You are viewing 1 of your 1 free articles
Pronator Teres: The Carpal Tunnel Pretender
Pronator trees syndrome is a relatively ’uncommon injury’. In his continuing series, Chris Mallac describes the anatomy and biomechanics of this condition, provides diagnostic guidelines, and shares ideas on how clinicians can manage athletes with this ’uncommon injury’.
Entrapment of the median nerve (MN) between the two heads of the pronator teres muscle (PTM) can lead to pain and functional disability in the arm and hand, and can lead to referred pain and neurological symptoms in the hand. This is known as Pronator teres syndrome (PTS). It is an uncommon condition suffered by athletes whose sports require strong grip in positions of forearm pronation – for example tennis players, rowers, bodybuilders and baseball batters. Its symptoms can mimic the more common carpal tunnel syndrome (CTS).
Anatomy and biomechanics
The PTM is attached proximally by two heads(1):
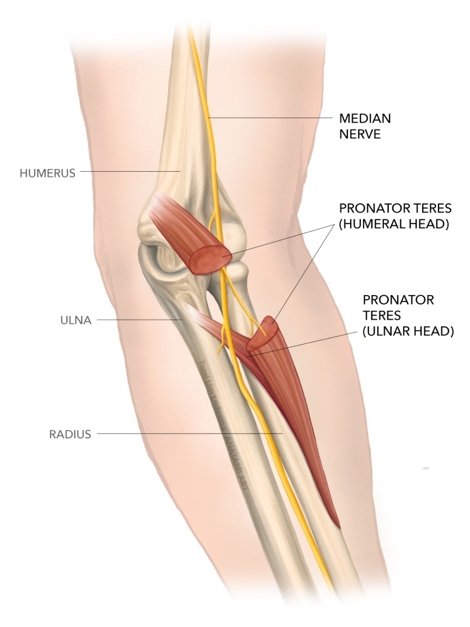
- The humeral head attaches proximal to the medial epicondyle, and to the adjacent fascia or the medial intermuscular septum of the arm.
- The ulnar head attaches to the medial side of the coronoid process of the ulna. The ulna head is more tendinous and may result in greater tension, which may compress the MN.
Both heads run diagonally downwards and merge to form a common flexor tendon, which inserts at the middle of the lateral surface of the radius (see figure 1). The MN enters the forearm from the cubital fossa between these two heads; the space between the two heads is called the pronator canal(2,3). The passage of the nerve has some variation - e.g. passing through the ulna head or passing beneath both heads between the PTM and the flexor digitorum profundus(3,4).
Near its passage through the PTM, the MN sends branches to the elbow joint, pronator teres, flexor carpi radialis, flexor pollicis longus, and flexor digitorum sublimis. It then gives rise to the anterior interosseous nerve (AIN), which usually supplies the flexor pollicis longus, flexor digitorum profundus, and pronator quadratus. This nerve is on the anterior aspect of the interosseous membrane in the forearm.
The main trunk of the MN courses in the forearm deep to the flexor digitorum sublimes, and at the wrist, gives off a sensory branch to the thenar eminence, which passes superficially to the flexor retinaculum. Hence, it is not involved in the carpal tunnel syndrome. The nerve continues into the hand supplying the first two lumbricales and all the thenar muscles - except the adductor pollicis(5). The primary role of this muscle is forceful pronation of the forearm and it may assist the elbow flexors in flexing the elbow via the humeral head that crosses the elbow joint.
Patho-etiology
In 1951, Seyffarth described a group of seventeen patients with symptoms that he considered to be caused by compression of the MN in its course through the PTM(6). In the first patients with PTS to be treated surgically, an anomalous fibrous band that compressed the MN was identified and cut. Since then, the syndrome has been recognised with increasing frequency.
PTS is the second most common cause of MN compression behind carpal tunnel syndrome (CTS). The MN may be entrapped or compressed by several structures in the arm including the PTM at the pronator canal(1,7,8). Others entrapment sites include the flexor digitorum superficialis arch, the lacertus fibrosis (bicipital aponeurosis), and ligament of Struthers and bony structures (supracondylar process of the humerus)(1,9).
Most often, the MN is compressed as it passes between the humeral and ulnar heads of the PTM with hypertrophy of this muscle. The risk of MN compression significantly increases in cases where the ulnar veins pass through the pronator canal with the MN. When the nerve is compressed between the PTM, the cause is most often due to hypertrophy of this muscle due to overuse involving strong and repetitive wrist/finger flexion with pronation of the forearm. This may mimic the pathophysiology of compartment syndromes in other muscle groups(9). As the muscle becomes enlarged and compresses the nerve, the conduction from the MN is diminished. This results in paresthesias in the median nerve distribution (lateral arm and hand) distal to the site of compression.
PTS must be distinguished from other conditions such as cervical radiculopathy, thoracic outlet syndrome, brachial plexus neuritis, overuse of the muscles of the forearm, and carpal tunnel syndrome (CTS). Ashehgan et al tried to determine the prevalence of PTS among patients with CTS(10). They compared clinical findings with the results of electrodiagnostic studies and performed sonographic assessments for the patients with the two syndromes. The study showed that PTS should be considered as a possibility among patients with CTS, and that the association is stronger for severe CTS. Furthermore, many previous reports have showed that multiple cases of PTS were misdiagnosed as CTS or other pathologies(11).
Diagnosis
The common signs and symptoms suffered by an athlete with PTS include(9,11,12):
- Aching discomfort (39%) and weakness (49%) of the muscles of the anterior forearm, worsened by cyclic stress and overuse.
- The symptoms may be insidious in onset or can occur following a sudden increase in use of pronation, usually involving sports that need strong grip and pronation movements (cricket, tennis, rowing, bodybuilding).
- Numbness (58% of cases) and paresthesia (25%) in the MN distribution and palmer cutaneous branch in the hand. This is usually more evident in the thumb and 1stfinger and palm of the hand.
- The pain can be exacerbated by strong contraction of the muscle in pronation and/or passive supination of the wrist.
- Thenar muscle atrophy.
- Low incidence of symptoms at night and upon awakening (2%). This is atypical in CTS, and thus can be used as a clinical differential diagnosis.
- Direct palpation compression of the PTM resulting in tenderness and symptom reproduction (12%). This is most evident in the proximal part of the muscle. The muscle may also indent on compression indicating a compartment syndrome type phenomenon.
- Positive ‘Tinel sign’ at the proximal part of the PTM (7%).
- Electromyographic studies of muscles innervated by the MN are considered mildly reliable. This may show decreased motor conduction velocity, spontaneous muscular fibrillation, and decreased maximal volitional activity on the muscles innervated by the MN.
- Nerve conduction velocity (NCV) or amplitude of the MN may decrease in the forearm, but distal sensory and motor latencies are normal, except when there is an associated CTS(12,13).
Ultrasound has been used to investigate the condition of PTS. The position of the MN between the two heads of the PTM can be seen during dynamic pronation of the forearm. The cross section of the nerve before, after, and at the site of crossing the PTM can also be assessed. Any noticeable reduction in cross-sectional diameter along with decrease in the nerve mobility throughout flexion, supination, and pronation is the criteria for entrapment of the MN.
In addition, any sign of fusiform enlargement and flattening of the nerve can be investigated(10). Furthermore, MRI may show a typical pattern of muscle denervation, and this is a key for the diagnosis of PTS. Also, on MR imaging, patient lesions show abnormally high-signal intensity on T2-weighed fat-suppressed images(12). Finally, injections of procaine hydrochloride into the PTM may be used as a diagnostic block to evaluate the cessation of symptoms that would indicate a positive PTS(9, 14).
Differential diagnosis
Typically, PTS can be differentiated from CTS by the following(4):
- Pain at proximal forearm.
- Numbness at thenar eminence, which iss innervated by the palmar cutaneous branch of the median nerve.
- Weakness of extrinsic muscles including pronator quadratus, flexor pollicis longus, and flexor digitorum profundus (FDP) of index and middle finger.
- Lack of nocturnal symptoms.
- Symptoms aggravated by pronation activity.
Management
Positive results are usually seen with conservative management of PTS, which should always be attempted prior to any surgical interventions. It has been suggested that a conservative period of three to six months is needed prior to surgical intervention and 50-70% will improve with conservative treatment(9).
Conservative treatment involves the following:
- Relative rest from the provoking activity.
- Stretching of the pronator teres (see figure 2).
- Nerve flossing techniques for the median nerve.
- Strengthening of the supination muscles (see figure 3).
- Modified sport/recreation.
Hold a weight (5-10kg) in the hand with the elbow bent. Position the weight so that the majority of the weight is towards the thumb side. This position will force the forearm into a position of supination and stretch in particular the short ulnar head of the pronator teres. Hold each stretch for 30 seconds and repeat five times.
For the imbalances between the PTM and supinator, direct supination strength work needs to be undertaken:
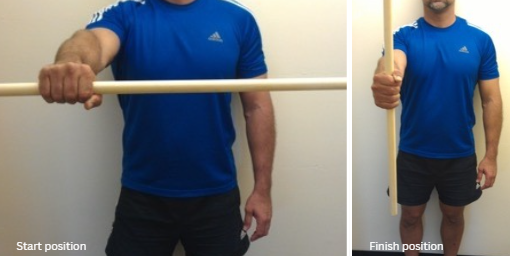
- Hold a hammer or a weighted stick on one hand.
- Keep the elbow extended and allow the weighted end to drop the arm into pronation (this works the supinator eccentrically).
- Return the hammer or stick back to the vertical position (this works the supinator concentrically).
- Perform three sets of 15 reps.
Cortisone injections can be attempted if conservative treatment is deemed not successful; injections are most typically performed in and around the nerve entrapment site. Surgery is the next option if neither conservative treatment nor injections improve the patient’s symptoms. The decision to have surgery may be determined as early as eight weeks or as long as six months after initiating conservative treatment. The overall result of pronator decompression from multiple studies indicates that 22– 92% of patients will have a complete recovery, 21–68% a partial recovery, and only 9–23% will experience no improvement(14).
The usual surgical procedure is decompression of the nerve entrapment via an anterior approach. Anatomical variants such as a supracondylar process (ligament of Struthers) can also be investigated and decompressed if required. The incision is made just above or at the elbow crease,and extended to the mid-forearm using a classic lazy S-incision, modified two longitudinal incisions, single transverse incision, or mini-oblique incision(14). Surgery usually involves decompressing all possible sites of entrapment as often it is difficult to completely differentiate where the nerve is being entrapped. In instances such as high-level athletes, careful identification of the site of entrapment is performed and only that site is decompressed.
Summary
PTS is a rare and often misdiagnosed condition in athletes who use repeat pronation movements in positions requiring grip strength. In this condition, hypertrophy of this muscle can lead to entrapment of the MN and give rise to symptoms similar to CTS. Management is usually first attempted conservatively and if this fails, reasonable success can be sought with decompression surgery.
References
- Rom J Morphol Embryol, 2015. 56(3):1127–1135
- Drake RL, Vogl W, Mitchell AWM, Gray H. Gray’s anatomy for students. 2nd edition, Churchill Livingstone–Elsevier, Philadelphia, 2010
- Rec., 75: 23-26, 1939
- Arch Orthop Trauma Surg, 1979, 93(4):307–312
- Georgetown Medical Bulletin, 1960. 13, 232-238
- Acta Psychiatrica et Neurologica Scandinavica, suppl., 1951. 74, 251-254
- Neurosurg, 2010; 113: 110-112
- Semin Musculoskelet Radiol. 2010; 14: 473-486
- J of Bone and Joint Surgery. 1981. 63-A(6),885-890
- Int J Biomed Sci 2016; 12 (3): 89-94
- Electromyogr Clin. Neurophysiol. 2007; 47: 89-92
- Korean Neurosurg Soc, 2014. 55 (5) : 296-299
- Brachial Plex Peripher Nerve Inter. 2008; 3: 17
- SICOT J 2016, 2:9
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.