Stressed loading: Second metatarsal stress fracture - Part II

Stress fractures of the second metatarsal are most common in ballet dancers, and thus the majority of the literature on the management of these conditions stems from these ballet-related research reports. The few series published in the orthopaedic literature report a quick recovery of these fractures after nonoperative treatment(1-3). For example, in a series of 64 stress fractures of the base of the second metatarsal in classic ballet dancers, these all healed with conservative care(2). If nonoperative management fails, surgery seems to give good results in most patients(4).
Stress fracture management
Management begins immediately after an abnormal reaction to stress or a stress fracture is suspected. Often plain film x-ray may not be positive for 10–21 days after the onset of symptoms. However, delaying intervention at this point may potentially accelerate the process to progress to a true stress fracture and frank fracture through the second metatarsal. Therefore, early diagnosis is very important if the athlete complains of foot pain related to exercise.It is widely accepted that the first priority is a period of rest from the stress or activity that is causing the symptoms. Zelko and DePalma describe the rest as ‘active’, allowing the athlete to exercise in a pain-free manner, prevent muscle atrophy and to maintain as much fitness as possible(5). Pain should be used as a guideline to treatment intensity, as pain during an activity may indicate exacerbation at the injury site.
Romani et al describe a 3-phase rehabilitation process that takes advantage of the physiologic healing process of the bone(6):
- Phase I- should allow time for the maturing of the periosteum, healing of damaged blood vessels to prevent ischemic injury to bone, and maturing of osteocytes(5,7).
- Phase II - should include general conditioning and strengthening specific to the injured extremity.
- Phase III- Functional weight bearing in phase III should allow for gradual remodelling of the bone and a return to the original level of activity. In the 3-phase protocol, gradually increased stress in phase III is alternated with periods of rest to let new osteocytes and periosteum mature during periods of remodelling, when the bone is weakest.
The case of the footballer
A 21 year-old elite football player who plays as an attacking midfielder presented with acute onset, right-midfoot pain sustained in a training session. He described a sudden clicking sensation on the dorsum of the midfoot over the 2ndand 3rdmetatarsals. The injury was caused by a sudden change in direction. He was able to continue training for ten more minutes; however he noticed the pain in the foot was increasing. He denied any previous sensations of midfoot pain leading up to this injury, and had spent the previous 11 weeks of pre-season training completely injury free. His rehabilitation followed the 3-phase process.Phase I
This phase focuses on removing the stress from the injured area (through use of a de-loading ‘moon boot’ – see figure 1), controlling pain, and preventing deconditioning (through cross-training). Physiologically, it is during this phase (usually up to 21 days) that the haversian canals in the bone are forming, the osteoblasts are laying down new cells, and the periosteum is maturing to buttress the weakened area of bone(8,9). Therefore, a period of initial de-loading is necessary to allow this physiological process to occur.
Acute symptoms should no longer occur with normal activities. A functional ‘moon boot’ with crutch walking is a preferable to plaster casting as the boot can be removed to exercise in a non-weight bearing manner. If poor foot alignment is present, orthotics should be fitted to correct it.
Figure 1: Moon boot for rehab
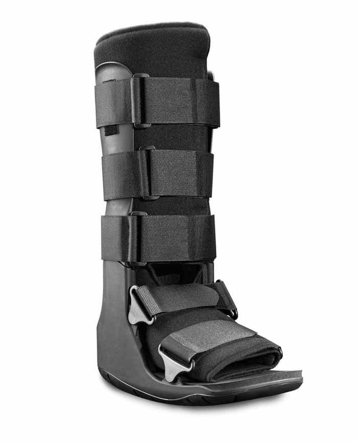
Ambulation should progress from crutch walking to full weight bearing as soon as it can be tolerated without pain. This footballer was initially non-weight bearing for the first three weeks and then progressed to touch weight bearing and then partial weight bearing over the next three weeks. This was all achieved in the absence of pain.
Condition the involved lower extremity daily with towel scrunches, ankle isometrics (calf, peroneals and tibialis posterior/anterior), and sitting range-of-motion movements on a wobble board (see box 1). These all need to remain free of pain. Exercises can be progressed by adding weight to the towel scrunches, and allowing active-range strengthening with rubber tubing.
Strength training for the upper extremity and leg conditioning for the unaffected side should continue. Cardiovascular fitness can be maintained by using the upper body ergometer or stationary bicycle or treading water in the deep tank of the pool. This player was conditioned on alternate days with upper body circuits (boxing, ropes and weights) and then swimming on the next (no kicking).
Box 1: Towel scrunches
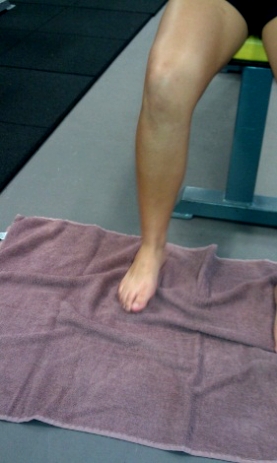
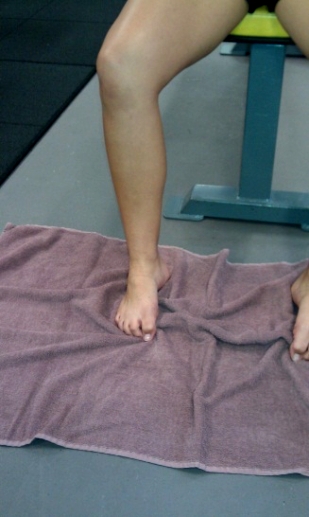
- Place a towel on a tiled or wooden floor (carpet won’t work).
- Place the foot relaxed on the towel with the foot in line with the knee and hip. The toes should be pointing directly ahead.
- Initiate the movement by attempting to firstly lift the arch. Attempt to draw the ball of the foot towards the heel and the arch will lift.
- Next use all the toes to curl the towel under the foot.
- Relax the foot and start again.
- This exercise does not cause any soreness the next day; rather, what will be felt is that the arch muscles will start to fatigue.
- The progression begins in sitting, then standing on two legs and standing on one leg. Full weight-bearing would be delayed until approximately six weeks post fracture.
Phase II
This phase (as proposed by Romani et al(6)), commences when phase I exercise and daily living activities can be performed without inflammation or symptoms. Patients must be instructed to keep their activity within a pain-free intensity and report any recurrence of pain to their therapist. Modalities that mask pain need to be avoided at this stage as they can mask the pain that signals a potentially harmful stress to the injured area. Ice and TENS should be used only after exercise to avoid masking any pain the treatments might be causing.
Pool training, which progresses from treading water in the deep pool to jogging in chest-deep water, should be added to the swimming workouts. Our football player commenced deep water running at the 3-week stage wearing a floatation belt performing 30 seconds on/30 seconds off hard running in the deep end for 30 minutes.
What also started at this stage was walking on an underwater treadmill with water up to the collarbones (which reduces effective bodyweight to only 20% of that on land). The footballer performed 30-minute walking sessions to normalise gait mechanics and maintain range of motion in the foot/ankle/knee and hip joints. Wobble-board exercises began to include weight bearing and balancing, while the rubber tubing exercises were progressed. In the final week prior to removal of the boot, he started bilateral calf raises with hand support.
Phase III
After two weeks of pain-free exercise in phase II (weeks 4 to 6 in this example), the running and functional activities of phase III are introduced. The efficacy of a cyclic training program to prevent stress fractures in military recruits has been documented by Scully and Besterman(10). By limiting the number of repetitive, high-skeletal stresses in the first two weeks of basic training, and modifying activity in the third week to exclude running, jumping, and double-time exercises, stress fracture rates were significantly reduced from 4.8% to 1.6% in a military population. The same researchers hypothesised that the initial two weeks of training promoted the formation of osteonised new bone, whereas rest in the third week allowed for the formation of periosteal new bone.
In the same manner, Zelko and DePalma have described a cyclic management strategy to facilitate normal bone remodelling in preparation for return to activity after a stress fracture(5). The running portion of phase III is completed in a cyclic fashion that mimics bone growth. As bone is being resorbed in the first few weeks of activity, running is encouraged to promote the formation of trabecular channels (functional phase). In the rest week (when the newly formed osteocytes and periosteum are maturing), running activity is decreased (ie the rest phase). In each successive cycle, the activity intensity in the rest phase is reduced to allow remodelling to occur.
In this example, a cycle of three weeks on/one week off is continued through the duration of the rehabilitation process. As the running program progresses to sprinting and sport-specific activities, the rest days between functional activities decrease, and the athlete is gradually prepared for the return to competition.
An injured athlete may note an increase in pain during the management process. If this increase in pain occurs during phase I or phase II, the offending activity should be either modified or discontinued. Those who notice pain during normal daily activities or treatment should NOT be progressed to the next phase of the protocol until the activity can be completed pain free.
During phase III, pain is usually an indication that the level of activity is too high; functional activity should instead resume at the last level that was completed pain free within that 4-week cycle. If pain persists even at a reduced level, the activity intensity should be scaled back to the level from the previous 4-week cycle. Individuals who have persistent pain should be referred back to their physician. In these cases, resuming treatment at the phase I or phase II level may be indicated.
In the example of our footballer, at six weeks post injury, the boot was removed and the player commenced full weight bearing mobilisation and running on an Alter-G running machine (see figure 2). The running volumes are shown in figures 3 and 4, which also provide the ‘acute-to-chronic workload ratio’ (ACWR) discussed in part one of this article. The table itemises the totals in tabulated form of volume, high intensity metres, change of direction and load.
Figure 2: Alter-G treadmill
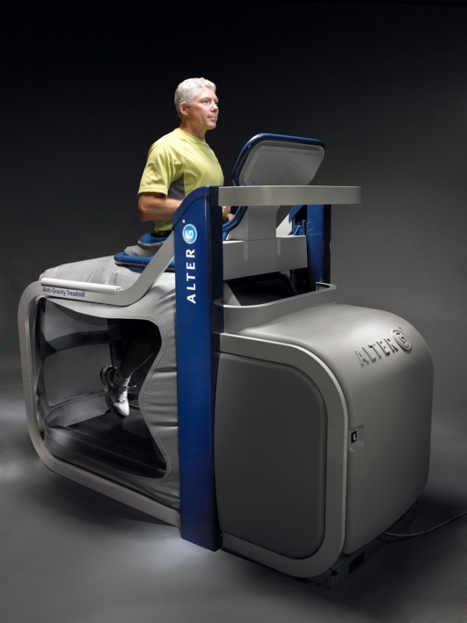
The progressions of running on the Alter-G were as follows;
- Week 6:6000m at 12-14 km/hour. Bodyweight was progressed from 60%, 65%, 70% over three running sessions conducted every second day.
- Week 7:9000m at 12-14 km/hour. Bodyweight progressed to 75%, 80% and 85%, conducted over three running sessions every second day.
- Week 8:11000m at 12-14 km/hour. Bodyweight progressed to 90%. However this was conducted so that the on Monday/Wednesday/Friday distance was set at 3000m, while on Saturday, it was set at 2000m.
At no point did the footballer feel any second metatarsal pain during or after the running. On alternative days, the footballer performed non-jump based gym exercises such as squats, partial deadlifts, hip thruster and static lunge movements. These were progressed over a six-week period and were increased in parallel with the running volumes. He conditioned ‘off feet’ on the non-running days using swimming/boxing/upper body circuits/bike.
Romani et al suggest that during the functional phase of the program, the athlete continues the phase II exercises, and progresses to mobility and jumping activities in the pool and on land(6). Once the athlete can squat 1½ times his/her body weight, higher-level plyometric training may begin. These (and all) functional activities should be implemented in the pool before their initiation on dry land. This progression enables the remodelling bone to begin, adapting to the stresses of jumping and cutting in a less stressful environment. Our footballer had been performing some double and single leg jumps in the pool as part of his off-feet swimming sessions.
At week 9, the footballer commenced on-field running (100% bodyweight). In this week, the total running volume actually dropped to only 8000m. As discussed above, this is a recommendation based on the literature, which shows that ‘cyclic’ training and periodic drops in volume allow for bone remodelling(5,10). Field running and football-related drills started at week 9 and were progressed over a 4-week period - again building for three weeks and then dropping the volume and intensity in the fourth week (see figure 3).
Figure 3: ACWR table

Showing distance (blue), high intensity metres defined as 19-25kph (orange) and change of directions (grey). The middle zone represents the period of time this footballer was not running.
From week 13 onwards, the footballer was included in all football-related skills and conditioning including contact training. Again, during this first ‘full week’ his total volume was reduced to allow for cyclic bone healing. He trained a full three weeks with a gradual increase in volume (distance), change of direction, high intensity metres and load (see figure 4). These are all measured using GPS technology. What he also started in week 13 was easy plyometric and gym-based landings off boxes. This was progressed over a 2-week period prior to his first match. He played his first competitive match at week 15 post diagnosis. He was and has remained pain free through-out the rehabilitation process.
Figure 4: Tabulation of volume, high intensity metres (19-25kph), change of direction and load
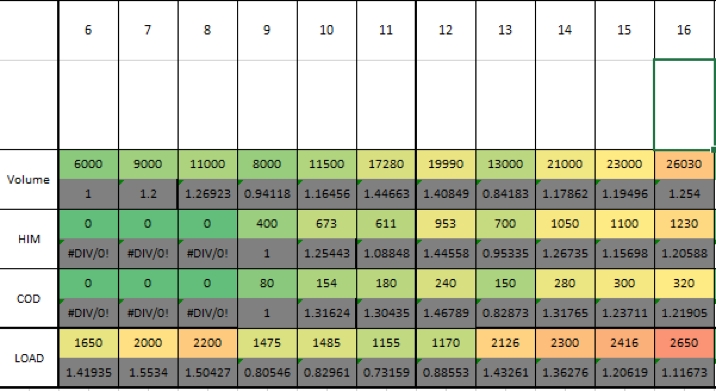
This commences at 6 weeks post diagnosis. The initial 6 weeks the footballer was non-weightbearing progressing to partial weight-bearing. Load is measured as time multiplied by rate of perceived exertion (RPE).
Summary
Stress fractures at the base of the second metatarsal are a reasonably uncommon injury suffered primarily by ballet dancers. This article has presented a case of second metatarsal stress fracture in an elite footballer. Early diagnosis using CT scan and/or MRI technology is crucial to prevent the progression to complicated fractures. Once identified, the management of this condition is reasonably straight forward, with a gradual progression in bone load through running progressions taking in to account the cycling of load over 3-4 week cycles. The running-based athlete will take 12-16 weeks to return to full function after diagnosis and initial off-loading.References
- J Bone Joint Surg Am. 1985, 67:1372–1375
- Foot Ankle Int. 1996. 17:89–94
- Am J Sports Me. 2004. 32(6):1535–1537
- Scand J Med Sci Sports. 2007. 17:383–386
- Postgrad Adv Sports Med. 1986; I-IX:1–20
- Journal of Athletic Training 2002;37(3):306–314
- Physician Sportsmed. 1981;9(5):47–58
- 1970; 10:532–541
- Am J Sports Med. 1985;13: 285–294
- Mil Med. 1982;147:285–287
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Further reading
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.






