Uncommon Injuries: Sural Nerve Neuropathy
In our continuing ’uncommon injury’ series, Chris Mallac looks at the sural nerve, and explains mechanism of injury, implications for musculoskeletal dysfunction in the athlete, and treatment options for the clinician.
The sural nerve, a sensory nerve, courses down the postural-lateral aspect of the calf. Its primary role is to innervate the skin over the distal one third of the lateral shin and outside of the foot towards the fifth toe. This nerve can be injured in athletes in a number of different ways, and although not debilitating, a sural nerve injury may present as long term neuropathic pain, which may hinder athletic performance. Although it performs primarily a sensory function, the nerve is of particular interest as it is widely used in electrophysiological studies and is a frequent donor nerve used for peripheral nerve grafting(1).
Anatomy and function
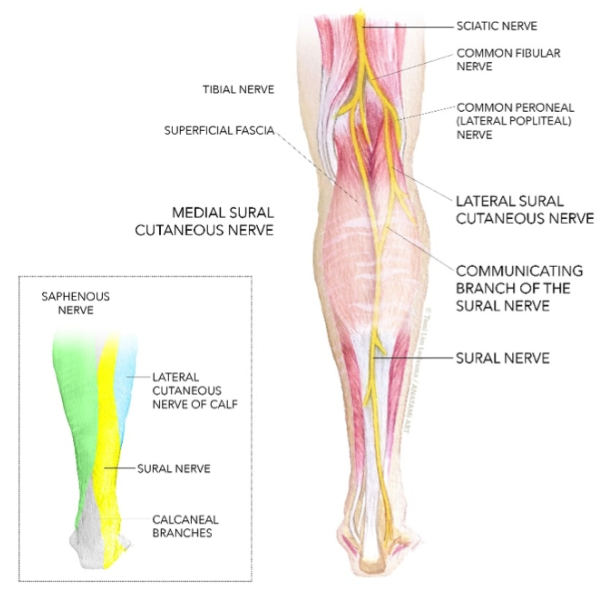
The sural nerve has a reasonably complex anatomical arrangement and in the literature many variations of the nerve exist. In simple terms, there are two sural nerves – the medial sural cutaneous nerve and lateral sural cutaneous nerve – and these eventually join via the peroneal communicating nerve to make the sural nerve (see Figure 1)(2-9). However, some other authors describe that the sural nerve is formed by the union of medial sural cutaneous nerve directly with the lateral sural cutaneous nerve (not the peroneal communicating nerve)(10-12). Due to this confusion, the term ‘sural nerve complex’ was used to accommodate these anatomical differences controversies(1).
Irrespective of which nerve joins the medial sural nerve, the terminal length of the nerve then continues to form the sural nerve that runs distally and laterally alongside the Achilles tendon. It then curves inferior to the lateral malleolus and passes along the lateral border of the foot, splitting into medial and lateral branches near the base of the fifth metatarsal(9, 13). The sural nerve is a sensory nerve of the lower limb that supplies the lower posterolateral part of the leg and lateral part of the dorsum of the foot. It is generally described as a sensory nerve but may contain motor fibres (discussed later in this article)(14-16).
Medial vs. lateral
Medial
The medial sural cutaneous nerve originates from the tibial nerve in the popliteal fossa, 3 - 5cm distal to the knee joint, and descends between the two heads of gastrocnemius muscle. This is deep to the fascia covering the muscle. It pierces the deep crural fascia of the leg to become superficial in the bottom third of the leg, at the junction of middle and distal thirds of the leg(1, 17).
As mentioned earlier, the medial sural cutaneous nerve joins the lateral sural cutaneous nerve via the peroneal communicating nerve to form the distal sural nerve. The peroneal communicating nerve originates in the popliteal fossa either from the lateral sural cutaneous nerve or directly from the common peroneal nerve(10).
The most common convergence of the sural nerve is when both the medial and lateral sural nerves join (40.2% - 83.7%)(18). Less commonly, the distal sural nerve may have contribution from only the medial sural nerve (13.3% - 53.8%), and from only the lateral sural nerve in rare cases (0 - 16%)(18). Kim et al (2006) studied the relative contributions of medial sural cutaneous nerve and peroneal communicating nerve to sural nerve by conduction study and showed that the main contributor to sural nerve was found to be the medial sural cutaneous nerve(4). It would appear therefore that the more important component of the eventual sural nerve is the medial sural cutaneous nerve, which courses through the two heads of the gastrocnemius. When there is no communication between the medial sural cutaneous nerve and peroneal communicating nerve, the medial sural cutaneous nerve itself continues as the sural nerve and supplies the lateral surface of the leg – giving off lateral branch to the heel, continuing as the lateral dorsal cutaneous nerve(3, 7).
The medial sural cutaneous nerve – some lesser known facts:
- Rather than coursing between the two heads of the gastrocnemius, it may become deeply embedded on the dorsal surface of the medial or lateral gastrocnemius muscle. If the nerve passes through the muscle, it may send branches to the gastrocnemius muscle. This abnormal course of the nerve may account for calf pain on contraction of gastrocnemius muscle if nerve entrapment is involved(8, 9, 19).
- Hwang et al (2003) found in a dissection study that the medial sural cutaneous nerve came off the nerve into the medial gastrocnemius muscle (30%) and diverged 5.5 mm from the tibial nerve tibial nerve. This was found in 30% of subjects(20).
- Sekiya et al (2006) looked at the communication between the sural nerve and tibial nerve and found that the sural nerve may contain some motor fibres(16). This was supported by extensive work on sural nerve using electrodes, where motor fibres in the sural nerve were found(14).
- Cases of anomalous innervation of abductor digiti quinti muscle of the foot via sural nerve have been documented(15). These have showed compound muscle action on the stimulation of sural nerve and medial sural cutaneous nerve, but not on stimulation of peroneal nerve - again suggesting that the sural nerve may have a slight motor function.
- The length of the nerves in the ‘sural nerve complex’ have also been variably reported. In one study, the length of the medial sural cutaneous nerve was 21 - 33cms, peroneal communicating nerve 20 - 38cms, lateral sural cutaneous nerve 5 - 13cms, and sural nerve 11 - 20cms(1). In another, the medial sural cutaneous nerve length was 17 - 31cms and lateral sural cutaneous nerve 15 - 32cms(11). In the most variable study, medial sural cutaneous nerve lengths ranged from 6 - 43cms, peroneal communicating nerves from 2.5 - 39cms, lateral sural cutaneous nerves from 8.5 - 40cms, and sural nerves from 3.5 - 39.5cms(19).
Lateral
The lateral sural cutaneous nerve originates from common peroneal nerve in the popliteal fossa. It descends downwards between deep the fascia and lateral head of gastrocnemius muscle. At the middle of the calf it pierces the deep fascia to become subcutaneous. It joins the medial sural cutaneous nerve via the peroneal communicating nerve (discussed above). It is rare for the lateral sural cutaneous nerve to continue as the sural nerve in isolation(18).
Distal sural nerve
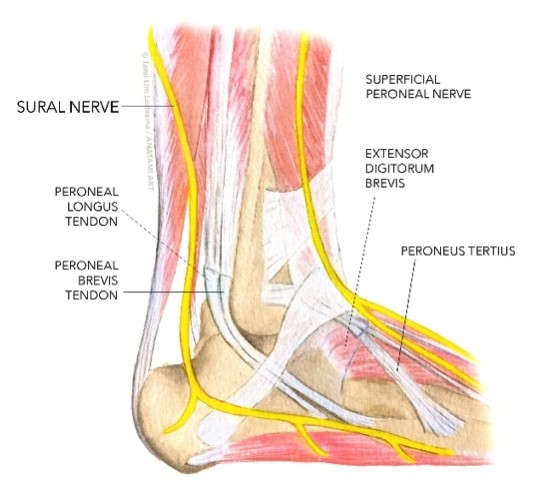
Due to the intimate relationship the sural nerve has with the Achilles tendon and the ankle joint, the distal sural nerve may be injured in lateral ankle sprains and damaged during surgical procedures of the Achilles tendon/lateral ankle. For this reason, its anatomy has been extensively studied (see Figure 2)(21).
The sural nerve crosses across the Achilles tendon from proximal-medial to distal-lateral. There exists a ‘hot zone’ around the lateral border of the Achilles tendon approximately 9 - 12 cm proximal to the tuber calcanei, where the nerve crosses over the posterolateral Achilles tendon and the two are closely related. For the surgeon, this is where care needs to be taken during Achilles tendon surgery. Within this area, no sutures should be applied without direct visualisation of the sural nerve to prevent sural nerve entrapment(21).
Interestingly, the relationship between the Achilles tendon and the sural nerve is not as intimate in taller individuals, where the distance between the Achilles tendon and the sural nerve increases with height. Furthermore, the sural nerve passes significantly closer to the Achilles tendon in older individuals(22).
As the nerve proceeds distal and lateral to the Achilles tendon, it passes posterior to the lateral malleolus with the peroneal tendons, and along the dorsolateral aspect of the foot (Figure 2). The anatomical course of the sural nerve corresponds to its cutaneous innervation, which includes the lateral lower third of the lower extremity, the lateral heel, and the dorsolateral aspect of the foot up to the base of the fifth toe(17).
Mechanism of injury
Injury to the sural nerve is uncommon, and it is not often reported as a cause of exercise-related leg pain. A few possible aetiologies of sural nerve injuries exist(23-37). These include:
- Compression of the nerve
- Crural fascia
- Mass lesions such as a Bakers Cyst or myositis ossificans at the level of gastrocnemius aponeurosis
- Scar tissue:
- Beneath the deep fascia of the gastrocnemius
- Peroneal nerve sheath degeneration
- Achilles Paratendinitis
- Ganglions and lipomas
- Extrinsic causes such as ski boots, heel straps, casts and tightly laced boots.Direct trauma due to fibular fracture, fracture of the fifth metatarsal, gastrocnemius muscle injury, achilles tendon rupture or surgically induced damage.
- Inversion ankle sprains that stretch the nerve.
- Adverse neurodynamics due to a tethering of the nerve in the crural fascia (fixation point). This would be more common in running and track and field.
It has been proposed that the nerve may be entrapped by the deep fascia of the calf, and this idea has the most relevance for the athlete(10, 13). During knee extension, the fascia could exert a compressive force on the medial sural nerve.
The muscular course of the sural nerve could account for the calf pains experienced during contraction of the gastrocnemius. At the emergence point of the nerve through the crural fascia, a fibrous arch is formed at the fascial opening through which the sural nerve passes. This is a potential entrapment site.
The superficial sural aponeurosis may be thickened and doubled, forming a fibrous tunnel that may compress the nerve(35, 38). The tension is worsened during passive forcible plantarflexion, and inversion of the foot increases tension in the sural nerve as the nerve is tightly adherent to the surrounding fascia. This action may flatten the nerve within the fibrous tunnel and pose a potential entrapment site of the sural nerve(38).
The other mechanism of injury that is highly relevant for the athlete is the potential for sural nerve damage following lateral ankle sprains, particularly those that involve severe adduction of the calcaneus and/or inversion of the ankle. As the nerve passes around the postural-lateral corner of the ankle, it may be injured during this mechanism. This may potentially lead to long term secondary neuropathic pain following ankle sprains(39).
Clinical diagnosis
As with most sports related musculoskeletal conditions, the diagnosis of sural neuropathy is largely based on clinical examination. It needs to be differentiated from other possible conditions such as sacral (S1) sciatica, exertional compartment syndrome of the lower limb, piriformis syndrome, popliteal artery entrapment and Achilles tendinopathy, all of which can present similar symptoms(35, 41).
The typical signs and symptoms include:
- Pain and sensory alterations over the distribution area of the nerve(40). This would include the postero-lateral side of the distal third of the leg, as well as the lateral aspect of the foot and fifth toe.
- Typical subjective sensory reports such as burning pain, hypaesthesia, dysaesthesia or paraesthesia over the foot or upper calf(35).
- Tenderness may be observed over the nerve course, while pressure over the point of maximum tenderness can reproduce the symptoms(41).
- A positive Hoffman-Tinel’s sign may affirm the diagnosis, although neurological examination could be normal.
- Possibly, there is a positive nerve mobility test indicating adverse neurodynamics of the sural nerve (see below)(39).
It is questionable whether imaging techniques can assist in establishing the diagnosis(35). Doppler studies, ultrasonography, computed tomography or magnetic resonance imaging scanning may assist in visualisation of the entrapment site. Using electrodiagnostic testing, an increase in distal latency and decrease in amplitude of the sensory action potential of the sural nerve could indicate long-term sural nerve entrapment neuropathy(9, 35, 42). Furthermore, local anaesthetic injections into the area of tenderness can lead to temporary resolution of the symptoms, representing an additional diagnostic tool(35).
Sural nerve neurodynamic test
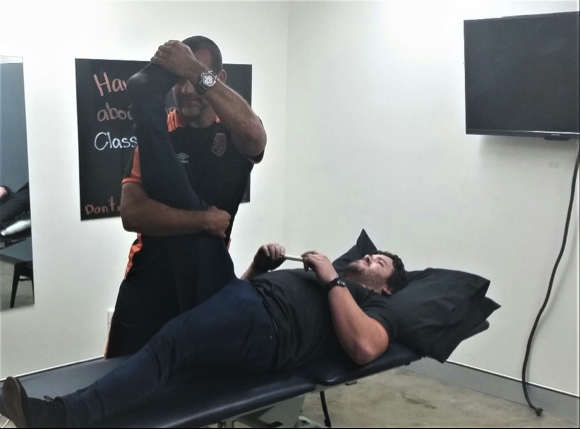
This test (see Figure 3) is described in detail by Michael Shacklock(39). It is performed if the patient describes symptoms in the lateral calf and foot, which may stem from mechanical dysfunction and mechanosensitivity of the sural nerve. This may arise from a sprained ankle, S1 nerve root irritation, cuboid syndrome and peroneal tendinitis.
To perform this test, the patient’s leg is grasped by the therapist’s hands so that the leg is supported and the foot is held in dorsiflexion and inversion. The leg is then passively raised into hip flexion. This is usually felt in the posterolateral calf and/or posterolateral ankle. This test would be positive if it satisfies three criteria:
- It must reproduce the pain or sensation they are complaining about in the same area.
- It needs to feel different to the uninvolved side.
- It will be made worse by adding a ‘sensitiser’ movement such as hip adduction, hip internal rotation or cervical flexion.
Management
Treatment of sural nerve neuropathy can be conservative or surgical depending on the exact cause.
Non-operative treatment
A non-operative approach may be more relevant in conditions where the nerve irritation is the result of tethering of the nerve by interfaces, or if the nerve has been subject to traction such as post ankle sprain. To successfully treat the mechanical nerve dysfunctions and adverse neurodynamics, the sural nerve test described above may be used to ‘move’ the nerve through its interfaces. Typical ‘slider’ techniques would be to use the same test and then to use repeat ankle plantarflexion/dorsiflexion to move the nerve, or knee flexion/extension to move the nerve. This is described in detail by Michael Shacklock(39).
Surgical
This is required when the removal of space-occupying masses is necessary, while in fascia-related cases of compression, neurolysis is the most effective technique(26). As the nerve is reasonably superficial and easy to access, sural nerve decompression can be accomplished under local anaesthesia, by a longitudinal section of the fascial tunnel, which releases the nerve from the surrounding fibrous tissue. In the area around the heads of the gastrocnemius, this may involve a long proximal dissection between the two muscle bellies.
Conclusion
Sural nerve neuropathy is a reasonably uncommon complaint in the athlete. It may manifest following ankle sprain or due to a tethering of the nerve through the crural fascia and gastrocnemius muscle, and this may be noticed upon forced plantarflexion movements. In other sports that use tight fitting boots and bindings such as skiing and snowboarding, the nerve may be compressed. Furthermore, space occupying lesions such as ganglions, lipomas, scar tissue and myositis ossificans may potentially compress the nerve.
The clinical description is usually straightforward with the athlete complaining of pain and/or neurological symptoms along the lateral calf and/or lateral foot to the little toe. It can easily be managed with nerve ‘sliders’ to improve the neurodynamics or it can be surgically released in the event of a space occupying compression.
References
- Journal of Hand Surgery, 1987. 12(6). 1119–1123
- Clinical Anatomy, 2011. 24(2). 237–245
- The Anatomical Record, 1954. 120(3), 533–543,1954
- Yonsei Medical Journal, 2006. 47(3), 415–422
- Foot Ankle Int. 2000; 21:475-477
- Foot Ankle Int. 2005; 26:560-567
- Surg Radiol Anat 2001;23:307–12
- Bergman RA, Thompson SA, Afifi AK, Saadeh FA (1988) Compendium of Human Anatomic Variation: Catalog, Atlas and World Literature. Urban & Schwarzenberg: Baltimore & Munich
- Archives of Physical Medicine and Rehabilitation, 1999. 80(5).604– 606
- Plastic and Reconstructive Surgery, 1994. 94(6), 850–855
- Clinical Anatomy, 2002. 15(4).263–266
- American Journal of Physical Medicine and Rehabilitation, 2008. 87(6). 438–442
- Pecina M, Krmpotic-Nemanic J, Markiewitz A. Tunnel syndromes: peripheral nerve compression syndromes. 3rd ed. Boca Raton (FL): CRC Press, 2001
- Neurology, 1997. 49(6). 1725–1728
- Electromyography and Clinical Neurophysiology, 1995. 35(1), 61–63
- Anatomical Science International, 2006. 81(2), 84–91
- Am J Phys Med Rehabil. 2001; 80: 543-546
- Sarrafian SK. Anatomy of the foot and ankle: descriptive, topographic, functional. 2nd ed. Philadelphia (PA): Lippincott: 1993
- Seema (2013) Study of Sural Nerve Complex in Human Cadaver. ISRN Anatomy. Volume2013, Article ID827276. 7 pages
- Annals of Plastic Surgery, 2003. 50(5), 517–522
- Br J Sports Med, 2007;41:456–458
- 2014. 37(3); e298-e301
- Clin Sports Med 1990:9:489-509
- J Musculoskel Med 1988; 5: 678-95
- Orthop Clin North Am 1994; 25: 47-5
- J Bone Joint Surg Br 1974;56B: 465-8
- Acta Orthop. 1989.55, 491-497
- J. Phys. Med. Rehabil. 2002. 81, 876-880
- Neurosurgery, 1992. 30(6) 927–930
- 1978. 239; 135
- Acta Neurochir. (Wien), 2000. 142, 951-952
- Am J Sports Med 2006; 34:793–8
- Foot Surg 1990; 29:119-21
- J Musculoskel Med. 2008; 25:126-128
- Am J Sports Med 2000; 28:679-82
- Foot Ankle 1981; 2:153-5
- Muscle Nerve 1980; 3:248-9
- Anat Cell Biol, 2014;47:144-147
- Shacklock (2005) Clinical Neurodynamics. Elsevier. Sydney
- Sunderland S. Nerves and nerve’ injuries. New York (NY): Churchill Livingstone; 1978
- Orthop Trauma, 2009;23:404-11
- Ital J Neurol Sci, 1994;15:119-20
Further reading
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.