Menopause and Adhesive Capsulitis
Megan Dutton explores how menopause-related endocrine and inflammatory changes may be the primary driver in adhesive capsulitis.
For years, existing literature has labeled adhesive capsulitis or frozen shoulder (FS) as “idiopathic”, commonly associated with diabetes, thyroid disease, cardiovascular, and metabolic conditions(1). Yet, a higher prevalence of frozen shoulder is noted in women, with peak incidence demonstrating a striking overlap with perimenopause and early post-menopause(2). Is it then not plausible to consider that menopause-related endocrine and inflammatory changes may be a primary biological driver in this complex, multifactorial condition rather than a coincidental risk factor?
The Menopause-Frozen Shoulder Overlap
Adhesive capsulitis affects an estimated 2–5% of the general adult population, with incidence rising sharply in individuals aged 40–60 years and peaking in the sixth decade of life(3). Epidemiological studies consistently demonstrate a notable female predominance, with approximately 60–70% of cases occurring in women compared with men, and women being at higher risk of severe and prolonged symptoms(4). While the exact mechanisms underlying this sex difference remain incompletely understood, hormonal factors, particularly those related to estrogen, are increasingly recognized as potential contributors.
A retrospective cohort analysis from Duke University suggested that post-menopausal women on hormone replacement therapy (HRT) had a lower incidence of adhesive capsulitis than those not receiving estrogen, providing early evidence that estrogen deficiency may influence susceptibility to the condition(5).
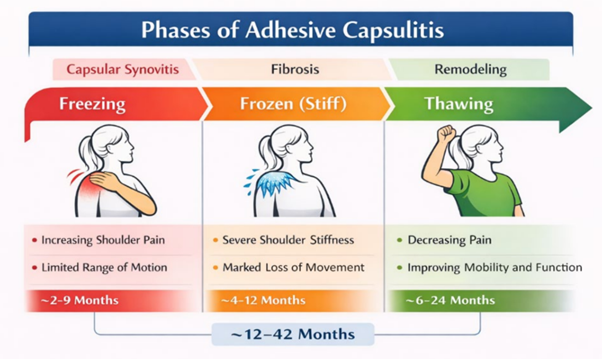
Clinically, adhesive capsulitis transitions through three characteristic phases: an initial freezing (painful) phase characterized by progressive synovitis and escalating pain; the frozen (stiffening) phase marked predominantly by capsular fibrosis and persistent global restriction of glenohumeral motion; and the thawing (recovery) phase, during which gradual recovery of range occurs over months to years (see Figure 1)(6).
Etiologically, primary adhesive capsulitis arises without an identifiable trigger and is often deemed idiopathic, whereas secondary adhesive capsulitis develops in the context of known precipitating factors such as trauma, surgery, prolonged immobilization, or systemic conditions(7). Recognition of these epidemiological patterns and pathophysiological distinctions is particularly relevant in midlife women, in whom declining estrogen levels may influence inflammatory and fibrotic pathways within the shoulder capsule. Ultimately, understanding these distinctions is essential for assessing and managing midlife female athletes.
Estrogen and Connective Tissue
Estrogen plays a central regulatory role in musculoskeletal homeostasis, influencing collagen synthesis, matrix remodeling, and fibroblast activity via estrogen receptor (ER-α/ER-β) signaling pathways. Experimental data demonstrate that estrogen modulates collagen turnover and reduces excessive cross-link formation, thereby maintaining tissue compliance(8). It is therefore not surprising that estrogen deficiency is associated with reduced fibrillar organization, increased stiffness, and altered extracellular matrix (ECM) remodeling dynamics(9). Beyond its structural role, estrogen exerts important vascular and immunomodulatory effects. It enhances endothelial nitric oxide production, supports microvascular perfusion, and modulates inflammatory cytokine expression(10).
Estrogen deficiency during menopause is associated with a shift toward a pro-inflammatory milieu and increased transforming growth factor-β (TGF-β) activity, both of which are key drivers of fibroblast proliferation and myofibroblast differentiation(11). Evidence from other tissues strengthens this biological plausibility. Postmenopausal women demonstrate increased rates of tendinopathy, alterations in pelvic floor connective tissue integrity, and increased dermal stiffness with reduced elasticity(12-14). These findings reflect a systemic alteration in connective tissue behavior rather than isolated regional pathology. The glenohumeral capsule may be particularly vulnerable to these changes. Shoulder biomechanics rely heavily on capsular compliance for normal arthrokinematics, and capsular tissue is sensitive to inflammatory mediators. In a low-estrogen environment, the balance between collagen synthesis and adaptive remodeling may shift toward pathological cross-linking and fibrosis(12). This theory is supported by histological studies of the capsular tissue in adhesive capsulitis, which demonstrate increased fibroblast density, myofibroblast differentiation, and upregulation of pro-fibrotic mediators(13). Consequently, capsular fibrosis in midlife women may represent the musculoskeletal manifestation of a broader systemic endocrine-modulated process.
Inflammatioin, Metabolism, and Fibrosis
Menopause is accompanied by measurable metabolic and inflammatory changes. Declining estrogen is associated with increased visceral adiposity, reduced insulin sensitivity, altered glucose handling, and upregulation of pro-inflammatory cytokines(14). These shifts occur even in lean, physically active women. The resultant subclinical insulin resistance may allow
advanced glycation end-products (AGEs) to accumulate within collagen matrices, increasing cross-link density and reducing tissue extensibility, similar to that seen in diabetic hyperglycemia(1, 19).
Unsurprisingly, a systematic review and meta-analysis have confirmed a strong relationship between frozen shoulder, metabolic, and inflammatory markers(15). This cytokine-driven fibroblast activation, coupled with impaired inflammatory resolution, promotes persistent fibrosis rather than adaptive repair. From a clinical standpoint, this raises important considerations. In a metabolically and immunologically primed environment, aggressive loading strategies may exacerbate pain and irritability. Heightened nociceptive sensitivity, reduced tissue adaptability, and prolonged inflammatory signaling can result in symptom escalation rather than functional progression. Subsequently, adhesive capsulitis may be better conceptualized as a metabolic–inflammatory condition with a musculoskeletal expression, rather than a purely mechanical capsular contracture.
Pain Perception
Estrogen also modulates nociceptive processing centrally and peripherally. It influences descending inhibitory pathways, neurotransmitter regulation, and inflammatory pain signaling. Reduced estrogen levels are associated with diminished endogenous pain inhibition and increased inflammatory pain sensitivity(16). Given the shoulder capsule’s dependence on capsular compliance and its sensitivity to inflammatory mediators, these endocrine, inflammatory, and neurophysiological shifts may create a permissive environment for capsular fibrosis and persistent pain characteristic of adhesive capsulitis(17).
Further, this pain perception may be aggravated by sleep disturbance, fatigue, mood fluctuation, and heightened stress reactivity, all factors known to frequently occur during the menopausal transition. These neuroendocrine interactions may help explain the characteristic clinical features of adhesive capsulitis in midlife women: severe night pain, pain disproportionate to measurable loss of motion, and heightened irritability with manual therapy or exercise. Importantly, pain behavior in this cohort should not be prematurely attributed to poor coping or nonspecific central sensitization. Hormone-mediated alterations in nociceptive modulation, layered upon a pro-fibrotic capsular process, offer a biologically coherent explanation for symptom severity.
Clinical Implications
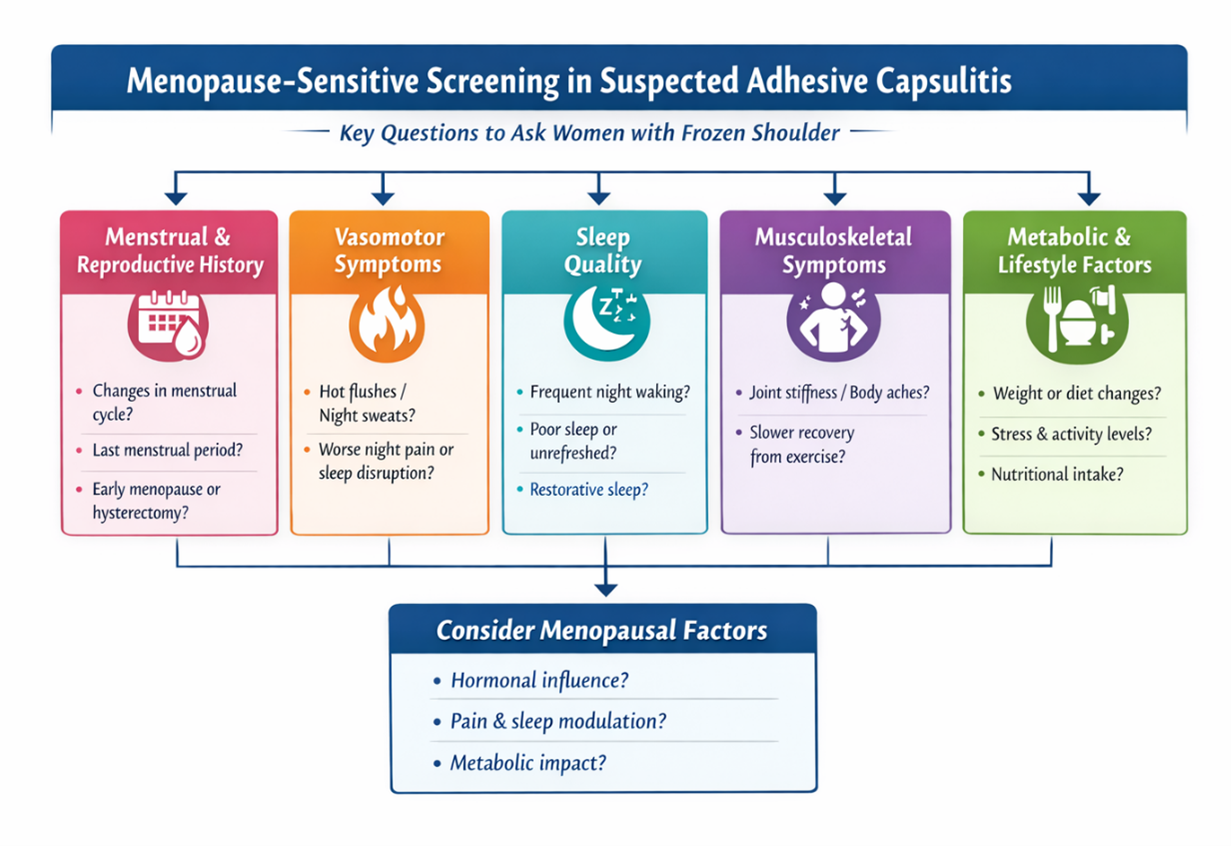
In athletic and highly active women, adhesive capsulitis is frequently attributed to training load, minor trauma, or technical error. However, the menopausal transition is rarely screened despite its biological relevance to connective tissue remodeling, inflammation, and pain modulation(19). Clinicians should include targeted questions regarding menstrual irregularity or recent cycle cessation, vasomotor symptoms, sleep disturbance, and history of early menopause, hysterectomy, or oophorectomy when assessing women aged 40–60 (see Figure 2). These variables may influence tissue irritability, recovery capacity, and rehabilitation response(19-22).
Further, certain clinical features may indicate a systemic contribution. Bilateral or sequential shoulder involvement, rapid stiffness progression, disproportionate night pain, and poor response to otherwise appropriate rehabilitation should prompt broader consideration of metabolic and endocrine influences. The established association between adhesive capsulitis and metabolic dysfunction further supports this systems-based assessment approach(20).
Importantly, interdisciplinary awareness is essential. Collaboration with general practitioners, endocrinologists, and women’s health specialists may be appropriate when systemic symptoms coexist or when recovery deviates from expected trajectories. Ultimately, failure to consider menopausal status risks misclassification of pathology, mistimed loading strategies, and avoidable patient frustration.
Rethinking Rehabilitation
Mechanical loading remains fundamental in musculoskeletal rehabilitation. However, in menopause-associated adhesive capsulitis, the biological context modifies tissue response to load. Estrogen deficiency, low-grade systemic inflammation, and altered nociceptive modulation may collectively reduce tissue adaptability while amplifying pain sensitivity(19-22). Histological evidence demonstrates fibroblast proliferation and pro-fibrotic signaling within the capsule, suggesting that aggressive stretching or high-intensity mobilization may exacerbate symptoms during high-irritability phases(16-18).
Expectation management is therefore critical. Symptom trajectories may be prolonged and fluctuate more than in purely mechanical shoulder conditions. Rehabilitation should prioritize symptom-guided loading, gradual exposure to range and strength development, and pain-informed progression rather than pain-provocation models.
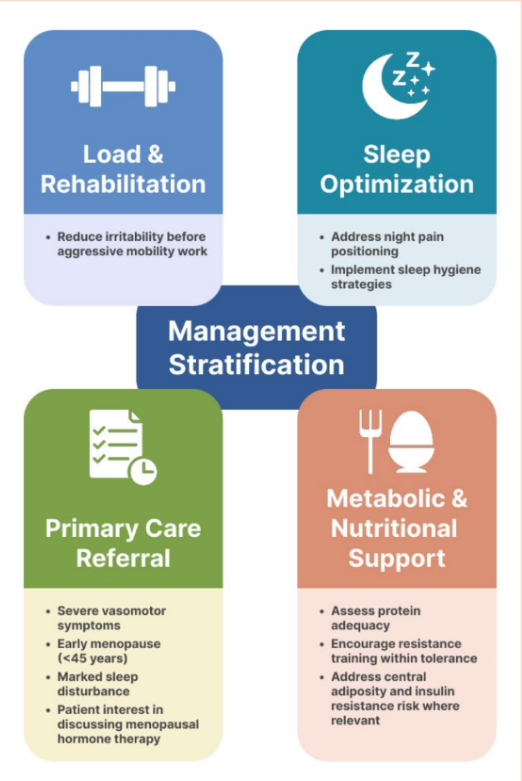
Further, adjunctive strategies warrant equal emphasis. Optimizing sleep, addressing psychosocial stress, and educating patients regarding hormonal influences may reduce central amplification and improve adherence(18). Where persistent severe night pain, rapid deterioration, or bilateral progression occur, escalation or referral should be considered (see Figure 3).
Reframing Idiopathic
Adhesive capsulitis in midlife women may be more accurately conceptualized as a systemic inflammatory–fibrotic condition influenced by hormonal transition. Estrogen decline affects connective tissue regulation, metabolic balance, inflammatory signaling, and pain modulation; all mechanisms that converge within the glenohumeral capsule. Acknowledging menopause does not over-medicalize care; it contextualizes it. The challenge for clincians is to evolve beyond purely biomechanical models toward biologically informed rehabilitation strategies.
References
-
Clin Orthop Relat Res. 2000;372:3-322.
-
J Clin Med. 2025;14:1780-1799.
-
J Shoulder Elbow Surg. 2016;25(6):e119-e127.
-
Clin Orthop Surg. 2021;13(2):168-175.
-
Ortho J Sports Med. 2023:11(7)(suppl 3).
-
JAMA Netw Open. 2020;3(12):e2029581.
-
J Orthop Sports Phys Ther. 2013;43(5):A1-A31.
-
Front Physiol. 2019;9:1834.
-
Br J Sports Med. 2016;50(19):1187–1191.
-
J Clin Endocrinol Metab. 2020;105(8):e2773–e2780.
-
J Shoulder Elbow Surg. 2017;26(11):e359-e371.
-
J Orthop Res. 2021;39(5):1021–1030.
-
J Shoulder Elbow Surg. 2019;28(5):e126-e134.
-
J Clin Med. 2025;14(20):7315.
-
BMC Musculoskelet Disord. 2025;26:475
-
Pain. 2018;159(Suppl 1):S3–S12
-
Br J Anaesth. 2019;123(2):e146–e157.
-
Maturitas. 2025;191:108135.
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.