You are viewing 1 of your 1 free articles
Is isokinetic shoulder testing worth the trouble?

The shoulder's rotator cuff consists of four small muscles doing a big job. Known as the SITS muscles, the supraspinatus, infraspinatus, trees minor, and subscapularis help keep the free-moving ball end of the humerus in the shallow glenoid fossa of the scapula (see figure 1). They attach on the ventral, dorsal, and superior portions of the humerus, providing both stability to the joint and mobility to the arm.
Figure 1: Ventral view of shoulder anatomy
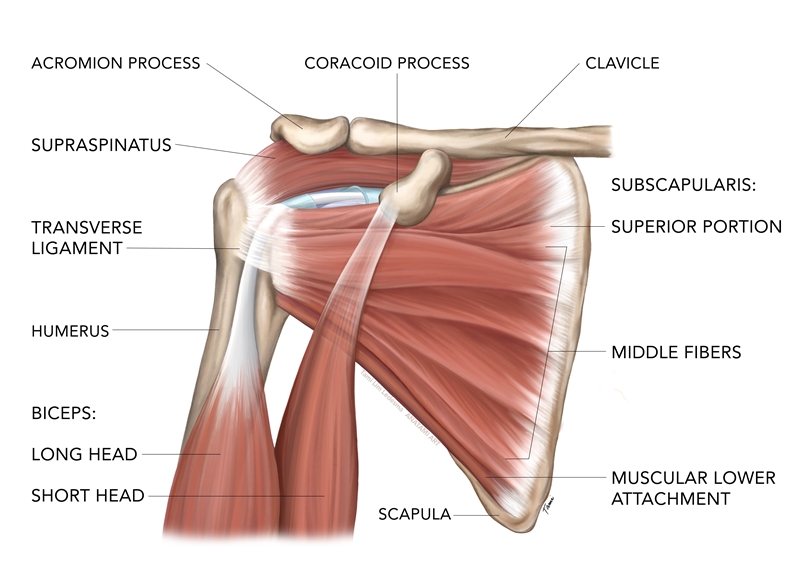
Athletes who participate in overhead sports are particularly vulnerable to acute injury to the rotator cuff. Acute injuries also occur in athletes from contact trauma or a fall on an extended arm. Chronic tendinopathy in these muscles develops from overuse, strain, joint degeneration, and anatomical anomalies. When weakness or injury occurs in one of the muscles, the imbalance around the joint may result in further injury to secondary structures due to the abnormal movement patterns(1). Joint and tendon degeneration may make the muscles more vulnerable to tearing.
Physiotherapist Chris Mallac recently presented an in-depth look at the anatomy, function, and mechanism of injury of the subscapularis. His current article explores the rehabilitation process with an emphasis on tests to diagnose the injury in the clinic as well as exercises for strengthening and improved function.
Strong words
Curiously, researchers in a just-published article on assessment of the shoulder complex strength in young synchronized swimmers made this bold statement:“Isokinetic assessment is essential in sports medicine, since it is the only test capable of diagnosing any shoulder strength deficit.(2)”
Mallac didn’t address using isokinetic assessment as a diagnostic tool or as a measure of progress and I began to wonder why these Spanish researchers felt it was so important. After all, with handheld dynamometers used for reliable manual muscle testing (MMT), is it necessary to have the expense and burden of the large isokinetic equipment for such small muscles?
In a review article, physiotherapists from Arizona expounded on the benefits of isokinetic testing for shoulder injuries, citing the ability to test more functionally using dynamic movements to measure strength, power, and speed(3). Summarizing studies that compared MMT (without dynamometer) to isokinetic testing, they found isokinetic testing more sensitive to subtle weakness than MMT. If indeed, small strength deficits (hard to detect with MMT) impact the movement quality of the shoulder joint, possibly leading to secondary injuries and further degeneration, then isokinetic testing may be more beneficial in measuring when return to play criteria are met.
They also point out the difficulty in establishing agonist/antagonist muscle strength ratios with MMT. These ratios become more important in a joint such as the glenohumeral joint, where the opposing muscles enhance the stability of the joint during movement. Isokinetic data is also better than MMT at detecting symmetry between contralateral joints. In the upper extremities, limb dominance usually means pre-existing asymmetry. However, the authors cite only a 5% to 10% difference as normal in all but elite overhead athletes(3). Isokinetic testing also allows comparison of testing results to normative data. Norm tables give the therapist a reference point to compare both the starting point and progress of the athlete during rehab.
The isokinetic machines offer many more advantages for both testing and developing a rehabilitation program. Often times they sit idle in a clinic collecting dust. Sure they may be clunky and require a bit more time for set up and use, but it may be worthwhile if it guides rehab and improves outcomes for overhead athletes.
References
1. Varacallo M, Mair SD. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018 Jan-2018 Oct 8.2. J Bodyw Mov Ther. 2018 Oct;22(4):968-971. doi: 10.1016/j.jbmt.2018.01.018. Epub 2018 Feb 6.
3. J Athletic Train. 2000;35(3)338-350
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.










