduce constipation.
- Eat a high fiber diet to reduce constipation.
- Engage the core and pelvic floor before any strenuous activities, lifting, or exercise.
- Consider reducing your caffeine intake as caffeine can irritate the bladder.
- Decrease load in core exercises.
References
- Lee D.G. et al. 2014. J Assoc of Chartered Physiotherap in Women’s Health. 114; 10–24.
- Reviews in Urology. 2004. 6(Suppl3):S3.
- Physiotherapy 2015. 101:e58.
- Clin Biomech (Bristol, Avon). 2017 January ; 41: 20–27. doi:10.1016/j.clinbiomech.2016.11.003.
- Pool Goudzwaard A., et al. 2004. Clin Biomechanics. 19: 564-571.
- Lee D.G. et al. 2008. J Bodywork and Movement Ther. 12: 333-348.
- Br J Sports Med 2015;49:196–199. doi:10.1136/bjsports-2014-093548
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.







