You are viewing 1 of your 1 free articles
Masterclass: Infraspinatus form and function

The infraspinatus (IS), a muscle of the glenohumeral joint, has multiple functions. These include shoulder external rotation, abduction, and stabilization. It works in conjunction with the other rotator cuff muscles, and forms the I of the SITS muscle group (supraspinatus, infraspinatus, teres minor, and subscapularis). The IS originates on the infraspinous fossa and the inferior surface of the spine of the scapular, and inserts on the greater tuberosity of the humeral head(1). The most anterior projection of the IS tendon extends almost to the anterior portion of the highest impression of the greater humeral tuberosity, lateral to the insertion of the supraspinatus(1). The muscle and its insertions are broken up into three distinct parts (see figure 1)(1,2):
- The cranial (transverse) band– This is the superior transverse part that originates from the inferior surface of the spine, and courses laterally to attach to the oblique part at the middle portion of the tendinous part. The tendinous portion of the cranial/transverse part is made up of thin membrane-like tissue, which attaches to the tendinous portion of the oblique part - but does not reach the greater tuberosity. Some researchers suggest that this transverse part shares innervation with the supraspinatus, making these fibers more like the supraspinatus and thus not IS(1).
- The central (oblique) band- The oblique part is a fan-shaped muscle bundle, which originates from the infraspinous fossa, running superolaterally. The oblique and transverse parts fuse together at the superior margin. The oblique part occupies most of the muscular and tendinous portion of the entire IS. The distinct features of the oblique part are as follows:
- Almost the entire tendinous portion of the IS is derived from the oblique part of the IS.
- The tendinous portion of the oblique part becomes longer and thicker superiorly.
- The most superior part of the tendinous portion of the oblique part reaches the anterior-most area of the greater tuberosity.
- The caudal (inferior) band- This thin and short tendinous portion occupies the rest of the IS muscle, and joins the thin and short tendinous portion of the teres minor.
Figure 1: Anatomy of the infraspinatus

The posterior portion of the supraspinatus and the superior portion of the IS blends together at the greater tuberosity, and is composed of thin and fragile fibres, perhaps accounting for the incidence of combined supraspinatus and IS tendon tears in this portion of the rotator cuff(1,3-5).
An important lateral rotator of the shoulder, the IS works in conjunction with the teres minor, posterior deltoid, and supraspinatus(6). It prevents distraction of the humeral head when throwing and decelerates the throwing arm(7). Because the superior tendinous portion of the oblique fibers of the IS reaches the anterior area of the greater tuberosity, it contributes as much to abduction as the supraspinatus(1,5,8,9). However, the role in abduction decreases with increasing lateral rotation angles(8,9). The IS also prevents the humeral head from migrating superiorly, counterbalancing the upward pull of the deltoid muscle during abduction(10).
Injury to the infraspinatus
Injury to the IS can be divided into three distinct clinical entities. :- Infraspinatus atrophy- Atrophy of the IS can occur in the following scenarios:
- Rotator cuff tears(11).
- Suprascapular nerve traction/compression by the superior transverse ligament (usually seen on overhead athletes).
- A ganglion that leads to atrophy of the muscle(12-15).
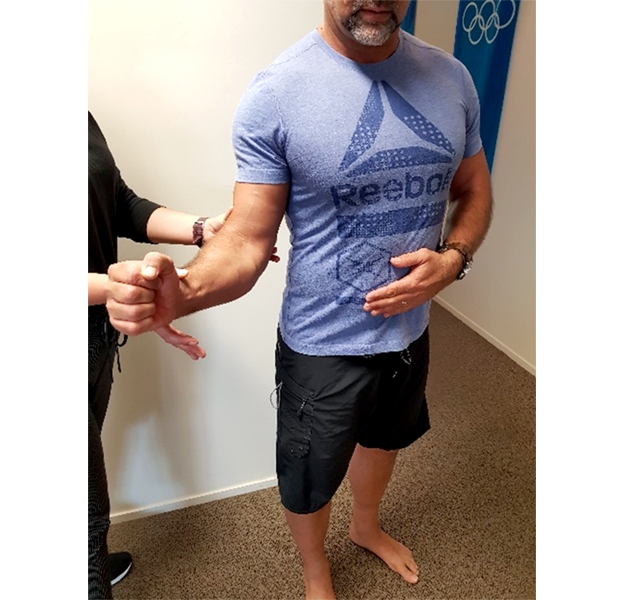
- Infraspinatus tendon tears -Tears of the IS are reasonably common. In a study using arthroscopy to view rotator cuff tears, 22% of full thickness tears were found to be isolated IS tears(16). This finding was similar to that of an MRI study, which showed the prevalence of IS tears to be 25%(17). In a study that looked at 210 cases of rotator cuff tears, 40% were combined supraspinatus and IS tears, while 11% were three-tendon tears, also involving subscapularis(18). Injury and consequent weakness in the IS are best assessed with external rotation with the IS in a shortened position (see figure 2 )(19).
- Myofascial trigger points (TP)- Myofascial TPs are a common source of shoulder pain and tightness in the IS muscle and may limit function of the shoulder. While TP’s in the IS can produce local muscle pain, they may also refer pain to the anterior shoulder and also down the arm, imitating cervical radiculopathy(20-22). Managing the TP’s with direct interventions such as soft tissue therapy and dry needling/injections can significantly improve pain and motion in patients with subacromial bursitis(23,24).
Figure 2: Infraspinatus strength testing (inner range)
Stretching
Tightness and overactivity in the IS is often found in association with shoulder pain syndromes, such as glenohumeral internal rotation deficit (GIRD)(25, 26). When treating GIRD, address tightness in the posterior shoulder muscles, including the IS(27,28). Two primary types of IS muscle stretches can be used:- Hand behind back stretches (see figure 3)- Cadaveric studies show that the middle/central portion of the IS is maximally stretched in internal rotation and shoulder extension(29).
- Across body stretches (see figure 4)- The inferior/caudal portion of the IS is most stretched in internal rotation during shoulder elevation as well as during shoulder extension(29).
Figure 3: Hand behind back stretch

Figure 4: Across body stretch

Strengthening
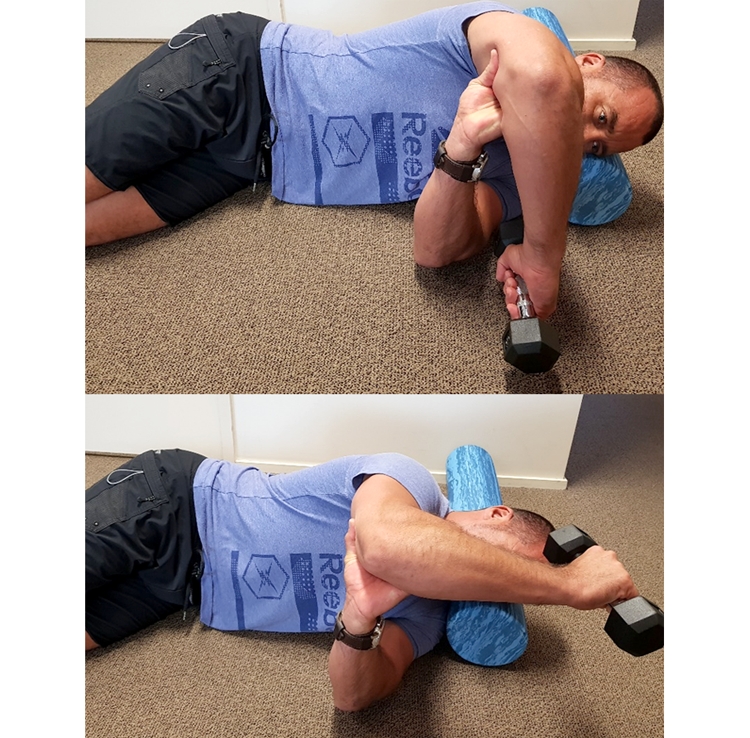
As mentioned, the IS externally rotates the shoulder and assists in shoulder abduction. Therefore, exercises that utilize the action of external rotation with some abduction, whilst minimizing the contribution from the deltoid, are beneficial(30). A study by Ha et al showed that the best exercise to elicit this activation was the ‘side lying wiper’ exercise (see figure 5). This had the most IS activity with the least activation of the middle trapezius and posterior deltoid. If this exercise cannot be used due to range of motion restrictions, then use side lying lateral rotation in a neutral position, as this also recruits IS with minimal contribution from the posterior deltoid(31).Figure 5: Side wiper exercise (top = start, bottom = finish)
Conclusion
The IS muscle is an important rotator cuff muscle, has primary roles in external rotation and shoulder stabilization, and a secondary role of assisting abduction. As the primary lateral rotator of the shoulder, it is prone to small tears and trigger points. In overhead athletes, the overhead action may lead to traction/compression of the suprascapular nerve, and to atrophy of the IS. In the presence of tightness, it may need direct stretching using both hand behind back positions and across body positions. Strengthen the muscle with direct external rotation exercises in a variety of shoulder abduction and/or flexion positions.References:
- Surg Radiol Anat. 2012. 34:257–265
- Surg Radiol Anat. 2017. 39:119–126.
- J Bone Jt Surg. 2010. 92(5):1088.
- J Bone Jt Surg. 2009. 91(Suppl 2 Part 1):1.
- J Bone Joint Surg Am. 2008. 90:962–9
- J Bone Jt Surg. 1944. 26(1):1
- Phys Ther. 1993. 73(10):668–677.
- J Bone Jt Surg Br. 1997. vol 79(1):77
- J Bone Jt Surg. 1994.76(5):667
- J Shoulder Elbow Surgery. 2003. 12:179-84.
- Clin Orthop Relat Res. 1994. 304:78
- Br J Sports Med. 2013. 47:239–244
- J Should Elbow Surg. 1998. 7(5):472–478
- 1992. 74
- Journal of Bone and Joint Surgery. 1994. 76-B. 4. 584-587.
- Eur Radiol. 2007. 17:491–8.
- 2011. 27:463–70.
- 1999. 15:56–66.
- J Shoulder Elbow Surg. 2017. 26, 1390–1398
- BMC musculoskeletal disorders. 2011. 12(1):139.
- Ann Rehabil Med 2017. 41(4):573-581
- J of Alternative and Complementary Medicine. 2017. 23(11); 890-896.
- Manual therapy. 2016. 26:62-9.
- European Journal of Pain. 2008. 12(7). 859-865.
- The Journal of Bone & Joint Surgery. 2005. 87(4):824–831.
- Clinical Biomechanics. 2011. 26(2).130-135
- Physical Therapy and Sport. 2008; 9; 109-116.
- Am J Sports Medicine. 2011. 39; 1997-2006.
- Clinical Biomechanics. 2006. 21; 474-480.
- J of Athletic Training 2013. 48(3):346–352.
- Reinold MM, Escamilla RF, Wilk KE. Current concepts in the scientific and clinical rationale behind exercises for glenohumeral and scapulothoracic musculature. J Orthop Sports Phys Ther. 2009; 39(2):105–117.
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









