Uncommon injuries: getting to the root of meniscal tears

Injuries to the meniscus are a common injury in athletes involved in sports that require loaded knee flexion with added axial compression and rotation. Many sports fit this profile; a few examples are the football codes, many of the combat sports, hockey, netball, basketball and tennis. These injuries range from very simple, small tears that can be managed non-surgically, to more serious larger tears that may fragment and displace, creating locking and catching sensations inside the knee - or large meniscus injuries in association with cruciate ligament injuries that usually require surgical intervention.
One form of meniscus injury that may have significant consequences to the natural biomechanics of the knee and early onset degeneration are meniscal root tears. The meniscal root insertions are an important factor in maintaining correct knee kinematics and for avoiding degenerative changes of the knee. Injuries to the meniscal roots can lead to meniscal extrusion, a decrease in the contact surface area of the knee, an increase in stress on the articular hyaline cartilage and ultimately articular degeneration with the consequence being osteoarthritis.
Anatomy and biomechanics
The semilunar-shaped medial and lateral fibrocartilage menisci have a concave superior surface that contours to the shape of the large convex femoral condyles(1-3), and a flat inferior tibial surface that articulates with the flat tibial plateau. The menisci are divided into three distinct segments(2-4):- Anterior horn/root with simple planar insertions into the tibial plateau;
- Body;
- Posterior horn/root with complex three-dimensional insertions into the tibial plateau.
The roots act as ‘anchors’ for the meniscus onto the tibia. Via the ‘roots’, the meniscus are designed to convert axial compressive loads into ‘hoop stresses’ during both knee extension and deep flexion. This is facilitated by the interlacing network of collagen fibres, proteogylcans and glycoproteins that make up the macroscopic structure of the fibrocartilage of the menisci(5).
The menisci transmit loads from the femur to the tibia through the stretching of circumferential collagen bundles in a radial direction. This creates an ‘extrusion’ effect on the meniscus towards the outside of the joint(3,4,6). The distribution of hoop stresses by the circumferential fibres helps to transmit relatively even axial loads across the joint surfaces, which prevents excessive loading and articular cartilage breakdown. This is shown in figure 1.
Figure 1: ‘Hoop stress’ distribution of forces on the meniscus
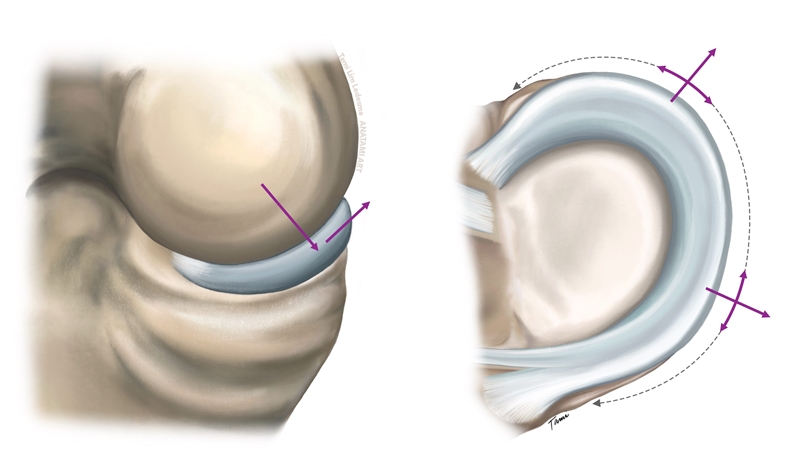
It is believed that the most important function for the prevention of arthritis in the knee is the maintenance of this ‘hoop tension’ in the meniscus, which allows correct intraarticular load transmission across the knee joint. The medial meniscus transmits approximately 90% load on the medial side and the lateral meniscus is approximately 70%(7,8). Therefore, the menisci will spare the cartilage from bearing 100% of the bodyweight. Furthermore, the menisci also have a role in proprioception of the knee because they act as secondary stabilisers, and they also contribute to synovial fluid production and thus knee joint lubrication.
It is beyond the scope of this paper to discuss the exact anatomy of the meniscal roots other than to highlight that they attach the meniscus firmly onto the tibia. The posterior roots of the meniscus are more comprehensive and three-dimensional and have quite advanced and intricate attachments compared to the anterior roots. With regards to injury prevalence, the posterior roots are more prone to injury, particularly the medial meniscus posterior root.
Although the anterior root insertions are not as three dimensional as the posterior roots, the medial meniscus anterior root attachment has been reported to have the largest insertion site of any of the meniscus root attachments(3,9). The medial meniscus anterior root has a close relationship to the anterior cruciate ligament (ACL) attachment into the tibia(3), and four types of insertions have been described for the anterior root of the medial meniscus(10).
Finally, the anterior horn has been described as having a connection to the anterior intermeniscal ligament, also known as the transverse ligament, in approximately 70% of knees(9-11). In 46% of cases, the anterior intermeniscal ligament traversed from the anterior horn of the medial meniscus to the anterior horn of the lateral meniscus, and from the anterior horn of the medial meniscus to the lateral aspect of the joint capsule anterior to the lateral meniscus in 26% of knees(11). The role of the intermeniscal ligaments remains controversial(12). Figure 2 provides an overview of the anatomy of the meniscus and the meniscal roots.
Figure 2: Anatomy of the meniscus and the meniscal roots
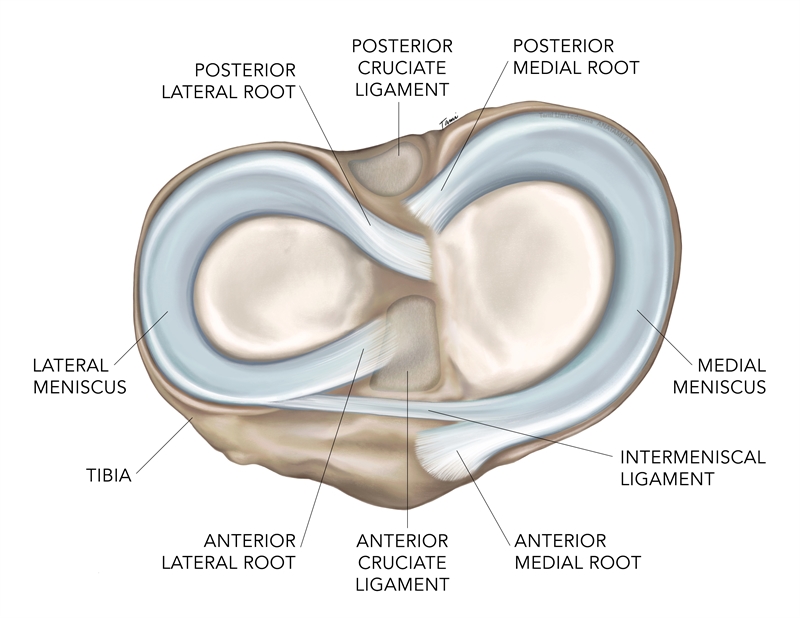
Pathogenesis of meniscal root tears
Meniscal root injuries were first described in 1991 by Pagnani et al(13), and a plethora of research has been conducted on meniscal root injuries (particularly medial meniscus posterior horn root injuries) in the last three decades. It is now accepted that an injury to the meniscal attachment, especially on the medial side, can lead to meniscal extrusion and an impairment in ‘hoop stress’ dissipation, and this in turn leads to stress being applied to the articular cartilage due to the decrease in contact surface area and accelerated articular degeneration(14,15).As with other meniscal tears, meniscal root injuries may occur in both the acute and chronic settings. The posterior root attachments are the most commonly injured areas, with the medial meniscus posterior root being the most vulnerable to injury. Acute tears occur in situations of acute knee ligament injuries such as ACL and PCL injuries, or may occur due to trauma from high compressive and shear forces that would be encountered in deep squatting or hyperflexion(5,13,16). Lateral meniscus posterior root tears are not as common as medial meniscus posterior root tears, and if they do occur, they tend to only occur in the sports setting in athletes.
The lateral meniscus is twice as mobile as the medial meniscus therefore the lateral meniscus has less of a role with stabilisation of the knee, and consequently will encounter less stress, than the medial meniscus(17, 18). Therefore, the lateral posterior horn has been reported to be less affected by chronic ACL instability episodes than the medial posterior horn(17). Researchers have reported that sports activity is involved in approximately 87% of lateral meniscal injuries, and 70% occurring with ‘pivot-contact’ sports such as football, soccer and combat sports(17).
Medial meniscal posterior root tears present in about 10% to 21% of arthroscopic meniscal repairs or meniscectomies(19,20). MRI imaging may miss up to one third of these injuries; therefore the actual prevalence may be even higher(19,20). Furthermore, posterior root tears of the medial meniscus have been reported to have an incidence of about 3%, along with multiligamentous tears(13,16).
It is interesting in that chronic medial meniscus posterior root tears are quite common in Asian countries in older individuals, where a floor-based lifestyle is habitual and traditional(19). In a hyper-flexed knee position that one would assume with a floor-based lifestyle, excessive pressure can be placed on the meniscus, especially the posterior horn medial meniscus root(19). In these populations, the proportion of medial meniscus posterior root tears may be as high as 20−30% of all medial meniscus tears(19,21). It occurs mostly in the older population, and the onset usually occurs after the age of 50(22).
Mechanisms of injury
In deep squats from 90 degrees onwards, the posterior horns of the medial and lateral menisci transmit more load than the anterior horns(1,23). As mentioned above, the posterior root of the medial meniscus has the least mobility of all the meniscus roots, and studies have reported that the stress placed upon the posterior medial root results in a higher incidence of tears compared with the other roots(4,18,20).Significant injuries to the meniscus medial posterior root attachments - such as root avulsions and full-length degenerative tears and radial tears adjacent to the root - have been linked to clinically significant medial meniscal extrusion. Meniscal extrusion exists when the meniscus is displaced relative to the margin of the tibial plateau(14). In the event of a meniscal extrusion, the transmission of ‘hoop stress’ is significantly impaired, leading to accelerated degenerative articular damage(14,15).
Research has established that a significant tear of the medial meniscus posterior root has a similar unfavourable outcome on peak tibiofemoral contact pressures (a 25% increase) as a total medial meniscectomy(24,25). It has also been demonstrated that medial meniscal posterior root injury results in increased tibial external rotation and lateral translation(24). Such changes may ultimately increase the varus limb alignment commonly reported in patients with these injuries(5). It is therefore imperative to accurately identify such meniscal root lesions to guide treatment, surgical decision making, and prognosis.
Diagnosis
Signs and SymptomsMeniscal root tears are usually very difficult to differentiate from other simpler meniscal injuries. Some of the features found in the clinical presentation may include:
- Joint line pain usually on the affected side.
- A popping sound in the event of trivial injury is common for medial meniscus posterior root tears(22).
- The sensations of locking and giving way may not be all that common with posterior root tears(26).
- Often, the precipitating incident may be quite benign. In around 70% of meniscal root tears, the mechanism of injury is only minor trauma, such as deep squatting(27).
- The most common physical sign is posterior knee pain with deep flexion and joint line tenderness(26).
- Studies show that McMurray testing is positive in only 57% of patients, and effusion present in only 14.3% of patients(26).
- The varus stress test in full extension with a relaxed knee may reproduce the meniscal extrusion that may be palpated along the anteromedial joint line. This test has been described for medial meniscal posterior root avulsion. Extrusion disappears when the knee is returned to normal alignment(28).
Imaging
Without robust physical signs and symptoms that can be used to guide clinical decision making, MRI has become increasingly used to diagnose meniscal root tears. Many authors describe varying sensitivity and specificity with MRI(20,29,30). With regards to the more common medial meniscus posterior root tears, it has been proposed that these are not difficult to diagnose if the diagnosis is based on three different discriminatory features on MRI-plane images along with clinical symptoms(31). These MRI signs include:
- The ‘ghost sign’ from the sagittal plane (detection rate of 100%), which is the absence of an identifiable meniscus in the sagittal plane, or high signal replacing the normal dark meniscal signal(5,14,31).
- A vertical linear defect (signs of truncation) on the coronal plane (100%).
- A radial linear defect on the axial plane (94%).
Furthermore, some other useful reference points for reading MRI’s include:
- T2-weighted sequences are generally considered to be the best images for visualisation of tears given their maximum specificity and sensitivity values(31), although, some consider axial images to provide the highest sensitivity and specificity(29).
- Given the difficulty of visualising a frank tear (because of the relatively small size of each meniscus root), the presence of meniscal extrusion has been described as a finding that highly correlates with the presence of a root tear(32).
- Medial meniscal extrusion is defined as partial or total displacement of the meniscus from the tibial articular cartilage(14,33).
- Studies have reported that greater than 3mm extrusion on midcoronal imaging is significantly associated with articular cartilage degeneration, severe meniscal degeneration, complex tear patterns, and tears involving the meniscus root(14).
Classification of injury
La Prade reviewed 71 cases of root tears and classified the tears into one of five types(34). He found that type-2 tears were the most common type of root tear found in their case study (67.6%). Table 1 describes the La Prade classification of meniscal root tears. See also figure 3, which visualises a complete radial root tear and an avulsion fracture of the root.
Table 1: Classification of meniscal root tears
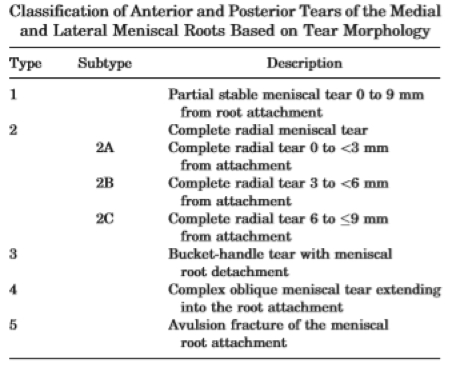

Figure 3: Visualizations of root tears
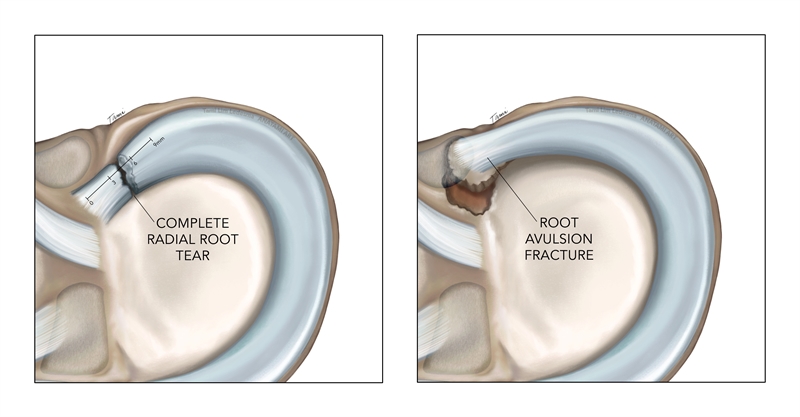
Conclusion
Meniscal root injuries can be considered as a catastrophic injury to the meniscus in the athlete, as damage to the root will significantly alter the ability of the meniscus to absorb and distribute load due to loss the ‘hoop stress’ mechanism. The meniscal root may be injured in athletes in the usual pivot shift mechanism (that also damages the cruciate ligaments), or damaged in full squat and knee flexion positions when under load. The posterior roots are the more commonly injured roots with the medial meniscal posterior root being by far the most common. These are difficult injuries to diagnose on clinical examination; therefore specific MRI features are usually needed to diagnose the injury prior to a knee arthroscopic investigation. Part two of this article will describe in detail the management plan for meniscal root tear injuries.References
- Sports Health. 2012;4(4):340-351
- Radiol Clin North Am. 2007;45(6):1033-1053, vii
- 1995;11(4):386-39
- Australas Radiol. 2006;50(4):306-313
- Br Med Bull. 2013;106:91-115
- Am J Sports Med. 2002;30(2):189-192
- Sports Med Arthrosc Rehabil Ther Technol. 2010;2:1
- J Bone Joint Surg Br. 1999;81:37-41
- 1995;11(1):96-103
- Am J Sports Med. 1998;26(4):540543
- Am J Sports Med. 2000;28(1):74-76
- 2012;19(2):135-139
- 1991;7(3):297-300
- Skeletal Radiol. 2004;33(10):569-574
- 2011;18(3):189-192
- 2009;25(9):1025-1032
- Orthop Traumatol Surg Res. 2009;95(8) (suppl 1):S65-S69
- Am J Sports Med. 1991;19(3):210-215; discussion 215-216
- 2004;20(4):373-378
- Knee Surg Sports Traumatol Arthrosc. 2008;16(9):849-854
- J Korean Knee Soc. 2005;17:160-4
- Arch Orthop Trauma Surg. 2004;124:642-5
- Clin Orthop Relat Res. 1975;109:184-192
- J Bone Joint Surg Am. 2008;90(9):1922-1931
- Am J Sports Med. 2009;37(1):124-129
- 2009;25(9):951-958
- 2011;27:346-54
- Knee Surg Sports Traumatol Arthrosc. 2011;19(12):2072-2075
- Knee Surg Sports Traumatol Arthrosc. 2012;20(10):2098-2103
- AJR Am J Roentgenol. 2005;185(6):1429-1434
- J Comput Assist Tomogr. 2008;32:452-7
- J Magn Reson Imaging. 2008;28(2):466-470
- Knee Surg Sports Traumatol Arthrosc. 2011;19(2):222-229
- AJSM Pre View, published on December 1, 2014 as doi:10.1177/0363546514559684
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









