Uncommon injuries: the deltoid ligament
Injuries to the deltoid ligament are an uncommon ligamentous sprain to the ankle. The mechanism of injury occurs due to forced eversion combined with external rotation. They are typically seen in footballers (all types), court sports athletes (netball, basketball, handball), combat sports such as Brazilian JuJitSu, as well as in off-road runners such as trail runners. The signs and symptoms are usually straightforward; however many of these type of injuries are also associated with syndesmosis injuries and ankle fractures. The management of deltoid ligament injury is similar to lateral ankle sprains, however, the rehabilitation period is often protracted.
Anatomy and biomechanics
The gross anatomy of the medial ankle joint and the associated ligamentous structures has been variably defined by several authors(1-11). Some of the confusion exists due to the deltoid ligament being a complex multi-fascicular ligament with deep intra-articular and superficial extra-articular fibres. A comprehensive description of the medial ankle involves the following (see figure 1):- The medial malleolus has two colliculi which are divided by a groove.
- The tibialis posterior tendon (PTT) and flexor digitorum longus (FDL) pass posterior to these colliculi.
- The tibial attachment of the deltoid ligament is to both colliculi and the intercollicular groove.
- Distally, many fibres fan outwards to insert onto the navicular, talus, calcaneus and spring ligament. Its narrow proximal attachment and broad distal attachment gives the ligament a triangular or deltoid shape – hence its name.
- The superficial fibres originate on the anterior colliculus, and cross two joints (tibiotalar and talocalcaneal).
- The deep fibres originate in the groove between and on the posterior colliculus, and only bridges the tibiotalar joint.
- The tendon sheath of the posterior tibial muscle covers the posterior and middle part of the deltoid ligament - in much the same way as the peroneal tendon sheath is associated with the calcaneofibular ligament on the lateral side.
- Historically, other authors have described from three to six differing anatomical divisions (2,3,6-9,12).
Figure 1: Gross anatomy of the medial ankle joint
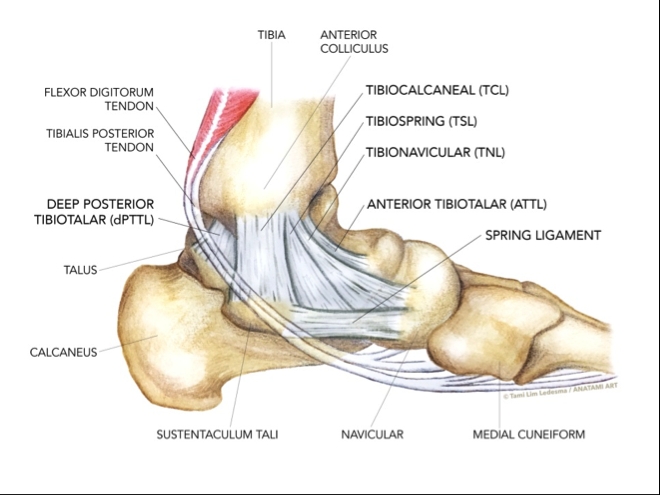
The most commonly accepted description of the deltoid ligament is the one originally proposed by Milner and Soames(4)who describe the six different parts of the deltoid ligament as(3-7,10):
- Tibionavicular (TNL) – superficial. This is sometimes considered to be a thickened portion of the anterior ankle capsule and not a distinct ligament(3). This ligament may not always be visible on an MRI scan(10).
- Tibiospring (TSL) – superficial.
- Tibiocalcaneal (TCL) – superficial. This is a thick ligament.
- Superficial posterior (sPTTL) – superficial. May be absent.
- Deep posterior (dPTTL) – deep. This is quite a thick and prominent ligament(7).
- Anterior tibiotalar (ATTL) – deep. May sometimes be absent(10).
Deltoid ligament functions
The primary functions of the deltoid ligament are as follows(13-15):- To provide medial stability to the tibiotalar joint by providing a firm fixation between the tibia and talus.
- To prevent the talus shifting into a valgus position, or to move anterolaterally, or to externally rotate.
- To transfer force between the tibia and tarsus.
- The broad insertion of the superficial deltoid ligament on the spring ligament also plays a key role in the stabilising function of the medial ligaments.
- The superficial layers of the deltoid ligament particularly limit the talar abduction, while the deep layers limit the external rotation(2).
- To pevent the talus shifting more than 2mm laterally, even if the lateral structures are not in place(2,16-18).
- The ATTL together with the anterior talofibular ligament (ATFL) on the lateral side is thought to restrict forward translation of the talus(18).
- The posterior tibiotalar ligament (PTTL) restricts internal rotation of the talus solely by means of its deep fibres(19).
- This spring ligament complex supports the talar head medially and stabilises the entire talocalcaneonavicular joint.
The following points are also relevant to function:
- Both deep and superficial layers are equally effective in limiting pronation of the talus. Therefore, the main causes of isolated deltoid ligament lesions are pronation or external rotation movements of the hindfoot.
- Sequential cutting of the superficial ligament still results in ankle stability, however gross instability of the ankle develops if the deep fibres are surgically cut(18).
- The deep PTTL appears to be the strongest ligament followed by the TSL.
- The TCL and TNL are weaker than the TSL(18).
- There is interlacing of the TSL and the TNL.
Injury pathology
Injuries to the deltoid ligament are reasonably uncommon. It has been estimated that isolated injuries account for about 3–4 % of all ankle ligament injuries(20). Severe deltoid sprains are often associated with fibular or lateral malleolar fractures, and other injuries. Large tears and ruptures affecting both layers are almost always associated with other injuries such as high-ankle sprains, lateral malleolar fractures, lateral sprains, or high fibular fractures. The tibialis posterior, flexor hallucis longus, and saphenous nerves may also be injured.As the deltoid ligament is an important medial structure that plays a role in preventing ankle eversion and some degree of external rotation of the foot, the position of the foot appears to have a role in injuries sustained during sprains. Damage to the deltoid ligament is believed to be a result of an external rotation force to the foot as the foot is everted.
Interestingly, one cadaveric study showed that external rotation may be the key movement that damages the deltoid ligament. It was found that external rotation force in a neutral (not everted) foot with the ankle in dorsiflexion was more likely to result in deltoid ligament injury. A similar force is likely to damage the syndesmosis in the everted foot(21). Furthermore, the deltoid ligament may also be injured along with lateral ankle ligaments in the classic inversion ankle sprain mechanisms.
Other noteworthy studies on injury pathology include the following:
- Schäfer and Hintermann (1996) found that during anterior ankle arthroscopy in 110 patients with chronic instability of the ankle joint, concomitant lesions of the deltoid ligament were found in 23 ankles(22).
- In a retrospective review of 47 ankles with chronic lateral ankle instability and no medial ankle pain, deltoid ligament injuries were observed in 72% of all ankles. Superficial deltoid injury was seen in eleven ankles, four ankles had a deep deltoid injury, and 20 ankles had both components of the deltoid ligament injured(23).
- In a subgroup of patients with MRI evidence of lateral ligament injury, the incidence of deltoid injury was 35%(24).
- Hinterman et al (2002) performed arthroscopic evaluation of 148 chronically unstable ankles and found the incidence of deltoid injury to be about 40%. All of these patients had damage to the lateral ligament complex(25). About one third of these patients reported symptoms on the medial aspect of the foot or ankle.
Signs and symptoms
The diagnosis of a medial ankle ligament injury is based on the typical mechanism of injury and particular clinical findings. Some of the key points clinicians should note are:- Patients with an acute injury of the deltoid ligament usually complain of pain in the anteromedial part of the ankle joint.
- A hallmark in diagnosis is the tenderness at the medial gutter of the ankle joint(13).
- Patients usually give a history of either an eversion-pronation trauma, or a supination-external-rotation trauma.
- Clinically the patient may present with a flatfoot, with prominence of the medial malleolus, pronounced hindfoot valgus and pronation of the affected foot.
- Ecchymosis and tenderness along the deltoid ligament are present.
- In contrast to patients with a tibialis posterior tendon dysfunction, the patient will be able to actively correct the hindfoot valgus deformity and perform a single heel rise.
- In patients with chronic medial ligament instability, accurate diagnosis may be more demanding. These patients usually report a medial ‘giving-way’, especially while walking down a hill or stairs. The chronic versions will present with anteromedial recurrent swelling and painful tenderness. Patients will also develop a chronic rotational instability, with increasing valgus malalignment and consecutive pain on the lateral aspect of the ankle joint.
- The anterior drawer test and the talar tilt test may be positive.
- Pain is reproduced on passive testing into external rotation and eversion.
Radiography and deltoid ligament injuries
Standard radiographs are used to exclude fractures after acute trauma. In chronic medial ankle instability, standard weight-bearing radiographs are taken to assess segmental deformities in all three planes. A Saltzmann view is usually used to view rearfoot alignment.MRI may help to identify a weakening or avulsion of the medial malleolus, osteochondral lesions, damage to the spring ligament and the tibialis posterior/flexor hallucis longus/flexor digitorum longus tendons.
However, MRI has been shown to be less reliable in detecting ligamentous deficits compared to arthroscopic assessment(26). Furthermore, MRI has also been shown to be unhelpful for determining whether operative or conservative treatment of the common SER-type ankle fractures is necessary(13).
In the case of chronic medial ankle instability, there are different classification systems based on clinical assessment, arthroscopic assessment, or intraoperative surgical findings. It is beyond the scope of this paper to provide an in-depth discussion on chronic medial ankle instability. The interested reader is directed to references 1, 13 and 22 at the end of this article.
Management
Management of deltoid sprains depends largely on whether the there is a partial tear (usually involving just the superficial section of the ligament), a complete tear (which includes the deep portion leading to instability), or whether there are concomitant injuries. Severe deltoid ligament injuries are most often associated with fracture of the tibia and/or fibula.As these will require surgical intervention, often the deltoid ligament may be repaired concurrently. Therefore, these serious types of deltoid injuries will not be discussed. Furthermore, surgical reconstruction should be considered in combined injuries of the deltoid ligament and the spring ligament, with or without involvement of the tibialis posterior tendon. Isolated deltoid sprains without fracture are rare and so there is little research evidence to guide management. Deltoid sprains which involve only the superficial portion and which are rotationally stable are thought to have a good prognosis and can be treated non-operatively.
Immediate treatment
- Immobilise with a boot and avoid full weight bearing for the initial 5-7 days. If touch or partial weight bearing is painful, the patient will require crutches.
- Ice the ankle in an ice bucket with as much dorsiflexion as is comfortable. This can be done for 20-minute sessions every few hours in the first few days.
- Compress and elevate the ankle in between icing sessions.
- No NSAIDs in the first four days.
In terms of optimal early loading, consider the following:
- Light Theraband exercises can be used to strengthen into inversion and internal rotation starting from a neutral foot position. Full eversion and external rotation movements are to be avoided.
- If the patient can tolerate it, they may be also able to perform double-leg calf raises starting in slight plantarflexion. In plantarflexion, the medial ankle muscle complex will contract to create an arch and invert the calcaneus. In this position the deltoid ligament will be protected from any tensile stress.
- If available, deep-water running can be performed with the ankle taped (to protect an eversion and external rotation force - see below).
- When the boot is removed and the client can comfortably mobilise pain free, running on an Alter-G treadmill (see figure 2) at 60% bodyweight can commence, with the foot and ankle taped to prevent pronation and eversion. This Alter G running needs to be performed as intervals – for example, 30 seconds on with 30 seconds rest. The speed can be chosen based on comfort. The level of bodyweight can be increased gradually from one session to the next. To allow adequate recovery between sessions, the Alter G running should be performed not daily, but every second day.
- Once the athlete reaches 90% bodyweight, then ground-based running may be commenced. If an Alter G is treadmill unavailable, the athlete can be progressed through stages of water running or underwater treadmill running. If Alter G and pool running is unavailable, it would be safe to have an athlete mobilising pain free in walking for a week before ground based running would commence.
For the athlete with a more severe isolated deltoid sprain (particularly the deep fibres), early stress by returning to too soon may lead to the ligament healing in a stretched position, contributing to instability. In this instance, the client may be immobilised in a boot for four weeks, then perform comfortable walking for two weeks prior to return to running. Return to light training should be delayed to about 6-8 weeks. This is particularly the case in patients where the spring ligament has also been injured.
Figure 2: Alter-G treadmill

Return to sport
The athlete can return to sport if they have met the following exit criteria:- Medial ankle swelling is controlled, and does not increase after loading sessions.
- The athlete has completed 2-3 full match-like training sessions with high speed metres, total volume and acceleration/deceleration efforts with hard changes of direction.
- Achieves 90% or greater on a crossover hop test.
Key points about a return to running program
- Always have the athlete taped to protect the ankle from excessive pronation and eversion forces. Below is an image of a combination of an anti-pronation tape (‘Low Dye’) and an anti-eversion taping.
Low-dye technique showing anti-pronation tape around the arch

Low-dye technique – finish

Anti-inversion taping superimposed on low dye technique
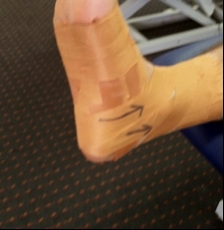
- Low-grade injuries such as superficial deltoid or minor deep deltoid ligament injuries would usually be protected for a period of time in a boot (discussed above) and then either progressed through Alter G or pool running prior to ground-based running. Based on this recommendation, ground running would commence at the earliest around 10-14 days post injury. More severe injuries would start running at six weeks post injury.
- The usual progressions would be;
- Straight-line running, building to 75% of full speed over a few sessions.
- Fartlek and interval running for conditioning, with a gradual progression in volume (speed capped to 75%).
- Start gentle ‘S’ runs, side shuffle movements and stepping movements. These are progressed slowly and comfortably so this also reaches 75% intensity. This will be concurrently done with (b) above.
- Build speed efforts to 100% with acceleration and deceleration distances gradually shortened over a few sessions – eg (in metres): 30/20/30 →20/20/20 →10/20/10.
- Once full speed is reached, the next criteria is to progress hard change of direction with rapid acceleration and deceleration movements.
- In footballers, long kicking of the ball is usually left until after all running stages are completed, as long kicking can place a large eversion and external rotation stress on the ankle.
- Running can be performed daily if the athlete does not react from one session to the next.
Conclusion
Deltoid ligament sprains are not a common injury to the ankle. If they do occur, even the mild strains of the superficial deltoid ligament will take longer to rehabilitate than mild injuries on the lateral aspect of the ankle. Higher grade injuries that involve the deep deltoid ligament will most likely result in a much longer convalescence period. More severe injuries are usually associated with more severe pathology such as malleolar fracture and/or syndesmosis injury.Due to the natural tendency for the ankle and foot to pronate and evert during loaded movements such as running and landing, early return to sport in an unhealed ligament complex may lead to over-stretching of the deltoid ligament, which may then progress to pathological chronic instability of the medial ankle. Therefore, the clinician is advised to move slowly in rehabilitation with the more significant injuries that involve the deep deltoid ligament.
References
- Foot Ankle Clin. 2003;8(4):723–38
- J Bone Joint Surg Am. 1956;38-A(4):761–81
- Foot Ankle Int. 2002; 23(6): 547-553
- Foot Ankle Int, 1998. 19:757–760
- Knee Surg Sports Traumatol Arthrosc. 2010; 18:557–569
- Foot Ankle; 1987. 8:19–22
- Am J Roentgenol, 1994; 162(2):377–383
- Acta Orthop Scand, 1979; 50:217–223
- Strat Traum Limb Recon, 2012; 7:73–85
- Radiology, 2007; 242(3):817–824
- Sarrafian SK (1993) Anatomy of the foot and ankle. Descriptive, topographic, functional, 2nd edn. Lippincott, Philadelphia, pp 159–217
- Radiology, 1992; 184(2):499–506
- American J of Sports Med, 2004; 32(1); 183-190
- Foot Ankle Int; 1999; 20(11):733–737
- Med Sci Sports Exerc, 1999; 31:459–469
- Acta Orthop Scand, 1960; 263:1–88
- Arch Surg, 1950 60:957–985
- Acta Orthop Scand, 1985; 56:1–75
- J Trauma; 1979. 19:266–269
- Foot Ankle Clin. 2013;18(2):255–91
- J Orthop Res. 2012; 30:1423-1429
- Knee Surg Sports Traumatol Arthrosc.1996;4(1):48-52
- Foot Ankle International. 2011; 32(9); 873-878
- Khor and Tan (2013). The Anatomic Pattern of Injuries in Acute Inversion Ankle Sprains; A Magnetic Resonance Imaging Study. Orthopedic Journal of Sports Medicine.
- Am J Sports Med; 30(3); 402-409.
- Skelet Radiol. 2012;41(7):787–801
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









