Shoulder instability: prevention for better performance

Shoulder instability is the abnormal movement of the shoulder joint beyond normal physiological ranges, which can result in subluxation (partial displacement) or dislocation (full displacement) of the humeral head in the glenoid cavity (shoulder joint complex)(1). This may occur as a direct result of trauma, due to structural deficits, or because of poor muscle recruitment of the shoulder joint(1).
Shoulder dislocation is two and a half times more likely to happen to men, and is most common in athletes aged 30-40(2). Other factors such as genetics and hyper-mobility syndrome increase the risk of dislocation. Dislocation following trauma generally causes structural damage within the joint and approximately two thirds of athletes will suffer a further dislocation at a later date due to these deficits(3). This happens because the ligaments, tendons, cartilage, and surrounding muscles either heal incorrectly or fail to heal. Either way, continued use of the shoulder causes further damage to these structures.
Non-traumatic instability (occurring without trauma) accounts for around 10% of dislocations and is usually the result of one of two issues:
- Inherent structural problems where already lax structures are further strained with repetitive use of the joint.
- Poor muscle activation and recruitment surrounding the scapula and shoulder joint (also called scapular dyskinesia). With repeated use, weakness and faulty biomechanics leads to failure of the joint stabilizing mechanisms(1).
Laxity and scapular dyskinesis
Laxity and scapular dyskinesis often go hand in hand with each other. Shoulder laxity is greater in athletes involved in overhead or throwing sports such as tennis, baseball, and swimming. Swimming in particular involves continued, repetitive overhead activity, and up to 91% of competitive swimmers have reported shoulder problems as a result. Of these, 21% begin as young as 8-11years old(4,5). This early onset of shoulder symptoms can lead to future problems. The training load continually increases but the structures are never fully rehabilitated, leading to increased laxity, dyskinesis, and eventually wear and tear of the surrounding structures.Scapular dyskinesia refers to the altered position and motion of the scapula, usually due to either poor muscle activation or increased laxity, as described above. Athletes with scapular dyskinesis are 43% more likely to develop shoulder pain than those without(6). Dyskinesis can cause narrowing of the subacromial space, which in turn leads to strain on the rotator cuff tendons. This weakens the rotator cuff, leading to painful conditions such a shoulder impingement syndrome or rotator cuff tendinopathy.
Exercise for prevention
Shoulder injuries predominantly occur through overuse. As mentioned previously, swimmers will likely suffer a shoulder injury at some point in their career. The repetitive, overhead, and high velocity demands of throwing sports also make athletes who participate in them particularly vulnerable to shoulder injuries. Most risk factors for shoulder injury in throwing sports are non-modifiable, meaning they cannot change - eg gender, participation level of competition and training, biomechanics, and external workload(7). The only study to date that has investigated the effects of implementing a prevention program for shoulder injuries found a 28% reduction in injury prevalence(8). This program required the subjects to complete a number of pre-training warm-up exercises (see fig 1 below).A dynamic warm-up prevention strategy such as this could be important for many upper limb dominant sports, particularly throwing sports, because it targets the risk factors for these injuries, including reduced internal rotation, external rotational strength, scapular strength, kinetic chain activation and thoracic mobility. Implementing this at the start of the competitive season could improve shoulder and thoracic mobility, reduce scapular dyskinesis, and strengthen the full kinetic chain.
Fig 1: Schematic diagram detailing the warm up exercises for a shoulder pain prevention program(8)
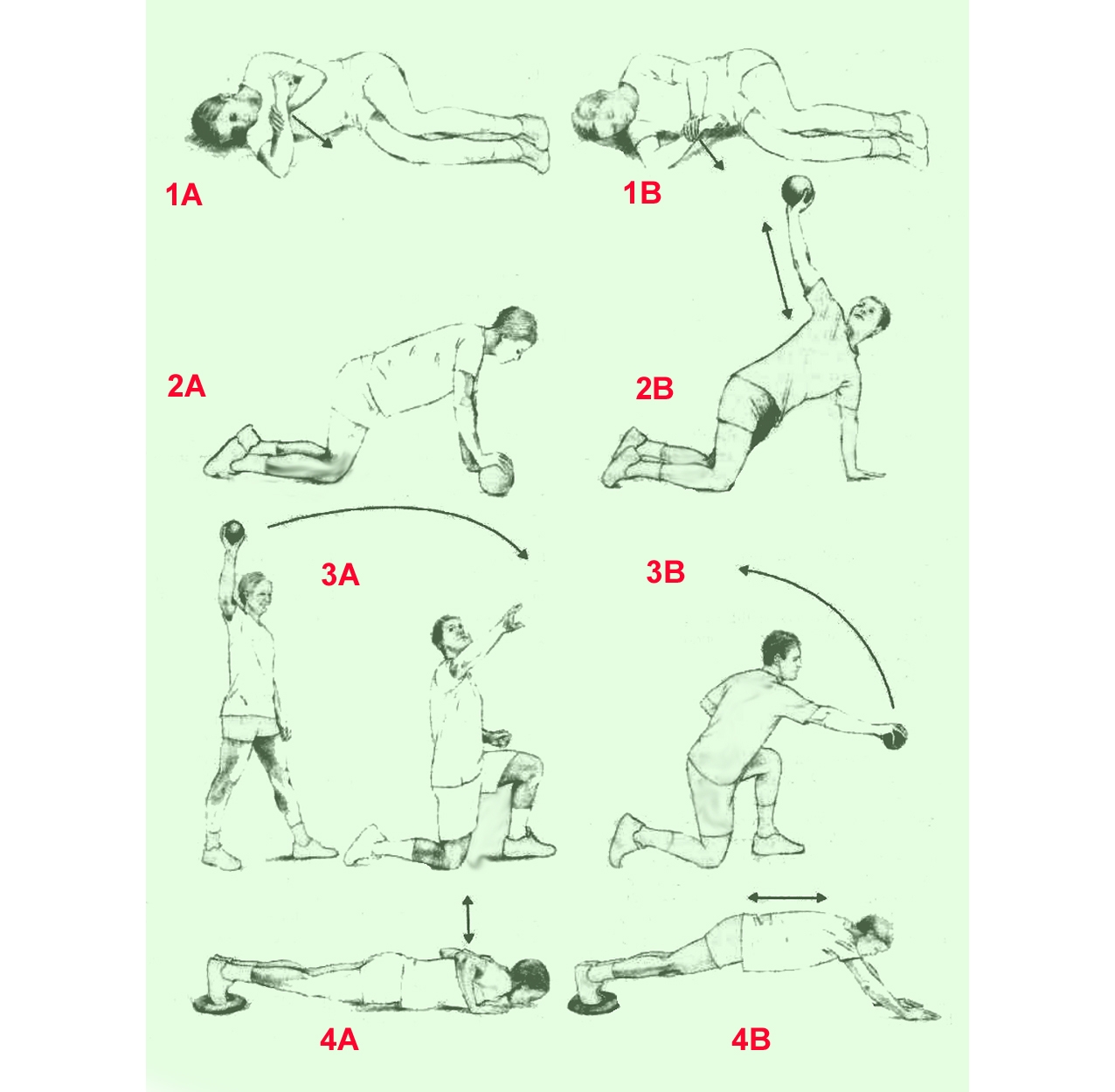
‘A’ refers to start position; ‘B’ refers to finish position
Exercise for rehabilitation
Shoulder rehabilitation plans must involve the full kinetic chain to account for the complex, multidimensional nature of throwing and overhead style sports. Throwing sports rely on the transfer of force and motion. This begins with foot contact on the ground, while the large leg and core muscles account for 51-55% of the kinetic energy that is transferred through to the upper limb(9). Rehabilitation exercises should therefore activate the shoulder, core, pelvis, and lower body in a sequential manner. Here is a suggested rehabilitation plan to restore shoulder stability and strength systematically.- Create a stable base
The exercises here (figures 2 and 3) strengthen the core for a stable trunk, whilst opening the chest and shoulders for optimal movement ranges. Hip twisting stabilizes the core through rotation, which is ideal for many sports involving twisting and using the shoulder and core together. The swimming exercise (see figure 3) isolates the scapular muscles whilst maintaining core activation. This encourages the shoulder complex to work with the trunk when isolated.
Figure 2: Hip twist start and finish position.


Figure 3: Swimming arms exercise start and finish position.


- Apply strength
Moving on, exercises should progressively apply overload for greater strength gains under demand. They should also retrain rotator cuff muscle activation, as these muscles are responsible for the scapular stability. Figure 4 shows leg pull in prone, which challenges shoulder stability and strength by holding up body weight and moving into the high plank position. Other useful exercises are scapular push-ups or reverse dumbbell flies.
Figure 4:Leg pull in prone strength exercise with leg raised

- Introduce mobility
As the shoulder complex becomes stronger, the goal is to maintain strength whilst moving through greater ranges of movement. Arm openings (figure 5) encourages a wide circle of mobility whilst maintaining scapular control. Other exercises include lateral rotations with resistance bands, and lateral rotation then elevation with bands.
Figure 5: Arm openings start and finish position


- Add full-body integration
Finally, the whole body needs to be integrated for maximizing the force development and transfer through the body to the shoulder. Thread the needle (see figure 6) when performed with a resistance band is an excellent example, as are forward lunges with scapular retractions (see figure 7) or any type of lunges with shoulder rotation.
Figure 6: Thread the needle


From a position of 4-point kneeling thread one arm through as far as comfortable, then open it out towards the ceiling as per the second picture.
Figure 7: Forward lunge with resistance band and scapular retraction

This exercise can be further modified to fully incorporate the whole body of the core, lower limbs, and upper limbs using a cross-body method. Here, the band is placed under a foot and held in the opposite hand. As the knees are bent (lunge) the band is pulled across the body and upwards with arm raised above the head to finish.
Return to sport
Despite undergoing extensive prevention programs and rehabilitation exercises, the clinician may still question an athlete’s readiness to return to high performance following shoulder instability. They may pass all the standard testing for strength, mobility and function, but these never fully replicate the grueling demands of competitive sport and an athlete’s willingness to accept high loads through high velocities.The ‘Athletic Shoulder Test’ is a newly-developed test that uses force platforms with the arm outstretched to replicate long-lever stress and the ability to transfer this force across the shoulder complex(10). It is still in its early stages of research, but so far is proving reliable for end-stage, high level sport testing.
Figure 8: Athletic Shoulder Test(10)

Diagram showing the three different positions shoulder strength is measured to evaluate readiness for return to performance.
Summary
- Shoulder instability is the abnormal movement within the shoulder joint, which can lead to subluxation, dislocation, or chronic shoulder pain.
- Scapular dyskinesis is the altered biomechanics of the scapula and occurs due to poor muscle activation or increased laxity surrounding the scapula.
- Shoulder instability and scapular dyskinesis are often worse in throwing sports due to overuse, repetition of overhead activity and large velocity demands - but can be improved using rehabilitation exercises.
- Prevention programs should include shoulder mobility, external rotation strength, scapular strength, kinetic chain activation and thoracic mobility exercises.
- Rehabilitation plans should utilize a whole body approach, incorporating global muscles and linking the upper and lower body through the core.
- Prevention is always better than rehabilitation for shoulder problems; due to the large range of mobility and lack of structural support, the risk of recurrent injury is ever present.
References
- Br J Sports Med. 2016; 50:440-447
- EFORT Open Rev. 2019 May 11;4(5):194-200 3. J Bone Joint Surg Am. 2006; 88: 2326-2336.
- SportsHealth. 2010;4: 246-251.
- J Athl Train. 2012; 47: 149-158.
- Br J Sports Med. 2018; 52: 1-10. doi: 10.1136/bjsports-2017-097559.
- ARTICLE 3 Br J Sports Med. 2018; 0:1-9. doi:10.1136/bjsports-2017-098254.
- Br J Sports Med. 2017; 51:1073-1080.
- PM & R. 2016; 8:S69-77.
- Br J Sports Med. 2019; 53(9): 524-525.
You need to be logged in to continue reading.
Please register for limited access or take a 30-day risk-free trial of Sports Injury Bulletin to experience the full benefits of a subscription. TAKE A RISK-FREE TRIAL
TAKE A RISK-FREE TRIAL
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










