The Invisible Limb of Football Rehabilitation
In football, injury impacts not only physical performance but also confidence, identity, and emotional well-being. Joshua Smith discusses how recovery must address both the mental and physical aspects to support a successful return to play.
Brasileiro Championship - Corinthians v Flamengo - Neo Quimica Arena, Sao Paulo, Brazil - Corinthians’ Andre shoots at goal REUTERS/Jorge Silva
In the high-stakes environment of modern football, the criteria for return to play (RTP) have become increasingly sophisticated. Medical departments utilize GPS data to monitor high-speed running loads, force plates to measure limb symmetry indices, and isokinetic dynamometry to ensure peak torque ratios are restored to preinjury levels. Practitioners have never had more data regarding the physical state of the athlete. Yet, despite these rigorous objective markers, reinjury rates in football remain stubbornly high, particularly following severe injuries such as anterior cruciate ligament (ACL) reconstruction or grade three hamstring strains.
"Moving rehab sessions to the pitch sideline during team training introduces contextual interference..."
Although sports injury rates remain a public health issue, affecting an estimated 8.6 million individuals annually in the US alone, a substantial gap persists in how rehabilitation programs address the psychosocial dimensions of recovery(1). There is often a perplexing disconnect between clinical and performance clearance. A player may demonstrate symmetrical quadriceps strength and pass a battery of hop tests in the gym, yet upon returning to the chaotic environment of a competitive match, they hesitate in a duel or alter their landing mechanics during an aerial challenge. This hesitation is rarely a failure of muscle fiber or graft integrity; it is a failure of psychological readiness.
Psychological readiness is defined as the possession of psychological resources to facilitate a safe, productive, and enjoyable return to sport. It is the often-overlooked invisible limb of rehabilitation. For the football medic, physiotherapist, or strength and conditioning coach, understanding and quantifying this state is no longer optional. It is a critical component of secondary injury prevention, and psychological factors are among the strongest predictors of whether an athlete returns to their preinjury level of play, often outweighing physical function metrics. Psychological and social factors are equally pivotal in determining whether athletes return to their preinjury performance or withdraw from the sport altogether(2,3).
The Biopsychosocial Model in Football
Historically, sports medicine relied heavily on the biomedical model, an approach that views injury as a purely tissue-based problem (see table 1). The logic follows that if we repair the tissue and restore the strength, the player is fixed. However, contemporary evidence overwhelmingly supports a biopsychosocial model for RTP(4). Sports injuries are not only physical setbacks but complex biopsychosocial events that profoundly affect athletes’ mental health, motivation, and identity(5). This model suggests that biological, psychological, and social factors interact dynamically to determine outcomes.
Table 1: Biomedical vs. biopsychosocial model in rehabilitation(4,5)
| Feature | The Biomedical Model | The Biopsychosocial Model |
| Core Philosophy | Injury is a purely tissue-based problem. | Biological, psychological, and social factors interact dynamically to determine outcomes. |
| Primary Logic | Tissue repair and restoring strength fix the player. | Addressing the mind is effectively addressing the biomechanics of the knee and ankle. |
| Biomechanical View | Relies heavily on objective physical function metrics. | A player’s fear of reinjury, known clinically as kinesiophobia, can directly influence their biological output. |
In football, this interaction is potent and observable. A player’s fear of reinjury, known clinically as kinesiophobia, can directly influence their biological output. High levels of fear alter neuromuscular control strategies. A fearful player may unconsciously adopt a stiff-knee landing strategy to limit joint excursion. This paradoxically increases the ground reaction forces that the passive structures, such as the ACL graft, need to absorb, rather than the muscular system(6). Furthermore, this emotional burden not only interferes with motivation but may also postpone or even block physical healing entirely(7). Therefore, psychological readiness is not merely about feeling good; it is a physiological safety mechanism. Addressing the mind is effectively addressing the biomechanics of the knee and ankle.
Psychological Barriers to Performance
While the psychological landscape of an injured footballer is complex, a spectrum of distress, ranging from frustration and fear of reinjury to depression and anxiety, can significantly disrupt their rehabilitation trajectory(8). Three dominant factors consistently emerge as predictors of successful RTP (see figure 1).
- Athletes most frequently cite fear as the barrier to returning to preinjury levels of performance. In a systematic review involving over 7,500 patients, researchers from La Trobe University demonstrated that fear of reinjury was the primary reason athletes cited for not returning to sport, even when their physical function was objectively normal(9). This fear creates a protection-performance trade-off in which the brain prioritizes protecting the injured site over performance cues. The result is often a player who is physically present on the pitch but mentally absent.
- Confidence in the injured body part is distinct from general self-confidence. A striker may be confident in their ability to score goals (self-efficacy) but lack confidence that their rehabilitated ankle will hold up under the load of a volley (injury-specific confidence)(10).
- Athletic identity disruption represents a profound psychological trauma for many players. For many athletes, sport is completely intertwined with their self-worth(11). The loss of the locker room environment and the inability to contribute to the team can trigger significant mood disturbances. Injury has the potential to undermine this sense of identity, leading to greater depressive symptoms and uncertainty about their competency and future career prospects(12). Players who feel isolated during rehab have lower psychological readiness scores upon return(13).
Neurocognitive Considerations and Biomechanics
Psychological readiness is a neurocognitive issue. A healthy footballer moves automatically, seeing the space and executing the relevant action without conscious thought. An injured footballer with low psychological readiness moves explicitly, thinking about the previously injured site, then the action, then the space. This reinvestment of conscious attention into movement mechanics slows down reaction time and occupies working memory (see table 2)(14).
| Healthy Athlete (Automatic Processing) | Injured Athlete (Conscious Processing) | |
| Input | Ball, Opponents, Tactics, Space | Ball, Opponents, "Is my knee safe?" |
| Processing | Subconscious (Implicit) | Conscious (Explicit / Reinvestment) |
| Mechanism | See space --> Cut | Think about knee --> Position foot --> Cut |
| Bandwidth | Optimal | Overloaded |
| Outcome | High reaction speed, fluid movement. | Slow reaction, stiff mechanics, high injury risk. |
In a match, a player’s brain is bombarded with stimuli. If the brain is also busy processing fear and consciously controlling the knee joint, the bandwidth is exceeded. The player becomes neurocognitively overloaded, which explains the mechanism of many non-contact reinjuries. The brain is distracted by fear and fails to send the correct pre-activation signal to the hamstrings during a landing, leaving the ACL vulnerable. Therefore, psychological readiness is essential for maintaining the feed-forward motor control required for high-speed football(15).
"...kinesiophobia, can directly influence their biological output."
Measuring the Mind
Just as clinicians use a goniometer for range of motion, they must use validated scales to quantify psychological readiness. Two scales are particularly relevant for football practitioners:
- The ACL-RSI (Anterior Cruciate Ligament Return to Sport after Injury) Scale(16).
- The I-PRRS (Injury-Psychological Readiness to Return to Sport) Scale(17).
Clinicians should use these scales for serial monitoring, and scores should trend upward from the return to run phase through to match play. However, while tools like the ACL-RSI and I-PRRS are invaluable, practitioners must remain vigilant for athletes who falsely inflate their scores to expedite their return to the pitch. Subjective questionnaire data must always be cross-referenced with objective body language. If a player scores a 100 on their confidence to change direction but still exhibits visible hesitation or a stiff-legged deceleration strategy during pitch-side drills, this disconnect warrants a deeper, open-ended conversation with the player. In addition, practitioners should merge data streams. Psychological readiness should not be siloed from biomechanical data.
Improving Psychological Readiness
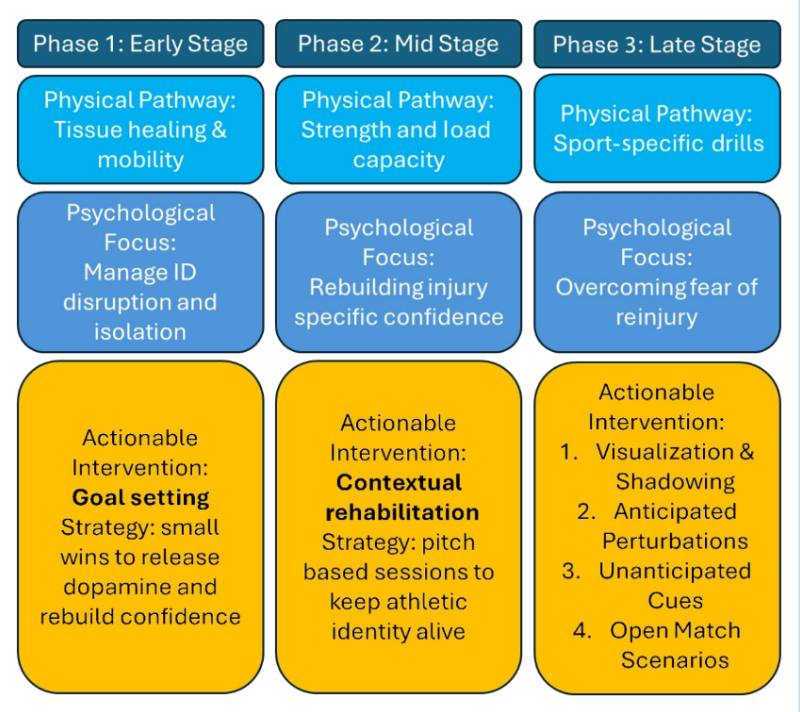
If a player shows low psychological readiness, simply telling them to trust their body is ineffective (see figure 2). The medical staff must integrate psychological conditioning into the physical rehabilitation program.
- Graded Exposure Therapy: The cornerstone of treating kinesiophobia. It involves exposing the athlete to fearful situations in a controlled and hierarchical manner, progressing from visualization to closed skills, then predictable perturbations, and finally open skills(18). To effectively treat kinesiophobia, practitioners should move athletes through a structured, four-step exposure sequence. For example, if a player fears the plant-and-cut maneuver:
• Step 1: The athlete mentally visualizes the cut, followed by performing the movement at 50% speed without a ball, focusing on kinesthetic awareness rather than joint mechanics.
• Step 2: The athlete performs the cut at 75% speed while a physiotherapist applies mild, predictable resistance using a band around the athlete’s waist.
• Step 3: The athlete runs toward a cone and must react to a directional point from the coach at the last second, forcing the brain to process environmental stimuli instead of knee safety.
• Step 4: The player enters a small-sided game where they must execute the cut to evade an actual defender, fully integrating the movement back into a chaotic environment. - Contextual Rehabilitation: Moving rehab sessions to the pitch sideline during team training introduces contextual interference early. Letting the player hear the whistle and the shouting keeps the athletic identity alive and reduces the shock of re-entering the team environment(19).
- Goal Setting and Autonomy: Intrinsically motivated athletes who use goal-setting and positive self-statements tend to exhibit better compliance with their treatment regimens and experience shorter recovery periods(20). Instead of dictating the rehab schedule, the clinician should involve the player in shared decision-making. Achieving small wins releases dopamine and rebuilds the confidence loop(21).
- Video Analysis as Biofeedback: Using visual evidence for cognitive reframing. Showing a player high-speed video proof that their knee is stable provides objective evidence that contradicts their subjective fear(18).
Social Readiness
Rehabilitation does not occur in a vacuum; an injured athlete’s broader social support system is a critical determinant of their recovery trajectory. Strong backing from coaches, physiotherapists, teammates, and family significantly improves both motivation and treatment compliance(22). Consequently, athletes who feel supported by their teams navigate their rehabilitation programs far more efficiently than those who feel isolated(8). Conversely, when sports organizations fail to provide adequate psychological resources, athletes are left vulnerable to an emotional downward spiral(23).
The head coach occupies a particularly influential position within this dynamic. A coach who repeatedly questions a player’s return timeline can inadvertently create immense pressure, which may mask true readiness and tempt the athlete to hide their apprehension. On the other hand, a coach who understands the psychological nuances of the RTP progression becomes a vital therapeutic ally. This alliance relies heavily on nuanced communication from the medical team. Rather than simply declaring a player "physically fit," practitioners must contextualize the psychological data. For example, if a player’s confidence scores are still tracking in the amber zone, the medical report should clearly advise non-contact team training to build neurocognitive readiness. The coach can then safely reintegrate the player using clear social signals, such as assigning them a different colored bib to indicate ’no contact’. This simple modification protects the athlete, allowing them to participate in tactical drills without the fear of an unexpected tackle and reinjury.
"Return to play in football is a high-stakes decision-making process..."
Conclusion
Return to play in football is a high-stakes decision-making process, and the era of relying solely on MRI scans and isokinetic tests is over. The evidence is clear that the mind heals on a different timeline than muscle. Ignoring psychological readiness leaves the footballer vulnerable to a protection-performance trade-off, increasing the risk of reinjury and performance stagnation. Clinicians must ensure that when a player crosses the white line, they are not just physically cleared but psychologically armored for the demands of the game.
References
1. Orthop Rev. 2026.
2. Monten J Sports Sci Med. 2020;9(2):59-64.
3. Work. 2025;80(4):1803-1821.
4. Sport Psychol. 2020;34(3):222-233.
5. Cogent Psychol. 2025;12(1):2537216.
6. Sports Health. 2018;10(3):228-233.
7. Front Psychol. 2025;16.
8. Int Rev Sport Exerc Psychol. 2021;14(1):51-73.
9. Br J Sports Med. 2014;48(22):1613-1619.
10. Sport Psychol. 2015;29(1):1-14.
11. BMJ Open. 2021;11(4):e044199.
12. Front Psychol. 2025;16.
13. Br J Sports Med. 2016;50(9):537-544.
14. J Athl Train. 2017;52(10):918-927.
15. J Orthop Sports Phys Ther. 2019;49(10):701-703.
16. Orthop J Sports Med. 2018;6(4).
17. J Athl Train. 2009;44(2):185-189.
18. Knee Surg Sports Traumatol Arthrosc. 2018;26(10):3012-3019.
19. Br J Sports Med. 2020;54(19):1149-1156.
20. J Sport Rehabil. 2020;29(4):498-502.
21. Br J Sports Med. 2016;50(14):853-864.
22. J Phys Educ Sport. 2021;21(6):3569-3576.
23. Behav Sci. 2024;14(3):254.
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.