You are viewing 1 of your 1 free articles
Slipping rib syndrome: an obscure cause of thoracic pain?

Thoracic movement
A number of rigid structures, including the ribs, sternum, and thoracic vertebrae, comprise the thoracic region. Intervertebral discs and costal cartilages facilitate the joint movement between these structures. This movement includes(2):- Flexion-extension – ranging from 4o at T1 to 12o degrees at T12.
- Lateral movement – this typically allows 6-7o per vertebral segment.
- Rotation – ranging from 9o at T1 to 2o at T12.
Although each individual joint motion is small, the combined movement at the costovertebral joints allows for respiration and spinal mobility, while at the same time facilitates load bearing and stabilization(3).
The rib-vertebrae interaction
Correct thoracic function depends on the rib-vertebra-sternum interface; it needs to be rigid enough for load bearing and stabilization, but mobile enough to allow necessary movement. Critical to this function are the costovertebral joints and their associated ligaments (see figure 1). These joints and ligaments are poorly understood and frequently overlooked, despite their abundance in the human thoracic spine (there are 108)(4). The costovertebral ligaments are dense, fibrous ligaments, containing a large amount of elastic fibres. These fibres are able to stretch with movement in one direction yet shorten with movement in the opposite direction; this means that when subject to repeated movements, they remain taut rather than becoming lax(5).Figure 1: Costovertebral joint and ligament structures*
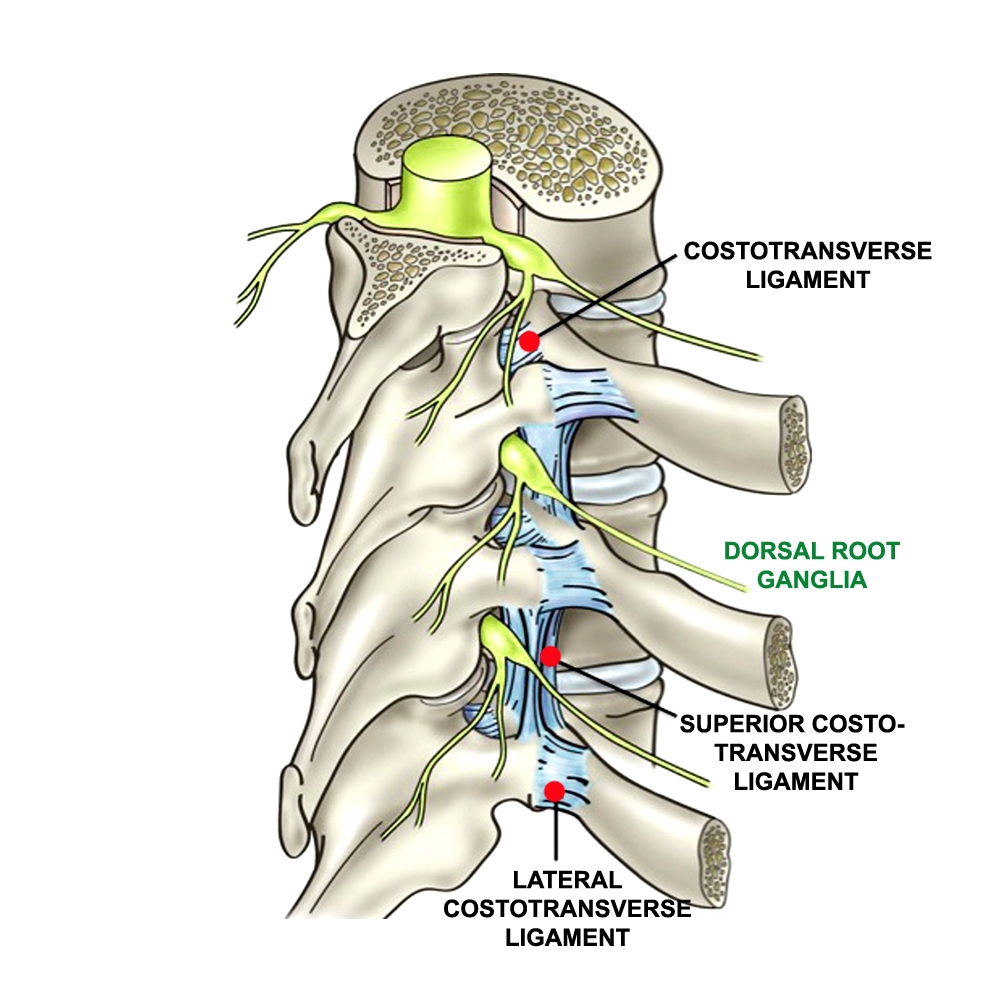
*Cureus. 2016 Nov; 8(11): e874 (image by David Fisher)
Costovertebral strain
Costovertebral strain occurs when the compression and torsion forces applied to the costovertebral joint are greater than it can withstand. This can result in damage to the costovertebral ligaments, cartilage or both. In extreme cases, the head of the rib may sublux, dislocate, or fracture.When a costovertebral strain injury occurs, an athlete typically experiences an intermittent sharp stabbing pain, along with a dull achy sensation, which may last for days, weeks or in severe case, even months(6,7). This pain is usually (though not always) unilateral, and exacerbated by movement of the spine, especially twisting and ipsilateral side bending. Deep breaths, coughing and sneezing typically also elicits pain in the posterior thorax, but can also radiate to the scapular region or anterior chest wall. There may also be palpable pain at the costotransverse joint and rib angle(8,9). In more severe cases, even simple activities such as rising from a chair, stretching, and turning over in bed can result in severe discomfort(10).
Costovertebral strain diagnosis
For clinicians dealing with an athlete presenting with posterior thoracic pain, correctly determining the aetiology of the condition can be difficult. This is partly due to the neural complexity of the thoracic spine, and the number of other conditions that can present with similar symptoms. These include (in no particular order)(4):- Rib/vertebra fracture
- Intervertebral disc protrusion/herniation
- Spinal stenosis
- Paraspinal muscle or ligament strain
- Upper thoracic syndrome (T4 syndrome)
- Ankylosing spondylitis
- Osteoarthritis
- Zygapophyseal joint dysfunction
- Pain resulting from other (potentially serious) conditions, including pain of cardiac, aortic, renal, pulmonary, oesophageal or gallbladder origin, and pain from metastatic malignant lesions.
In athletes where there is no history of impact/trauma or loading prior to the onset of thoracic pain, further investigations may be warranted. This is particularly true for older athletes (over the age of 40) where pain could arise from a number of disease conditions (as indicated above)(4). These investigations may include X-ray imaging, MRI and/or CT scans, ultrasound imaging and spirography. In addition to imaging, the savvy clinician will be able to help rule conditions in or out by a process of differential diagnosis using mobility/pain tests, the patient’s history and the presence or absence of other symptoms. Due to space constraints, it is beyond the scope of this article to provide detailed differential diagnosis criteria for posterior thoracic pain; however, readers are directed to this case study paper by Fruth, which can be downloaded in full, and which serves as an excellent starting point.
Mysterious pain onset: slipping rib?
In many cases of posterior thoracic pain, a clear onset trigger – for example an unusual loading or impact event, or participation in a new mode of training - is identifiable. However, this is not universally the case, even when further testing shows no other condition/disease is present. When other injuries or conditions have been ruled out, clinicians may feel they have drawn a complete blank. However, there exists another possible cause, which although uncommon, is frequently misdiagnosed or underdiagnosed – ‘slipping rib syndrome’.Slipping rib syndrome (SRS) is a condition that can arise from the hypermobility of the anterior ends of the false rib costal cartilages (see figure 2). Also referred to by a number of other terms such as ‘clicking rib’, ‘interchondral subluxation’, ‘painful rib syndrome’, and ‘traumatic intercostals neuritis’, undiagnosed slipping rib syndrome can subsequently lead to months or even years of unresolved thoracic pain(11). This syndrome was first described in 1919, but while the literature contains a number of reported cases, it is rarely mentioned in medical textbooks(12).
The primary cause of SRS is rib hypermobility, which is caused by the relative weakness of the sternocostal, costochondral, and/or costovertebral/costotransverse ligaments. In particular, the false ribs (ribs 8, 9 and 10) are most susceptible to hypermobility. This is because these ribs do not form a rigid continuum spanning the thoracic vertebrae and the sternum; instead of attaching to the sternum at the anterior end, they are connected to each other via a cartilaginous/fibrous band (see figure 2).
Figure 2: Rib structure and false rib costal cartilages
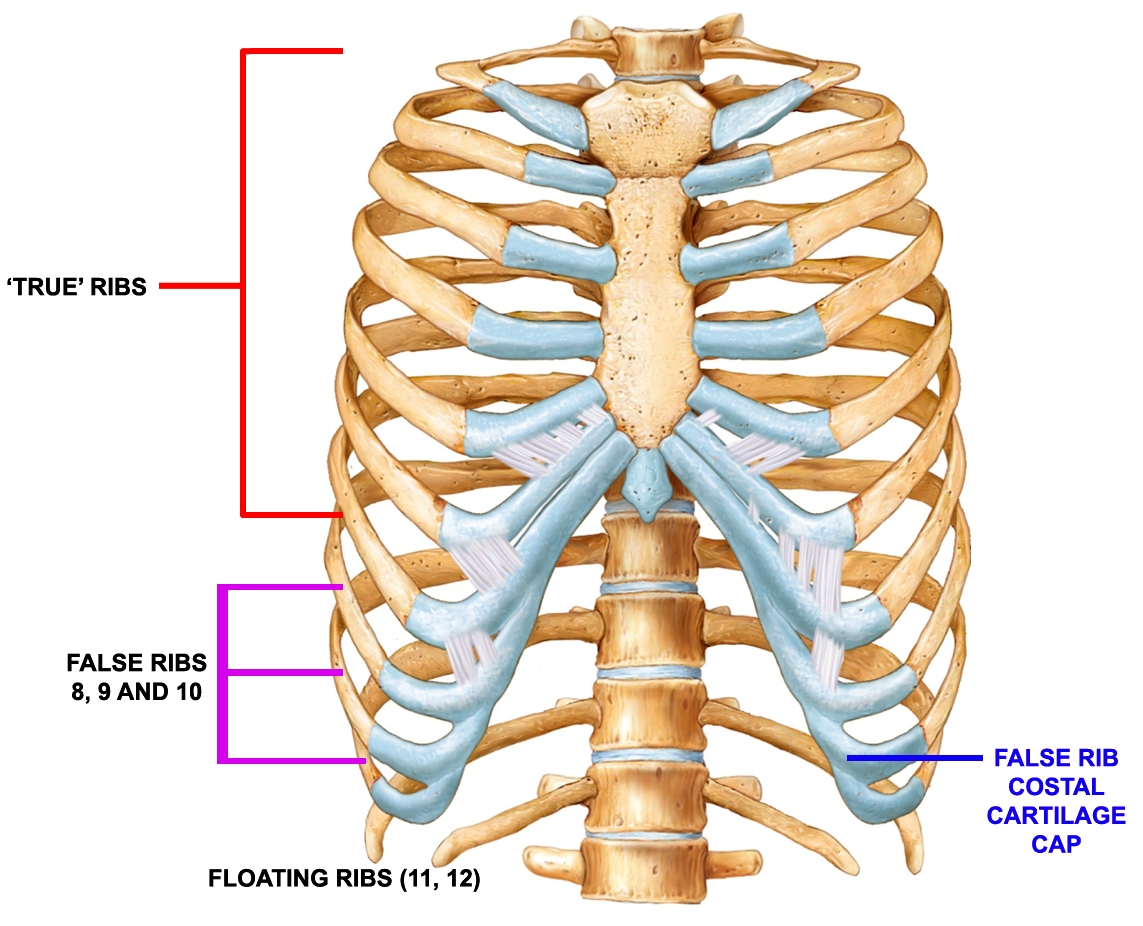
Surgical studies have shown that this hyper mobility of the anterior ends of the false rib costal cartilages may lead to slipping of the affected rib under the superior adjacent rib, resulting in intercostal nerve irritation, strain of the intercostal muscles and costovertebral strain(13,14). While this false rib hyper mobility stems from the anterior ends of the false rib costal cartilages, it is important to appreciate that the rib cage system is a closed one. When one end of the rib moves, the other end moves too, which means that anterior rib hypermobility inevitably leads to problems in the posterior thoracic area (such as costovertebral strain), leading to pain (and very often) accompanied by a ‘clicking sensation’ during movement.
Homing in on SRS
Slipping rib syndrome can occur both as a result of an impact to the ribs and (as we have mentioned above), or spontaneously and without any prior trauma. Where SRS is the cause of thoracic pain, radiology and imaging tests are unlikely to be useful(11). There is however a relatively simple clinical test that (when combined with imaging and patient history information) can help diagnose SRS. Known as the ‘hooking maneuver’, this test was first described by Heinz and Zavala in 1977(15). To perform this test, the clinician places his or her fingers under the lower costal margin and pulls the hand in an anterior direction (see figure 3). If the patient experiences pain or clicking, this indicates a positive test. To confirm the diagnosis however, the use of a rib block analgesic is recommended; an absence of pain following a repeat of this test confirms a diagnosis SRS(16).Figure 3: The ‘hooking maneuver’
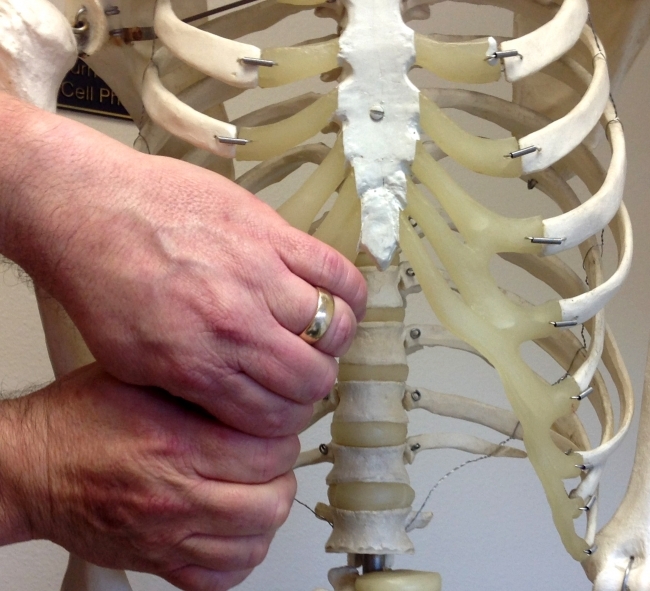
The clinician places his/her fingers under the inferior rib margin on the affected side and gently pulls the rib edge both anteriorly and superiorly.
Treatment options and prognosis
In mild cases of SRS, many athletes may experience relief with an initial period of rest and the avoidance of movements or postures that exacerbate the symptoms. This can be followed by various conservative treatments, which include soft-tissue mobilization and myofascial release, as well as stretching and strengthening activities. Anti-inflammatory pain medication taken as directed can also be helpful(11).In more severe cases, surgery may be required, which often involves the resection of any abnormal cartilaginous attachment of the affect rib(s). Although the rehabilitation period for surgery is much lengthier, the long-term outcome is still good. Possibly one of the most important benefits of an SRS diagnosis, however, is reassurance. Athletes find comfort in knowing that nothing is seriously wrong and that they can resume activities as tolerated. Crucially, it is also the first step to setting them on the road to recovery!
References
- Journal of Manual and Manipulative Therapy. 2003;11:43– 48.
- Comput Methods Biomech Biomed Engin. 2015;18:556–570
- Cureus. 2016 Nov; 8(11): e874
- Phys Ther. 2006;86:254–268
- Hollinshead’s Textbook of Anatomy. New York Press 1974
- Br J Surg. 1984;71:522–523
- Geriatrics. 1995;50:46–49
- Topics in Clinical Chiropractic. 1999;6:20 –38
- Topics in Clinical Chiropractic. 1999;6:79 –92 4,10
- Postgrad Med. 1989;86:75–78
- Journal of Athletic Training 2005;40(2):120–122
- Practitioner. 1919;102:314–322
- J Pediatr Surg. 1997;32:1081–1082
- NY State J Med. 1963;63:1670–1675
- Am Med Assoc. 1977; 237:794–795
- Med Sci Sports Exerc. 2003;35: 1634–1637
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










