Foot pain: looking up the kinetic chain
Foot injuries among athletes can originate from many sources. Tracy Ward explores the common problems, what may cause them and how you can prevent yours by looking further afield.
The foot is the most complex region of the lower limb, and probably the most intricate area in the body. It serves as a launching pad of the athlete; being the first part to contact the ground, absorbing the ground’s forces (which can exceed more than four times your body weight running or up to 12 times with jumping and impact) and propelling the athlete forwards, or in to any direction they desire(1).. It is therefore not surprising that the foot can become overused and subject to numerous localised injuries. However, the problems can also originate from further up the kinetic chain (further up the leg) such as the pelvis/hips, knee and/or ankle. Injuries or bio-mechanical problems more proximally up the leg can have a subsequent, indirect effect on the foot mechanics(2).. Directly or indirectly, foot problems can therefore be a huge burden on the athlete. Here we present the issues to consider and how to address them.
Collectively the foot and ankle structure hosts 26 small bones that form 33 joints to allow the dynamic nature the foot provides to meet the athlete’s demands. Over 100 muscles, ligaments and tendons connect these joints together. Additional structures then connect the foot to the lower leg. The Achilles tendon connects the calcaneus (heel) to the calf muscles and provides major ankle stability. The front of the leg is supported by the tibialis anterior, which provides the upward motion to the foot, and the back of the leg is supported by tibialis posterior, which supports the foot arch. The peroneal muscles are located on the outside of the leg and ankle and provide lateral stability. These intricate connections depict how a foot imbalance can affect the rest of the lower leg, and vice versa.
Ankle sprains are damage to the ligaments, and are reportedly the most common trauma ankle/foot injury in athletes(3).. Approximately 30% of ankle sprains then go on to develop chronic ankle instability, giving a less stable base at the bottom of the leg to impact the ground. This then affects the whole lower limb as the alignment of the leg will be imbalanced and stress the joints and muscles incorrectly. Achilles tendonitis and plantar fasciitis are the two most common overuse injuries, resulting in inflammation of the Achilles tendon and plantar fascia (ligament along the sole of the foot) respectively(4).
Stress fractures can occur to any of the foot bones (see figure 1). These are likely found where the athlete is heavier weight bearing and will depend on how they strike the ground. Finally, tendon strains can occur to the anterior or posterior tibialis muscles, or to any of the tendons associated with the foot and ankle. How these structures become impaired can be the result of the athlete’s biomechanics. This is simply how they move; how their foot strikes the ground and how all the muscles and joints respond to this further up the limb.
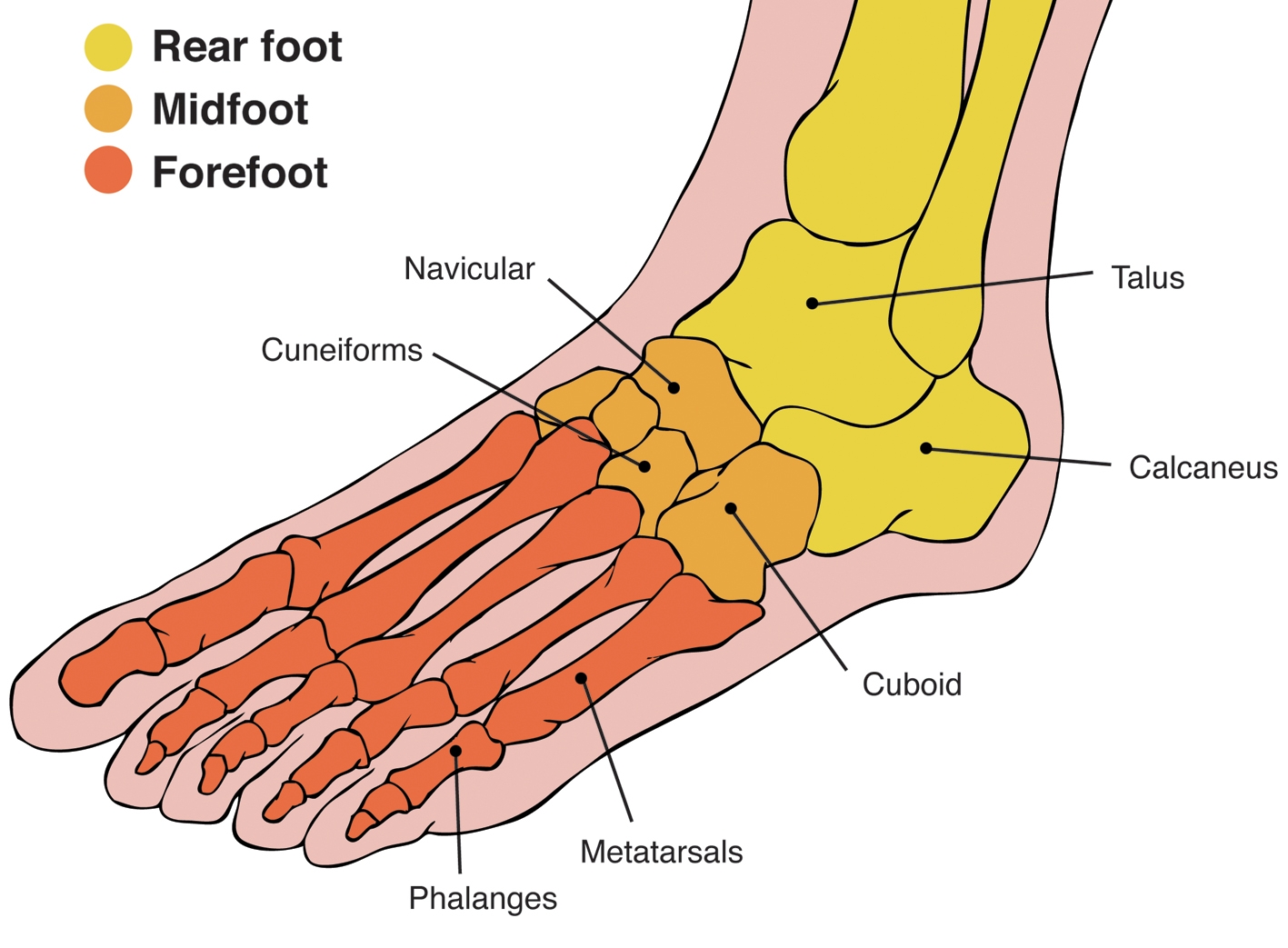
Figure 1: Foot anatomy
The sections of the foot are shown as the forefoot, midfoot and rearfoot. Within these sections the main bones are labelled. The forefoot consists of the toes (phalanges) and these are connected to the midfoot by the metatarsals. The midfoot region is the shock-absorbing section and is formed by the cuneiform, navicular and three cuneiform bones. The rearfoot houses the talus and calcaneus (heel bone) and together these form the subtalar joint. The subtalar joint provides approximately 40 degrees of inversion and 20 degrees eversion of the ankle. The talus then meets with the ends of the tibia and fibula to form the ankle joint (talocrural joint) and is responsible for 20-30 degrees ankle dorsiflexion and 30-50 degrees plantarflexion.Biomechanics
Running pattern is difficult to analyse for every sport and every individual within this one discussion, as how the athlete contacts the ground will depend on what they intend to do next. Distance runners will impact the ground usually with their heel first (see figure 2); however, those who are sprinting or rapidly changing direction may utilise the forefoot initially. How the foot plants the ground can have substantial consequences thereafter.
The foot usually strikes the ground initially with supination at the subtalar joint; this is where the sole of the foot is angled slightly upwards. As the weight loads through the foot, it then rolls inwards in to pronation, with more weight on the inner edge of the foot. The position of the foot controls the alignment of the rest of the leg as they work in coordination. Figure 2 shows the different positions of the knees and hips at the different phases of foot strike. Too much rotation of the foot, however, can then be detrimental as it impairs these other positions.
If the foot strikes in an excess pattern of increased pronation or supination, research has shown that the athlete is subject to greater ground reaction forces and rate of loading; this is the force returned from the ground, and the speed at which the load transmits through the foot(5).. If the foot presents more in to pronation, there is excess internal rotation of the lower limb. This causes increased pressure to the medial structures, such as the big toe and plantar fascia. The calf muscles and peroneal muscles then work harder to control the foot angle and prevent further rotation. This creates an imbalance of forces at the patella (knee cap) and can strain the quadriceps and iliotibial band. Conversely, a more supinated foot strike has less mobility at the foot and ankle because they cannot roll in their natural movement pattern(6).. Less mobility leads to less shock absorption so a greater force is transmitted through the foot, ankle up to the knee and hip. Ankle sprains are also more common with supination and inversion, as this places the lateral ankle ligaments on full stretch and strain.
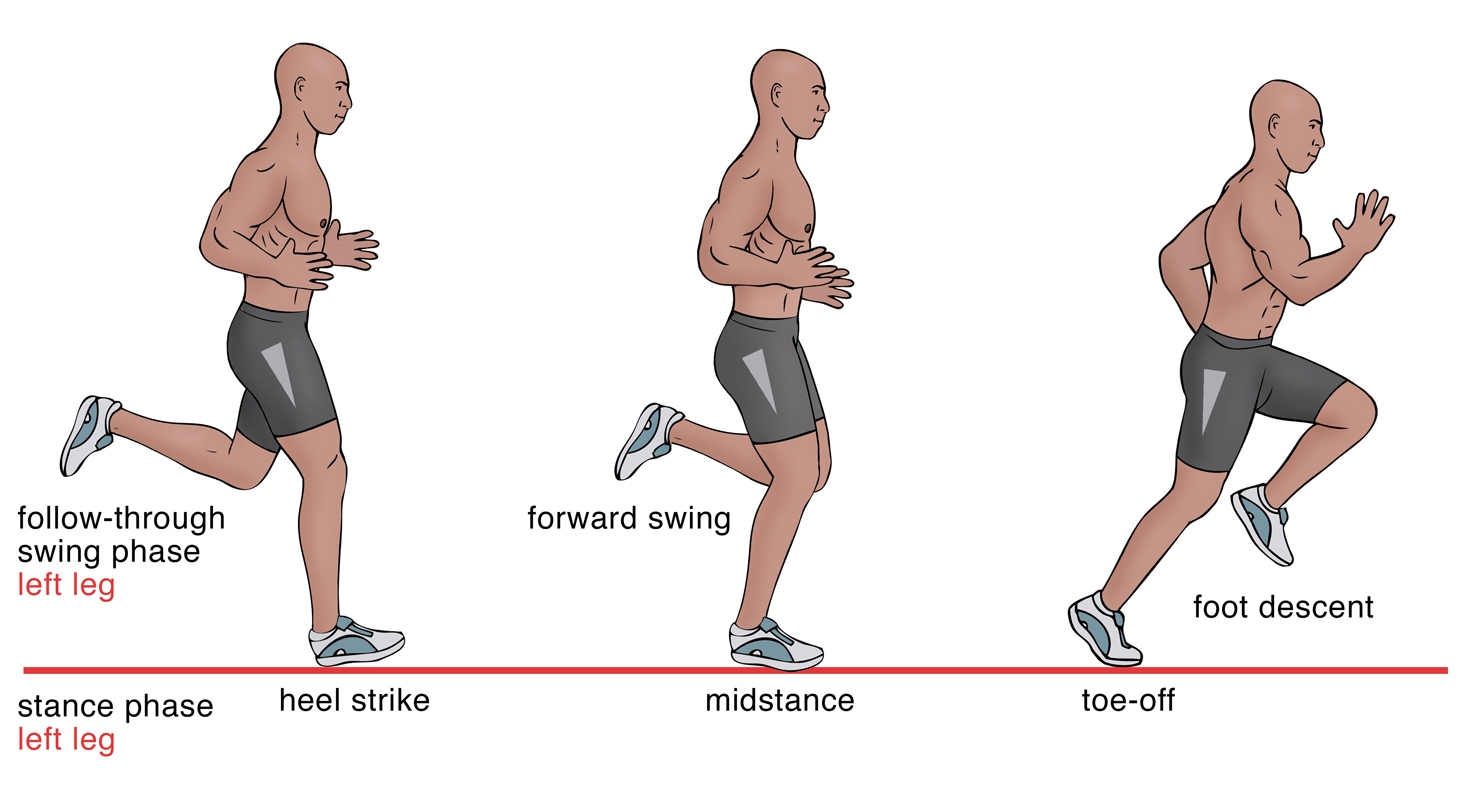
Figure 2: The phases of a running pattern(7)
The runner strikes with the heel, then plants the foot in mid-stance, before pushing off with the toes.Problems not to miss
In addition to the common local foot and ankle injuries mentioned earlier on, there are other sources of foot pain, not originating from the foot, that should not be overlooked: ankle impingement, gluteal weakness, and core instability.
1. Ankle impingement
Ankle impingement can occur anteriorly or posteriorly. Both types involve the pinching of structures which restrict the ankle and foot movements and can be severely disabling. Dancing, athletics and soccer are the most commonly reported affected sports(8).. Ankle impingement can be the result of ankle instability. Lax ankle ligaments allows greater translation of the joints and small bones, allowing gliding of the bones and can impinge on the surrounding soft tissues and tendons(9).. This painful condition can refer pain throughout the foot and ankle. This is a complex problem to diagnose and must be considered if other injuries are ruled out.
2. Gluteal weakness
Gluteal weakness is often due to an asymmetry at the pelvis. This can occur naturally as we weight bear more favourably through our dominant leg and cause it to be stronger and more stable. Furthermore, the gluteals often are not brought to full activation during everyday activities, as this requires proper squatting or deadlift manoeuvres, and therefore a lack of activation means they will eventually inhibit their function. Any injury that causes pain will also cause a pain inhibition effect on the gluteals. This is because of the powerful and propulsive role the gluteal muscles have, that if you have injured any lower limb structure, the body inhibits the gluteals to slow you down. This will reduce the ability of the athlete to push harder(10). This is why regular gluteal training is essential to all athletes whether they are injured, or not.
3. Core instability
The core muscles are enclosed within your trunk region and work endlessly to maintain posture and keep the body in correct alignment. This ensures the forces are distributed correctly throughout the body and that one limb, joint or structure is not overloaded. The core muscles respond to changing dynamics and as you change position they transfer the weight as required, and bridge the space, and load between the upper and lower limbs(11)..
Treat from above
Once the local injury has been treated directly, the therapist should then explore the additional intrinsic factors that may have contributed to the problem. These are the problems within the body including muscle weakness and imbalances. The main areas are the gluteal muscles and core stability. Balance is also a huge factor, incorporating all muscles and core work.
1.Gluteal strengthening
These should be performed for the weak side initially to make up the discrepancy, and thereafter completed on both sides for bilateral stability and balance. Up to 3 sets of 10 can be instructed; however, it is more about quality of the movement and control than numerous repetitions.
2.Core stability and balance
These should be performed on both sides to encompass the whole core region. These exercises are all done on a mat, on the stable floor surface. There is great speculation that performing core exercises on an unstable surface such as a Bosu ball, gym ball, wobble cushion etc provides greater core demand. Whilst this does provide an added challenge to the athlete, a recent study showed that performing core exercises on the unstable surfaces had no further advantage to physical fitness than the same exercises performed on the stable ground(12).. So whilst they may be more core intensive, they do not transfer to greater fitness benefits and perhaps executing the exercise with good technique is more important here than trying to achieve the hardest version.
3. Single-leg balancing
Balance exercises on one leg are important to allow the whole kinetic chain to work together and coordinate, because most of the above exercises work muscle groups in isolation. These can also be tailored to the athlete by mimicking positions they may encounter during play. Single-leg balancing also strengthens the intrinsic foot muscles (small muscles between the foot bones) by encouraging them to function as they grip the surface for stability.
Suggested exercises to strengthen the kinetic chain





Treat outside the box
Once the intrinsic factors have been addressed, the therapist should also consider the extrinsic influences. These are the external, environmental factors that may contribute to injury such as type and support of footwear, training plans, and training surfaces.
1. Footwear selection
Footwear is a hugely individual preference, and will also come down to the type of sport being played. Once the foot strike pattern has been identified the correct footwear can be selected. Those who overpronate will require a shoe with extra stability and control, and this usually consists of a medial arch support within the shoe. Those who have excess supination will require a trainer that provides extra cushioning and padding to absorb more shock. Trainers gradually lose their support and shock absorption capacity and, for the amateur, after 250 miles they will have depleted approximately 30-50% of their support. By 500 miles the athlete should be looking to replace their trainers to maintain good support(13).. For the serious athlete the mileages could be much less. Having two pairs to alternate will also accustom the foot to different supports and minimise the wearing down of one trainer. More frequent change than this is not recommended, however, because new footwear will be more rigid, and research has shown that this causes an increase in the plantar pressure; this is the pressure the athlete places through the foot when running and could place extra strain through the foot structures(14) .
2. Modified training plans/grounds
The surface by which an athlete plays on can be attributed to injury, although the evidence for this is not outstanding. In general, harder, drier surfaces can cause overuse injuries such as stress fractures and tendinopathy, as there is less shock absorption and more impact through the joints. Artificial grounds generally have a higher shoe-surface friction and are related to higher injury rates(15). If an athlete is recovering from injury, return to sport should be guided through suitable surfaces/softer grounds initially before return to normal surfaces.
Summary
- The foot is responsible for all weight bearing activities, absorbing the ground’s reaction forces, and propelling the athlete in movement;
- The position the foot strikes the ground can influence injury, particularly if the foot is over-pronated or supinated;
- The stability and alignment of the hips and knees can affect the angle the foot is positioned at, and impacts the ground;
- Local foot positioning and patterns should be assessed first, followed by correction of abnormal foot strike, altered arches, knee position and pelvic position.
- Strengthening exercises should work the gluteal muscles, core stability, alignment of the lower limb, and balance work;
- Other factors to consider include the type of trainer or footwear, insoles, training grounds, and training plans.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









