Plantar fasciitis and foot strength - is there a correlation?

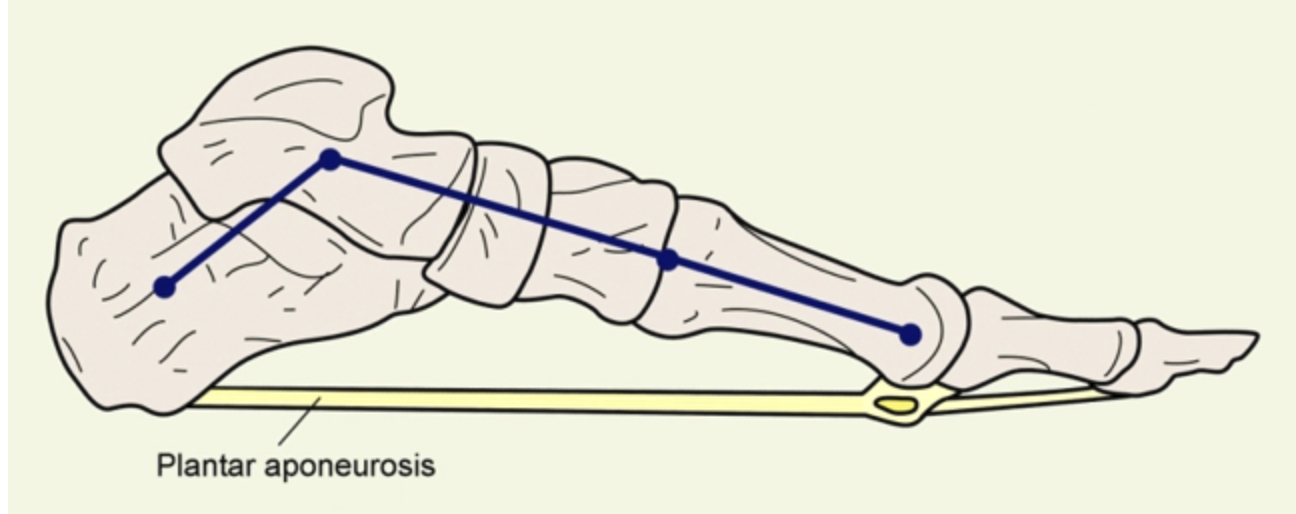
While plantar fasciitis (PF) plagues only 8% of athletes, it can be debilitating and require extended time off from sport(1). Plantar fascia (also called the plantar aponeurosis) pain strikes at the origin of the fascia on the medial tubercle of the calcaneus (see figure 1). Athletes typically feel the pain on their first steps out of bed in the morning. Those athletes with heavier body types or a high body mass index, like gridiron football linemen or weightlifters, are more susceptible to PF(1).
Figure 1: The plantar aponeurosis
To determine if lower extremity strength is a risk factor for PF, researchers from La Trobe University conducted a systematic review of evidence on the topic(1). This review included prospective case-controlled studies, cross-sectional studies, and randomized trials. All studies assessed the strength or muscle size of lower extremity muscles. Of the initial literature search, seven studies met the criteria for inclusion in the review. While the quality of the included studies was high, the strength of evidence in their conclusions was low. However, some interesting correlations were noted in the review.
Two studies that examined hallux plantar flexion strength found that those with PF were weaker than those without heel pain. However, only one of these studies reached significance in their findings. Three studies measuring lesser toe plantar strength found similar results, with subjects with plantar pain testing weaker than their pain-free controls. This difference reached significance in two of the studies.
The one study that tested ankle strength in subjects with heel pain found a significant weakness in inversion and eversion compared to controls. Their dorsiflexion strength was also less than those without heel pain, but not significantly so. The same proved true with the production of plantar flexion torque, which was lower in those with heel pain.
Interestingly, a meta-analysis of two studies of calf muscle endurance strength found no significant difference in the performance of a single-leg calf raise exercise between those with PF and without. Another study examining rocker-board plantar flexion endurance discovered those with heel pain were significantly unable to complete as many repetitions as the pain-free subjects.
A study looking at muscle volume via MRI found the rearfoot, forefoot, and total foot volumes smaller in those with heel pain. However, the cross-sectional area of the tibialis posterior was the same in both groups. This study was quite small (eight subjects) and did not reach significance. Another analysis normalized muscle volume to body weight and found the differences in the rearfoot and total foot to be significant.
Practical implications
While all the studies in this review were quite heterogeneous, they offer a total picture of lower foot and ankle strength as it exists in those with PF. The authors caution drawing conclusions from the work; however, the overwhelming trend in the review is that intrinsic foot muscle weakness correlates with PF. Interestingly, calf muscle strength and volume does not seem to accompany PF. The question to resolve with further research is whether the weakness is a chicken or an egg? Does foot muscle weakness contribute to the development of PF, or do the muscles become weak secondary to the pain and disfunction caused by PF?Current treatment modalities offer limited success in the treatment of PF. Often treatment focuses on stretching the plantar fascia, especially during the night. However, even with vigilant stretching, the pain can linger for months. This review didn’t examine interventions, but neither modalities nor stretching address the strength deficits observed in the feet of those who suffer from PF.
According to this review, calf weakness and tightness, also long thought to contribute to the strain on the plantar fascia, may not play a role in this condition. Rather, the non-contractile fascia may bear an increased load due to foot muscle weakness. The authors note that the study does not conclude that strengthening the muscles of the feet will improve PF pain. However, a treatment plan for PF should include strengthening of the feet (see figures 2 and 3).
Figure 2: Towel Scrunches
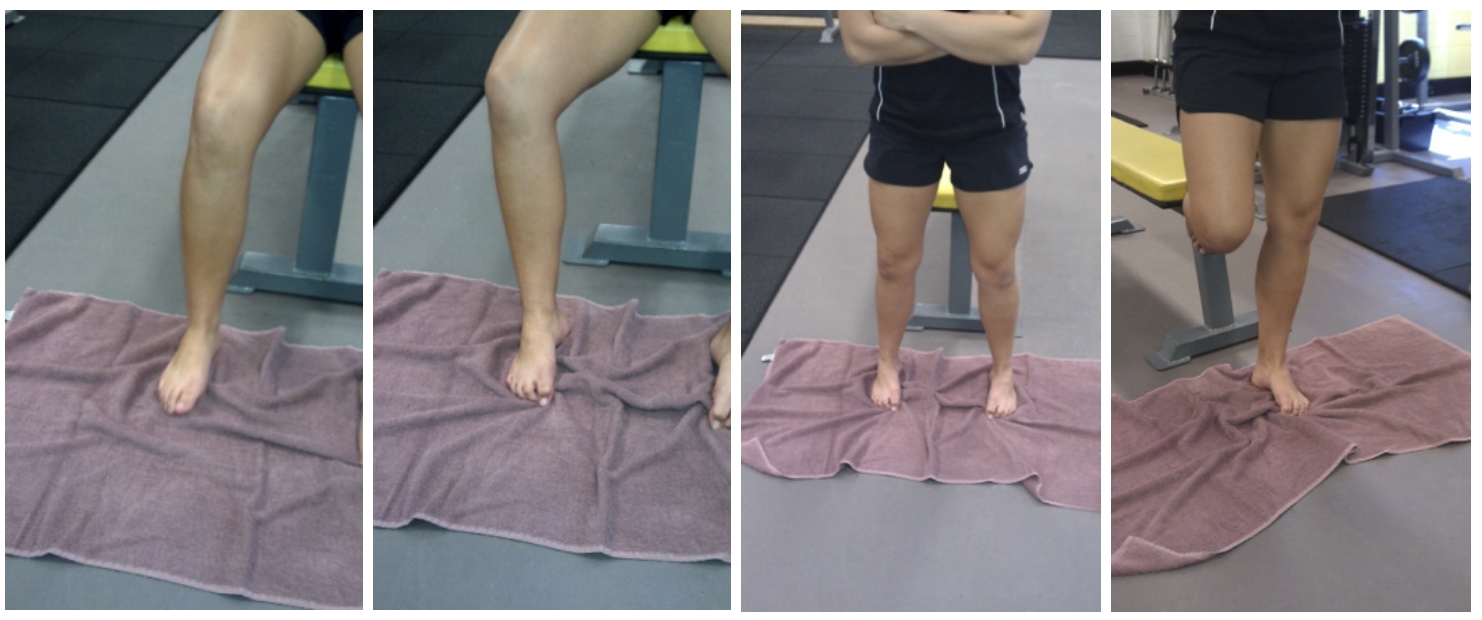
Begin in sitting and scrunch a towel with both feet. Progress to standing scrunches with both feet, then standing on one foot.
Figure 3: Cup exercise

Pick up a cotton ball with one foot and place it into a small cup. Begin in sitting and progress to standing sets of 10 reps.
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










