You are viewing 1 of your 1 free articles
Axillary nerve injury: a pressing problem

Athletes who participate in contact sports such as football, rugby, ice hockey and wrestling, are particularly vulnerable to injuries to the axillary nerve(1,2). Common mechanisms of injury include falls, shoulder dislocations, blows to the upper arm, and compression. Vulnerable during any surgical procedure at the shoulder, iatrogenic injury to the axillary nerve remains a serious complication of shoulder surgery.
Anatomy
The axillary nerve originates from the C5 and C6 spinal nerve roots, and arises from the lateral aspect of the posterior cord of the brachial plexus(3). It courses laterally and inferiorly (lateral to the radial nerve) and anterior to the subscapularis muscle (see figure 1). It then passes dorsally through the quadrilateral space just below the shoulder joint. The subscapularis muscle and the capsule of the joint form the superior border; the surgical neck of the humerus the lateral; the long head of triceps the medial; and the teres major muscle the inferior border.After passing posteriorly through the quadrangular space, the axillary nerve divides into anterior and posterior branches. The shorter posterior branch supplies the more posterior deltoid muscle fibres and the teres minor(4). It also gives rise to the upper lateral cutaneous nerve and supplies the skin over the deltoid.
The anterior branch of the axillary nerve innervates the anterior and middle parts of deltoid muscle, and the shoulder joint capsule(5). In 65% of shoulders, the axillary nerve splits into the anterior and posterior branches within the quadrangular space. In the other 35% of shoulders, the nerve splits within the deltoid muscle(5). The nerve is only free for a short distance in the axilla then for the remainder of its length, attaches to the deltoid muscle by numerous branches. This renders it susceptible to stretch injury in shoulder dislocation and local trauma.
Figure 1: Anatomy of the Axillary nerve
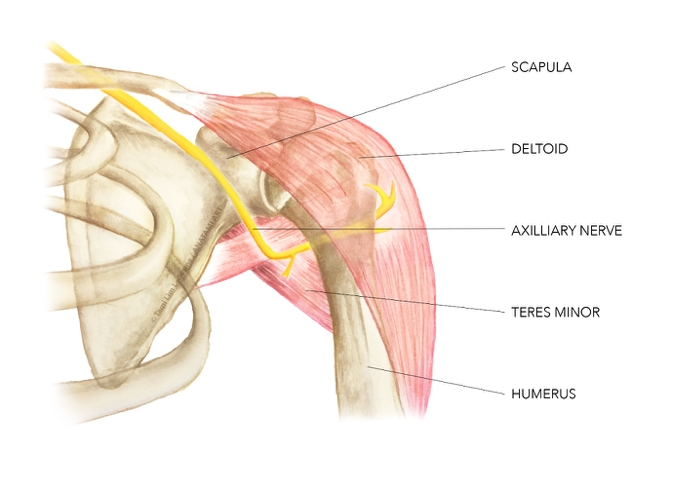
Injury to the axillary nerve
The axillary nerve is one of the most commonly injured peripheral nerves in athletes who participate in contact sports. However, the axillary nerve may be injured in other ways outside of the sport setting. The multiple mechanisms of injury include:- Following fracture of the neck of the humerus(6).
- Following anterior shoulder dislocation.
- During reduction of a shoulder dislocation(7).
- Blunt shoulder trauma such as direct contact(2,8).
- Compression neuropathy such as ‘quadrilateral space syndrome’ (entrapment of axillary nerve)(9,10).
- Iatrogenic injuries in surgery(5):
- Shoulder arthroscopy
- Thermal shrinkage of the shoulder capsule
- Plate fixation of the proximal humerus (the deltoid muscle is retracted)
- Intramuscular injections in deltoid, intra-articular and intra-bursal steroid injections due to lack of proper anatomical knowledge of the nerve(11-13).
The incidence of axillary nerve palsy following anterior dislocation of the shoulder has variably been reported as being between 5.8% and 48%(14-16). The mechanism of axillary nerve injury in shoulder dislocations consists of traction and compression forces applied during stretching of the nerve across the humerus, as it dislocates anteriorly. This commonly leads to an injury to the nerve before it enters the quadrilateral space. This is proximal to the branch point of the anterior and posterior divisions. Therefore, the anterior branch of the axillary nerve that courses through the quadrilateral space (around the surgical neck of the humerus - deep to the deltoid) is affected. This results in loss of motor strength to the anterior and middle portions of the deltoid.
In addition, the posterior branch of the axillary nerve, which divides at the inferior aspect of the glenoid and then branches into the superior lateral cutaneous nerve of the arm and the nerve to the teres minor, is also affected(17-19). These nerve injuries following shoulder dislocation may be initially missed. This is because in many patients, such injuries may pass undetected (being mild in degree), or because the joint or bony injuries dominate the clinical picture.
Axillary nerve injury after blunt shoulder trauma suggests that extreme shoulder displacement and scapular thoracic movement (with relative fixation of the proximal portion of the axillary nerve, posterior cord and brachial plexus) can also be a mechanism of injury. The iatrogenic injuries may be due to anatomical variations of the axillary nerve beneath the deltoid muscle. Surgeons need to appreciate the exact anatomical location of the nerve and its course to avoid the possible damages and to protect the nerve during surgery and injections.
The unhappy triad
Gonzalez and Lopez first reported the combination of peripheral nerve injury and rotator cuff tear following anterior dislocation of the shoulder(20). This is termed the ‘unhappy triad’ of the shoulder(21), and the ‘terrible triad’ of the shoulder(22). The incidence of the terrible triad was assumed to be 9–18% of all shoulder dislocations. Then Takase et al reported a unique case of concurrent rotator cuff tear and axillary nerve palsy associated with anterior dislocation of the shoulder and a large glenoid rim fracture - a so-called ‘terrible tetrad’(23).Quadrilateral space syndrome is seen in overhead sports that require repetitive throwing actions. This represents a chronic compression syndrome of the axillary nerve(24). This syndrome develops due to the close proximity of the teres minor to the quadrilateral space. Teres minor forms the superior margin of the quadrilateral space. If fibrous bands develop at the inferior edge of the teres minor, they can compress both the axillary nerve and the posterior humeral circumflex artery. Quadrilateral space syndrome can cause complete denervation of the deltoid and teres minor muscles by compressing the axillary nerve. Compression could be more severe in the abducted, externally rotated (throwing) position(24).
Recovery following axillary nerve injury
Prognosis following anterior dislocation for neurological recovery is reportedly excellent, as lesions associated with dislocations are typically either neuropraxic or axonotmetic lesions(4,9). Perlmutter noted that in 11 contact athletes who suffered isolated injuries to the axillary nerve (all from direct contact and collisions), all had excellent functional recovery of the shoulder range of motion and strength even with residual loss of deltoid strength and muscle bulk(2).Recovery often occurs spontaneously with closed injuries because the lesion is typically in continuity and the nerve injury is a neurapraxia. The majority of nerve injuries are temporary neuropraxias, which typically resolve within 6-12 months of injury. However, permanent axillary nerve deficit can occur(8,14).
An athlete with an axillary nerve injury can be deceptively functional on simple examination; Alnot et al noted that normal shoulder range of motion is possible following an axillary nerve injury if the suprascapular nerve and rotator cuff muscles are intact(25). However, without the deltoid, the shoulder will fatigue easily and possibly limit endurance-based activities(26).
Escamilla describes how the moment arms for the deltoid are more significant over 60 degrees of abduction, whereas the moment arm from 0-60 degrees favours the rotator cuff muscles(27). This implies that the deltoid is a more effective abductor at higher abduction angles than the rotator cuff muscles(27). However, sole reliance on the rotator cuff may be problematic in later years, especially given high rates of partial or complete rotator cuff tears in the aging population(28,29).
What can complicate the recovery following an axillary nerve injury is an associated injury to the rotator cuff at the time of dislocation or proximal humerus fracture. Therefore, early diagnosis and surgical repair of rotator cuff tears associated with shoulder dislocation is crucial, as early repairs favour improved outcomes compared with delayed repairs(30). Due to pain and swelling in the shoulder following dislocation or fracture, it may be difficult to diagnose rotator cuff tears. Anterior dislocations are associated with 14–63% chance of rotator cuff tear(31); therefore an MRI should always be performed when the patient has persistent pain or muscle weakness after reduction of the shoulder after dislocation.
Injury signs and symptoms
Accurate diagnosis of an axillary nerve injury is based on a careful history and physical examination, as well as an understanding of the anatomy of the shoulder and the axillary nerve in particular. Clinical features suggestive of nerve injury are as follows:- Direct trauma to the shoulder either as traction (dislocation) or compression (direct hit).
- Widespread pain within the shoulder (however a number of axillary nerve injuries may be asymptomatic).
- Difficulty in abducting the shoulder.
- Loss of muscle bulk of the deltoid.
- Loss of sensation over the deltoid. This last symptom may be difficult to assess in the acute situation, as most athletes with a shoulder dislocation report a dead or numb arm sensation.
Diagnostic workup
Examinations and radiographs that may be useful in this stage are as follows:- Electrophysiological testing, nerve conduction and needle electromyography, and recording the compound muscle action potential (CMAP) from stimulating the axillary nerve at Erb’s point. NB - it is worth noting that in the acute situation, nerve conduction and needle electromyography may be normal, even when the relevant nerve is ruptured. Electrophysiological changes take about 7–10 days to develop after nerve injury caused by nerve transection(4). In such cases, clinical suspicion of the injury is paramount.
- Xrays and MRI/MRA. These are useful to exclude co-existing injuries such as glenoid rim fractures, rotator cuff injuries.
Treatment
The majority of axillary nerve injuries are mild. These are usually due to closed trauma, and this may result in temporary neuropraxia or axonotmesis of the nerve. These can resolve spontaneously with complete and rapid recovery of deltoid function. Therefore, the bulk of axillary nerve injuries may be successfully managed conservatively.The initial management of isolated axillary nerve injury includes symptomatic management with rest, reassurance that function will return in the majority of patients, and physical therapy. The main ‘work-on’ points for the therapist are as follows:
- Maintaining shoulder range of motion (initially passive followed later by active). This can be done using PNF techniques (discussed below).
- Strengthen the rotator cuff.
- Strengthen the periscapular stabilisers.
Any bony (glenoid rim fracture or proximal humerus), ligamentous (Bankart lesion) injury or rotator cuff rupture should be treated as indicated. Maintaining shoulder range of motion is important to avoid shoulder joint contracture. Loss of shoulder mobility may ultimately affect functional outcome, despite a return of axillary nerve function.
EMG/nerve conduction velocity studies should be obtained within the first 3-6 weeks to document the nerve injury, and to obtain a baseline for later comparison(18). Because the axillary nerve is relatively short, in the case of a second-degree injury (axonotmesis), recovery should be seen between 3-4 months after injury. Surgical exploration and possible nerve grafting are generally recommended if no return of function has occurred by 4–6 months after injury(8,25,32).
PNF techniques
Proprioceptive Neuromuscular Facilitation (PNF), a therapeutic approach based on human anatomy and neurophysiology, uses proprioceptive, cutaneous (touch) and auditory input to produce functional movement. Often used in the rehabilitation setting for stroke victims, paralysis, neuromuscular disorders, and patients who have suffered peripheral nerve injuries, PNF has merit for axillary nerve injuries awaiting neurological recovery.The neuro-physiological basis of PNF stems from Sherrington’s laws of facilitation and inhibition. As a nerve signal travels down the corticospinal tract (spinal cord), it hits its target motor neurons (that form the peripheral nerve) and the nerve excitation can spill over to adjacent ‘fringe’ motor neurons in the same motor neuron pool. For example, if you extend your knee (quadriceps activation) with your foot dorsiflexed (tibialis anterior), the resulting quadricep contraction is stronger.
This is explained by the fact the nerve root level for the quadriceps and tibialis anterior is both at L4. This is a great way to ‘excite’ a weak muscle and improve its contraction. Conversely, other muscles not in the fringe area with the motor nerve pool will be dampened down. This known as inhibition. This is great muscles that are high tone and need to be calmed down.
What influences the motor nerve the most are the stretch receptors found in the tissues in and around the target muscle that need to be excited or inhibited. PNF therefore uses the proprioceptors to modulate the alpha motor neuron. The primary principle behind PNF therapy is the activation of the stretch reflexes via:
- Golgi tendon organs (GTOs). These detect changes in tension.
- Muscle spindles. These are sensitive to a change in length, as well as the rate of change in length of the muscle fibre.
PNF for strengthening of the shoulder involves two distinct patterns of movement. The first is known as diagonal 1:
Shoulder flexion, adduction, external rotation (d1 flexion) and extension, abduction, internal rotation (d1 extension); elbow flexed/extended; wrist & fingers extension to flexion (see figure 2).
Figure 2: D1 extension and flexion
D1 extension start position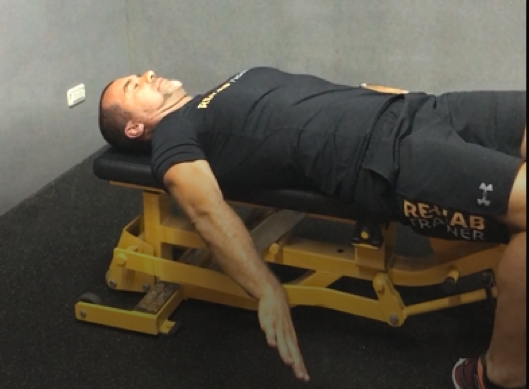
D1 flexion position
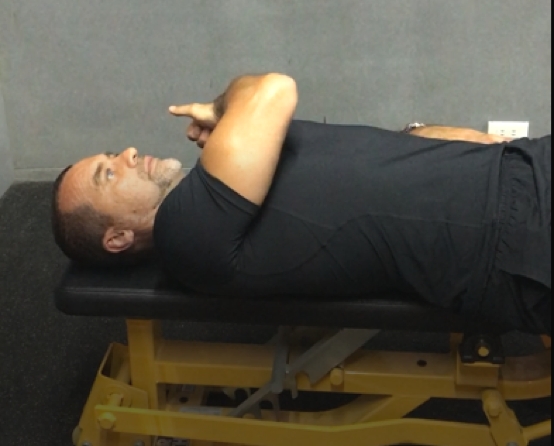
The second is diagonal 2:
Shoulder flexion, abduction, lateral rotation (d2 flexion) and extension, adduction and medial rotation (d2 extension); elbow extended; wrist & fingers flexion to extension (see figure 3).
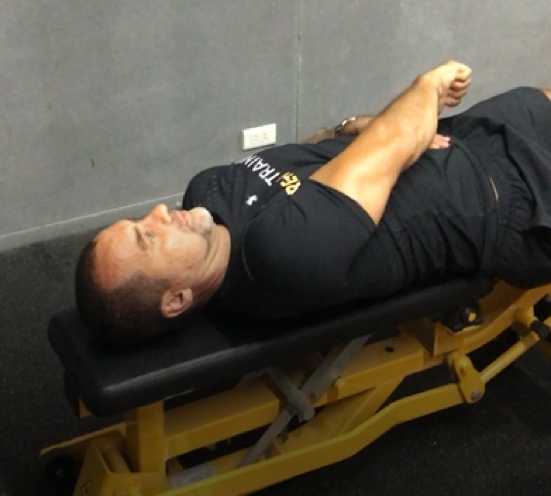
Figure 3: D2 flexion and extension
D2 flexion start position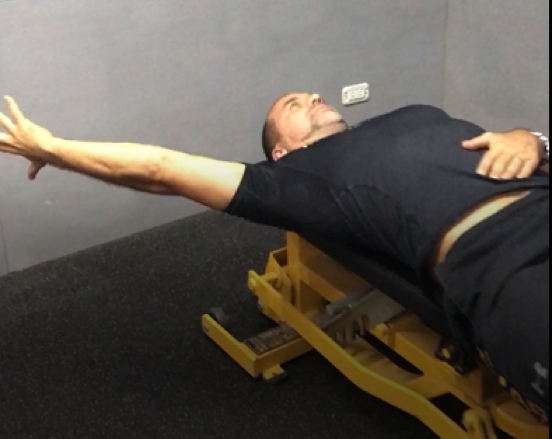
D2 extension position
It is far beyond the scope of this paper to describe all of the various methods used in PNF strengthening. These have traditionally all been guided by the therapist. In short, the basic techniques used in strengthening are:
- Rhythmic initiation (useful in the early stage when deltoid contraction is absent).
- Repeated contraction.
- Slow reversal (useful as the deltoid function returns).
- Rhythmic stabilisation.
Surgical management
The indications for surgical management include:- A symptomatic patient with persistent deltoid weakness and no improvement in shoulder function;
- Serial electrodiagnostic studies showing no improvement by 4-6 months(2, 18, 32).
- Rupture of components of the infraclavicular brachial plexus without associated fracture or dislocation. (This is a rare but recognised event following blunt trauma to the shoulder)(33, 34)
Acute nerve ruptures should be surgically repaired, and the outcome is far superior when the surgery is performed early(8,25,32). Delaying the repair of the nerve is associated with increased technical difficulty - principally because the nerve ends are retracted and embedded in scar tissue. In cases where there has been an associated vascular injury, nerve stumps may be encased in a false aneurysm, further complicating the difficulty of the repair. Delayed surgery may also be unsuccessful if the denervated muscle has become fibrosed. In such situations, even with successful nerve reinnervation, the functional outcome may remain poor(35).
Nerve repair, nerve grafting, and nerve transfer have all been described for isolated axillary nerve injury with good results(26, 32).The typical types of surgical interventions, their success rates and important points about surgical interventions can be summarised as follows:
- Studies suggest that the best outcomes after nerve grafting and nerve transfer are achieved when performed within one year following the nerve injury(32,36).
- There are comparable results between nerve transfers (triceps branch of the radial nerve transferred to the axillary nerve) and nerve grafting for axillary nerve injury(37).
- In a study of ten patients with isolated axillary nerve injury after trauma(38):
- Two patients were treated nonoperatively because of good shoulder function with retained active motor potentials on EMG. These had moderate to good outcomes.
- Four were treated with sural nerve grafting, three of which had good outcomes.
- Three patients had a radial to axillary nerve transfer all with good outcomes.
- One patient had nerve exploration with finding of a neuroma with a good result.
- Management of persistent axillary neuropathy has traditionally consisted of axillary nerve grafting, with 73% to 88% of patients regaining useful deltoid strength(39-41).
- Triceps branch to axillary nerve transfer was originally described for C5 and C6 brachial plexus injuries(42). This type of surgical transfer has been effective for restoring shoulder abduction, external rotation and stability. It has the advantages of a single neurorrhaphy in close proximity to the target muscle, and a single operative site. It shows excellent functional deltoid strength recovery(43).
Conclusion
Axillary nerve injury remains the most common peripheral nerve injury to affect the shoulder. It is most often is seen after shoulder joint dislocation, proximal humerus fracture, or a direct blow to the deltoid muscle. Compression neuropathy has been reported to occur in the quadrilateral space syndrome.The axillary nerve is vulnerable during any operative procedure involving the inferior aspect of the shoulder, and iatrogenic injury remains a serious complication of shoulder surgery. During the acute phase of injury, the shoulder should be rested, and when clinically indicated, a patient should undergo an extensive rehabilitation program emphasising range of motion and strengthening of the shoulder girdle muscles.
If no axillary nerve recovery is observed by 4-6 months after injury, surgical exploration may be indicated, especially if the mechanism of injury is consistent with nerve rupture. Patients who sustain injury to the axillary nerve have a variable prognosis for nerve recovery although return of function of the involved shoulder typically is good to excellent, depending on associated ligamentous or bony injury.
References
- Neurosurg Focus. 2011. 31(5). E10
- Am J Sports Med 1997;25:65–8
- David Johnson. Pectoral Girdle and Upper limb. Gray’s Anatomy. 40th Ed, Elsevier Churchill Livingstone. 2008; 821
- 1951. 74(4) 491–516, 1951
- Surgical and Radiologic Anatomy. 2009;31(3):43-47
- J Neurol Neurosurg Psychiatry 1984;47:742–4
- Can J Neurol Sci. 1992;19:300–1
- J Neurol Neurosurg Psychiatry 1982;45:1027–32
- Surg Radiol Anat. 2010;32(3): 193-201
- J Am Acad Orthop Surg 2001; 9(5): 328–35
- Am J Phys Med Rehabil. 2007;86(6):507-11
- Human Vaccines. 2011;7(8):845-84
- Journal of the Tsuruma Health Science Society. 2003;27(1): 33-37
- J Bone Joint Surg Br 1994; 76(3): 381–3
- J Bone Joint Surg Am 2012; 94(1): 18–26
- J Bone Joint Surg Br 1999; 81: 679–85
- J Bone Joint Surg Am 2003; 85-A(8): 1497–501
- Am J Sports Med 2004; 32(3): 803–19
- J Shoulder Elbow Surg 1992; 1(1): 31–6
- J Bone Joint Surg Am. 1991. 73(4) pp620–621
- J Orthopaedic Trauma. 1994. 8(5), 429–430
- J Shoulder and Elbow Surgery. 1995. 4(1), pp51–53
- Takase et al (2014) Concurrent Rotator Cuff Tear and Axillary Nerve Palsy Associated with Anterior Dislocation of the Shoulder and Large Glenoid Rim Fracture: A ‘‘Terrible Tetrad’’. Case Reports in Orthopedics
- AmJSportsMed 14:511– 513, 1986
- Revue de Chirurgie Orthopaedique. 1996; 82:579–89
- J Hand Surg. 2014; 39: 940-7
- Sports Med 2009;39:663-85
- J Bone Joint Surg. 1995;77A:10-5
- J Shoulder Elbow Surg 1999;8:296-9
- Clinical Orthopaedics and Related Research. 1983. 175. 18–24
- Annals of the Royal College of Surgeons of England. 2009.91(1) pp.2–7
- J Hand Surg. 1982; 7:271–8
- 1985; 16:305–6.
- J Accid Emerg Med 2000;17:3780–9
- Seddon H. Surgical disorders of the peripheral nerves. Edinburgh: Churchill-Livingstone Press, 1972
- Chir Main 2000; 19(1): 31–5
- J Hand Surg Am 2014; 39(7): 1351–7
- J Plast Surg Hand Surg 2012; 46(3–4): 257–61
- J Bone Joint Surg [Br].1999;81:212–17
- Int Orthop. 1991;15: 7-11
- J Bone Joint Surg 1997;79B;527-31
- J Hand Surg. 2003;28A:633-8
- Plast Surg. 2015. 23(2). 77-80
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









