Navigating the Clinical Impact of Hormonal Contraceptives: Part II
In Part II of this series, Candice Macmillan provides a Clinical Decision-Making Framework for Contraceptive Use by athletes.
In the evolving landscape of sports medicine, the intersection of reproductive health and athletic performance has become a focal point for practitioners. Despite the prevalence of hormonal contraceptive (HC) use among sportswomen, athletes frequently report feeling under-informed about how these medications affect their performance and injury risk(1). As discussed in Part I, the influence of different contraceptive methods is highly individualized, with varying effects on injury risk and physiological markers(2).
To bridge this information gap, a structured, athlete-centered approach that balances reproductive rights, symptom management, and performance optimization can help practitioners guide athletes in contraceptive choice. Part II details a robust 7-step decision-making framework designed to guide practitioners and athletes through the complexities of contraceptive selection.
The Regulatory Landscape: WADA and Reproductive Rights
Before diving into clinical selection, it is essential to address the regulatory status of contraceptives. The World Anti-Doping Agency (WADA) does not include hormonal or non-hormonal contraceptives on its prohibited list. While some HCs can theoretically alter hormone levels, they remain permitted to ensure gender equity and protect the essential reproductive health rights of female athletes(3). However, practitioners should note that while HCs are permitted, they must still be declared during doping tests as they can occasionally influence biological passport markers.
A Seven-Step Contraceptive Decision Algorithm
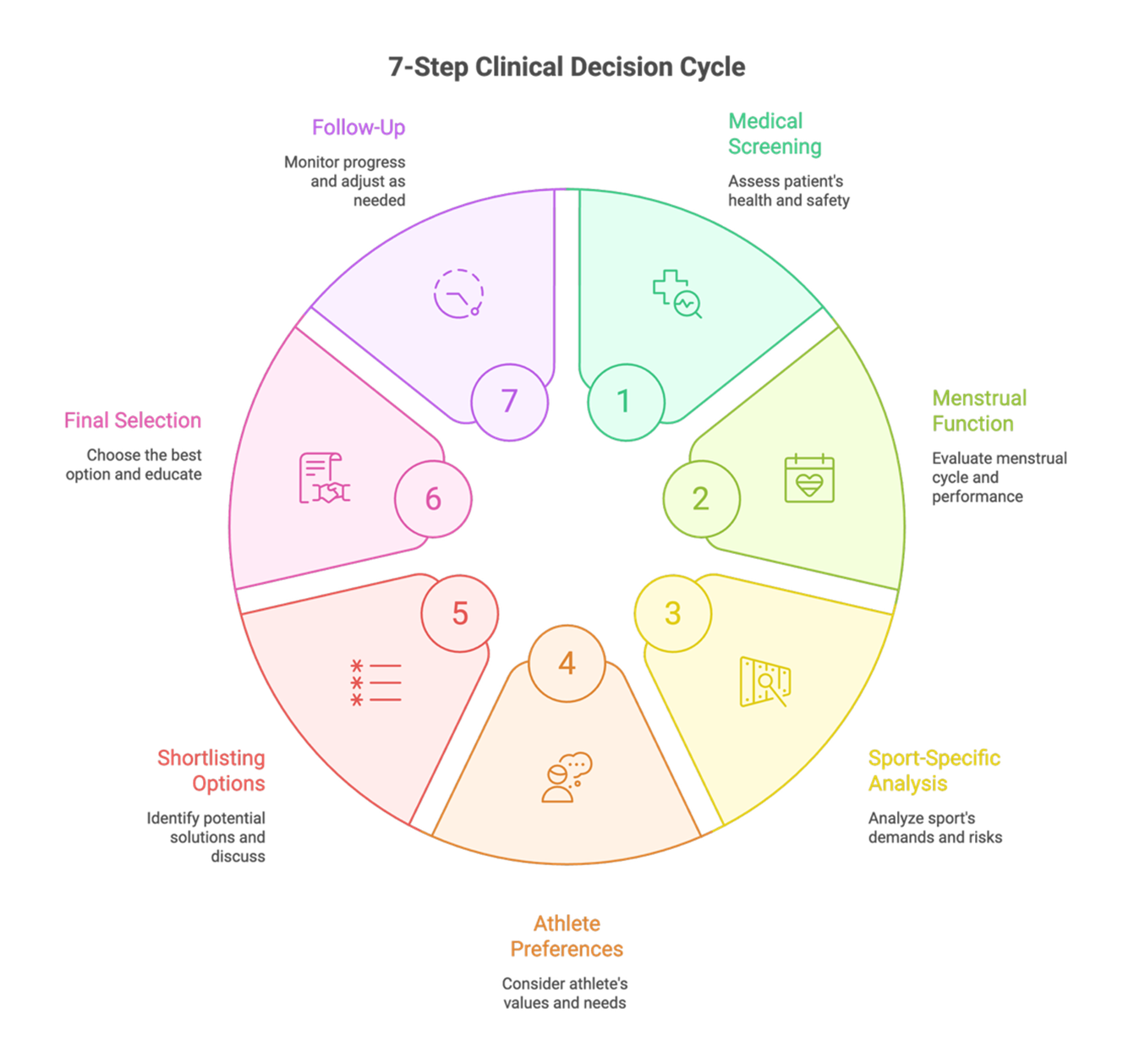
A robust framework must move beyond simple "pill or no pill" discussions (see Figure 1). Instead, it should prioritize individualized, athlete-centered counseling that integrates performance demands with medical safety.
Step One: Medical Screening and Safety
The first priority is ensuring medical eligibility based on the WHO Medical Eligibility Criteria (WHO MEC)(4). Clinicians must rule out absolute contraindications (red flags), particularly for estrogen-containing methods like the combined oral contraceptive pill (COCP), and be cognizant of yellow flags (usually not recommended):
Red flags:
-
Smoking and age: Older than 35 and smokes >15 cigarettes per day.
-
Migraine with aura: Avoid COCP due to increased stroke risk.
-
Cardiovascular/Thromboembolic disease: Avoid COCP due to VTE risk.
-
Current breast cancer: Avoid all hormonal methods.
-
Severe liver disease: Use non-hormonal options.
-
Bone Health Risk: Avoid Depot Medroxyprogesterone Acetate (DMPA) - progestin-only injection- if there is a history of stress fractures or low bone mineral density (BMD), as it can negatively impact bone health.
-
Post major surgery: with prolonged immobilization.
-
Postpartum: <21 days postpartum with other risk factors for VTE (e.g., smoking, obesity, pre-eclampsia).
Yellow flags:
-
Smoking & Age: Smokers aged 35 who smoke <15 cigarettes/day.
-
Blood Pressure: Hypertension (systolic 140–159 or diastolic 90–99 mmHg).
-
Postpartum & Breastfeeding: Six weeks to < six months postpartum.
-
Non-breastfeeding: <21 days postpartum (without other risk factors).
-
Medications: Current use of certain anticonvulsants (phenytoin, carbamazepine, barbiturates, topiramate) or rifampicin/rifabutin.
-
History: Past breast cancer with no recurrence for five years.
-
Diabetes: Diabetes with nephropathy/retinopathy/neuropathy or >20-year duration.
Step Two: Menstrual Function and Performance Requirements
Once safety is established, the practitioner must assess the athlete’s specific physiological needs. This involves a "decision point" regarding the athlete’s goals for their cycle:
-
Monitoring RED-S: Clinicians prefer non-hormonal options (Copper IUD) or low-systemic hormonal methods (LNG-IUD) (which has a local rather than systemic effect) if there is a need to maintain natural cycles to monitor for Relative Energy Deficiency in Sport (RED-S).
-
Symptom Management: For athletes suffering from heavy menstrual bleeding (menorrhagia) or dysmenorrhea that impairs training, the Levonorgestrel IUD (LNG-IUD), COCP, or Progestogen-Only Pill (POP) is an effective choice.
-
Cycle Predictability: Athletes who need to time their cycles around major competitions may prefer the COCP or POP.
-
Total Suppression: Continuous use of the COCP, implants, or DMPA (if bone health is not a concern) can suppress menstruation entirely.
Step Three: Sport-Specific Analysis
The demands of the athlete’s specific discipline play a critical role in method selection:
-
Endurance Sports: These athletes are at high risk for anemia. Practitioners should avoid the Copper IUD if it causes heavy bleeding and instead consider the LNG-IUD, which can reduce bleeding by about 90%, thereby improving iron status and endurance(5).
-
Aesthetic and Weight-Category Sports: In sports like gymnastics or combat sports, weight and fluid retention are critical. Methods that minimize weight fluctuation, such as the LNG-IUD, POP, or Copper IUD, are generally preferred over those that may cause bloating.
-
Contact Sports: Research indicates that IUDs are safe in contact sports like rugby or football, with no evidence of increased displacement risk.
-
Travel-Heavy Athletes: Frequent international travel can make daily pill compliance difficult. For these athletes, Long-Acting Reversible Contraceptives (LARC), such as IUDs or implants, are ideal.
Step Four: Athlete Preferences, Values, and Practicalities
The athlete’s voice is non-negotiable. This step evaluates:
-
Desire to avoid hormones entirely.
-
Comfort level with pelvic procedures (required for IUD insertion).
-
Past experiences with side effects like acne or mood changes.
-
Cultural or religious considerations regarding menstruation and contraception.
Step Five: Shortlisting Options and Shared Decision-Making
The clinician and athlete should collaborate to shortlist two to three evidence-based options. For example, an endurance athlete with heavy bleeding might choose between an LNG-IUD or the COCP. Shared decision-making ensures the athlete feels ownership over the choice, which improves long-term adherence.
Step Six: Final Selection and Comprehensive Education
Upon making a final choice, the athlete must be educated on:
-
Expected side effects and the adjustment period.
-
Interaction with performance markers (recovery, mood, iron status).
-
Masking effects: Education is vital on how hormonal methods can mask the menstrual irregularities associated with RED-S, which could lead to missed warnings of bone stress injuries.
Step Seven: Follow-Up and Monitoring
Contraceptive management is not a one-time event. A three-month follow-up should assess bleeding patterns, mood, and changes in performance. A six-month follow-up should re-evaluate goals, check RED-S and other markers, and review menstrual cycle tracking.
Case study: Elite Rugby Player (Contact Sport)
|
Profile: 27-year-old professional rugby player with a chaotic international match schedule. Clinical Presentation: Suffers from severe dysmenorrhea (painful periods) and PMS that significantly reduces her training intensity. She has a history of poor compliance with daily oral contraceptives due to travel across time zones. Preferences: Wants a long-term, "set and forget" solution but expresses concern about the safety of an IUD during high-impact tackles. |
|
|
Step One - Medical Screening |
No contraindications to hormonal methods (no migraines or VTE risk).
|
|
Step Two - Menstrual/Performance Needs: |
Strong indication to reduce painful periods and PMS to maintain training consistency.
|
|
Step Three - Sport-Specific Factors |
IUDs are safe in contact sports with no increased risk of displacement. LARC is preferred to eliminate the risk of missed doses during travel. |
|
Step Four - Athlete preferences |
The athlete expresses that she is comfortable with the idea of insertion of an IUD in the doctor’s office, but also with injections. |
|
Step Five - Shortlisting options |
Shortlisting options: LNG-IUD or DMPA. |
|
Step Six - Final Selection and Education |
Athlete selects LNG-IUD. The practitioner educated the athlete about possible changes in mood and other side effects associated with progestin-only contraceptives and the process of inserting an IUD.
Rationale: It provides superior management of dysmenorrhea, requires no daily adherence, and is clinically safe for high-impact collisions. |
|
Step Seven - Monitoring |
Encourage the athlete to track symptoms (good and bad) and to follow up after three and six months. |
Key Clinical Takeaways for Practitioners
Implementing this framework requires a shift toward individualized care. Practitioners should remember:
-
The Masking Effect: Be vigilant with athletes in aesthetic or endurance sports, as HCs can hide the amenorrhea that signals low energy availability.
-
Iron Status is Performance: For many female athletes, choosing a contraceptive that reduces bleeding is a direct performance-enhancing intervention through the preservation of iron stores.
-
Flexibility: If an athlete experiences negative mood changes or performance decrements, be prepared to adjust the method. Every athlete’s hormonal profile is unique.
By utilizing this structured decision-making algorithm, sports medicine professionals can ensure that contraceptive choices support both the reproductive health and the gold-medal aspirations of the athletes they serve
References
- PES. 2023;27(1):10-16.
- Sports Med. 2020;50(10):1785-1812.
- Drugs: Education, Prevention and Policy. 2024;31(4):396-402.
- Medical Eligibility Criteria for Contraceptive Use. 6th Edition. World Health Organization; 2025.
- Royal Institute of Philosophy Supplement. 2013;73:129-143.
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.