You are viewing 1 of your 1 free articles
The Language of Pain
Pain and sport often go hand in hand. Karen Litzy explains the best way to communicate with athletes about their pain experience.
2016 - Great Britain’s Johanna Konta receives physio treatment during the second round. Peter Ciboria Livepic
Athletes are told to push through the pain, grin and bear, suck it up, or take one for the team. There are times when this might be appropriate, but for the most part, a complaint of pain from an athlete is just as valid as one from anyone else. If an athlete complains of pain that causes him or her to miss a practice or a competition, then this complaint must be taken seriously.
According to the International Association for the Study of Pain, pain is defined as, “An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage”(1).
This means that one can feel pain with or without actual damage to the tissue of the body. Dr. David Butler further clarifies the perception of pain in the Explain Pain Handbook as, “Pain will occur when your brain concludes that there is more credible evidence of danger related to your body than there is credible evidence of safety related to your body”(2).
In the last 10 to 15 years, treatment paradigms for pain have shifted from a strictly biomedical model of care towards a biopsychosocial model of care. The biomedical model of care focuses on purely biological factors as the main cause of disease. This means that there has to be an ‘issue with the tissues’ for pain to be present. The biopsychosocial model of care includes the biological factors in the biomedical model of illness/pain, but also takes into account psychological (thoughts, emotions, and behaviors) and social (socio-economical, socio-environmental, and cultural) factors as playing a significant role in human functioning in the context of disease and pain. It is important to acknowledge that pain is multifactorial and is more than just “physical”. When working with athletes the psychosocial aspects of pain are real and must be addressed within the medical team.
According to the International Olympic Committee Consensus Statement on Pain Management in Elite Athletes, there are several mechanisms that lead to pain in athletes(3). They are:
- Acute Traumatic Injury: This type of injury occurs to otherwise healthy tissue and results in a compromise of that tissue. This may result in inflammation, bruising and pain in the area of the injury. Because of its traumatic nature this may cause anxiety, fear and uncertainty for the athlete.
- Overuse Injuries: This injury is usually from a repeated motion or adding load to tissues that are not ready to handle that load capacity or to tissues that have not had adequate rest and recovery time. These injuries occur in otherwise healthy tissue or in tissues that are already damaged. This may result in inflammation and pain.
- Subacute recurrent injuries or chronic degenerative conditions: These injuries can be a continuation of an overuse injury or they can be the same injury that occurs in the same site after the athlete has returned to full competitive play.
Each of these injuries can be devastating for an athlete as they can mean time off from sport, time away from their team, or even an end to their athletic career. Therefore, healthcare practitioners need to have honest and evidenced-based conversations with the athlete about their pain and injury. Clearly explain the science behind pain in a way that will resonate with the athlete (according to their health literacy), decrease fear, and allow them to make informed decisions about their return to play.
Talking about pain
The language used to describe pain can make all the difference to an athlete’s perception of their condition, prognosis, and pain. Here are some suggestions to use when talking to injured athletes:
There are no such things pain pathways, pain fibers or pain receptors. Pain is actually the brain’s interpretation of damage or danger within the body(4). Therefore, instead of using those terms when describing pain, replace the word PAIN with DANGER.
- If an athlete has pain with an acute injury, reassure them that this is completely normal. It is the brain’s way of alerting them that something is wrong. Then educate the athlete on their specific injury and the associated healing time. Instruct them that the pain will most likely lessen as the injury heals and the danger to the body decreases. Think of Acute pain as a defender not an offender.
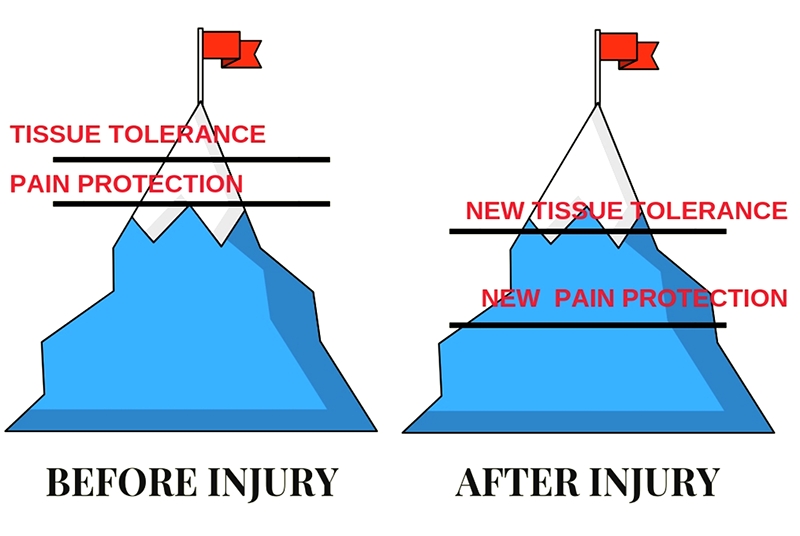
- If the athlete is suffering from chronic pain, the description of what may be happening in the body differs from that of an acute injury. It is important that the athlete understand that there are changes in biological structures that process and integrate danger messages. The nervous system becomes more sensitive in that it may take less of an input or stimulus to generate pain. The athlete may not be causing more tissue damage but instead the system is more sensitive. For this concept, using a graphic like the double mountain peaks (adapted from the book Explain Pain Supercharged) to explain how sensitivity to pain is altered in chronic pain conditions, can be very helpful (see figure 1)(5).
Adapted from Explain Pain Supercharged(5)
The language used when speaking with athletes matters. As mentioned above, an injury to an athlete can be career-ending, and as a result, there is a strong psychological component. Avoid using language that will contribute to fear or catastrophizing. Clinicians should tailor their language when speaking with people in pain (see table 1)(6).
| Questionable wording | Alternative wording |
|---|---|
| Degenerative disc disease | Age-related changes |
| Slipped disc | Transient changes in the structure of the disc |
| Wear and tear | Normal age-related changes |
| Your back is unstable | Your back is strong and robust; you may need more control its movement |
| Bone on bone | Narrowing or tightening |
| You have the (insert body part) of a 90-year-old | Never say this to anyone unless they are over 90 years old! |
| Don’t worry | We will work on this together |
| Your sacrum popped out | May be a strain or sprain in your ligaments. In most adults, sacroiliac joints are fused and don’t actually move. |
Having honest, realistic conversations with athletes about pain and injury is paramount for their health, both now and in the future. In order to have these conversations one must understand the point of view of the athlete. When conducting a thorough subjective interview, be sure to really listen to the athlete. Allow them to tell their full story, including their fears and concerns. Try to go deeper into that story by utilizing motivational interviewing and open-ended questions. Highlight the parts of their story where they are having ‘wins’ both big and small. Highlighting the positives of the story versus only the negatives of the story can help to increase confidence and decrease fear. Finally, allow them to be the best guide for their plan of care.
Treatment
When planning a treatment protocol, regardless of diagnosis, keep in mind some simple dos and don’ts such as those outlined below.
What to do:
- Movement with graded exposure to load;
- Pain education meant to invoke safety and not fear;
- Incorporate activities the patient enjoys;
- Allow the patient to explore movement without too many restrictions;
- Address their sleep and eating habits;
- Be an partner/coach not and operator;
- Create and be part of a multidisciplinary team.
What NOT to do:
- Do not create dependence;
- Do not make the patient think they are fragile;
- Do not take on their recovery as your own;
- Do not over medicalize their diagnosis;
- Do not exclude the patient from the decision making process;
- Do not assume the patient know what is happening with their body.
Professional, student, and weekend athletes all have the same goal: return to play. By carefully choosing the right language and having honest discussions about pain and injury, healthcare practitioners can guide rehabilitation and return athletes to their sport with confidence.
References
- IASP Terminology - IASP. www.iasp-pain.org/terminology?navItemNumber=576#Pain. Accessed January 22, 2019.
- Moseley, G. and Butler, D. (2015). Explain Pain Handbook. Adelaide City West: Noigroup Publications.
- Br J Sports Med. 2017;51:1245-1258.
- Trends in Neurosciences. 9(6): 254-255.
- Mosley, G. and Butler, D. (2017). Explain Pain Supercharged. South Australia: NOI.
- JOSPT. 2018;48(7):519–522
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.