Lumbar spondylolysis in adolescent athletes: breaking the curse!

Spondylolysis is a fracture at the pars interarticularis of a vertebra. In the general population, the incidence of spondylolysis as a cause of low back pain is around 6% in adults and 4.4% in the paediatric population(1). However, in adolescent athletes, the occurrence of spondylolysis may be as as high as 47-55% in those with low back pain(2,3). Early diagnosis is important to prevent non-union which has been associated with an increased incidence of spondylolisthesis(3). Moreover, earlier recognition of acute spondylolysis is associated with improved fracture healing (3).
Pathology
The pars interarticularis is a small isthmus of bone between the superior and inferior articular facets of spinal vertebra (see figure 1)(4). The fracture can be unilateral or bilateral, and although any spinal level may be affected, 71% to 95% of lesions occur at L5, and 5% to 23% at L4(5,6). The likely cause is a stress reaction, which occurs as a result of high loads combined with compression, extension, or rotation movements(7). Spondylolysis commonly occurs in sports involving these movements - for example gymnastics, cricket, tennis, golf, football, hockey, athletics, swimming, and basketball(3,8-11). The injury starts as a stress fracture and, if appropriate management is not administered, can develop into a full fracture, non-union, and eventually a spondylolythesis(3,5). The simplest classification (see table 1) divides individuals into developmental or acquired spondylolysis (5,12).Figure 1: Location of the pars interarticularis
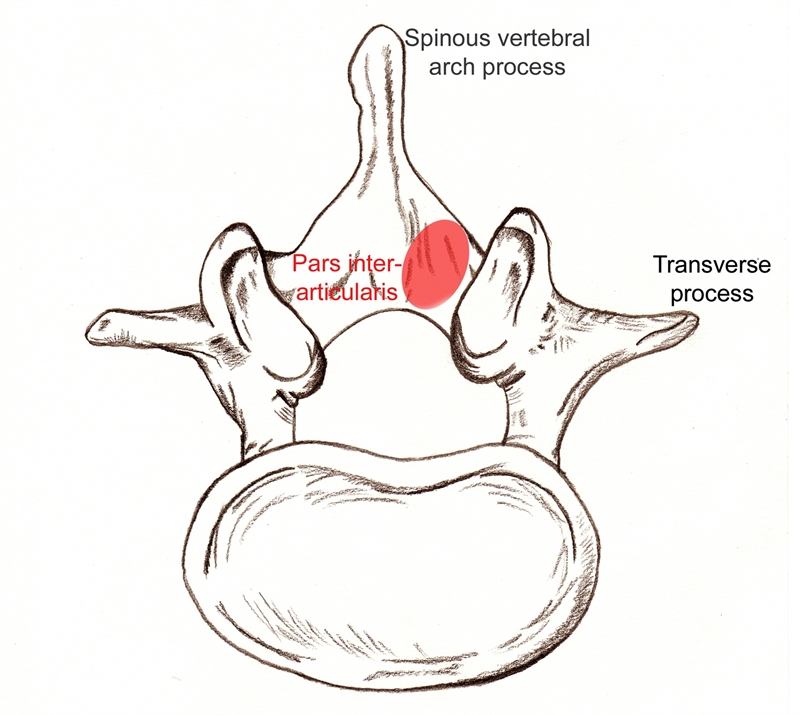
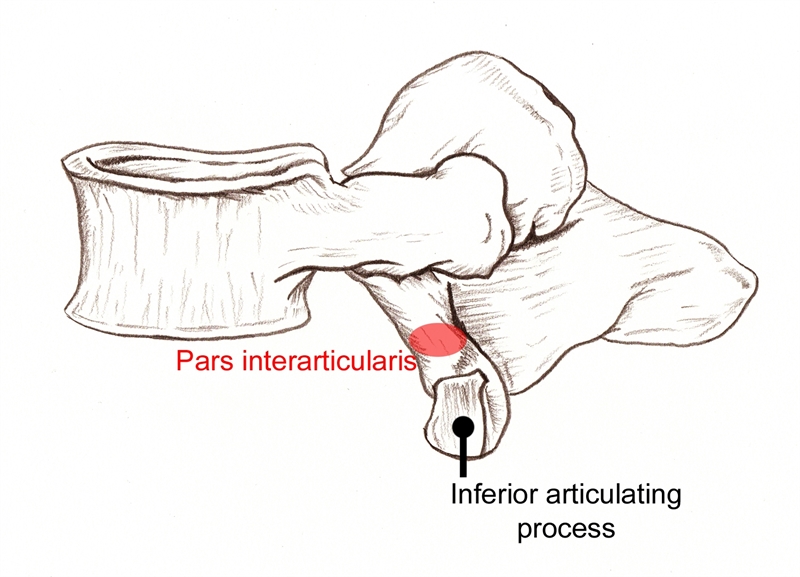
| Developmental | Acquired |
|---|---|
| * A genetic predisposition to failure of the pars interarticularis.* Ossification occurs from anterior to posterior and can become incomplete.* The isthmus arch may be thinner and elongated and therefore more exposed to load. | * Acute or repetitive trauma* Acute trauma occurs with a sudden incident, e.g. collision or fall.* Repetitive trauma occurs with repeated hyperextension or rotational activities combined with compression. |
Risk factors
Due to the sacral angle, the inferior facet of L5 faces anteriorly while the superior facet of S1 faces posteriorly. This means that during the motions indicated, under heavily loaded conditions, a large anterior shear force is created on the L5 pars interarticularis. In young athletes, the spine is still undergoing growth and remodelling, with full bony maturation of the pars interarticularis not occurring until the age of 25(6). The anterior shear, along with bony immaturity of adolescence, contribute to the high rate of spondylolysis in the adolescent population(5).The rate of growth and maturation varies from child to child, which results in significant differences in size, strength, and skeletal maturity among children of the same chronological age(12). Children between 6 and 10 years of age, on average, grow about 5 to 8 cm per year and gain about 2 to 3 kg per year. This increases further still in adolescence where weight gain occurs during the maximal growth in height. Girls gain about 7kg in fat-free mass, whereas boys gain about twice this amount(12). For these physiological reasons, not all athletes will tolerate the same volume of training. Therefore, volume of training should be monitored.
Individuals who stand with an excessive anterior pelvic tilt increase the anterior shear forces at the L5 level, thus increasing the risk for spondylolysis at L5(5). Additional findings in adolescents who commonly present with this baseline posture include:(5,6,8,10-12:
- Lower abdominal weakness
- Hip flexor, hamstring and thoracolumbar fascial hypertonicity
- Increased femoral anteversion
- Genu recurvatum, and increased thoracic kyphosis)
- Reduced hip-lumbar and thoracolumbar dissociation
These are areas that should be targeted within the conservative management plan (see below).
Presentation
Given the high incidence of pathology, early diagnosis ensures appropriate management and improves healing success rates (3). Early diagnosis also calms expectations and helps to focus recovery on effective ways to return the athlete to pre-injury levels of activity (13). Therefore, all complaints of back pain in an adolescent athlete require a thorough history and physical examination (see table 2) (12).| History | Physical presentation |
|---|---|
| - Insidious but can be acute onset of extension-related pain.- Pain with impact — running/jumping.- Pain with extension-type activities — tennis serving, bowling in cricket, golf swing, above-head catching, throwing-in football.- Pain improves with rest.- Pain can be dull or sharp.- Pain can refer to buttock or thigh, but not likely to have radicular signs. | - Hyperlordosis.- Hypertonicity in hamstrings and hip flexors.- Paraspinal spasm unilaterally or bilaterally.- Hypermobile in lumbar spine.- Reduced hip-lumbar and thoracolumbar dissociation.- Focal tenderness on palpation. |
Investigations
The single-leg hyperextension test has been used as a useful clinical tool to detect acute spondylolysis(5). However, solid evidence now suggests this to be neither a specific nor reliable method of diagnoses(3). Most other clinical tests also fail to distinguish between spondylolysis and other causes of lower back pain(14).Instead, radiological visualization in conjunction with the patient’s history is critical for diagnosis(3). Magnetic resonance imaging (MRI) has many useful advantages including being non-invasive, and with an absence of ionizing radiation. However, the use of MRI for first-line investigation has shown a significant number of false-negative scans(1,3). The current gold standard for investigating spondylolysis is bone scintigraphy with SPECT (single photon emission computed tomography). This should be complimented with thin-sliced reverse-gantry axial computed tomography (CT) if bone scintigraphy is positive(3).
Conservative treatment
Adolescent athletes return to play 92.2% of the time with nonoperative management. This compares with 90.3% return to play following surgery(13). Conservative treatment consists of activity restriction, rest and physiotherapy, with or without bracing(13). Most young athletes recover simply with rest from sports activity for three months, followed by a graded return to sport(8,12,15). Athletes who rest for three months are 16 times more likely to have an excellent result compared with those who don’t(15). Interestingly, bony healing on radiographs does not necessarily correlate with clinical outcome(15). In fact, some individuals with spondylolysis present without symptoms(5).Some studies recommend thoracolumbar bracing to limit extension and rotation of the spine(10). However, since there is limited evidence that supports the effectiveness of bracing over isolated rest, this practice remains highly controversial(12). Rehabilitation exercises, during the hiatus from sport, should focus on the following:
- Improving trunk and pelvic stabilisation
- Reducing lordosis
- Improving hamstring and hip flexor flexibility
- Building abdominal and hip abduction strength
- Increasing thoracolumbar spine and trunk mobility(5,8,9,12)
The 4-stage model
A specific 4-stage model of reconditioning, proposed originally for young golfers, provides a structured guideline for rehabilitation of all athletes during the 12 weeks of rest from sport(11).- Acute Phase
Goals: Establish hip-lumbar and thoracolumbar dissociation. Ensure hip mobility. Improve lumbo-pelvic control.

Dynamic hamstring/ neural mobility

Dynamic anterior hip/ rectus femoris mobility

Dynamic thoraco-lumbar dissociation. Aiming to move from thoracic only.
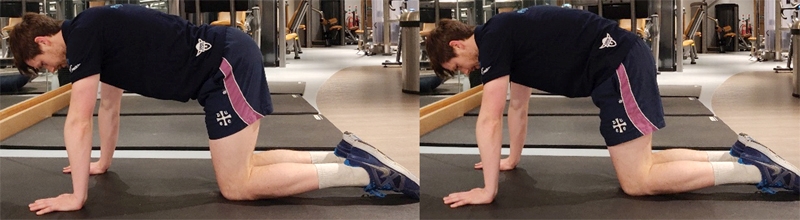
Dynamic lumbo-pelvic dissociation using anterior/posterior tilt at pelvis only.
- Sub-acute/load-introduction
Goals: Increase stability challenges (anti-extension, anti-rotation, and anti-lateral flexion tasks). Introduction of general strength training.

Examples of stability challenge and general strength training exercises (split stance, pallof press, body weight split squat, and dead bug)
- Reconditioning
Goals: Progression of strength training (self-directed – 2 reps in reserve), 5 rep max (RM) training load. Increased trunk stiffness.
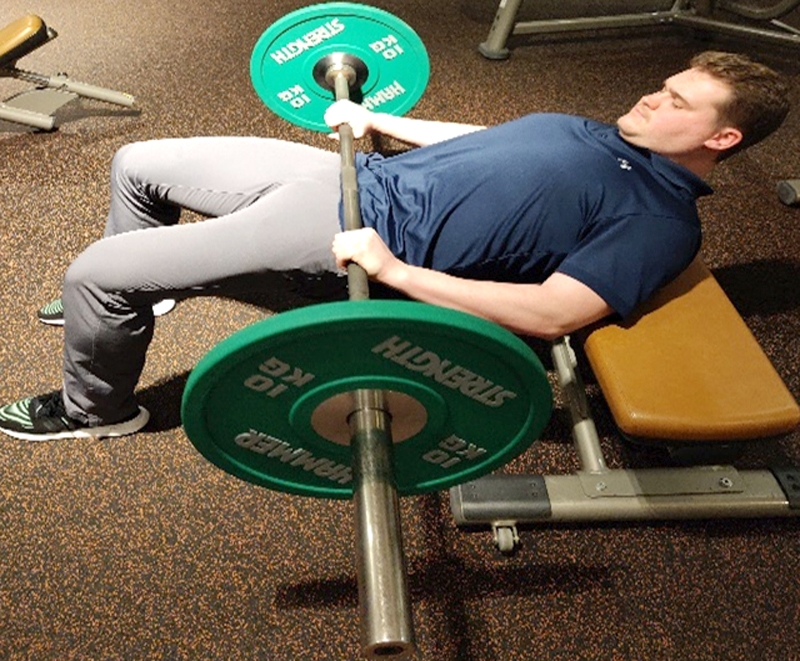
Barbell hip thruster. Keeping lumbar spine control.

Trapbar deadlift.

Short distance med-ball throws for functional trunk stiffness development(16). Avoid lumbar extension.

Weighted sled push for functional trunk stiffness development (16).
- Return-to-play
Goals: Graded return to sports-specific activity following 3 months of cessation.
Surgical intervention
Surgical intervention in young athletes should be reserved only for those who fail a lengthy dedicated course of activity restriction and rehabilitation(13). The medical consensus favours fixation methods utilising wires, hooks, and pedicle screw instrumentation(13).References
- Yamaguchi Jr et al (2012). J Child Orthop. 6: 237-240
- Micheli & Wood (1995). Arch Pediatr Adolesc Med. 149(1) :15-18
- Masci et al. (2006). Br J Sports Med. 40: 940-946
- Morita et al. (1995). J Bone Joint Surg. 77: 620–5.
- Lawrence et al. (2016). Phys Th in Sport. 20: 56-60
- McCleary & Congeni (2007). Curr Sports Med Reports. 6(1): 62-66
- Chosa et al. (2004). J Ortho Research. 22: 158-163
- Donaldson (2014). Sports Health. 6(4): 356-359
- Robinson et al. (2018). Br J Sports Med. 0: 1-6
- Ruiz-Cotorro et al (2006). Br J Sports Med. 40: 441-446
- Brearley et al. (2018). UKSCA conference Milton Keynes.
- Purcell & Micheli (2009). Sports Health. 1(3): 212-222
- Overley et al. (2018). Global Spine J. 8(2): 190-197
- Sundell et al. (2013). Int J Sports Med. 34(3): 263-267
- Rassi et al. (2013). Am J Phys Med & Rehab. 92(12): 1070-1074
- Spencer et al. (2016). J Athletic Training. 51(8): 613-628
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









