You are viewing 1 of your 1 free articles
Subacromial-subdeltoid bursitis: Shoulder pain isn't always the rotator cuff

The subacromial-subdeltoid bursa (SASD) is a potentially pain-sensitive structure of the glenohumeral joint. Along with the rotator cuff tendons, it has been implicated as a primary pathology in painful shoulder conditions of overhead athletes (eg swimmers, weightlifters, gymnasts, tennis players etc). An SASD bursitis is commonly found in association with different stages of rotator cuff pathology¹, but it may also be an isolated pathology due to direct inflammation or trauma to the bursa². When inflamed, a bursitis limits movements such as internal rotation, abduction and flexion³.
Anatomy and Biomechanics
There are numerous bursa found around the glenohumeral joint, which include (see figure 1):- Subacromial (SAB)
- Subdeltoid (SDB)
- Subcorocoid (SCB)
- Coracobrachial (CBB)
- Subtendinous bursa of subscapularis (SSB)
The SAB is the largest of these, and is in fact the largest bursa in the body. The SAB and SDB in most cases are co-functional and therefore are often grouped as being one big bursa - the SASD bursa.
Figure 1: Bursa around the glenohumeral joint
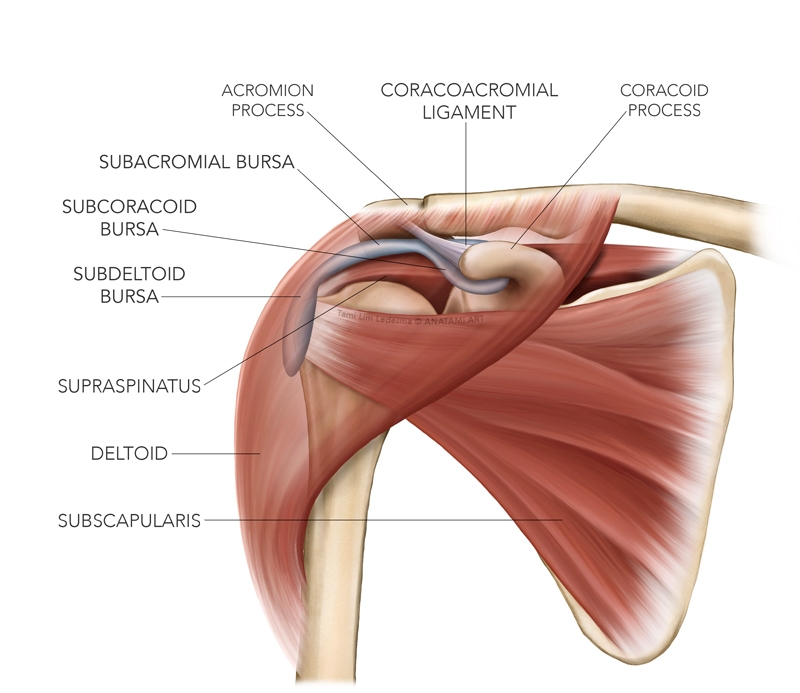
The most extensive anatomical review of the shoulder bursa was conducted by Kennedy et al (2017)⁴, and the key findings can be summarised thus:
- It is a large and consistent structure that is cap-like in shape.
- It does not communicate directly with the glenohumeral joint.
- It is considered to comprise of three separate bursa: the subacromial, the subdeltoid and the subcorocoid components⁴.
- The subacromial bursa has a direct connection with both the subdeltoid bursa (forming the subacromial- subdeltoid bursa) and the subcorocoid bursa⁴.
- The roof of the bursa attaches to the anterior portion of the under-surface of the acromion process⁵, and attaches to approximately 55% of the acromial length⁶. It may extend slightly medial to the underside of the acromioclavicular joint⁶, and also extends under the coracoacromial ligament, and is attached firmly to this ligament⁷.
- The floor of the bursa is attached and blended to the superior part of the supraspinatus ligament⁶'⁷, and may extend anteriorly to also cover the subscapularis tendon, the long head of biceps tendon sheath and the bicipital groove. It may also attach to the infraspinatus posteriorly⁶'⁷.
- The floor of the bursa extends laterally to the outer margin of the greater tubercle of the humerus (subdeltoid portion)⁶'⁷, and at times may extend further down the lateral humerus (ie essentially an inferior bursal extension)⁶.
- The bursa has a widespread network of sensory receptors suggesting that the bursa plays a significant role in pain perception as well as neuromuscular coordination and proprioception. This network may also provide valuable information for the proper control of the shoulder – namely to limit dangerous compressive and shear forces that may impinge the subacromial structures⁸.
- A normal bursa is usually no greater than 2mm thick; however, a pathological bursa with fluid may be thicker than 3mm⁹.
Injury to the SASD bursa
The most common causes of injury to the SASD bursa are as follows¹⁰:- AC joint pathology. If the bursa extends beneath the AC joint then osteophytes and/or swelling in the AC joint may directly impinge on the underlying SASD bursa.
- Supraspinatus tendon tear. In a normal shoulder, the SASD bursa does not communicate with the glenohumeral joint, as it lies above the supraspinatus tendon. In the event of a full-thickness tear of the tendon, the bursa may now communicate with the glenohumeral joint and fluid accumulation may develop.
- Supraspinatus calcific tendinopathy. In this pathology, calcium may leak into the SASD bursa. This type of bursitis is more common in women, and the pain can severe and disabling. Painkilling medications do not usually help¹⁰.
- Direct acute trauma to the bursa. Can include a fall onto the elbow, which drives the humeral head up into the bursa and overlying acromion process. In severe trauma the SASD bursa may rupture.
- Chronic trauma. Repeated impingement of the bursa due to altered glenohumeral centring and dysfunctional scapular mechanics in the overhead athlete may be problematic to overhead athletes such as swimmers, tennis players, gymnasts, weight lifters and throwers, as their exposure to potentially impinging positions is relatively high.
Signs and symptoms
The typical symptoms experienced in SASB include:- Insidious onset of shoulder pain over a few weeks to months, or pain that is acute in nature following a trauma that compresses the humeral head into the acromion with loaded exercises (eg weighted dips).
- Pain is usually felt in the anterior and lateral part of the shoulder, but may radiate down to the mid-humerus level.
- It may be painful to palpate around the top of the humeral head.
- Pain in bed when sleeping on the shoulder or sleeping with the arm overhead and when severe will wake the patient at night.
- A loss of shoulder internal rotation movements – eg putting the hand behind the back.
Testing
The two physical tests commonly used in the clinical diagnosis of a SASD bursitis are as follows:*Neer’s test¹¹(see figure 1) – The therapist stabilises the scapular with one hand and forcefully flexes the shoulder with the other hand. This test is believed to compress not only the bursa, but the rotator cuff tendons and long head of bicep under the acromion process. It has been suggested that if the arm is internally rotated then this isolates the supraspinatus, and in external rotation it isolates the subscapularis¹².
Figure 1: Neer’s Test
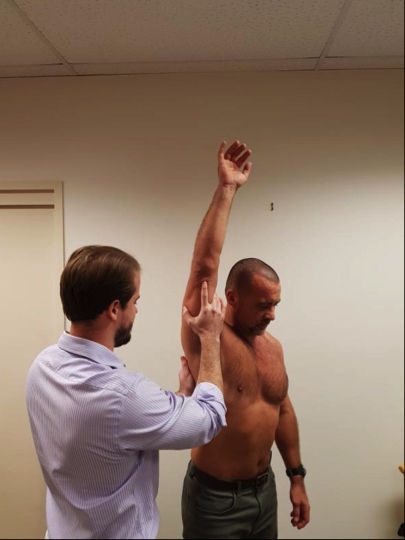
*Hawkins-Kennedy test¹³( see figures 2a and 2b) -The patient’s arm is raised to 90 degrees in forward flexion. The assessor braces the arm in passive forward flexion with one arm and then passively internally rotates the shoulder with the other hand. Pain under the acromion process is positive as a clinical diagnosis of impingement due to the greater tuberosity rotating into the acromion process.
Figure 2a: Hawkins-Kennedy test start
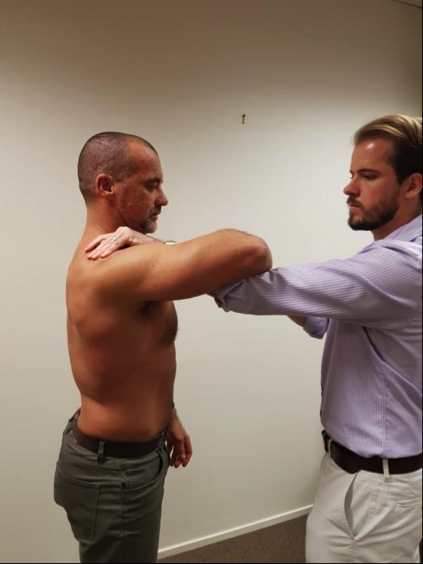
Figure 2b: Hawkins -Kennedy test finish
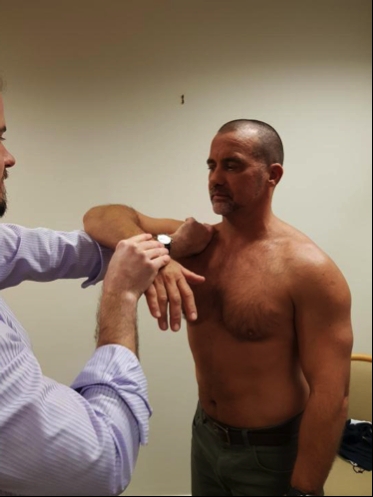
These physical tests used for detecting SASD bursitis may be sensitive, but not necessarily specific for the bursa (since other subacromial structures such as the rotator cuff tendons are also painful with testing)¹⁴'¹⁵.
Treatment
ConservativeIn an acute setting of SASD bursitis, the athlete may need a short period of load management and activity modification to allow the inflamed bursa to recover. For example;
- The high level swimmer may need to reduce pool mileage for a 7-10 day period.
- The elite tennis player may need to limit overhead serving and power in serving.
- The Olympic weightlifter may need to limit overhead lifts for a period of time such as avoiding jerks and snatches.
- Cross-fit athletes may need to avoid overhead loading for short period – eg avoiding handstand positions, overhead squats, instead performing workouts that keep the arm below 90 degrees abduction for a period of time.
Kinematics
The clinician needs to understand the kinematics of the glenohumeral joint to fully appreciate the consequences of how a decrease in subacromial space can adversely affect the SASD bursa and what factors lead to a decrease in space between the acromion and the humeral head. In the normal healthy shoulder, the space between the humeral head to the coracoacromial arch is 1-1.5 cm in height¹⁶and the humeral head to the underside of the acromion process is usually 7-14mm¹⁷. This space may be reduced due to anatomical factors such as the shape of the acromion process and thickening of the coracoacromial ligament.Movement disorders that may affect this space and narrow the space have the potential to chronically impinge the subacromial tissues. In summary, a few significant movement faults to consider are as follows:
- Excessive superior humeral head translation– This is due to excessive deltoid contraction during abduction and is more evident if the arm is abducted in internal rotation as the deltoid has a greater pull and the subacromial space naturally diminishes due to the greater tuberosity rotating closer the acromion process. Interventions to minimise this upward translation are to choose abduction exercises in that involve external rotation.
- Excessive anterior and superior humeral head migration– This is due to a tight posterior capsule¹⁶. Interventions to minimise this upward and anterior translation include stretches for the posterior shoulder capsule.
- Poor depression and centring of the humeral head in abduction– This occurs due to poor rotator cuff activation, particularly the supraspinatus and subscapularis. Interventions for this include isolated activation exercises for the supraspinatus and subscapularis.
To move the acromion process away from the humeral head during abduction movements, the scapular needs to move into upward rotation, external rotation, elevation and posterior tilt¹⁸'¹⁹. Scapulothoracic muscle imbalances and ribcage mobility will both enable this scapular movement. Interventions to improve these individual functions include:
- Improve upward rotation– Reduce hypertonicity and improve myofascial length of the downward rotators such as pectoralis minor, levator scapulae and rhomboids. Improve activation of the upward rotators such as serratus anterior and lower trapezius.
- Improve scapular external rotation– Reduce hypertonicity and improve myofascial length of the internal rotators such as the pectoralis minor and improve activation of the external rotators such as the serratus anterior.
- Improve elevation of the scapular- Reduce hypertonicity and improve myofascial length of the depressors such as the pectoralis minor and the latissimus dorsi. Improve activation of the elevators such as the upper trapezius.
- Improve posterior tilt of the scapular- Reduce hypertonicity and improve myofascial length of the anterior tilt muscles such as the pectoralis minor and improve activation of the posterior tilt muscles such as the serratus anterior.
- Improve rib cage mobility- By improving thoracic spine extension²⁰.
Injection
Injections into the SASD bursa using delayed-release corticosteroids and local anaesthetic (lidocaine) are reasonably common and may have a rapid and significant effect on improving pain and function. Due to the confined space of the bursa, a local anaesthetic will only work in relieving pain in the bursa. If the patient notices almost complete resolution of shoulder pain following injection, then the clinician has more concrete evidence the pain is emanating from the bursa. If pain remains unchanged, the clinician may suspect extra-bursal causes of pain such as AC joint or supraspinatus tendon²¹.References
- Br J Sports Med. 2009; 43:236–241
- BMC Musculoskelet Disord. 2011; 12:119–136
- 2009; 25:305–320
- Clinical Anatomy. 2017; 30:213–226
- Hochberg MC, Silman AJ, Smolen JS, Weinblatt ME, Weisman MH. 2011. Rheumatology. 5th Ed. Philadelphia: Mosby Elsevier. p 686
- 1998; 14:465–470
- Acta Anat (Basel). 1992; 145:354–363
- J Orthop Sci. 1997; 2:295–300
- J Comput Assist Tomog. 2006; 30:316–320
- J Ultrasound. 2015; 18:151–158
- Clin Orthop Rel Res. 1983; 173: 70
- Aust J of Physiotherapy. 2011; 54(3), 159-170
- Am J Sports Med. 1980; 8: 151
- J Bone Joint Surg Am. 2011; 93: 1827-32
- Br J Sports Med. 2008;42:80-92
- Am J Sports Med. 1994;22:779-88
- J Bone Joint Surg Br. 1970;52:524-7
- J Electromyogr Kinesiol. 2009;19:789-99
- Br J Sports Med. 2004;38:64-8
- Arch Phys Med Rehabil. 1999;80:945-50
- Journal of Ultrasound. 2012; 15, 61-68
Newsletter Sign Up
Subscriber Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Newsletter Sign Up
Coaches Testimonials
Dr. Alexandra Fandetti-Robin, Back & Body Chiropractic
Elspeth Cowell MSCh DpodM SRCh HCPC reg
William Hunter, Nuffield Health
Be at the leading edge of sports injury management
Our international team of qualified experts (see above) spend hours poring over scores of technical journals and medical papers that even the most interested professionals don't have time to read.
For 17 years, we've helped hard-working physiotherapists and sports professionals like you, overwhelmed by the vast amount of new research, bring science to their treatment. Sports Injury Bulletin is the ideal resource for practitioners too busy to cull through all the monthly journals to find meaningful and applicable studies.
*includes 3 coaching manuals
Get Inspired
All the latest techniques and approaches
Sports Injury Bulletin brings together a worldwide panel of experts – including physiotherapists, doctors, researchers and sports scientists. Together we deliver everything you need to help your clients avoid – or recover as quickly as possible from – injuries.
We strip away the scientific jargon and deliver you easy-to-follow training exercises, nutrition tips, psychological strategies and recovery programmes and exercises in plain English.









